No definitive medical treatments currently exist. So, abstaining from direct sunlight gazing for any reason is the primary preventative measure against solar retinopathy.
This article outlines two separate cases of solar retinopathy. In addition to reviewing the most current literature on the condition, we describe the typical clinical presentation and discuss a potential variant—eclipse retinopathy.
Case One
History
A 62-year-old white male presented complaining of blurred vision and associated photosensitivity in both eyes. The patient said that he first noticed these complications several years earlier.


1,
2. Fundus photographs of the 62-year-old patient described in Case One
(OD left, OS right). Note the red lesions located at both foveas.
He admitted to gazing at the sun for unknown lengths of time while under the influence of lysergic acid diethylamide (LSD).
He did not report wearing any protective filters at that time. The visual symptoms manifested shortly after the incident and have persisted ever since.
The patient’s last eye exam was five years ago. Ocular and family histories were unremarkable; however, his medical history was significant for diabetes, hypertension, hyperlipidemia and schizophrenia, as well as cocaine, alcohol and nicotine dependence.
His current medications included aspirin, hydrochlorothiazide, metformin, mirtazapine and potassium chloride. He reported drug allergies to thorazine, penicillin and haloperidol.
Diagnostic Data
On initial examination, his best-corrected visual acuity measured 20/20-2 OD and 20/25+2 OS. His pupils, extraocular motilities and confrontation visual fields were within normal limits. Slit lamp examination was significant for conjunctival pingueculas and trace lenticular nuclear sclerosis OU.
His IOP was 17mm Hg OD and 16mm Hg OS. Funduscopy revealed pink and distinct optic nerves with an estimated cup-to-disc ratio of 0.7 OU. The macular regions revealed red lesions at both foveas, and were surrounded by a well-circumscribed area of retinal pigment epithelium (RPE) hyperpigmentation (figures 1 and 2). The posterior poles and peripheral retinae were within normal limits OU.
We obtained a spectral-domain optical coherence tomography (SD-OCT) scan of the maculae and optic nerves, which revealed central RPE disruptions with an intra-retinal cyst in each eye (figures 3 and 4). Central macular thickness measured 222µm OD and 211µm OS.
Additionally, the SD-OCT scan revealed normal retinal nerve fiber layer (RNFL) thickness without any evidence of thinning OU.
Diagnosis
Based upon the patient’s history and clinical findings, we diagnosed him with solar retinopathy.
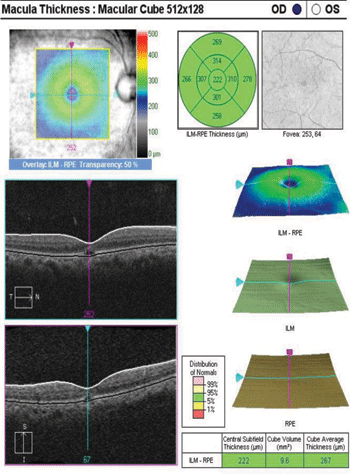
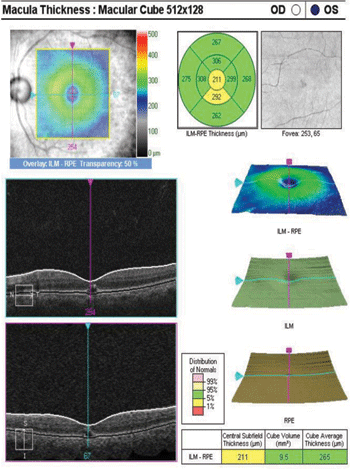
3, 4. SD-OCT scan revealed central RPE disruptions and an intraretinal cysts OU (OD left, OS right).
Case Two
History
A 64-year-old white male presented complaining of longstanding blurred vision in his left eye that did not improve with spectacle use.

5.
In Case Two, the 64-year-old patient’s left eye exhibited pigment
irregularity surrounded by an area of hypopigmentation at the macula.
At a previous eye examination, the patient reported staring at a partial solar eclipse on July 9, 1964 with his left eye, while holding his right eye closed.
After viewing the eclipse for several minutes, the patient noted seeing only “white” out of his left eye for the rest of the afternoon.
He did not report wearing any protective filters during the eclipse gazing.
His ocular history was remarkable for pigment dispersion glaucoma.
His medical history was significant for hypertension and bipolar disorder. Current medications included latanoprost, dorzolamide/timolol, atenolol, hydrochlorothiazide/lisinopril and lithium carbonate.
He reported no known allergies.
Diagnostic Data
On examination, his best-corrected visual acuity measured 20/50+1 OD and 20/25-2 OS. His pupils, extraocular motilities and confrontation visual fields were within normal limits.
Slit lamp examination revealed corneal Krukenberg spindle and iris transillumination defects OU, as well as visually significant, bilateral nuclear sclerotic cataracts (OD > OS).
His IOP measured 14mm Hg OD and 16mm Hg OS. Funduscopy revealed pink and distinct optic nerves in both eyes, with an estimated cup-to-disc ratio of 0.65 OD and 0.7 OS.
The left optic nerve exhibited superior notching and vessel barring, while the right nerve appeared healthy. The macular region of the left eye demonstrated pigment irregularity surrounded by an area of hypopigmentation (figure 5).
Again, the right macula appeared healthy. Both posterior poles were within normal limits; however, the peripheral retinae were significant for pavingstone degeneration OU.
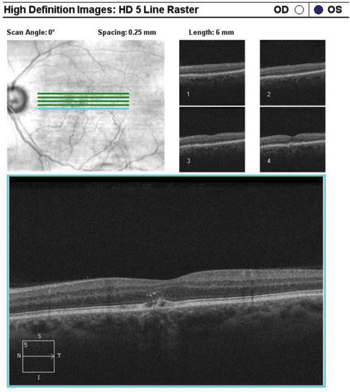
6. High-definition, five-line raster of the left eye highlighted the RPE disruption.
SD-OCT of both maculae and optic nerves revealed central RPE disruptions and a central thickness of 282µm OS.
Additional imaging using the high-definition, five-line raster highlighted the RPE disruption (figure 6).
The scans of the right eye revealed a normal foveal contour with a central thickness of 287µm.
The SD-OCT scan also revealed thinning in the RNFL superior quadrant of the right eye, as well as thinning in all quadrants of the left eye (figure 7).
A review of the patient’s previous 24-2 Humphrey visual field test showed scattered defects OU.
Diagnosis
Based upon the patient’s history and clinical findings, we diagnosed him with eclipse retinopathy.
Treatment and Follow-up
We educated both patients on our findings and firmly discouraged any future direct sunlight gazing for any reason.
We also discussed the benefits of UV-protective eyewear while outdoors.
We scheduled both patients for regular follow-up examinations every six-months to measure the stability of their best-corrected visual acuities, as well as obtain dilated fundus photographs and macular SD-OCT scans.
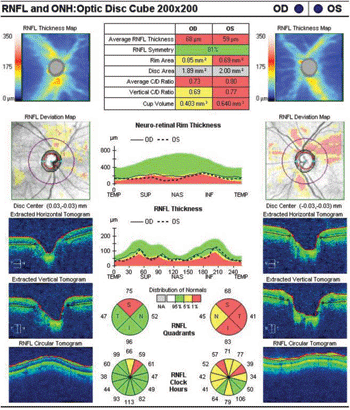
|
| 7. SD-OCT scan of both eyes revealed thinning in the RNFL superior quadrant of the right eye, as well as thinning in all quadrants of the left eye.
|
Discussion
Solar retinopathy results from retinal and macular damage secondary to direct exposure to sunlight and/or other light radiant energy. Variants of solar retinopathy that sometimes are used synonymously include eclipse retinopathy and foveomacular retinitis.
Eclipse retinopathy is a unique form of solar retinopathy that is a consequence of retinal damage sustained during solar eclipse viewing, whereas foveomacular retinitis describes the clinical characteristics of solar retinopathy without eliciting a history of solar exposure.1
The exact prevalence of solar retinopathy is unknown. This likely is because most cases are unreported due to the mild and nonspecific visual complaints following sun exposure. Nevertheless, the incidence of reported cases tends to increase following a national public announcement of a solar eclipse.2
The largest nationwide active case study was conducted by the British Ophthalmological Surveillance Unit following the full solar eclipse on August 11, 1999.3 Its researchers reported 70 cases of solar retinal injury within the UK alone. In 39% of the cases, the time spent looking at the eclipse was reported to be less than 60 seconds. The male-to-female ratio was 1.2:1.0, with an average age of 29.5 years.3 A cross-reference of smaller studies following the 1999 eclipse revealed similar trends.4
Solar eclipse gazing remains the most common reason why patients stare into the sun.5 Other explanations described in the literature include religious and cultural rituals, mental illness, hallucinogenic drug abuse, recreational sunbathing, military deployment in bright/desert environments and incidental exposure secondary to simple curiosity.1,6,7
During solar retinal exposure, most patients often report a positive afterimage with short-term dazzling sensations.1 Visual disturbances arise quickly after exposure, with varied complaints of a small central scotoma, photophobia or reduced visual acuity. In cases of severe exposure, metamorphopsia, chromotopsia and headaches with orbital and retro-orbital pain also may occur.1,4
The most common visual complaint is decreased visual acuity (ranging from 20/30 to 20/200), which generally varies with exposure severity.8,9 One study of 319 patients with solar retinopathy indicated improvements in vision to 20/40 or better in 80% of cases without any deterioration over time.5 The researchers also reported no color vision defects.5
A similar study of 70 cases revealed no permanent visual loss over a three-month duration.3 The clinical course and presentation of solar retinopathy is consistent throughout the literature. Within the first 24 to 48 hours following solar retinal exposure, clinical examination of the macula typically reveals normal to subtle pigmentary mottling and edema.
A yellow spot develops in the fovea with a loss of reflex, and a surrounding cuff of hyperpigmentation becomes more apparent within a week after exposure. The macular changes include RPE hypopigmentation, with an increase in foveal erythema after one month. Persistent macular pigmentary irregularity is observed as a longstanding change, followed by resolution of foveal erythema with or without retention of foveal RPE hypopigmentation.1,3,10,11
The mechanism of how light causes retinal damage has been studied thoroughly.1,12-14 For light to harm any part of the eye, it must be absorbed. In the human eye, the ocular media—including the cornea, aqueous, lens and vitreous—control the absorption of radiant energy from light reaching the retina.1
The transmissions through these structures remain a constant throughout life, with the exception of the lens secondary to age-related changes. Light transmission via an aging lens is reduced to longer and less harmful wavelengths, due to both reflection and scattering.12 Interestingly, cataract development can be a protective measure against chronic shorter wavelengths that ultimately cause retinal changes.1
However, the ocular media’s transparency permits light to focus entirely on the retina—particularly the macula. As a result, the retina becomes highly susceptible to light absorption and consequent damage.12
Three models of how light damages the retina have been proposed, including mechanical, thermal and photochemical methods. Mechanical and thermal disruptions are caused by absorption of shorter wavelengths that alter retinal structure. Mechanical damage produces sonic transients or shock waves, whereas thermal damage is the result of increased temperature within the retina (typically by 10ºC to 20ºC).
Neither of these processes are likely to cause solar retinopathy, and are in fact intentionally exploited during ophthalmic laser treatment (e.g., Nd:YAG and argon laser photocoagulation).12
Photochemical damage, on the other hand, results when long-wavelength blue and/or UV light is absorbed. This initiates a chain of chemical reactions that disrupt the normal physiological structure of the retina.12,13 Recent research provides evidence that solar retinopathy chiefly is caused by photochemical effects.13,14
With the development of more advanced imaging devices, the understanding of solar retinopathy’s impact on vision has improved dramatically in the last decade. Several reviews of OCT findings indicated that patients with solar retinopathy exhibit significant foveal pathology.10,15,16 In these studies, associated retinal defects were concentrated centrally at the level of the inner and outer photoreceptor segment junction.10,15,16
In another evaluation of OCT findings in patients with a history of solar eclipse retinopathy, researchers documented the presence of voids with decreased foveal thickness at the photoreceptor layer in 10 of 21 affected eyes.17 Signal defects in both the inner and outer photoreceptor segments also were observed.
In these individuals, there appears to be a strong correlation between decreased central foveal thickness and full-thickness voids on OCT analysis with reduced visual acuity.17-19 Such findings are consistent with those documented in smaller case reports using OCT analysis as a predictor of visual function in patients with confirmed solar retinopathy.11,20,21
Additionally, a retrospective, observational case series comparing OCT findings and fluorescein angiography (FA) was published in 2009.20 Most defects observed on FA revealed small punctate or pinpoint central RPE transmission, or window defects. It is worth noting that in all reported cases of definitive solar retinopathy, FA did not reveal characteristic lesions of the disease.20
Multifocal electroretinogram (mfERG), a newer electrophysiological technique that objectively maps retinal function, also has been used to screen patients suspected of solar retinopathy. One study showed that eight patients experienced a reduction in central retinal function after initial solar exposure using mfERG testing.22
At the two-month follow-up, all patients showed improvements in both visual acuity and mfERG amplitude; however, when compared to normal subjects, there was still an overall acuity reduction.22
Another study showed similar reductions in mfERG findings, with gradual visual recovery in a smaller patient population.23 The long-term effects of retinal function in patients with chronic solar retinopathy also elicited a decrease in mfERG response.23,24 These testing results accurately correlate to the clinical presentation and visual acuity outcome in solar retinopathy patients.
In addition to the retina, acute and chronic UV exposure damages other ocular structures that absorb light. The five most common sun-induced ocular disorders include: cataracts, age-related macular degeneration, pterygium, photokeratitis and periocular skin cancer.25 Other sunlight-related eye diseases include pinguecula, conjunctival melanoma, climatic droplet keratopathy, primary spheroidal degeneration and intraocular malignant melanoma.25
Ultimately, the best treatment for solar retinal damage is prevention. Adequate education on the harmful effects of sunlight on retinal tissue and other ocular media should be discussed. Appropriate referrals for psychological services should be considered for patients who continue to practice such behavior.1
Proper UV protection should be recommended for individuals who are more prone to light damage––specifically those who spend considerable time outdoors or live in an environment that receives a significant volume of sunshine throughout the year.
It is important to note that during a solar eclipse, normal sun spectacle eyewear is insufficient to protect the retina. Indirect observation (e.g., watching a live broadcast on the computer or television) is the safest course.1 Viewing with a pinhole camera also is permissible.
While treatment often is unnecessary, the use of systemic steroids has been proposed.7 However, no current clinical studies exist to confirm the efficacy of this approach.
Given a positive history of sun gazing, clinical characteristics of subtle foveal lesions confirmed via OCT and a proportionately correlated best-corrected visual acuity, you can confidently diagnose an individual with solar retinopathy. In the absence of a positive history with similar clinical findings, other conditions that involve the fovea should be considered, including age-related macular degeneration, macular holes, epiretinal membranes and hereditary macular dystrophies.
The exact prevalence of solar retinopathy is unknown, likely because most individuals fail to report mild and/or nonspecific visual complaints following sun exposure. Visual prognosis is excellent in most instances, with no treatment required. Finally, be sure to instruct all patients not to directly gaze at the sun or an eclipse for any reason.
As a public service announcement, the next solar eclipse is predicted to occur on November 3, 2013, and will be visible to inhabitants of Europe, Asia, Africa and parts of North America.26
Dr. To currently is starting an interprofessional polytrauma/TBI advanced clinical fellowship in optometry at the James A. Haley Veterans’ Hospital in Tampa, Fla. He managed these two cases during his residency at the Lake City VA Medical Center in Florida.
Dr. McGonigal is the associate chief of optometry and optometric residency coordinator at the Lake City VA Medical Center.
Dr. Patel is a resident supervisor and director of low vision services at the Lake City VA Medical Center.
1. Istock TH. Solar retinopathy: a review of the literature and case report. J Am Optom Assoc. 1985 May;56(5):374-82.
2. Tsatsos M, Eke T. Public health warnings of solar retinopathy risk in European newspapers prior to the 2006 solar eclipse. Arch Soc Esp Oftalmol. 2007 Dec;82(12):735.
3. Michaelides M, Rajendram R, Marshall J, Keightley S. Eclipse retinopathy. Eye (Lond). 2001 Apr;15(Pt 2):148-51.
4. Källmark FP, Ygge J. Photo-induced foveal injury after viewing a solar eclipse. Acta Ophthalmol Scand. 2005 Oct;83(5):586-9.
5. Rai N, Thuladar L, Brandt F, et al. Solar retinopathy. A study from Nepal and from Germany. Doc Ophthalmol. 1998;95(2):99-108.
6. Hope-Ross M, Travers S, Mooney D. Solar retinopathy following religious rituals. Br J Ophthalmol. 1988 Dec;72(12):931-4.
7. Schatz H, Mendelblatt F. Solar retinopathy from sun-gazing under the influence of LSD. Br J Ophthalmol. 1973 Apr;57(4):270-3.
8. Atmaca LS, Idil A, Can D. Early and late visual prognosis in solar retinopathy. Graefes Arch Clin Exp Ophthalmol. 1995 Dec;233(12):801-4.
9. MacFaul, PA. Visual prognosis after solar retinopathy. Br J Ophthalmol. 1969 Aug;53(8):534-41.
10. Hossein M, Bonyadi J. Spectral-domain optical coherence tomography features of mild and severe acute solar retinopathy. Ophthalmic Surg Lasers Imaging. 2011 Sep 8;(42):84-6.
11. Chen JC, Lee LR. Solar retinopathy and associated optical coherence tomography findings. Clin Exp Optom. 2004 Nov;87(6):390-3.
12. Roh S, Weiter JJ. Light damage to the eye. J Fla Med Assoc. 1994 Apr;81(4):248-51.
13. Algvere PV, Marshall J, Seregard S. Age-related maculopathy and the impact of blue light hazard. Acta Ophthalmol Scand. 2006 Feb;84(1):4-15.
14. Okuno T. Hazards of blue solar light. Appl Opt. 2008 Jun 1;47(16):2988-92.
15. Chen KC, Jung JJ, Aizman A. High definition spectral domain optical coherence tomography findings in three patients with solar retinopathy and review of the literature. Open Ophthalmol J. 2012;6:29-35.
16. Suhr CL, Buffano RM, Sellers A. The use of optical coherence tomography to aid in diagnosing solar maculopathy. Optometry. 2011 Aug;82(8):481-4.
17. Gulkilik G, Taskapili M. Association between visual acuity loss and optical coherence tomography findings in patients with late solar retinopathy. Retina. 2009 Feb;29(2):257-61.
18. Chen RW, Gorczynska I, Srinivasan VJ, et al. High-speed ultrahigh-resolution optical coherence tomography findings in chronic solar retinopathy. Retin Cases Brief Rep. 2008 Spring;2(2):103-5.
19. Cho HJ, Yoo ES, Kim CG. Comparison of spectral-domain and time-domain optical coherence tomography in solar retinopathy. Korean J Ophthalmol. 2011 Aug;25(4):278-81.
20. Jain A, Desai RU, Charalel RA, et al. Solar retinopathy: comparison of optical coherence tomography (OCT) and fluorescein angiography (FA). Retina. 2009 Oct;29(9):1340-5.
21. Klemencic S, McMahon J, Upadhyay S, Messner L. Spectral domain optical coherence tomography as a predictor of visual function in chronic solar maculopathy. Optom Vis Sci. 2011 Aug;88(8):1014-9.
22. Arda H, Oner A, Mutlu S, et al. Multifocal electroretinogram for assessing sun damage following the solar eclipse of 29 March 2006: multifocal electroretinography in solar maculopathy. Doc Ophthalmol. 2007 May;114(3):159-62.
23. Schatz P, Eriksson U. Multifocal electroretinography and optical coherence tomography in two patients with solar retinopathy. Acta Ophthalmol Scand. 2004 Aug;82(4):476-80.
24. Stangos AN, Petropoulos IK, Pournaras JA, et al. Optical coherence tomography and multifocal electroretinogram findings in chronic solar retinopathy. Am J Ophthalmol. 2007 Jul;144(1):131-4.
25. Young RW. The family of sunlight-related eye diseases. Optom Vis Sci. 1994 Feb;71(2):125-44.
26. Timeanddate.com. November 3, 2013: Total solar eclipse. Available at:
www.timeanddate.com/eclipse/solar/2013-november-3. Accessed August 7, 2013.

