 |
Phenylephrine hydrochloride is ubiquitous among all ophthalmic practices. While it is used mostly to perform routine dilations, this readily available drug has a robust roster of ophthalmic uses, some of which might surprise you. But once you understand its mechanism of action, you will be confident when reaching for phenylephrine for far more than dilation; you will also be prepared for any potential side effects.
How It Works
Phenylephrine functions as a direct-acting sympathomimetic agent, which works to primarily stimulate alpha-1 adrenergic receptors.1 The body’s autonomic nervous system (ANS), which regulates many involuntary organ functions, is divided into the parasympathetic and the sympathetic nervous system. The parasympathetic system is responsible for functions that occur when the body is at rest while the sympathetic nervous system elicits an action response.
These two branches work synergistically to regulate internal organs within the body.2 Administering phenylephrine stimulates the sympathetic branch, giving rise to its various applications (Table 1).
|
|
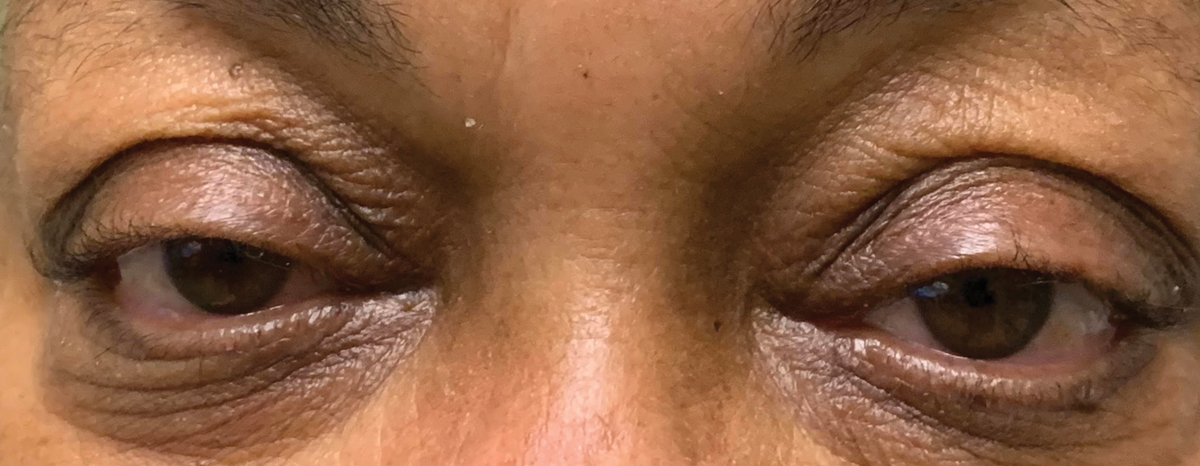
Mild ptosis secondary to sympathetic dysfunction. Click image to enlarge. |
In-office Use
Ophthalmic solutions of phenylephrine are available in different concentrations, depending on use. The 1% formulation is primarily for dilated ophthalmic exams in newborns. The most widely used concentration is the 2.5% phenylephrine hydrochloride solution, which is used routinely for dilations in adults and children over three months of age. Finally, 10% is also available but used less commonly due to its potential systemic absorption.1 Here’s a look at the many ways you can use this ophthalmic drug in your practice:Pharmacologic dilation. Phenylephrine acts on the alpha-1 receptors located on the iris dilator, which stimulates smooth muscle contraction and allows for pupillary dilation and funduscopic examination.3 While the end result is pupillary dilation, phenylephrine has little effect on accommodation. Instead, ciliary muscle contraction causes accommodation and yields a change in power within the crystalline lens. This is regulated via the parasympathetic, not the sympathetic, branch of the ANS.
Though there has been conflicting evidence in the literature, researchers generally believe phenylephrine administration does not interfere with parasympathetic activity; however, testing accommodation through a dilated pupil increases blur and reduces the depth of field, making it difficult to acquire accurate measurements.2
Inflammation. Phenylephrine causes sympathetic stimulation of blood vessels, leading to vasoconstriction.2 In the ophthalmic setting, 0.12% phenylephrine is an ingredient in some over-the-counter eye drops that are marketed to alleviate red eyes through vasoconstriction.1
This function is also useful in determining the degree of ocular inflammation, specifically when distinguishing scleritis from episcleritis. Episcleritis is the inflammation of the episcleral vascular network, which causes activation of immune cells and inflammatory mediators that lead to vasodilation. Thus, application of 2.5% phenylephrine can be a useful tool to evaluate the depth of vascular inflammation. Approximately 10 to 15 minutes following instillation, the superficial blood vessels of the episclera will blanch, leaving an otherwise white and quiet eye. However, if scleritis is present, hyperemia will remain after phenylephrine instillation due to the lack of drug penetration to the deeper vessels of the sclera.4
General UsesBeyond optometry, phenylephrine hydrochloride is indicated for intravenous use to elevate blood pressure in patients with severe hypotension in the setting of septic shock or anesthesia. It’s also used intranasally for congestion and topically as a component of hemorrhoid cream due to its vasoconstrictive properties.2 |
Uveitis. In the management of anterior uveitis, phenylephrine has many benefits. Due to the mechanism resulting in dilation, the 10% concentration is often potent enough to aid in breaking recalcitrant posterior synechia.5
Since photophobia in these conditions is attributed to the pupillary response to light, phenylephrine’s mydriatic properties will also help paralyze the pupil and mitigate pain. Researchers further suggest that phenylephrine acts on aqueous flow dynamics and vascular permeability of the uvea, yielding improvement in anterior chamber flare following instillation.6
Ptosis. Patients may present with ptosis for several reasons, and phenylephrine may help you weed through the differentials. The eyelid is innervated primarily through cranial nerve III and, to a lesser degree, the sympathetic muscle of Müller. Thus, the phenylephrine test can be helpful in the diagnosis and potential surgical outcome for patients with mild ptosis.
This test is performed by instilling 2.5% phenylephrine to the superior fornix and re-measuring the ptosis after 10 minutes. An improvement after phenylephrine indicates a sympathetic etiology.7 This test is an important indicator for successful Müller’s muscle resection prior to surgical repair.8
Retinal vasculature. While phenylephrine has many anterior segment applications, topical ophthalmic application may also penetrate the posterior segment and affect the retinal vasculature.
Recent studies using OCT angiography have determined that the topically administered drug can diffuse through the ocular tissues and reach the retrobulbar region, activating its vasoconstrictive properties on the short posterior ciliary arteries and the central retinal artery. The result is a significant reduction in the peripapillary retinal vessel density. As such, clinicians should be cautious when using phenylephrine in patients who already have severe damage to their optic disc vasculature.9
Table 1. Ophthalmic Uses of Topical Phenylephrine | |
| Diagnostic | Therapeutic |
|
|
Stay on Alert
As with all pharmaceutical agents, phenylephrine is not free of side effects, even with topical administration. The most common reactions include nausea, vomiting and headache.1 Systemically, it can increase blood pressure and heart rate and decrease oxygen saturation.10 While these potentially devastating side effects are more common with intravenous use, they are possible with more potent concentrations of ophthalmic versions, such as the 10% form that runs the risk of systemic absorption.
Maximum plasma level of phenylephrine is reached approximately 20 minutes following topical application, at which time patients should be carefully assessed for any adverse reactions. To limit systemic absorption, clinicians can apply digital pressure over the lacrimal sac or eyelid closure to reduce absorption through the conjunctival blood vessels and nasolacrimal duct.11
While eye care practitioners come across phenylephrine on a daily basis for routine dilations, several other ophthalmic uses are within reach as well. Phenylephrine’s unique mechanism provides many diagnostic and therapeutic capabilities, if used with caution.
1. Richards E, Lopez MJ, Maani CV. Phenylephrine. Treasure Island, FL: StatPearls Publishing; January 2020: 30521222. 2. Esteve-Taboada JJ, Del Águila-Carrasco AJ, Bernal-Molina P, et al. Effect of phenylephrine on the accommodative system. J Ophthalmol. 2016;2016:7968918. 3. Liu JC, Green W, Van Stavern GP, Culican SM. Assessing the utility of 2.5% phenylephrine for diagnostic pupillary dilation. Can J Ophthalmol. 2017;52(4):349-54. 4. Schonberg S, Stokkermans TJ. Episcleritis. 2020 Aug 10. Treasure Island, FL: StatPearls Publishing; January 2020: 30521217. 5. Agrawal RV, Murthy S, Sangwan V, Biswas J. Current approach in diagnosis and management of anterior uveitis. Indian J Ophthalmol. 2010;58(1):11-9. 6. Zaczek A, Zetterström C. The effect of phenylephrine on pain and flare intensity in eyes with uveitis. Acta Ophthalmol Scand. 2000t;78(5):516-8. 7. Koka K, Patel BC. Ptosis Correction. Treasure Island, FL: StatPearls Publishing; January 2020: 30969650. 8. Grace Lee N, Lin LW, Mehta S, Freitag SK. Response to phenylephrine testing in upper eyelids with ptosis. Digit J Ophthalmol. 2015;21(3):1-12. 9. Cheng J, Yu J, Jiang C, Sun X. Phenylephrine affects peripapillary retinal vasculature-an optic coherence tomography angiography study. Front Physiol. 2017 Dec;8:996. 10. Alpay A, Canturk Ugurbas S, Aydemir C. Efficiency and safety of phenylephrine and tropicamide used in premature retinopathy: a prospective observational study. BMC Pediatr. 2019;19(1):415. 11. Ahmed N, Riad W, Altorpaq A, Zahoor A. Ocular phenylephrine 2.5% continues to be dangerous. BMJ Case Rep. 2009;2009:bcr08.2008.0795. |

