When a patient in his or her 40s first reports trouble seeing at near, what is your next step? Someone wearing spectacles might reasonably wish to stay with them. Or maybe not—you might take this occasion to introduce or reiterate the option of contact lens correction, as the patient will need new lenses (either progressives or stand-alone reading glasses) anyway. One piece of advice from multiple sources: Be proactive in discussing multifocal contact lenses, which today are considered better than ever, with unprecedented high success rates.
Naturally, a long-time contact lens wearer might prefer to stay in contact lenses. These days, there are several effective multifocal contact lens designs—including soft, gas permeable and hybrid lenses—that satisfy wide-ranging yet individualized visual demands. The mantra seems to be, multifocal contact lenses will fulfill most of a patient’s visual demands most of the time. Efforts to maximize lighting, a critical factor especially with near vision, as well as the occasional use of a pocket magnifier may improve success.
Practitioners today must grapple with some pertinent and potentially profitable facts. For one, the presbyopic population continues to expand—with the number of presbyopes in the US projected rise to 116 million (36%) in 2016 from 108 million (35%) in 2011.1 Even as the population grows, however, we also know that contact lens use diminishes sharply with age.
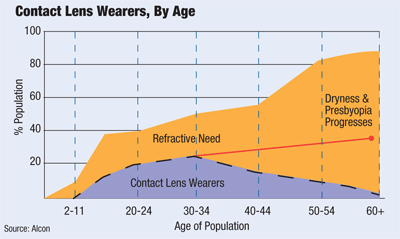
Contact lens wear declines as refractive need begins to dramatically increase. The red line shows a projection of the potential contact lens wearing population if drop-outs could be eliminated.
The good news: Contact lens wearers are largely committed to remaining in contact lenses. This is the core of your patient population for multifocal contact lenses. Some 91% of contact lens wearers ages 35 to 55 have their hearts set on continuing with contact lenses.2
Here we find an unmet need among early presbyopes. In a 2009 survey of 500 presbyopic patients, only 8% of contact lens wearers reported being told about multifocal contact lenses when they first complained about near vision problems.3 The same study found that one out of three patients said they would likely switch to another practitioner if their current doctor did not inform them about multifocal contact lenses.
Fact is, many presbyopes express an interest in trying multifocal contact lenses. In a 2007 survey conducted by the Contact Lens Council, 40% of patients reported that they were unaware that multifocal contact lenses could correct their presbyopia.4
The key is to start the patient in multifocal contact lenses early in presbyopia.5 What are the advantages? The patient adapts more smoothly when moving into a low-add lens. At this stage, the patient is less likely to get frustrated and perhaps drop out. Success rates are high when fitting presbyopes at an early stage—and those satisfied patients are likely to boost referrals to your practice.
Be Proactive
When dealing with a patient who reports or exhibits symptoms of early presbyopia, the first step is to communicate all available options to correct the problem.
A patient accustomed to glasses may lean toward progressive addition lenses or some other spectacle correction, such as reading glasses. But don’t assume that is a given—don’t take it for granted that a patient is unwilling to try contact lenses, even those well into their 40s. Looking at the long term, contact lenses are not solely for the young; depending on their tear film integrity and other factors, some patients wear contact lenses happily well into their 70s.
Explaining all options inevitably includes the pros and cons of monovision. Though recognizing that monovision works in the short term, specialty contact lens practitioners tend to cast aspersions on this option, seeing it as an inferior (though less expensive) option and envisioning worsened binocularity down the road.
“Monovision is dead,” proclaims Jack Schaeffer, OD, of Schaeffer Eyecare Center in Birmingham, Ala. “Monovision is a cop-out. It is an alternative avenue for a doctor to charge a lower fee, spend less time and give the patient less care.” At some point, monovision is going to reduce stereopsis, and patients will also experience reduced night vision. “You’re putting the patient and others in danger when driving at night because of the reduced vision,” Dr. Schaeffer says.
“Doctors should charge a higher fee for multifocal contact lenses to compensate for their time,” says Dr. Schaeffer, “because it takes additional chair time and expertise to have multifocal success.”
As with any presbyopic correction, monovision delivers a mix of advantages and disadvantages. “It’s not only harder to fit them in a multifocal after they’ve used monovision,” says Thomas Quinn, OD, a private practitioner from Athens, Ohio. “We believe that there’s also a neurological adaptation required. It’s like asking a runner to swim and a swimmer to run. It’s hard to switch. Likewise, there’s some brain adaptation when you switch from monovision to multifocals.”
A prerequisite to success is a patient who understands how multifocal contact lenses work and what it takes to achieve an optimal fit. This is where an exhaustive face-to-face conversation with the patient comes in. Few other patient encounters in eye care demand such an extensive degree of practitioner-patient communication. Here you convey the pros and cons of all available corrective options, carefully interview the patient about occupational and leisure-activity visual demands, and develop an early sense of which multifocal contact lens design might best satisfy the patient’s specific individual needs.
Be careful here. Emphasize the benefits of your first lens of choice without suggesting that it will solve all their visual needs at all times. There is no magic bullet. All presbyopic corrections come with trade-offs. Discuss the limitations of multifocal contact lenses and the other presbyopia correction options. Set realistic expectations for the patient. A patient who knows what to expect and is willing to accept the compromises is less likely to drop out of contact lens wear or blame your practice for promising more than you delivered.
Be Creative
Many contact lens practitioners recommend using the manufacturer’s evidence-based fitting guidelines, at least as a way to choose an initial lens design. Some clinicians, especially those with extensive experience fitting all types of contact lenses, may choose to disregard the guidelines altogether and place their faith in their own empirically-based intuition, which is fine, too. Whatever your level of expertise, though, it’s hard to question the value of evidence-based fitting guidelines that incorporate clinical research rigorously conducted by experienced specialty contact lens practitioners.
One of those investigators is New York optometrist Susan Resnick. She favors the use of fitting guidelines, perhaps in part because she has worked hard contributing to these advisory documents.
“One of the mistakes—probably less prevalent among the newer clinicians than among older ones like myself—is that sometimes we rely on past experience to approach new products,” she says. “And that can be a problem. Because some of us have ingrained habits that have worked in the past, we feel like we have experience in making the sort of adjustments and knowing where to start. You start tweaking too soon, you start changing the recipe before you’ve tasted it.”
Dr. Resnick advises colleagues to follow the guidelines for your first trial pair of lenses, and to follow the manufacturer’s nomogram and flowchart for troubleshooting. Once you select an initial lens, and carefully evaluate it, you will be on the path to a more efficient and successful fitting outcome.
In the meantime, have the patient try their new lenses—first within and then outside the office—for 10 minutes or so as the lenses settle. Listen closely to the patient’s account of their initial experience with the lenses. Fitting multifocal contact lenses often calls for clinical creativity based largely on the patient’s subjective experience. It’s one of the instances in which the patient’s subjective impressions play a paramount role in achieving clinical success.
After the initial fitting, you should have the patient come back in a week or two, or else call the patient to get a report of his impressions. You don’t need to speak face-to-face to find out how the patient is doing. If they’re having trouble with some aspect of their vision, invite the patient to visit so you might rectify the matter.
Be Persistent
Practitioners recommend limiting the number of lens choices of varying powers that you try to two or three. That is, don’t abandon the modality if your initial lens design and prescription leave the patient with subpar vision in some circumstances. Maybe a different lens or adjustment of powers will provide just what the patient needs. Crucial to clinical success is the effort to fit patients according their occupational and leisure-time activities. A patient who is an avid reader has different visual needs from, say, an avid golfer.
Practitioners commonly agree to provide follow-up care on a per-visit cost basis. A time frame of 60 to 90 days for anticipated follow-up visits—which may or may not prove to be necessary—sets a general limit for follow-up visits. At some point, you or the patient may decide that another option is best, but do allow for some trial-and-error before making that decision.
Be Realistic
Kenny Rogers famously put some valuable advice to song: “Know when to walk away.” Maybe the optometrist is something of a clinical version of “The Gambler” when it comes to tricky contact lens fits. Given today’s lens designs, the odds are on your side. The question boils down to, how exactly do you know the time has come to discontinue fitting? “There are some patients who want to try every single power combination that you have,” says Jason Miller, OD, of Powell, Ohio. “And certainly that can be very time-consuming. Number one, I try to minimize the number of follow-ups. If you understand the designs of the lenses, you can usually make a couple changes and correct someone’s vision early on. But there are times when some patients are a very challenging fit, either because of their expectations or visual needs.”
That stands to reason. But how do you address it? “Narrow it down to two lens choices for the patient, one that may give a little more distance and one that maybe gives a little more near,” Dr. Miller says, echoing a popular refrain in optometric offices: “Ask them, ‘Which do you like better, lens one or lens two? Which one gives you better vision?’ Let them decide. That will help minimize your follow up.”
Be Fairly Compensated
No one disputes the reality that fitting multifocal contact lenses—especially with mid- to late-stage presbyopia—is a time-consuming task requiring extensive consultation and chair time. When setting fees, don’t undervalue the worth of your expertise, not to mention your time.
Many practitioners favor a sort of modified global fee approach. That is, they charge for a comprehensive eye exam, a diagnostic contact lens fitting and materials. The degree of follow up care hinges on the patient’s prognosis at the initial visit. In the case of a failed fit, many clinicians limit refunds solely for returnable lenses.
“We use a modified global fee structure,” says S. Barry Eiden, OD, who practices in Deerfield and Park Ridge, Ill. “We will perform a contact lens diagnostic evaluation and initial fitting to determine the lens design that we feel will be most appropriate. If the patient is an established and successful contact lens wearer, we may dispense diagnostic lenses and order their annual supply at that time in order to keep costs under control.”
But, many cases require aftercare visits, he adds, “which we charge in advance for a specified period of time. Then again, some cases that require aftercare may be more straightforward and we decide to perform perhaps only one or two aftercare visits, which we charge on a per-visit basis.”
Satisfy an Underserved Population
There exists a large unmet need for contact lens patients, including those with incipient presbyopia. It’s an expensive proposition for the patient, not to mention one of the more time-consuming services you can deliver. The best time to fit a presbyope in contact lenses is at the early stages of visual symptoms.
The idea here is to start the patient in multifocal contact lenses when they are easiest to fit, owing to a low add. As the patient adapts to and embraces multifocal contact lenses over time, you not only have a satisfied patient but also one who is likely to tell family members and friends about your skills and corrective options.
1. The 2011 Comprehensive Report on the Global Presbyopia Correcting Surgery Market. St. Louis, MO: Market Scope.
2. Reindel WT, Edmunds FR. A clinical assessment of presbyopic soft contact lens designs: comparing the impact of SofLens multifocal contact lenses and Acuvue bifocal contact lenses on successfully adapted monovision patients. Rev Optom. 2003 Apr 15;140(4).
3. Studebaker JB. Soft multifocals: practice growth opportunity. Contact Lens Spectrum. June 2009.
4. Eye on innovation [survey]. Landover, MD: Contact Lens Council; 2007.
5. Alcon Laboratories. Best practices for multifocal contact lens use in your practice [webinar]. August 8, 2012.

