An electronic medical records system may be helpful if used correctly, but can be disastrous if something goes wrong. Meanwhile, an optical coherence tomographer is quickly becoming a tool that optometrists simply cannot do without.
These are just a couple of the findings from our Annual Diagnostic Technology Survey, based on responses from 260 optometrists to an email questionnaire.
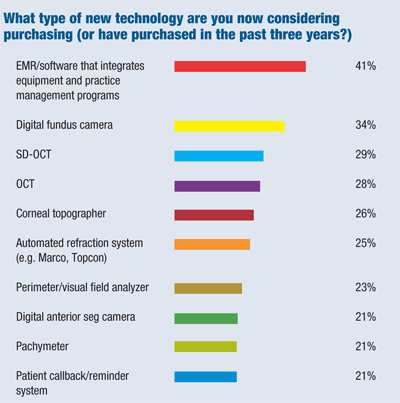
Among our questions, we asked our readers which instruments or equipment they currently want to buy or have purchased in the past three years.
The top 10 most bought or most wished-for items are:
1. EMR
EMR systems are not diagnostic equipment, of course. Still, they elbowed out the other technology-related products on our survey by a wide margin—41% of our respondents say they’ve recently bought or are looking to buy an EMR system and/or software that integrates equipment and practice management programs.
“EMR has without a doubt been the most significant improvement in the practice,” says optometrist James Budd, of Monroeville, Pa. “There are some growing pains, but it’s infinitely better than paper.”
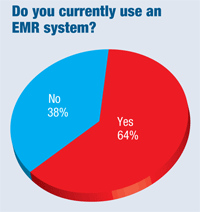
Indeed, as many as 64% of respondents now use an EMR system. Compare that to just 39% in 2009—which was the year that Congress passed the Health Information Technology for Economic and Clinical Health (HITECH) Act to promote the adoption and “meaningful use” of health information technology.
As you know by now, the HITECH Act provides financial incentives for those who use a certified EMR system. On the other hand, the act will reduce Medicare and Medicaid reimbursements for those who cannot document “meaningful use” of such a system by 2015.
The HITECH Act is worthy in spirit; but in practical terms, reaction to the requirement that doctors embrace this technology has been hit or miss.
“Eight new computers and [a leading EMR/practice management system] were purchased in the last quarter of 2011 to take advantage of certain Federal tax deductions and tax credits,” says Ira J. Cohen, O.D., of his Lake Worth, Fla., practice. “So far, it has created a lot of stress in the office and dissension among the staff members.”
Many doctors complain of losing days of data if the system goes down. Optometrist Larry Gunnell of Wichita Falls, Texas, voices another common complaint: “Sometimes I feel more like a proofreader than a clinician. Autofill is a real problem when it comes to lens prescriptions.”
Fortunately for many practitioners, the technology actually does what it’s supposed to do.
“I wanted to be more organized, with better capability to recall charts and data,” says William Jackson, O.D., of Lake Jackson, Texas. “This purchase has done just that. It has also allowed the office to be more organized and more consistent in billing and coding.”
2. Digital Fundus Camera
About one-third (34%) of O.D.s who responded to our survey now own or are considering a digital fundus camera.
Robert Buonfiglio, O.D., of Saugus, Mass., recently bought one. “While I’m hoping it enhances revenue, it also allows me to show patients the insides of their eyes,” he says. “For patients with diabetes, I now send photos with any changes labeled to their primary care doctors. It’s my hope that doing this will produce more referrals, not only for diabetic evaluations but for red eyes, foreign bodies, etc.”
Lamont P. Freeman, O.D., sees a large number of patients with diabetes at his clinic in Brooklyn. “The adage, ‘A picture is worth a thousand words,’ is not just a saying. It’s very real,” he says of his digital fundus camera. “All [of our] recommendations are accepted by patients after they view their fundus.” Additional benefits include increased income, better patient flow, increased number of patients and increased utilization of services, he says.
Kenneth R. Mueller, O.D., of Hannibal, Mo., appreciates the usefulness of the Pictor (Volk Optical), a new handheld, portable anterior and posterior camera. “It offers nice photographic capabilities for mobility-challenged patients in an ergonomic and affordable device,” he says.
3. & 4. SD-OCT and TD-OCT
Optical coherence tomography is not officially part of the standard operating equipment for optometric practices—yet. But once optometrists get an OCT, they wonder how they got along without it.
Specifically, 28% of our respondents own or want to own a time-domain (TD) OCT, and 29% voiced the same interest in a spectral-domain (SD) OCT. (Respondents were allowed to choose more than one option in the survey.)
Paul Heersink, O.D., of Monte Vista, Colo., says the SD-OCT is the single best instrument purchase he’s ever made. “It gives me unparalleled confidence in managing retinal conditions. It improves my ability to educate my patients on their retinal condition [by] showing the problem in a way that they can more easily understand,” he says.

Furthermore, Dr. Heersink adds, “as a rural practitioner in solo practice, it has been invaluable to me because I often have to make the call to send someone three to four hours away for a referral. Now I know whether it’s necessary or not because I’ve already sent it to the retina specialist for his opinion.”
Unfortunately, the billing for an OCT changed in 2011 from a single-eye test to a bilateral one, effectively cutting the reimbursement fee in half. “With the cut in reimbursement, the instrument is not paying for itself,” says optometrist Bob Day, of Garland, Texas. “But I am able to better care for my patients.”
Expanded indications for OCT can help to defray the cost while continuing to improve care. Although OCT traditionally had been reserved for retinal disease diagnosis, it has lately made inroads in the management of other conditions. For instance, newer software modules can analyze retinal nerve fiber layer dropout and ganglion cell loss in glaucoma, as well as corneal thickness and the anterior segment angle.
“The OCT that we bought last year has increased referrals and has improved patient care dramatically,” says Todd Cohan, O.D., of Long Grove, Ill. “We have been diagnosing glaucoma suspects way ahead of time and are able to provide more preventative eye care. The patients have been more than impressed. As a result, our medical billing has increased with more medical follow-up exams.”
5. Corneal Topographer
Some 26% of our respondents recently have purchased or are considering a corneal topographer. Optometrist Michael Raff of Brockport, N.Y., got one last year. “We increased contact lens fit/refit fees by $5, which offset the cost for the instrument while upgrading the technology,” he says.
Jared Hadlock of Montrose, Colo., bought a three-in-one topographer/autorefractor/keratometer. “We needed a new AR and wanted a topo, so it was a great way to knock out two birds with one stone for not much more in price than just an AR,” he says. “We’ve been able to find more keratoconus patients than we originally thought we had. It has definitely added a ‘wow’ factor for patients as well. It’s easy and does all the measurements at one time, so it’s quick, too.”
6. Automated Refraction System
Twenty-five percent of optometrists have bought or want to buy an automated refraction system. Matthew Stanley, O.D., recently added it to two exam lanes in his Manhattan, Kan., office. “I save nearly five minutes per patient on refraction,” he says. “The patients are wowed by the technology and love seeing the difference between their old and new Rx.” This effect has boosted his optical sales, he adds.
Carlton Chan, O.D., of Solana Beach, Calif., realized a dramatically different benefit: “The Marco TRS saved my career. It solved all my back problems.”
7. Perimeter/Visual Field Analyzer
If you want to diagnose and treat glaucoma, you need a perimeter. And 23% of our respondents are “scouting the field” for one. Some doctors, such as Michael Lange, O.D., of Ocala, Fla., went for the added investment of a visual field analyzer. “It’s highly sensitive for detecting early glaucoma field loss,” he says. “Patients love it and I trust it. It can perform a billable full-threshold test on a new patient in around four minutes, get better dependability indices for many patients, and give me better decision-making data on those ‘iffy’ early suspects.”
8. Digital Anterior Seg Camera
“We have done posterior segment photos for many years, and anterior seg photography is a logical and practical extension of posterior seg documentation,” says Larry Cusma, O.D., of Scotia, N.Y. Other optometrists appear to think the same—about one in five (21%) have recently bought an anterior seg camera or are looking to buy one. “It’s a great device for showing patients their ocular pathology of the anterior seg, and reinforcing the need for regular exams and follow-up monitoring,” Dr. Cusma says.
9. Pachymeter
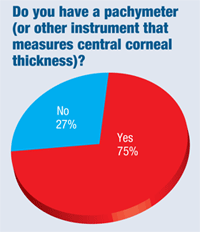
Three out of four optometrists (75%) say they now have a pachymeter (or other instrument that measures corneal thickness). That’s up from about two-thirds (68%) who reported they had one in our 2010 survey. About 21% of our respondents are in the market for one.
“It’s amazing how the pachymeter affects how I view whether or not someone is a glaucoma suspect,” says Lorelei Zeiler, O.D., of Caledonia, Ontario. “If the patient has large discs, large cupping or higher IOPs (20mm Hg to 24mm Hg) but thick corneas—no worries. Thin corneas? Yes, worry!”
10. Patient Callback/Reminder System
About one in five (21%) respondents recently obtained or are shopping for one of these patient retention systems. The connectivity with EMR systems and the high-tech advancements—such as sending a text message to a patient’s smartphone—has led to renewed interest and savings in this practice management technology.
Ten percent of our respondents say that increasing revenue is their most important reason for buying new equipment. While adding revenue is always an important consideration, this statistic takes a distant second place compared to improving patient care—77% of O.D.s say this is their primary reason for investing in new technology.
• Specular microscope. “The utilization and reimbursement make this technology a financial ‘home run,’” Dr. Gunnell says. •
Handheld tonometer. “We bought the Icare tonometer to replace the
non-contact tonometer (NCT) as a screening device used by the
technician. Patients love it,” says Suzanne Corbitt of St. Johnsbury,
Vt. “It is so much easier to get an IOP reading on children (and adults
alike) who are very apprehensive about the NCT or even the Goldmann
tonometer. It gets the technician more involved with the exam and it has
made the overall exam that much more efficient for the doctors.” •
Patient education system. “I can create or upload practice or product
info into these displays, and people love to watch them—no one can
resist a TV screen [in the waiting room],” Dr. Lange says. “Now I get
asked about new products or services by an open-minded patient instead
of having to ‘pitch’ a product or treatment…[and] I don’t have to waste
chair time doing it.”
Other Hot Items
• Wide-field scanning
laser ophthalmoscope. “The Optomap (Optos) has greatly impacted my
practice,” says Marcia Leverett, O.D., of Virginia Beach, Va. “It has
increased my revenues, helped in diagnosing retinal disease and helped
me to start thinking in an even more medically-oriented way for my whole
practice. I would not want to practice without it now.”

