With 74 million baby boomers born between the years of 1946 and 1964, it comes as no surprise that a great deal of these patients are now looking for presbyopic solutions.1
In an ideal world, our patients would love for us to just wave a magic wand and restore the accommodative ability of their crystalline lenses. But instead, we resort to running down the list of their options, each with pros and cons, and letting them choose whatever seems like the best one. The problem is, none of the options are just perfect. Sometimes it seems easier to stop after explaining progressive add lenses, and get them to the optical already.
But now more than ever, technology has advanced to a point where viable options do exist. And with the number of multifocal lens fits increasing more than 136% since 2005, the time to adapt your practice to this growing demographic is now.2,3
So, how can you incorporate the sometimes challenging and time-consuming task of fitting your presbyopes in multifocal contact lenses (MFCLs)?
Unfortunately, there are many ways to go wrong. Here are some of the most commonly made mistakes (in no particular order)—and ways to circumvent them:
1. Don’t tell your emerging presbyopes about multifocal lenses.
A sure way to guarantee that you won’t fit any multifocal lenses is to never talk about them! And, there’s no question that, by the time you’re done with an exam and explained the options to the patient (for the 10th time that day!), it can be tempting to just the leave out the whole discussion.
I understand: There just seems to be so many things to educate our patients about. Have you ever finished with the exam, dropped the patient off in optical, and then your optician comes back saying, “We’re all done with glasses selection, but he/she would really like a contact lens fitting, too”? How can you remedy that situation? Luckily, there are several ways to plant the idea in the patient’s head long before you’re running down the laundry list of options:
- Utilize your waiting room. The waiting room is a perfect place to subtly inject the idea of MFCLs into the patient’s psyche. Especially if you have a sub-waiting area. At my practice, we leave the general waiting room mostly free of marketing material, and instead place those materials in the sub-waiting area. Typically, patients are more concerned with filling out paperwork or socializing with other patients when they first arrive.
But once they’ve begun their exam, spent some time with our staff, and are dilating, they are (hopefully) in the mode of getting their eye exam. At this point, carefully placed posters, brochures, or even custom-made signage directing patients to ask you about MFCLs work nicely. - Utilize your support staff. Think about it––do your patients spend more time with you, or more time with your staff? There are many ways staff members can let patients know that MFCLs may be an option for them. One example: while the technician enters the patient’s age or chief complaint of “blurred vision at near,” he or she may simply say, “Have you heard that there are contact lenses for that nowadays? Make sure to ask Dr. Denton if you’re a candidate.”
2. Don’t address comfort issues!
An estimated 20 to 30 million Americans have early-stage signs or symptoms of dry eye, with the disease being more common in older individuals (45 years and older).4 Also, contact lenses have been shown to increase dryness. Silicone hydrogel lenses, preferred because of the health benefits they provide, are also an inherently hydrophobic material. And, despite lens manufacturers’ efforts to create a hydrophilic surface, lenses tend to revert back to being hydrophobic after a few hours of wear.
If we don’t have a discussion with these patients regarding comfort, we risk losing them after they get home and the lenses lose wettability, thus changing the lid interaction with the lens, the stiffness or modulus of the lens, and the comfort. It’s best to make sure the patient knows that comfort might become an issue—and if it does become an issue, what they can do to make lens wear tolerable.
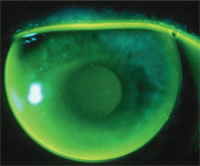
Improved stereoacuity is one reason for the increased popularity of multifocal contact lenses, as seen in this patient with a well-fit aspheric multifocal gas permeable lens. Photo: Edward S. Bennett, O.D.
The first variable to consider in keeping a lens comfortable is the contact lens solution. Luckily, there are several good options to enhance patient comfort. Specifically, hydrogen peroxide solutions have produced favorable results for patients with wearing discomfort. This solution seems to work even better if the patient is sensitive to solution preservatives.
Newly released solutions that contain surfactants and increase the wettability of lenses can also be the key to keeping patients comfortable in their lenses for the long term.
It’s also important to educate MFCL patients about appropriate artificial tears. In fact, there are some artificial tears that they will want to avoid, because certain tears can actually affect the lens modulus and alter vision. In general, I like to prescribe tears that contain a natural wetting agent (such as hyaluronic acid) or are preservative-free.
3. Allow the patient to expect “perfect” results.
There’s no better way to fail at MFCL fitting than to let patients think that their lenses will do what their crystalline lens used to.
Also, if you don’t take the time to find out what patients spend their time doing, you will very likely miss the mark in fitting their lenses. Possibly the singlemost important step in selecting the right patients for a multifocal fit, and ensuring that they will have success, is letting them know what can be expected from these lenses.
I learned from some very good mentors that this phrase works well: “My goal is to get you through most tasks, most of the time. If you’re looking to settle in with a good book and read for six hours or drive a long way at night, your progressive add lenses will be a better bet. But, if you want to be able to do most things—sit down to dinner and not have to pull out reading glasses, for example—then I can most likely make you happy.”
In other words, make sure the bar is so low that they have to trip over it!
4. Test monocular acuties, and allow the patient to compare acuities monocularly.
At least once a week, I encounter a patient who swears he loves his lenses, except one eye is better than the other at near/distance, or both! It reminds me of the old joke: “Doc, it hurts when I do this!” The inevitable punchline: “Well then, stop doing that!”
When fitting MFCLs, test monocular acuities and ensure neither eye is lagging behind. But, above all, emphasize to the patient that the new rule is: Use both eyes at all times! One eye may be skewed toward distance and the other toward near, but they will always perform better together.
5. Don’t use real-world examples in your exam room.
Remember, you live in a black and white world in your exam room. When the patient leaves, she does not live in a black and white world. Color and contrast needs are extremely variable from patient to patient, and it helps to find out what their specific needs are.
I believe that there’s no substitute for the good ‘ole “college try”—in other words, at least one week of wearing the lenses in their world to see if they are performing well. Often, I preface a patient’s week trial of their lenses by saying, “OK, these are working well in my exam room, but let’s see how they perform in your world. Pay attention to how they are working and we will address any issues when you return.”

Use visual aids and images to help better explain multifocal contact lenses to potential patients. Image: Eyeimaginations.
In addition, keep magazines, phone books, newspapers or other reading materials in the room for some real-world trials. Maybe you could even install a street sign at the end of a long hallway in your office? (Just kidding!)
6. Don’t learn about different multifocal options.
We all have our go-to lens, but what happens when it just isn’t working? If you don’t know the alternatives, you might inadvertently cause a dropout.
Soft multifocal lenses are designed using the concept of simultaneous vision. This means that the patient is viewing distance and near images at the same time. When two distinct images fall on the retina concurrently, the patient loses a bit of contrast sensitivity and gains stereopsis. (Which is, by the way, something to mention when comparing these lenses to monovision.)
There are currently two types of simultaneous vision lens designs: concentric and aspheric.
- Concentric lenses utilize a distance or near optical zone, which makes pupil size and lens centration critical for the fit. These come in distance-centered, near-centered, pupil-intelligent and aspheric-blended varieties. These lenses tend to work best for emerging or early presbyopes with low add powers.
- Aspheric designs offer a gradual change in power from the center to the periphery. They have either an anterior surface or posterior surface aspheric design, and they work particularly well for modified monovision.

Soft multifocal lenses are designed for simultaneous vision, in which light rays pass through distance and near zones at the same time. Multifocal lenses are designed with aspheric curves (left) or concentric configurations (middle, right).
The availability of two lenses of similar design having different power gradients provides the ability to overcome problems related to poor contrast sensitivity. Poor contrast sensitivity (as opposed to improper lens power) may be the indication for a particularly sensitive patient’s inability to achieve satisfactory distance vision.
7. Don’t be selective—try MFCLs on everyone!
Before you travel down the MFCL road, be sure to know the patient’s expectations. As I said before, they work for “most patients most of the time.” But certain presbyopes may suffer from severe dry eye, work in a meticulous environment that requires perfect vision and contrast sensitivity, or just may not be good candidates for various other reasons.
There’s no substitute for getting to know your patients’ needs and expectations. Do this with face-to-face time or a simple questionnaire to facilitate quicker screening.
8. Don’t over-refract.
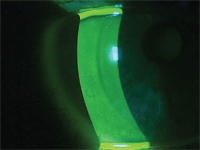
Make
sure the fit is legit. This patient’s multifocal RGP, which sat nasally
on the right eye, was fitting too tightly. Notice the indentation of
the lens on the temporal cornea after its removal. Photo: Mile Brujic, O.D.
As great as it would be if we could empirically select a lens and achieve visual perfection right off the bat, it is almost always necessary to implement some sort of over-refraction. I find that using the phoropter for these situations is not the most effective strategy. Nor is pulling out your entire trial lens set from optometry school and ending up with 50 loose lenses strewn about.
Use simple flipper bars, purchased or acquired from various contact lens manufacturers, and perform quick trials for the patient by using real-world materials rather than black-on-white charts. Remember, we’re trying to get the patient away from focusing on these charts. Sure, I want the patient to be 20/20, but sometimes as long as they’re 20/Happy (and meeting minimum visual acuity requirements, of course), then I’ve done my job.
9. Don’t be proactive.
As with just about everything, it’s up to you to ensure that you build a successful multifocal lens practice. Discuss the idea of contact lenses and offer the patient a quick trial of contacts to use in-office while picking out glasses. Once the lenses are in, and the patient sees how comfortable they are and how much more clearly they can see, you’ve planted the idea of contact lenses.
Then, remove the lenses before they leave, and give them the option of scheduling a fitting.
10. Do it all yourself.
Make sure your team knows your goals in establishing your practice as the place to go for clear vision at all distances without relying on glasses. Get them excited about it by fitting your presbyopic employees and let them sing your praises. Designate your contact lens technician to do simple trial lens over-refractions when possible.
Successfully fitting multifocal lenses is a big practice-builder and has the potential to generate patient referrals—while giving patients real solutions without having to leave your practice.
Dr. Denton is in private practice in Burnsville, N.C. She is a fellow of the American Academy of Optometry, an executive board member of the Ocular Surface Society of Optometry, and director of mentorship for Women of Vision.
1. U.S. Census Bureau. U.S. Interim Projections by Age, Sex, Race, and Hispanic Origin: 2000-2050. Available at:
www.census.gov/population/www/projections/usinterimproj. Accessed September 2011.
2. inVentiv Advance Insights Contact Lens Report. Data ending December 2010.
3. Cleveland Research Company. 2009. Third Quarter 2009 Contact Lens Research Summary. Press Release.
4. Moss SE, Klein R, Klein BE. Prevalence of and risk factors for dry eye syndrome. Arch Ophthalmol. 2000 Sep;118(9):1264-8.

