 |
A 59-year-old man presented acutely with a red, swollen, painful left eye that had been steadily worsening for several days. He reported crusty lids upon awakening and a brownish discharge. Gross evaluation revealed periorbital edema, extreme photophobia and chronic tearing, which was worse in the left eye than the right. Palpable, but not tender, preauricular nodes were present bilaterally. He denied any recent illness or known exposure to anybody with similarly affected eyes.
Examination
His visual acuities were 20/20 OD and 20/40 OS. Biomicroscopy demonstrated extensive subconjunctival hemorrhaging the left eye, involving nearly all of the visible bulbar surface. The inferior palpebral conjunctiva displayed a notable follicular reaction, with a dense, whitish pseudomembrane in the lower cul-de-sac. The left cornea displayed mild haze, but did not stain with fluorescein, and no infiltrates were observed. The right eye also displayed a mild inferior palpebral follicular reaction and bulbar hyperemia, but no subconjunctival hemorrhage; the right cornea was unremarkable. Bilaterally, his anterior chambers were deep and quiet. His intraocular pressure was measured at 11mm Hg OD and OS. The patient was diagnosed with acute hemorrhagic conjunctivitis (AHC).
Viral Rarities
When we discuss viral pathogens within the sphere of ocular disease, the most common entities that come to mind are likely members of the Herpesviridae family, most specifically herpes simplex and herpes zoster. Beyond these, physicians recognize that the adenoviruses—members of the Adenoviridae family—are also common pathogens, implicated in a variety of conjunctival infections such as pharyngoconjunctival fever and epidemic keratoconjunctivitis. However, other viral entities may impact the eye, particularly in cases of ocular surface infection.
AHC is a comparatively rare condition when contrasted with adenoviral conjunctivitis or herpes simplex keratitis. It is attributable to specific members of the Picornaviridae family, most commonly Coxsackievirus and enterovirus strains.1-8 AHC can affect individuals of any age, race or gender, although it does appear to have a predilection for younger individuals, particularly those between ages 11 and 15 years.7 The infection is more commonly noted to occur in developing nations, or in communities of comparatively lower socioeconomic status.1-6 Epidemics have occurred in regions throughout the world since the early 1970s.1-7 Although AHC is considered uncommon in the United States, outbreaks have been noted in warm, tropical areas such as Florida.9,10 Investigators believe the viral pathogens—especially enterovirus—can survive and replicate better at higher temperatures and humidity levels.11
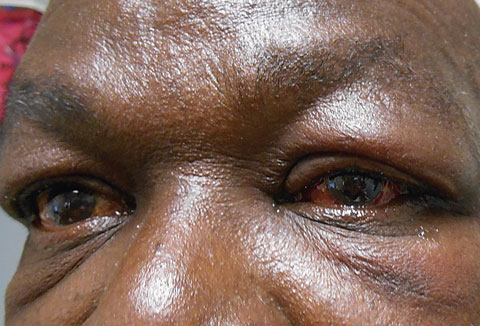 |
| This 59-year-old male patient’s symptoms began in the left eye and spread to the right eye after several days. |
The course of AHC typically begins innocuously enough, with itching and redness of the involved eye. Over the course of several days, the lids become increasingly swollen and serous discharge develops, causing lid crusting or matting upon awakening.7 The fellow eye often becomes involved at this point. Pain intensifies, photophobia ensues and a low-grade fever is possible.7 Viral-induced inflammation causes rapid dilation of small conjunctival blood vessels, which invariably rupture, resulting in petechial hemorrhages; these soon coalesce, resulting in conspicuous subconjunctival hemorrhaging that is characteristic of the disease.7 The severely red eyes, increasing discomfort, discharge and compromised vision (from ocular discharge or corneal involvement) usually prompts patients to seek medical attention within a week. Examination will reveal the aforementioned findings, as well as a moderate-to-severe follicular response, variable punctate keratopathy and, in extreme cases, subepithelial corneal infiltrates. Preauricular lymphadenopathy is also possible, though it appears to occur in less than 10% of affected individuals.7
Making the Diagnosis
Detection of AHC is often empirical and based upon the clinical presentation, history and systematic exclusion of other, similar conjunctivitides, such as bacterial conjunctivitis, epidemic keratoconjunctivitis, adult inclusion conjunctivitis and atopic keratoconjunctivitis. Laboratory testing is considered impractical in the typical clinical setting, given the rapid course and non–sight threatening nature of the infection. Collecting conjunctival swab samples and subjecting them to reverse transcription polymerase chain reaction can detect the offending pathogen.7
Patients with AHC are extremely contagious, so employ proper disinfection protocols upon examination. Patients should likewise be warned about the potential to spread the disease. As with many viral pathogens, a specific antimicrobial therapy for picornavirus infection is not known to exist, and hence there is no particular treatment of choice for AHC. Most physicians endorse palliative therapy with cool compresses and ophthalmic lubricants as needed.
Although some discourage using topical steroids (due to a fear of potential corneal superinfection), we have found that corticosteroids significantly improve symptoms in patients with both adenoviral and acute hemorrhagic conjunctivitis and when used in conjunction with a broad-spectrum antibiotic the risk of superinfection is practically nil. Hence, we often prescribe a combination antibiotic/corticosteroid four times daily for these individuals. In all cases, AHC is self-limited and the infection resolves within a week after inoculation, although the subconjunctival hemorrhage and related periorbital edema may persist for up to 14 days.8
The presence of pseudomembrane in this case was atypical, as this feature is not commonly associated with AHC. Nonetheless, practitioners should be aware of the potential for membrane formation in all cases of ocular surface infection, and must always address them appropriately. Ideally, membranes should be removed from the conjunctiva thoroughly so as to prevent contracture, scarring, foreshortening of the fornix and potential symblepharon formation. This can sometimes be facilitated by simply using a cotton-tipped applicator under topical anesthesia. In our case, however, it required the use of small tissue forceps to gently peel away the pseudomembrane; this resulted in little discomfort and no further ocular insult.
Zebra Spotting
There’s a popular metaphor in medicine that applies to diagnosis: When you hear hoof beats, think horses before zebras.
We find ourselves echoing this mantra over and over in our clinical teaching roles. Yet every once in a while, the zebra is bound to make an appearance. Recognizing key elements of rare conditions such as AHC and dealing with them appropriately can help to prevent anxiety, inappropriate therapy and poor outcomes.
Special thanks to Gregory Wolfe, OD, for allowing us to share this case with our readers.
|
1. Mirkovic RR, Kono R, Yin-Murphy Met al. Enterovirus type 70: the etiologic agent of pandemic acute haemorrhagic conjunctivitis. Bull World Health Organ. 1973;49(4):341-6. 2. Moura FE, Ribeiro DC, Gurgel N, et al. Acute haemorrhagic conjunctivitis outbreak in the city of Fortaleza, northeast Brazil. Br J Ophthalmol. 2006 Sep;90(9):1091-3. 3. Gopalkrishna V, Patil PR, Kolhapure RM, et al. Outbreak of acute hemorrhagic conjunctivitis in Maharashtra and Gujarat states of India, caused by Coxsackie virus A-24 variant. J Med Virol. 2007 Jun;79(6):748-53. 4. Khan A, Sharif S, Shaukat S, et al. An outbreak of acute hemorrhagic conjunctivitis (AHC) caused by coxsackievirus A24 variant in Pakistan. Virus Res. 2008 Oct;137(1):150-2. 5. Centers for Disease Control and Prevention (CDC). Notes from the field: acute hemorrhagic conjunctivitis outbreaks caused by coxsackievirus A24v — Uganda and southern Sudan, 2010. MMWR Morb Mortal Wkly Rep. 2010 Aug 20;59(32):1024. 6. Aubry C, Gautret P, Nougairede A, et al. 2012 outbreak of acute haemorrhagic conjunctivitis in Indian Ocean Islands: identification of Coxsackievirus A24 in a returned traveller. Euro Surveill. 2012 May 31;17(22). pii: 20185. 7. Harada K, Fujimoto T, Asato Y, Uchio E. Virological and epidemiological analysis of coxsackievirus A24 variant epidemic of acute hemorrhagic conjunctivitis in Okinawa, Japan, in 2011. Clin Ophthalmol. 2015 Jun 15;9:1085-92. 8. Langford MP, Anders EA, Burch MA. Acute hemorrhagic conjunctivitis: anti-coxsackievirus A24 variant secretory immunoglobulin A in acute and convalescent tear. Clin Ophthalmol. 2015 Sep 10;9:1665-73. 9. Sklar VE, Patriarca PA, Onorato IM, et al. Clinical findings and results of treatment in an outbreak of acute hemorrhagic conjunctivitis in southern Florida. Am J Ophthalmol. 1983 Jan;95(1):45-54. 10. Hatch MH, Malison MD, Palmer EL. Isolation of enterovirus 70 from patients with acute hemorrhagic conjunctivitis in Key West, Florida. N Engl J Med. 1981 Dec 31;305(27):1648-8. 11. Mimura T, Usui T, Yamagami S, et al. Recent causes of subconjunctival hemorrhage. Ophthalmologica. 2010;224(3):133-7. |

