This stems from the fact that, at this point in time, the preponderance of US population at risk for glaucoma is white. About 85% of all adults over 65 in the US population are white; for the population over age 75, whites make up an even larger percentage of the total population (90%).1
However, shifts that are occurring in the demographics of the US population are going to markedly change the make-up and prevalence of glaucoma in the coming decades. Two major population trends are affecting, and will continue to affect, the prevalence of glaucoma for decades. Those are the aging of US society and the growth of minority populations.
An Aging Population
The prevalence of glaucoma is believed to be about 2% (with estimates ranging between 1.6% and 2.7%) in adults over the age of 40.1,3 In the year 2000, an estimated 2.2 million Americans had glaucoma, including those either diagnosed or unknown.1,3 This number is expected to reach 3.3 million by the year 2020.3 The rapid growth in glaucoma is due to the aging of baby boomer population.
Various definitions for baby boomers exist, but it is generally regarded as the cohort born from 1946 to 1964. The first of the baby boom population turned 65 in 2011, and by 2034 all of the baby boom population will be over 65. Based on 2012 census data, 41 million Americans are over the age of 65. Population predictions indicate that from 2010 to 2050 the number of adults over 65 will more than double, to 88.5 million.4
The current aging of the US population has been accompanied by phenomenal growth in the number of the “oldest-old.” The single-fastest growing segment of the US population currently is the group over the age of 90.4 The number of the oldest-old population will continue to grow in the coming decades, with the numbers of Americans reaching age 90 accelerating rapidly after 2030.
Numerous studies have shown that the prevalence of glaucoma increases with age. The Eye Disease Prevalence Research Group developed estimates of glaucoma prevalence from data that included multiple US-based and international studies. The group estimated that open-angle glaucoma prevalence increased from 0.7% at age 40 to 7.7% for those over age 80.3 Self-reported epidemiologic data from the National Health Interview Survey found glaucoma prevalence increasing from 0.2% at age 18 to over 10.7% for those over 75.3 The growth in the oldest-old is important, as the prevalence of glaucoma triples in those over 75 compared to those aged 65.3
| |
|
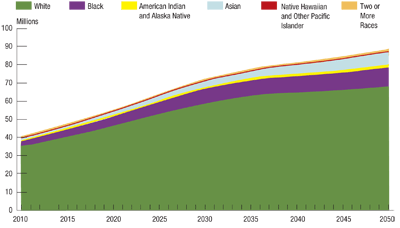
Unless otherwise specified, data refer to population who reported a race alone. Populations for each race group include both Hispanics and non-Hispanics, as those of Hispanic ethnicity may be of any race. Source: US Census Bureau
|
While data is limited, there is no indication that new cases of glaucoma decline in those who reach very advanced age. As such, the number of people who develop glaucoma can be expected to increase throughout the lifespan. The growth of early glaucoma in octogenarians and nonagenarians will present both logistical challenges in caring for adults who may have multi-morbidity, cognitive impairment and frailty, and ethical ones in balancing the benefits of treatment of a disease with a long-term course to impairment with the remaining life expectancy.
Growth of Minority Populations
A second significant contributor to the increasing prevalence of glaucoma is the growth of the non-Caucasian older adult population. It is well known that race plays a role in glaucoma development, with minorities over-burdened by the disease. Over the next several decades, growth in the minority population will be most rapid in those under 65, but by 2050 minorities will make up 42% of the adult population over 65 and 33% of the population over age 85.4 Based on this, the number of minorities with glaucoma will exceed the number of non-Hispanic whites with the disease by the year 2035.5
Among adults over 40, African Americans and Hispanics have between 50% and 300% higher odds of having glaucoma than do whites, at all ages.3 Glaucoma will be particularly significant among older Hispanics due to the exponential growth of this group. Hispanics accounted for 50% of the total growth in the entire US population between the 2000 and 2010 Census reports.6 This rapid growth will continue—the Hispanic population is expected to make up 20% of adults over 65 and 15% of adults over 85 by 2050.6
Other minority populations (Asians, Pacific Islanders, American Indians, Native Alaskans) are expected to increase in numbers relative to whites as well. Among this group, glaucoma risk is most well defined among Asian Americans. Older Asian populations have a risk of open-angle glaucoma estimated to be 6.6% for those over the age of 40. This rate is slightly higher than that seen among Latinos and much higher than that seen in non-Hispanic whites.7
In assessing glaucoma risk among the growing minority older adult population, it’s important to recognize the difference between race and ethnicity. For purposes of the US Census, Hispanic is considered an ethnicity, not a race. The terms Hispanic and Latino are frequently used interchangeably. More specifically, Latino refers to individuals with geographic ties to the Caribbean and Central or South America. Hispanic refers more broadly to those with Spanish ancestry or who are Spanish speakers. Latino ethnicity would include Portuguese-speaking Brazilians, whereas Hispanic ethnicity would not.
When filing out Census forms, individuals may self-identify in a yes/no format as Hispanic/Latino or not Hispanic/Latino. A follow-up question allows individuals who answered yes to identify themselves among one of 23 subgroups largely based on country of origin.
There is a separate race question in the Census, where individual Hispanics may identify themselves as white, black, multiracial or other race. This leads to groups of Americans who identify themselves as Hispanic-whites, Hispanic-blacks or Hispanic of multiracial origin, among several other possibilities. The growth in the racial group identified as white in the US has largely been driven by Hispanics who self-identify their race as white.6
Importantly, the risk of developing glaucoma is not the same among all Hispanic subgroups. Latinos have been found to have higher rates than other Hispanics.3 Among Latinos, Mexican-Americans have generally been found to have a higher risk of open-angle glaucoma than do others who identify themselves as Hispanic. It has been speculated that these differences may be due to the degree of Native American ancestry among Hispanic subgroups.
The two major studies that looked at glaucoma among Hispanics (Proyecto VER) and Latinos (LALES) had significant differences in Native American admixture in their study cohorts. In Proyecto VER, 40% of participants had Native American ancestry, while just 5% of LALES participants did.8 The Mexican-American ethnic group is a key demographic, given that it is the largest among the growing US Hispanic/Latino population.
A similar issue is found among the population of older Asian Americans. While not as numerous as Hispanics and African Americans in the population, the number of older Asians is expected to triple in the US by 2050. Asians of Vietnamese and Chinese descent have a much higher risk of narrow-angle glaucoma than do other ethnic Asians.7 Americans of Japanese descent have a 10-fold higher risk of normal tension glaucoma than do other Asian subgroups.7
Why ethnicity and race impact glaucoma is unclear. There are a variety of anatomical, biochemical and genetic associations with the glaucomas that have been found to segregate by race and ethnicity without being exclusive to a single race. African Americans are known to have a greater likelihood of having thinner corneas, anatomically larger optic discs and variant lamina cribrosa configurations compared to other ethnic groups.9
Mongolians, Indians and Chinese have been found to have differences in anterior chamber angle depth and configuration compared to other ethnic Asian groups and non-Asians.10 The ability to manage ocular oxidative stress appears lower among African Americans.11 Latinos may have an inherently lower tolerance to factors relating intraocular pressure to blood pressure.8,9
Gene-wide association studies have identified a number of single nucleotide polymorphisms associated with open-angle glaucoma, angle closure and normal tension that seem to segregate by race.12 It is entirely possible that race and ethnicity are simply markers for these and other, as-yet unknown biomarkers of glaucoma. Understanding the race-based risk of glaucoma will become even more complex in the future as the number people identified as multiracial grows.
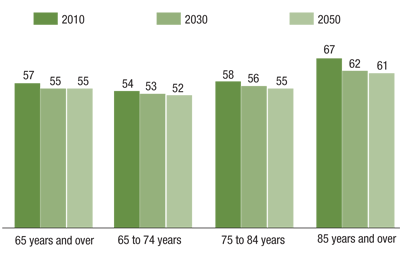
|
|
|
Percent Female for Older Population by Age for the United States: 2010, 2030 and 2050. Source: US Census Bureau
|
A secondary effect of the increase in the number of minority glaucoma patients will be an increase in the number of years these individuals will likely suffer from the disease. In addition to having a higher risk of glaucoma, African Americans and Hispanics begin to develop glaucoma at earlier ages than do whites.3 The prevalence of glaucoma in African Americans and Latinos is about 2% for those in their early 50s. It does not reach 2% for whites until age reaches the late 60s to early 70s.
At the other end of the glaucoma age continuum, life expectancy is longer for Hispanics and Asians than for other ethnic groups. Among those in the US population who live to 65, Hispanics have the longest remaining life expectancy of any ethnic group, at more than 20 years.4 At younger ages, African Americans have lower life expectancy than other ethnic groups; however, among the oldest Americans—those 85 and older—there is a shift and African Americans have a slightly longer life expectancy than other racial groups.4 The end result will be a longer required treatment period.
Gender Distinctions
The expected time course of the disease is also impacted by gender. In studies done across the world, the absolute number of women with glaucoma exceeds that of men with the disease (a 60:40 ratio).13 The gender gap in glaucoma is largely due to the differential survival of women and men.
At birth, across all racial and ethnic groups in the US population, women are expected to live about four to five years longer than men. The gap in the life expectancy of men compared to women narrows with advancing age over 65, but men never quite catch up in terms of expected survival, even among those men over 90.4
In terms of absolute risk, women have higher odds of developing narrow-angle glaucoma than do men. There is variation among ethnic groups, but most estimates place the gender risk at two to four times higher for women than men. The excess risk is largely attributed to the anatomically smaller anterior chambers found in women.13 The evidence for gender differences in open-angle glaucoma risk is less clear. Studies of gender differences in POAG when stratified by age and race or ethnicity produce relatively small numbers. This leads to wide estimate intervals, making interpretation of the exact gender impact difficult. Studies do indicate that women are more likely than men to become visually impaired from glaucoma.
The differential survival of women gives them more years of disease exposure. Life expectancy alone does not account for all of the gender disparity in visual impairment associated with glaucoma, however. Socioeconomic and educational opportunity is thought to play a role in this disparity, particularly outside of the US population.
Poverty Status
Poverty is associated with the development of myriad health conditions. The question, “Does poverty lead to glaucoma?” has not been fully answered, but has had some study. The US government uses a metric the poverty-to-income ratio (PIR) as a measure of socioeconomic status. The PIR is a continuous measure that takes into account the income, expenses and family size. Those with PIR <1.0 have income below the federal poverty level for families, whereas those with PIR >4 are considered to have high income.
Elongation of the vertical cup/disc (CD) ratio is a hallmark sign of glaucoma. Many studies use the vertical cup/disc ratio at the 97.5th population percentile as the cut point for a disc defined as glaucomatous. Within the overall US population, this level is a vertical CD ratio of 0.63.1 One study has compared the 97.5th percentile of vertical CD ratio among the US population at various PIR categories. No differences in the vertical CD ratio size that defined glaucoma were found between PIR categories. This indicates that socioeconomic status does not seem to be related to early glaucoma.
This same study showed that PIR did have an impact on the vertical CD ratio at the 99.5th population percentile.1 As PIR category changed from high income to middle income to the poverty level, the vertical cup/disc ratio increased. This change is likely representative of an overall delay in the diagnosis of glaucoma or higher numbers of treatment failures for those in lower socioeconomic classes producing larger vertical CD ratios even at the most extreme range found within the population.
Studies in the United Kingdom and Canada have shown that those in lower socioeconomic classes are more likely to present with more advanced glaucoma at the time of the initial diagnosis.14 Lower socioeconomic status within the US population has been associated with lower medication adherence in studies using electronic drop monitoring.15 Race and age also appear to play a role with adherence, with African Americans and older adults showing lower adherence compared to younger adults and people of European ancestry.15 Insurance claims data monitoring in the US population has shown that half of all patients stop glaucoma medications within six months of initiating therapy and less than 40% fill prescriptions three years after diagnosis.16
Additionally, in the US population, those in lower socioeconomic classes are known to have lower utilization of eye care services.17 Education level and socioeconomic status are closely tied together, and lower eye care utilization rates are also seen in Americans with lower educational attainment.17
While not directly related to education level, health literacy (or the ability to understand health-related information) has been shown to play a role in glaucoma adherence. Glaucoma patients with poor health literacy are less likely to fill prescriptions and adhere to medication dosage schedules, and more likely to miss scheduled appointments.18
Simplified dosages schemes, improved doctor/patient communication and better education have been shown to increase patient adherence in glaucoma treatment.19 Providing appropriate education and strategies to patients that are increasingly diverse will be an ongoing challenge for ODs.
The increasing diversity of the US population will present challenges in delivering care to patients with glaucoma. The public health task is daunting. Current estimates are that 60% to 70% of glaucoma in the US population is undiagnosed.21 This may be even higher among the rapidly growing Latino population.8
When taking into account the low levels of adherence to glaucoma medication regimens, as much as 80% of glaucoma in the US population may be untreated.20,21 This is despite the fact that more than double the number of patients estimated to have glaucoma in the US population report using drops for the disease or ocular hypertension.20 This suggests that there is a nationwide issue of diagnostic accuracy among both optometrists and ophthalmologists.
The Challenges Ahead
Optometrists need to be prepared to see a larger and more diverse glaucoma population. To meet the coming demand, vastly greater numbers of the higher at-risk population will need to be screened. The absence of a simple screening test for glaucoma means more comprehensive examinations with appropriate follow-up testing are going to be need to be provided by optometrists.
Larger societal issues, such as lower levels of health insurance coverage, higher levels of poverty and lower education level, will make reaching this population difficult. Once glaucoma patients are diagnosed, optometrists as a group need to take a far greater role in treatment.
The use of culturally sensitive materials and approaches can help reach the ultimate goal of prevention of visual impairment in this rapidly changing segment of the patient population.
Dr. Swanson is an associate professor of optometry at the University of Alabama at Birmingham School of Optometry.
1. Swanson MW. The 97.5th and 99.5th Percentile of Vertical Cup Disc Ratio in the United States Optometry & Vision Science: January 2011, Vol. 88, Issue 1, pp. 86-92 doi:10.1097/OPX.0b013e3181fc3638
2. Vincent GK, Velkoff VA. The Next Four Decades, The Older Population in the United States: 2010 to 2050, Current Population Reports.2010, U.S. Census Bureau, Washington, DC P25-1138.
3. Klein R, Klein BE. The prevalence of age-related eye diseases and visual impairment in aging: current estimates. Invest Ophthalmol Vis Sci. 2013 Dec 13;54(14): doi: 10.1167/iovs.13-12789.
4. Arias E. United States Life Tables, 2009. National Vital Statistics Reports, Vol. 62, No. 7, January 6, 2014 .
5. Vajaranant TS, Wu S, Torres M, Varma R. The changing face of primary open-angle glaucoma in the United States: demographic and geographic changes from 2011 to 2050. Am J Ophthalmol. 2012 Aug;154(2):303-314.e3. doi: 10.1016/j.ajo.2012.02.024. Epub 2012 Apr 27.
6. Ennis SR, Ríos-Vargas M, Albert NG. The Hispanic Population: 2010 Census Briefs. Issued May 2011
C2010BR-04 Available at www.cdc.gov/nchs/data/nvsr/nvsr62/nvsr62_07.pdf. Accessed 6/2/2014.
7. Stein JD. Differences in Rates of Glaucoma among Asian Americans and Other Racial Groups, and among Various Asian Ethnic Groups Ophthalmology; 2011:1031-7.
8. Kim E, Varma R. 9. Arch Ophthalmol. Glaucoma in Latinos/Hispanics.Current Opinion in Ophthalmology 2010 ;21:100–105. doi:10.1001/archopht.123.4.527.
9. Karmel M. Glaucoma in the African American and Latino Communities. EyeNet Available at www.aao.org/publications/eyenet/201006/glaucoma.cfm. Accessed July 1, 2014.
10. Aung T, Winifred P, Nolan WP, et al. Anterior Chamber Depth and the Risk of Primary Angle Closure in 2 East Asian Populations FREE Arch Ophthalmol. 2005;123(4):527-32. doi:10.1001/archopht.123.4.527.
11. Siegfried CJ, Shui YB, Holekamp NM, et al. Racial Differences in Ocular Oxidative Metabolism, Implications for Ocular Disease. Arch Ophthalmol. 2011;129(7):849-54. doi:10.1001/archophthalmol.2011.169
12. Chandra A, Mitry D, Wright A, et al. Genome-wide association studies: applications and insights gained in Ophthalmology.Eye advance online publication 27 June 2014; doi: 10.1038/eye.2014.145
13. Vajaranant TS1, Nayak S, Wilensky JT, Joslin CE. Gender and glaucoma: what we know and what we need to know. Curr Opin Ophthalmol. 2010 Mar;21(2):91-9. doi: 10.1097/ICU.0b013e3283360b7e
14. Buys YM, Jin YP; Canadian Glaucoma Risk Factor Study Group. Socioeconomic status as a risk factor for late presentation of glaucoma in Canada. Can J Ophthalmol. 2013 Apr;48(2):83-7. doi: 10.1016/j.jcjo.2012.10.003
15. Dreer LE, Girkin C, Mansberger SL. Determinants of medication adherence to topical glaucoma therapy. J Glaucoma. 2012 Apr-May;21(4):234-40. doi: 10.1097/IJG.0b013e31821dac86
16.Nordstrom BL, Friedman DS, Mozaffari E, et al. Persistence and adherence with topical glaucoma therapy. Am J Ophthalmol. 2005 Oct;140(4):598-606.
17. Zhang X, Beckles GL, Chou CF, et al. Socioeconomic disparity in use of eye care services among US adults with age-related eye diseases: National Health Interview Survey, 2002 and 2008. JAMA Ophthalmol. 2013 Sep;131(9):1198-206. doi: 10.1001/jamaophthalmol.2013.4694
18. Muir KW, Christensen L, Bosworth HB. Health literacy and glaucoma. Curr Opin Ophthalmol. 2013 Mar;24(2):119-24. doi: 10.1097/ICU.0b013e32835c8b0e
19. Okeke CO, Quigley HA, Jampel HD, et al. Interventions improve poor adherence with once daily glaucoma medications in electronically monitored patients. Ophthalmology. 2009 Dec;116(12):2286-93. doi: 10.1016/j.ophtha.2009.05.026. Epub 2009 Oct 7.
20. Swanson MW. Undiagnosed and Over Diagnosed glaucoma in the United States. Invest Ophthalmol Vis Sci 2012;53: ARVO E-Abstract 6379/A17
21. Varma R, Ying-Lai M, Francis BA, et al; Los Angeles Latino Eye Study Group. Prevalence of open-angle glaucoma and ocular hypertension in Latinos: the Los Angeles Latino Eye Study. Ophthalmology. 2004 Aug;111(8):1439-48.

