
Modern cataract surgery has evolved into a remarkably brief operation with very few complications. When complications do occur, however, they may be classified into three categories by time of occurrence: intraoperative, early postoperative (first few days), or late postoperative (several weeks or months later). They may be further classified by location: anterior segment (cornea, intraocular lens and lens capsule) or posterior segment (vitreous and retina).
Complications may occur at any time during or after the procedure. When monitoring for late complications, comanaging optometrists generally see the patient at one day, one week, one month, and three months after surgery.
The following cases illustrate three late posterior segment complications that you may encounter when comanaging patients during the post-operative period.
Case One: Late CME
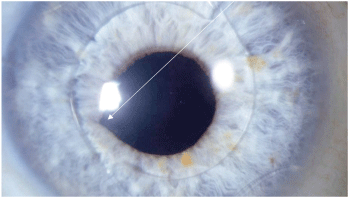
1. The right eye of a patient who developed late cystoid macular edema. Note the vitreous strand connected to the corneal inclusion, which nicks the pupil at 8:00.
This patient experienced cystoid macular edema (CME) 10 months after surgery due to a lens nucleus fragment dropping into the posterior chamber at the time of surgery.
History and diagnostic data. A 59-year-old white female presented with very dense bilateral nuclear cataracts. She postponed cataract surgery several times, and now her best-corrected visual acuity measured 20/400 O.D. and 20/200 O.S.
Her right eye was operated on first, and the surgeon noted: Hydrodissection and
hydrodelineation were performed with balanced salt solution. The phacoemulsification tip was tested and introduced into the eye. Using the divide-and-conquer technique, the lens nucleus was emulsified and aspirated. During removal of the last quadrant of the nucleus, a posterior capsule rent was noted, and the lens nucleus fell into the posterior chamber. Phacoemulsification was then immediately stopped. At this point, a retinal surgeon was called in to remove the nucleus fragment in the vitreous.
Discussion. The intact lens capsule serves as a barrier between the anterior and posterior chambers. When the capsule is broken during surgery, the incidence of posterior complications increases. A greater incidence of both retinal detachment and CME has been reported in all references to complications of cataract surgery.1
Cystoid macular edema usually occurs within the first six weeks of surgery.1 In this case, CME occurred almost one year later. The problem was not simply due to a broken capsule. During removal of the nucleus fragment that fell into the posterior chamber, a small strand of vitreous became attached to the corneal incision. Because the damaged posterior capsule could not support a posterior chamber IOL, an anterior chamber IOL was inserted after the broken capsule and lens fragment were removed from the vitreous.
Posterior chamber IOLs are removed through the anterior chamber by enlarging the original cataract incision and pulling the lens and broken capsule through. The vitreous can become attached to the lens or broken capsule, and some of it maybe dragged into the anterior chamber during this maneuver, as in this case.
A small vitreous strand became attached to the corneal incision during this procedure. It can be seen just nicking the pupil margin (figure 1). After several months, the repeated effect of trauma at the pupil margin and traction at the vitreous base stimulated enough prostaglandin release to cause a small area of CME.
A laser procedure severed the vitreous strand, and the patient was treated topically with a non-steroidal anti-inflammatory drug (NSAID) q.i.d. for one month. Following treatment, her vision returned to 20/20 at the one-month follow-up examination.
Additional discussion. The denser the nucleus, the more time and instrument energy are needed to phacoemulsify it.
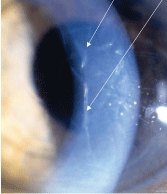
2. This patient demonstrated post-surgical endothelial striae, which were caused by corneal trauma due to an extended phacoemulsification time.
Increased time inside the eye and additional instrument energy both may contribute to a heightened risk for complications. Also, in cases in which increased phacoemulsification time and energy are required, a patient may experience a longer recovery time due to associated corneal folds, corneal edema and endothelial striae (figure 2).
The question for the referring O.D.: Should we refer cases earlier, before the nucleus becomes this dense? Earlier referral would make nucleus phacoemulsification less of a risk, because less energy would be required. Also, one study recommends earlier surgery in cases of compromised zonules, due to pseudoexfoliation.2 Because of the progressive nature of zonual weakening in psuedoexfoliation, earlier surgery decreases the risk of intraocular complications.
Case Two: Retinal Detachment
This patient experienced a retinal detachment seven months after cataract surgery.
History and diagnostic data. A 57-year-old white male underwent uneventful cataract surgery with a posterior chamber IOL implant in his left eye. The lens capsule was not broken. The initial post-op period was uneventful.
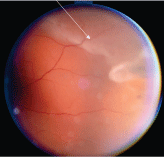
3. This patient experienced a temporal retinal detaachment O.S.
After seven months, he returned, complaining that saw more membrane material that had an arc-shape at the side of that eye.
He was dilated and found to have increased pigment in the vitreous and a temporal retinal detachment (figure 3) that had not reached the macula. He was immediately sent to a retinal surgeon, who repaired the detachment with a scleral buckle. Final corrected vision measured 20/20 at the two-week follow-up examination.
Discussion. Retinal detachment after modern cataract surgery is a rare event that usually occurs within the first few months after surgery. In more than 35 years of experience, I have noticed that a retinal detachment is far more common in younger individuals who are moderately to significantly myopic. A retinal detachment does seem to have the classic relationship to posterior vitreous detachment (PVD), as many patients younger than age 60 who have cataract surgery have not yet had a PVD.
Additional discussion. After IOL surgery, patients frequently complain of seeing flashes of light and/or new floaters. Often, the IOL edge or front surface causes photopsia, while normal floaters, which were previously obscured by the cataract, become more visible. Take these complaints seriously and investigate them.
All patients should have their pupils dilated and their vitreous carefully inspected for pigment. During IOL surgery, pigment from the posterior iris surface may dislodge and settle in the vitreous. A dramatic increase in pigment in the vitreous suggests a retinal break caused by vitreous traction. The additional pigment comes from the retinal pigment epithelium, not the iris. The presence of fluid under the break suggests a retinal detachment.
Case Three: Endophthalmitis
This patient developed endophthalmitis five months after undergoing combined cataract surgery and trabeculectomy.
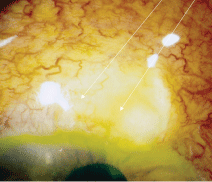
4. This glaucoma filtering surgery patient presented with an infected bleb, red eye and discharge O.S.
History and diagnostic data. A 77-year-old white male had been treated for bilateral glaucoma for several years. During the past three years, he developed a visually significant cataract in his left eye.
Neither argon laser trabeculoplasty (ALT) nor two separate glaucoma medications adequately controlled the intraocular pressure in the patients left eye.
So, his surgeon decided to remove the patients cataract and create a bleb to better control IOP. Both procedures yielded no complications.
Five months after the combined surgeries, the patient visited our clinic and presented with red eye and discharge O.S. (figure 4). He had 2+ cells in the bleb and additional cells in the anterior and posterior chambers of his left eye.
The patient was immediately sent to the glaucoma surgeon and was diagnosed with impending endophthalmitis. The surgeon hospitalized the patient, and a retinal specialist treated him with intravitreal antibiotics. Eventually, the patient experienced a total recovery and regained good vision.
Discussion. The presence of a filtering bleb poses a heightened risk for an infection over a patients entire lifetime. Within a five-year period after cataract surgery, 23% of patients may develop a bleb-related complication that could lead to endophthalmitis.6 Unlike acute endophthalmitis, which occurs in the immediate post-op period, late-onset trabeculectomy-related endophthalmitis occurs at least one to two months after surgery.3 When combating endophthalmitis, mere hours can make a significant difference in overall visual outcome.4
Late infection rates of 2% to 3% have been reported with blebs located superiorly; even higher rates have been associated with inferiorly- located blebs.5 Pay careful attention to the bleb, and monitor the patient for decreasing vision, anterior chamber cells, pain and redness.6
Additional discussion. If a glaucoma patient has a trabeculectomy and presents with a red eye, you must consider the possibility of endophthalmitis.
Following trabeculectomy, the surface of the globe is weakened, and bacteria have easier access to the inside of the eye. The patient needs to be monitored daily and treated with a broad-spectrum antibiotic or steroid/antibiotic combination. If you observe cells in the bleb, anterior chamber or anterior vitreous, immediately refer the patient to a specialist.
Cataract surgery is the single most-frequently performed ophthalmic surgery in the
Dr. Garston is a professor at the New England College of Optometry. He is also a full-time senior staff optometrist at MIT Medical Department and a founding fellow of the Optometric Retina Society.
1. Flach AJ. The incidence, pathogenesis and treatment of cystoid macular edema following cataract surgery. Trans Am Ophthalmol Soc 1998;96:557-634.
2. Bayramlar H, Hepsen IF, Yilmaz H. Mature cataracts increase risk of capsular complications in manual small-incision cataract surgery of pseudoexfoliative eyes. Can J Ophthalmol 2007 Feb;42(1):46-50.
3. Ashkenazi I, Melamed S, Avni I, et al. Risk factors associated with late infection of filtering blebs and endophthalmitis. Ophthalmic Surg 1991 Oct;22(10):570-4.
4. Smit BA. How to manage endophthalmitis in trabeculectomy patients. Rev Optom 2002 Jun;139(6):59-62.
5. Parrish R, Minckler D. Late endophthalmitisfiltering surgery time bomb? Ophthalmology 1996 May;103(8):1167-8.
6. Grewal RK. How to distinguish bleb related infections. Rev Ophthalmol 2003 Mar;10(3):61-5.

