
|

|
As the disease progresses, symptoms may include ocular pain localized to the area of redundant conjunctiva, chronic foreign body sensation, epiphora and tearing. The excess conjunctiva can lead to a poor distribution of the tear film and excess movement of the conjunctiva, exacerbating the symptoms.
It is important to consider conjunctivochalasis in any patient who presents with ocular discomfort. Risk factors are increased age (50 and higher), history of dry eye disease, prior eye surgery or a history of conjunctival chemosis. The condition also may be associated with blepharitis and contact lens wear.
In symptomatic patients, redundant conjunctival folds between the lower lid margin and the globe are often seen temporally; however, it may present with 360° conjunctival involvement. Fluorescein and lissamine green staining can help identify areas of compromise.
Multimedia
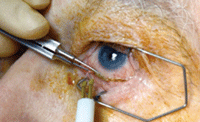
View
a narrated video of cautery and resection procedures.
Photo/video courtesy of Elizabeth Yeu, MD, and Thomas Joly, MD, Virginia Eye Consultants.
The differential diagnosis can be difficult, as common signs and symptoms may be misleading. One tool that may help is tear film osmolarity. In symptomatic patients with a low osmolarity reading, conditions other than dry eye may be present.
Pain is another differentiator—patients with ocular surface disease often complain of chronic irritation; however, those with conjunctivochalasis complain of pain specifically in the affected area.
Lastly, conjunctivochalasis may look similar to conjunctival chemosis, which often responds to antihistamines and anti-inflammatories. If you get a limited response from such therapies, consider conjunctivochalasis as the diagnosis.
Conventional treatments include artificial tears and concurrent treatment of ocular surface inflammation (e.g., topical steroids, non-steroidals, cyclosporine). If unsuccessful, the next step would be surgical intervention via conjunctival cautery or resection, performed 1mm to 2mm away from the limbal area to preserve its stem cells. With either procedure, the goal is to tighten up the excess/loose conjunctiva, reducing friction and chronic irritation on the ocular surface.
Superficial conjunctival cautery is an effective treatment for mild to moderate disease; conjunctival resection is reserved for more advanced cases. Cautery essentially shortens the conjunctiva, while the clamped forceps help to create a seal at the base. For moderate to severe cases, resection is indicated, with or without an amniotic membrane graft, which some surgeons use to promote wound healing (others believe the cost of the membrane does not justify its use).
The amniotic graft can be secured onto the conjunctiva with dissolvable sutures or fibrin tissue glue. Postoperative medications include topical antibiotics for one week, topical steroids for two weeks and topical NSAIDs for two weeks.
As comanaging doctors, optometrists play an integral role in identifying and treating this condition. A surgical referral is indicated to successfully treat this frequently overlooked diagnosis.

