 |
Research shows that if a doctor only relies on symptoms to make a diagnosis of dry eye disease (DED), they will likely be wrong about 40% of the time.1,2 So how could a patient have symptoms of dryness, grittiness, blurred or fluctuating vision and irritated eyes that typically occur late in the day or after computer use and not have DED?
Diagnostic Dilemma
A patient presents in your office for a dry eye evaluation with the common symptoms of dry eye disease. You measure tear osmolarity at 284 OD and 287 OS. InflammaDry (RPS) testing is negative. Meibomian gland expression reveals mild turbid meibum and there is mild truncation of the glands on meibography. The tear film break-up time (TBUT) is four seconds, and there is trace inferior corneal staining with NaFl dye. So now what do you do?
Using symptoms to diagnose this patient could give you the wrong diagnosis, not just because there are times when patients with DED don’t experience symptoms, but also because many conditions have symptoms similar to DED.1 This patient had been on therapies for almost six months before seeking another doctor, stating that his drops weren’t working. During examination, a cover test revealed exophoria at distance, which was confirmed with Von Graefe, and further testing diagnosed convergence insufficiency. The patient was referred to a vision therapy specialist and returned to the office with no dry eye symptoms and even mentioned that his headaches had resolved.
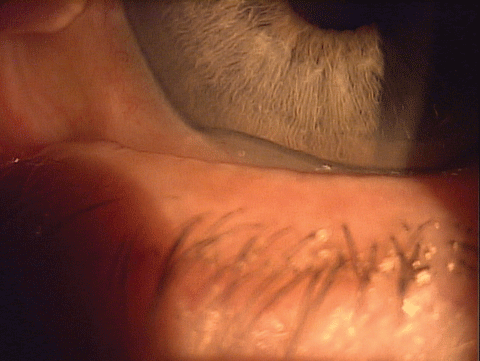 |
| A patient referred for DED was actually diagnosed with conjunctivochalasis. |
As this patient illustrates, too often patients are put on dry eye medications and artificial tears simply because their symptoms match that of DED. They also have a test or two, particularly the older, more invasive ones such as TBUT, that appear to confirm dry eye and even trace inferior corneal staining. The patient then uses medications for dry eye expecting relief; instead, they return frustrated and blame the drops (which would have worked if the patient really had dry eye) or even seek another eye care provider.
DED Differentials
In addition to the aforementioned convergence insufficiency, other dry eye disease differentials include:• Conjunctival concretions. These may cause gritty eyes or foreign body sensation.
• Conjunctivochalasis (CCH). This eventually may lead to DED and typically causes symptoms of grittiness, foreign body sensation, epiphora and red, irritated eyes.
Patients with CCH usually test positive for corneal and conjunctival staining and a rapid TBUT; typically in mild to moderate cases, osmolarity is normal while MMP-9 testing is elevated.3-5
The presence of more frequent subconjunctival hemorrhages may point more toward a diagnosis of CCH, but the overlap with dry eye disease represents yet another reason for consideration of advanced testing in ocular surface disease management.6
• Salzmann’s nodular degeneration (SND). This has been shown to mimic dry eye and, like DED, is bilateral in 63% of cases.7,8 Histopathologically, the epithelium over the nodules is considerably thinned in SND, resulting in symptoms of dryness, foreign body sensation, gritty eyes and irritation.7 The most common symptom is blurred vision.8 However, studies show that about 40% of patients with SND also have meibomian gland dysfunction (MGD).9,10 Added to that, research has linked it to inflammation and inflammatory systemic conditions such as Crohn’s disease.9,10
• Anterior blepharitis. Patients with Staphylococcal and Demodex blepharitis can experience itching, irritation, dryness and blurred vision.
• Contact lens discomfort. Discomfort associated with contact lens wear typically results in symptoms of dry eye but dissipates when the contact lens is not worn. The cause of these dry eye symptoms could range from early DED and MGD to issues with the contact lens material, solution or compliance.
Other contact lens complications such as giant papillary conjunctivitis (GPC) can result in DED symptoms as well, ranging from decreased contact lens wearing time to foreign body sensation and irritated eyes.11
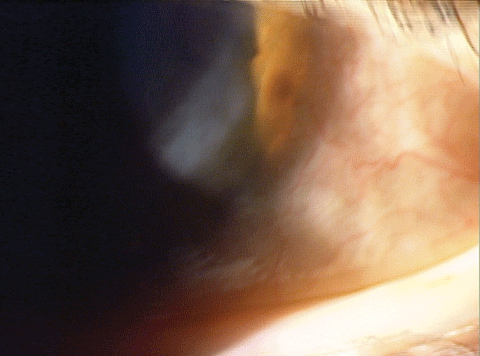 |
| A patient presenting with DED symptoms diagnosed with mild Salzmann’s nodular degeneration. |
• Conjunctivitis. Bacterial, viral and allergic conjunctivitis can all present with similar patient complaints as DED. For example, studies show that a large percentage of patients with DED have symptoms of itching, and patients with allergic conjunctivitis complain of dryness.12 Differentiating conjunctivitis from dry eye disease requires an astute clinician, as the difference often involves a systemic finding such as allergic dermatitis or rhinitis, which occur in allergic conjunctivitis cases but rarely in DED.13
Recently, a colleague spent a day in the Advanced OSD clinic to enhance his knowledge of DED management. At the end of the day I apologized because, of the nine new patients that day, only one had a diagnosis of DED. He responded by saying that learning more about these other potential causes was more valuable to his dry eye clinic than anything else he could have observed.
DED Testing
One of the only ways to determine if a patient has a condition other than DED even though symptoms point to dry eye disease is to use advanced testing—such as point-of-care diagnostics—skilled clinical evaluation and newer testing procedures such as meibomian gland expression and meibography.14
Clinicians should also include a cover test and binocular function testing in their dry eye work-up.15 Combining tests increases specificity and sensitivity for an accurate diagnosis. Using only traditional testing known to have very low sensitivity to dry eye, such as NaFl staining and Schirmer tear testing, could further mislead the clinician, resulting in months of futile therapy for a diagnosis that isn’t truly there.1,16-18
Dr. Karpecki is a consultant/advisor to: AMO, Alcon Labs, Allergan, Akorn, Bausch + Lomb/Valeant, BioTissue, Bruder Healthcare, Beaver-Visitec, Cambium Pharmaceuticals, Essilor, Eyemaginations, Eyes4Lives, Focus Laboratories, Glaukos, iCare USA, Ocusoft, Konan Medical, Optometric Medical Solutions, Reichert, Shire Pharmaceuticals, RySurg, Science Based Health, SightRisk, TearLab, TearScience, TLC Vision, Topcon and Vmax.
|
1. Sullivan BD, Crews LA, Messmer EM, et al. Correlations between commonly used objective signs and symptoms for the diagnosis of dry eye disease: clinical implications. Acta Ophthalmo-logica, 2014 Mar;92(2):161-6. 2. Bron A, Tomlinson A, Foulks GN, et al. Rethinking dry eye disease: a perspective on clinical implications. Ocul Surf. 2014 Apr;12(2 Suppl):S1-31. 3. Yamamoto Y, Yokoi N, Higashihara H, et al. Clinical characteristics of short tear film breakup time type dry eye. Nippon Ganka Gakkai Zasshi. 2012 Dec;116(12):1137. 4. Acera A, Rocha G, Vecino E, et al. Inflammatory markers in the tears of patients with ocular surface disease. Ophthalmic Res. 2008 Oct;40(6):315-21. 5. Acera A, Vecino E, Duran JA. Tear MMP-9 levels as a marker of ocular surface in-flammation in conjunctivochalasis. Invest Ophthalmol Vis Sci. 2013 Dec 23;54(13):8285-91. 6. Yamamoto Y, Yokoi N, Ogata M, et al. Correlation between recurrent subconjunctival hemorrhages and conjunctivochalasis by clinical profile and successful surgical out-come. Eye Contact Lens. 2015 Nov;41(6):367-72. 7. Hurmeric V, Yoo SH, Karp CL, et al. In vivo morphologic characteristics of Salzmann nodular degeneration with ultra-high-resolution optical coherence tomography. Am J Ophthalmol. 2011 Feb;151(2):248-56.e2. 8. Fario AA, Halperin GI, Sved N, et al. Salzmann’s nodular corneal degeneration clini-cal characteristics and surgical outcomes. Cornea. 2006 Jan;25(1):11-5. 9. Graue-Hernandez EO, Mannis MJ, Eliasieh K, et al. Salzmann nodular degeneration. Cornea. 2010 Mar;29(3):283-9. 10. Roszkowska AM, Spinella R, Aragona P. Recurrence of Salzmann nodular degen-eration of the cornea in a Crohn’s disease patient. Int Ophthalmol. 2013 Apr;33(2):185-7. 11. Forister JF, Forister EF, Yeung KK, et al. Prevalence of contact lens-related compli-cations: UCLA contact lens study. Eye Contact Lens. Jul 2009;35(4):176-80. 12. Hom MM, Nguyen AL, Bielory L. Allergic conjunctivitis and dry eye syndrome. Ann Allergy Asthma Immunol. 2012 Mar;108(3):163-6. 13. Ortiz RA, Barnes KC. Genetics of allergic diseases. Immunol Allergy Clin North Am. 2015 Feb;35(1):19-44. 14. Lemp MA, Bron AJ, Baudouin C. Tear osmolarity in the diagnosis and management of dry eye disease. Am J Ophthalmol. 2011 May;151(5):792-8. 15. Rueff EM, King-Smith PE, Bailey MD. Can binocular vision disorders contribute to contact lens discomfort. Optom Vis Ci. 2015 Sep;92(9): 214-21. 16. Savini G, Prabhawasat P, Kojima T, et al. The challenge of dry eye diagnosis. Clini-cal Ophthalmology. 2008;2(1):31–55. 17. Schiffman RM, Christianson MD, Jacobsen G, et al. Reliability and validity of the Ocular Surface Disease Index. Arch Ophthalmol. 2000 May;118(5):615-21. 18. Nichols KK, Nichols JJ, Mitchell GL. The lack of association between signs and symptoms in patients with dry eye disease. Cornea. 2004 Nov;23(8):762-70. |

