Frequently, corneal sutures are used following various intraocular procedures—such as cataract surgery, glaucoma drainage device insertion, retinal detachment repair and full-thickness penetrating keratoplasty (PK)—to seal the open wound and protect the eye from outside pathogens. Typically, the sutures remain attached and cause no complications.
But, in some cases, they can be problematic. Suture abscesses can develop, which allow bacteria into the anterior chamber.1 Or, the patient’s own normal flora can cause microbial keratitis following suture removal.2 Ultimately, however, patients with suture-related infections can develop endophthalmitis, which could possibly lead to permanent vision loss.3
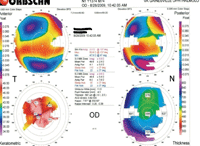
1. Corneal topography revealed a steep area of corneal astigmatism at 137° in our patient’s right eye.
With a better understanding of the potential suture-related sequelae, the clinician can quickly detect and treat any infections that may occur.
Here, we discuss a case of endophthalmitis following routine suture removal and review current management and treatment options for this devastating condition.
History
An 80-year-old white male presented to the Gainesville, Fla., VA Medical Center cornea clinic for a routine follow-up evaluation. His ocular history was significant for PK O.D. in 2005 secondary to pseudophakic bullous keratopathy, pseudophakia O.U. (anterior chamber IOL O.D., posterior chamber IOL O.S.) and the presence of an involuted bleb with iris prolapse O.S. He was using Pred Forte 1% ophthalmic suspension (prednisolone acetate, Allergan) q.d. O.D. to prevent graft rejection. His medical history was significant for colon carcinoma (for which he was receiving chemotherapy), hypertension, angina, back and shoulder pain, and chronic obstructive pulmonary disease (COPD). He had no known systemic or drug allergies.
Diagnostic Data
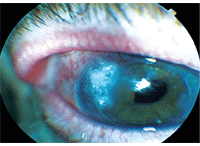
2. Slit lamp examination showed a clear graft and an overlying bandage contact lens.
His best-corrected visual acuity (with spectacles) was 20/60 O.D. with -6.75+2.75D x 133 and 20/25 O.S. with -2.00+0.50D x 10. Pupils were irregularly peaked inferotemporally O.U., with no afferent defect. Intraocular pressure measured 13mm Hg O.D. and 18mm Hg O.S. at 8:52 a.m.
Anterior segment evaluation revealed a clear graft with intact interrupted sutures, a pterygium located nasally and an anterior chamber IOL O.D., with a moderate amount of capsular opacification. Dilated fundus examination was unremarkable, except for the presence of a single dot hemorrhage located superonasally in the mid-periphery of the left eye.
During this visit, corneal topography on Orbscan (Bausch + Lomb) showed a steep area of corneal astigmatism located at 137° in his right eye (figure 1). Another suture located at 47° appeared loose and required removal. So, one suture was removed at each of these areas. (We instilled one drop of Betadine [povidone-iodine 5%, Purdue Pharma] solution before pulling the sutures.) Subsequently, we instructed the patient to use both Ocuflox (ofloxacin, Allergan) and Pred Forte 1% q.i.d. O.D. for four days, and then continue with Pred Forte 1% q.d. only. He was scheduled to return in six to eight weeks for topography assessment and manifest refraction.
Three days later, the patient returned to the clinic complaining of floating lines, spots in his vision, pain, photophobia, tearing and a yellow discharge in his right eye. His best-corrected visual acuity was hand motion O.D. and 20/20-2 O.S. He reported good compliance with Ocuflox and Pred Forte 1% q.i.d. O.D. Intraocular pressure measured 26mm Hg O.D. and 19mm Hg O.S. Anterior segment evaluation of his right eye revealed grade 2 to 3+ conjunctival injection, a hazy graft with intact sutures, a 3mm by 3mm ulcer located superotemporally with indistinct borders that encompassed the host-graft interface with surrounding mucous, and a 1.3mm high hypopyon in the anterior chamber. A dilated fundus exam revealed a cloudy vitreous; however, the remaining fundus structures were difficult to assess secondary to the hazy media. A B-scan ultrasound revealed vitreous debris, but no signs of retinal detachment.
At this point, we made a tentative diagnosis of corneal ulcer with suspected endophthalmitis secondary to suture pull O.D. We performed a corneal scraping and cultured on blood, chocolate, Sabouraud and thioglycolate agars. Gram and Giemsa stains were also performed. Immediately, we started the patient on topical fortified tobramycin 1.4% qh, topical vancomycin 2% qh (alternating between the two) and Vigamox (moxifloxacin, Alcon) six times a day. He was seen by a retinal specialist the same day, where he received a vitreous tap and intravitreal injections of vancomycin, ceftazadime and dexamethasone. He was then seen every one to three days for follow-up.
At seven days following the suture pull, his best-corrected visual acuity was finger counting at four feet O.D. Anterior segment evaluation now revealed the epithelial defect to be 3.5mm by 3.7mm in size, and there was dehiscence with a positive Seidel test at the graft-host interface. Additionally, we noted a 1.7mm-high hypopyon mixed with red blood cells. Culture results (of the corneal scrapings and vitreous tap) were positive for methicillin-sensitive Staphylococcus aureus. The patient was glued at the graft-host interface using Iso-Dent (Ellman International) sealant, and a bandage contact lens was placed over the cornea. We instructed him to continue using fortified tobramycin 1.4% q.i.d., vancomycin q2h (upon waking) and Pred Forte 1% b.i.d. Additionally, we started him on Cyclogyl (cyclopentolate, Alcon) b.i.d. as well as 100mg doxycycline b.i.d. and 1,000mg vitamin C b.i.d.
By 18-day follow-up (21 days following suture pull), his best-corrected visual acuity had improved to 20/200 O.D. Anterior segment evaluation revealed mild epithelial haze at the graft-host interface, the ocular adhesive was still in place with an overlying bandage contact lens, and there was grade 2 to 3+ cells in the anterior chamber. The corneal ulcer and endophthalmitis appeared to be resolving nicely. We advised him to stop using fortified tobramycin 1.4%, vancomycin, doxycycline and vitamin C. We then instructed him to start using tobramycin 0.3% q.i.d. and continue dosing the Pred Forte 1% and Cyclogel b.i.d.
At one-month follow-up (33 days following suture pull), his best-corrected visual acuity measured 20/80 O.D. Slit lamp exam revealed a clear graft with intact glue superotemporally and an overlying bandage contact lens (figure 2). The anterior chamber was deep with trace cells. We instructed him to continue using tobramycin 0.3% q.i.d. and Pred Forte 1% t.i.d.
Over the next two months, the patient had difficulty returning to the clinic due to other health conditions, but he continued to wear the bandage contact lens during that time. When the patient returned, the bandage contact lens and the ocular adhesive were easily removed with a jeweler’s forceps without complications. The area underneath the adhesive appeared vascularized and the epithelium was intact. He was instructed to continue using Pred Forte 1% t.i.d. to prevent a graft failure and to aggressively lubricate the eye with preservative-free artificial tears. We scheduled him to be followed in the cornea clinic every month to monitor his condition.
Discussion

• Clinical features. Although there are several subtypes of endophthalmitis, the most commonly presenting sign is markedly decreased vision.4 Ocular findings usually include an intense conjunctival injection, chemosis, eyelid edema, and often a mucopurulent discharge. Other clinical signs indicative of endophthalmitis include hypopyon, severe anterior chamber reaction, vitreous cells and haze (vitritis) and a decreased pupillary red reflex.5 Progressive vitritis is a standard sign in any presenting case of endophthalmitis.4 In the Endophthalmitis Vitrectomy Study (EVS) conducted on 420 postoperative patients between 1990 and 1994, 86% of the study patients exhibited a visual acuity of less than 5/200; 86% had a hypopyon; almost 80% of patients had no retinal vessel on indirect ophthalmoscopy; and 67% of patients had an undetectable red reflex.6
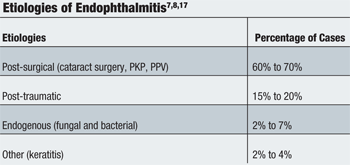
• Etiology. Endophthalmitis generally is classified as being exogenous or endogenous, depending on where the source of the pathogen originated. Exogenous endophthalmitis generally occurs following ocular surgery (postoperative) or following ocular trauma (post-traumatic).7 Endogenous endophthalmitis occurs systemically when infectious organisms travel through the blood stream from a distant location in the body to cross the blood-ocular barrier and enter the internal ocular spaces.8 Although uncommon, other causative conditions or procedures, such as bacterial keratitis, corneal suture removal or intravitreal anti-VEGF injection, have been reported.9 (See “Etiologies of Endophthalmitis”)
Typical causative agents vary based on the subtype of endophthalmitis. The EVS results indicated that postoperative endophthalmitis normally results from infection by gram-positive organisms, such as coagulase-negative Staphylococcus epidermidis, coagulase-positive Staphylococcus aureus and the Streptoocccus species.4 Post-traumatic endophthalmitis cultures show Bacillus and Staphylococcus aureus species in 95% of eyes, with a few cases attributed to S. Epidermidis and the Streptococcus species.4 Endogenous endophthalmitis may be caused by bacteria, fungi or, in rare instances, parasites.4 (See “Organisms Involved in Endophthalmitis”)
The human body intermittently harbors many strains of Staphylococci, and most of the time, these bacteria do not cause symptoms. S. epidermidis is the species most pathogenic to humans, followed by S. aureus and S. saprophyticus.10 Staphylococcus aureus is unique because it has the ability to produce coagulase, an enzyme that induces clot formation. S. aureus has been attributed to several deadly human diseases, such as toxic shock syndrome, endocarditis and pneumonia. Ocular findings caused by S. aureus include blepharitis, conjunctivitis, ulcerative keratitis, hordeola, dacryocystitis and endophthalmitis.10 Despite the presence of coagulase, there is no substantial evidence to suggest that coagulase is the exact cause of the pathogenicity.10
Research is still emerging regarding the precise molecular and cellular events that occur during endophthalmitis. Bacteria that gain entry into the interior portion of the eye can replicate with relative impunity due to the immunologically privileged nature of the eye.11 During the growth phase, these virulent organisms produce toxins that are harmful to retinal function.11
Additionally, the presence of organisms in these immune-deprived areas causes intraocular inflammation. During this inflammatory period, materials such as cell envelopes, peptidoglycan fragments and teichoic acid or lipopolysaccharide are shed into intraocular spaces, likely as a result of bacterial cell death from antibiotics or from bacterial growth. These toxic materials may stimulate other immune cells to produce cytokines and perpetuate the inflammatory response. This continuous reaction leads to increased permeability of the blood-ocular fluid barrier and causes a surge of inflammatory events.11 During the later stages of endophthalmitis, lymphocytes migrate into inflamed intraocular tissues and cause an immunoglobulin response. Further progression of endophthalmitis can lead to major ocular damage, including panophthalmitis, corneal perforation, and possibly phthisis bulbi in the end stage.4
As previously mentioned, corneal sutures are a risk factor for the development of microbial keratitis, which can progress rapidly to endophthalmitis. They can act as a source or a “wick” for bacteria, while the suture tract provides a conduit for bacteria to enter the eye.12 Loose or broken sutures can lead to abscesses and endophthalmitis.1,13 Abscesses occur as a direct result of sutures extending beyond the corneal epithelium, allowing bacteria to easily invade the corneal stroma.1 Sutures are commonly placed anterior to Descemet’s membrane, which may permit bacteria to travel from the tear film into the anterior chamber.1
Early case reports described examples of endophthalmitis following suture removal after PK that were associated with wound dehiscence.14 These reports indicated that use of fine suture material, corticosteroids and chronic topical antibiotics as well as early removal of corneal sutures and lack of septic techniques both before and after suture removal are predisposing factors to wound dehiscence and subsequent infection.14
While most reports of bacterial endophthalmitis following corneal suture removal identified the patient’s normal external flora as the causative agent, only one case reported Clostridium sordellii endophthalmitis 19 days after an exposed suture was removed.15 That patient reported dirt and soil exposure at work, which likely introduced C. sordellii onto the exposed suture or into the suture track at the time of removal.
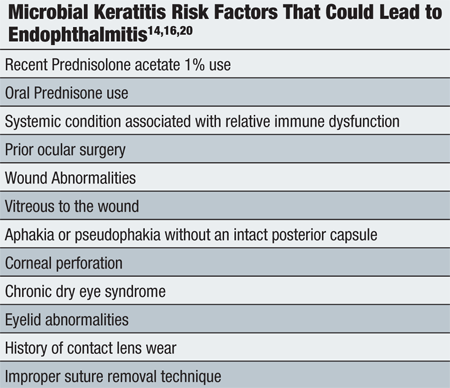
Other postoperative risk factors for microbial keratitis and further endophthalmitis include topical or oral corticosteroid use, systemic conditions associated with a relative immune dysfunction (such as diabetes and leukemia), lack of an intact posterior capsule, dry eye, wound abnormalities and/or corneal perforations.16 The patient described above instilled Pred
Forte 1% q.d. O.D. as a maintenance dose to prevent graft rejection, which may have contributed to the development of microbial keratitis and endophthalmitis. (See “Microbial Keratitis Risk Factors That Could Lead to Endophthalmitis”)
Prophylaxis and Prevention
Prophylactic measures prior to suture removal must be employed in order to provide a normal healing process and to make every attempt to prevent such an unfavorable outcome.
Topical povidone-iodine 5% is well known for having strong antimicrobial activity with minimal toxicity. In the United States, preparation of the eye with topical povidone-iodine 5% before cataract surgery is common. With regard to suture removal after penetrating keratoplasty, ophthalmologists commonly use a topical broad-spectrum antibiotic both before and after the suture is removed. But, one report suggested that povidone-iodine 5% solution should be used in addition to antibiotic drops and sterile technique prior to suture removal to prevent endophthalmitis.22
Loose and exposed sutures occurring after cataract surgery or corneal transplantation must be monitored vigilantly or removed to prevent serious complications, such as microbial keratitis. Patients with ocular surface disease require close monitoring with fluorescein staining because they are at risk for sutures surfacing through the epithelial layer.2
Advanced age has been reported as a risk factor for delayed wound healing, and should be considered prior to suture removal.3,20 In one such reported case, it was unclear whether the patient’s general immune status played a role in his ocular pathology, because he was being treated for colon cancer. Such associations should be considered in patients with a history of cancer, organ transplantation, diabetes, HIV, or other predisposing medical conditions.
Management and Treatment
Any suspected case of endophthalmitis warrants urgent medical attention. Whether the cause is postoperative, post-traumatic or endogenous, the initial evaluation is the same, including scrupulous visual acuity measurement, followed by careful examination of the eye for any predisposing factors. One should also perform B-scan ultrasonography to rule out any posterior segment pathology that may further qualify the management, such as retina pathology or a dislocated lens. In addition, the clinician should obtain aqueous and vitreous taps cultured with blood, chocolate, Sabouraud and thioglycolate agars, as well as Gram and Giemsa stains.4,5 For cases of postoperative endophthalmitis, the patient should be empirically treated with intravitreal injections of vancomycin and ceftazadime. The use of intravitreal corticosteroids remains controversial, and the clinician must determine its appropriateness in postoperative endophthalmitis.4 Amikacin can be substituted for ceftazadime in beta-lactam-sensitive patients.4,6,7,10 Patients are often started on topical antibiotics, such as gatifloxacin (Zymar, Allergan) or moxifloxacin at least four to six times a day. Intensive, fortified topical antibiotics, such as vancomycin and tobramycin, dosed qh are especially necessary in the setting of filtering blebs, wound leaks or exposed sutures.4,5 Additionally, aggressive treatment with the aforementioned antibiotics should be used to treat those patients who exhibit an associated keratitis.
Immediate pars plana vitrectomy for all types of endophthalmitis may be beneficial, because the procedure removes the infecting organisms, clears vitreous debris and improves distribution of intravitreal antibiotics.6 According to the results of the EVS, a pars plana vitrectomy benefitted those patients whose initial visual acuity was light perception only.6 The EVS indicated that a vitrectomy allowed a threefold chance of achieving 20/40 or better visual acuity, a twofold chance of achieving 20/100 or better acuity and a 50% decrease in the chance of permanent visual damage.6 In patients with initial hand motion visual acuity, there was no difference in visual outcome, whether or not a vitrectomy was performed.6 It is important to note, however, that this study only investigated endophthalmitis following cataract surgery with secondary intraocular lens placement, and excluded patients with prior penetrating ocular trauma, a strong suspicion of fungal endophthalmitis, or significant clouding of the anterior chamber or vitreous cavity sufficient enough to obscure a second-order retinal arteriole.6
In the case of traumatic endophthalmitis, orbital computed tomography is necessary to rule out an intraocular foreign body. One report indicated that people who experienced a penetrating injury were more than three times less likely to develop infectious endophthalmitis if they sought medical help within 24 hours of the injury compared to patients who sought help more than 24 hours after the injury.18 Further, those individuals age 50 and older were at a higher risk for developing endophthalmitis after a penetrating injury, possibly due to a higher susceptibility for infection and a propensity to postpone prompt medical attention.18
Patients with endogenous endophthalmitis usually have an underlying disease, such as diabetes, cancer, organ transplantation, intravenous-line associated sepsis, intravenous drug use and HIV.19 Treatment is aimed at ameliorating or eliminating the underlying problem, because the source likely originated elsewhere in the body. The provision of systemic antibiotics or antifungals is central in the treatment of this disease. In one literature review, eyes with endogenous fungal endophthalmitis were shown to have a better outcome than endogenous bacterial endophthalmitis.4 Overall, endogenous endophthalmitis has a poor visual outcome, with most patients exhibiting vision worse than 20/400.
In one report of endophthalmitis following suture removal 10 months after penetrating keratoplasty, the patient was chronically immunosuppressed following a renal transplantation, which likely decreased his ability to fight off small amounts of pathogens. In addition, the patient had chronic dacryocystitis, which appeared to be the source of the intraocular infection.
The report also suggested that evaluating the nasolacrimal sac is important in any patient with chronic ocular infections, especially postoperatively.21
When corneal wound dehiscence occurs, swift treatment to seal the perforation is of paramount importance. Ocular adhesives have been used since the early 1950s. Currently, three classes of adhesives exist: cyanoacrylate-based, fibrin/blood-based and miscellaneous newer agents.23 Cyanoacrylate-based adhesives (e.g., Dermabond [Johnson & Johnson] and Iso-Dent) are the most widely used and provide excellent gram-positive coverage.23-27 In addition, they prevent stromal melting by inhibiting leukocytes and can be left on for months.23,25-27 Fibrin/blood-based adhesives (e.g., Beriplast [CSL Surgery] and Hemaseel [Haemacure Corporation]) use the patient’s own blood or donor blood to simulate the properties of a clot.23 The application of such adhesives is beneficial for sutureless pterygium surgery because it is easily placed under the conjunctiva or amniotic membrane grafts.23
One report found cyanoacrylate-based adhesives better for sealing corneal incisions by demonstrating a threefold higher resistance to IOP than fibrin glue.24 Miscellaneous newer agents (e.g., CoSeal [Baxter Healthcare]) contain polyethylene glycol and serve as protective coatings in addition to sealing wounds.23 Due to their short life, however, these glues are best used only when a bandage contact lens cannot be placed over the eye.23 Close observation is mandatory, because one report illuminated three cases of infectious keratitis that were concealed by the opaqueness of the cyanoacrylate.26
As illustrated by the patient outlined in this case report, the cornea must be protected during this infectious and inflammatory period. To prevent significant dehiscence and corneal melting, patients are often started on doxycycline and vitamin C.28 Doxycycline is a broad-spectrum antibiotic that has been proven effective in the treatment of several ocular diseases, including significant blepharitis, acne rosacea, keratitis sicca and even recurrent corneal erosions.29 One report suggested that a minimum concentration of 100 micromolars of doxycycline inhibited corneal degrading enzyme matrix metalloproteinase (MMP) by chelating the metal ions that are structurally essential.29 Another study proved that doxycycline had a strong inhibitory effect on proinflammatory cytokine interleukin-1 (IL-1) by suppressing its bioactivity.30 In essence, the mechanism is twofold. First, doxycycline inhibits a pathologically activated corneal enzyme MMP, and second it promotes ocular surface repair by suppressing inflammation and stabilizing the corneal epithelium.29,30 This study further validated doxycycline to be equally as effective as potent corticosteroids in controlling IL-1beta in the treatment of keratitis sicca.30
While doxycycline inhibits the breakdown of corneal epithelium and suppresses inflammation, ascorbic acid (vitamin C) promotes collagen tissue healing in the cornea. Ascorbic acid acts as an important cofactor in collagen synthesis by stabilizing the collagen triple-helix structure.31 Ascorbic acid is naturally elevated in the aqueous humor compared to serum concentration, thereby reducing damage from ultraviolet light and increased free radicals.31 Numerous studies have shown that ascorbic acid can help heal corneal ulcers, reduce corneal fibroblast proliferation after corneal injury and reduce inflammation following glaucoma filtering surgery.31
Because some patients have experienced wound dehiscence up to 31 years after penetrating keratoplasty, it is likely that the corneal wound never regains the tensile strength of an intact cornea and remains a point of structural weakness of the eye. So, you should inform your patients that they are at long-term risk of wound dehiscence following penetrating keratoplasty and should educate them on relevant safety measures.
Corneal sutures pose a risk for the development of microbial keratitis and possibly endophthalmitis. While a majority of endophthalmitis cases result postoperatively, post-traumatically or endogenously, we described a case of microbial keratitis with endophthalmitis following routine corneal suture removal. It is possible that the patient’s long-term use of topical steroids, as well as his current cancer therapy, may have played a role in the pathophysiology of this case.
Whether patients are followed immediately after cataract surgery or present many years after a penetrating keratoplasty with an exposed suture, optometrists should be aware of the risks involved. Proper monitoring and safe removal techniques with prophylactic antibiotics are recommended to ensure bacteria do not cause a harmful surface and/or intraocular infection. Furthermore, clinicians should be educated about treatment options for corneal dehiscence with effective medications and approved ocular adhesives.
Dr. Cohen completed his residency at the Gainesville, Fla. VA clinic in June 2010. He now practices independently in South Florida. He has no direct financial interest in any of the products mentioned. Dr. Marcus-Freeman is a staff optometrist and optometry residency coordinator at Malcolm Randall VA Medical Center in Gainesville. Dr. Page is a staff optometrist and residency attending at the same facility.
1. Confino J, Brown SI. Bacterial endophthalmitis associated with exposed monofilament sutures following corneal transplantation. Am J Ophthalmol. 1985 Feb 15;99(2):111-3.
2. Christo CG, van Rooij J, Geerards AJ, et al. Suture-related complications following keratoplasty: a 5-year retrospective study. Cornea. 2001 Nov;20(8):816-9.
3. Spigelman AV. Visual loss following suture removal postkeratoplasty. Cornea. 1988;7(3):214-7.
4. Lemley CA, Han DP. Endophthalmitis: a review of current evaluation and management. Retina. 2007 Jul-Aug;27(6):662-80.
5. Doft BH, Wisniewski SR, Kelsey SF, et al. Diabetes and postoperative endophthalmitis in the endophthalmitis vitrectomy study. Arch Ophthalmol. 2001 May;119(5):650-6.
6. Endophthalmitis Vitrectomy Study Group. Results of the Endophthalmitis Vitrectomy Study. A randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Arch Ophthalmol. 1995 Dec;113(12):1479-96.
7. Fan JC, Niederer RL, von Lany H, Polkinghorne PJ. Infectious endophthalmitis: clinical features, management and visual outcomes. Clin Experiment Ophthalmol. 2008 Oct;36(7):631-6.
8. Jackson TL. Endogenous bacterial endophthalmitis: a 17-year prospective series and review of 267 reported cases. Surv Ophthalmol. 2003 Jul-Aug;48(4):403-23.
9. Diago T, McCannel CA, Bakri SJ, et al. Infectious endophthalmitis after intravitreal injection of antiangiogenic agents. Retina. 2009 May;29(5):601-5.
10. Mao LK, Flynn HW Jr, Miller D, Pflugfelder SC. Endophthalmitis caused by Staphylococcus aureus. Am J Ophthalmol. 1993 Nov 15;116(5):584-9.
11. Callegan MC, Engelbert M, Parke DW 2nd, et al. Bacterial endophthalmitis: epidemiology, therapeutics, and bacterium-host interactions. Clin Microbiol Rev. 2002 Jan;15(1):111-24.
12. Khurshid GS, Fahy GT. Endophthalmitis secondary to corneal sutures: series of delayed-onset keratitis requiring intravitreal antibiotics. J Cataract Refract Surg. 2003 Jul;29(7):1370-2.
13. Maumenee AE. The Pocklington lecture, 1976. Recent advances in corneal transplantation. Trans Ophthalmol Soc U K. 1976;96(4):462-70.
14. Forstot SL, Abel R Jr, Binder PS. Bacterial endophthalmitis following suture removal after penetrating keratoplasty. Am J Ophthalmol. 1975 Sep;80(3 Pt 2):509-12.
15. Zink JM, Singh-Parikshak R, Sugar A, Johnson MW. Clostridium sordellii endophthalmitis after suture removal from a corneal transplant. Cornea. 2004 Jul;23(5):522-3.
16. Scott IU, Flynn HW Jr, Feuer W, et al. Endophthalmitis associated with microbial keratitis. Ophthalmology. 1996 Nov;103(11):1864-70.
17. Benz MS, Scott IU, Flynn HW Jr, et al. Endophthalmitis isolates and antibiotic sensitivities: a 6-year review of culture-proven cases. Am J Ophthalmol. 2004 Jan;137(1):38-42.
18. Thompson JT. Infectious endophthalmitis after penetrating injuries with retained intraocular foreign bodies. National Eye Trauma System. Ophthalmology. 1993 Oct;100(10):1468-74.
19. Schiedler V, Scott IU, Flynn HW Jr, et al. Culture-proven endogenous endophthalmitis: clinical features and visual acuity outcomes. Am J Ophthalmol. 2004 Apr;137(4):725-31.
20. Abou-Jaoude ES. Spontaneous wound dehiscence after removal of single continuous penetrating keratoplasty suture. Ophthalmology. 2002 Jul;109(7):1291-6.
21. Weiss JL, Nelson JD, Lindstrom RL, Doughman DJ. Bacterial endophthalmitis following penetrating keratoplasty suture removal. Cornea. 1984-1985;3(4):278-80.
22. Culbert RB, Devenyi RG. Bacterial endophthalmitis after suture removal. J Cataract Refract Surg. 1999 May;25(5):725-7.
23. Bhatia SS. Ocular surface sealants and adhesives. Ocul Surf. 2006 Jul;4(3):146-54.
24. Chen WL, Lin CT, Hsieh CY, et al. Comparison of the bacteriostatic effects, corneal cytotoxicity, and the ability to seal corneal incisions among three different tissue adhesives. Cornea. 2007 Dec;26(10):1228-34.
25. Vote BJ, Elder MJ. Cyanoacrylate glue for corneal perforations: a description of a surgical technique and a review of the literature. Clin Experiment Ophthalmol. 2000 Dec;28(6):437-42.
26. Cavanaugh TB, Gottsch JD. Infectious keratitis and cyanoacrylate adhesive. Am J Ophthalmol. 1991 Apr 15;111(4):466-72.
27. Eiferman RA, Snyder JW. Antibacterial effect of cyanoacrylate glue. Arch Ophthalmol. 1983 Jun;101(6):958-60.
28. Dursun D, Kim MC, Solomon A, Pflugfelder SC. Treatment of recalcitrant recurrent corneal erosions with inhibitors of matrix metalloproteinase-9, doxycycline and corticosteroids. Am J Ophthalmol. 2001 Jul;132(1):8-13.
29. Smith VA, Cook SD. Doxycycline-a role in ocular surface repair. Br J Ophthalmol. 2004 May;88(5):619-25.
30. Solomon A, Rosenblatt M, Li DQ, et al. Doxycycline inhibition of interleukin-1 in the corneal epithelium. Invest Ophthalmol Vis Sci. 2000 Aug;41(9):2544-57.
31. Gross RL. The effect of ascorbate on wound healing. Int Ophthalmol Clin. 2000 Fall;40(4):51-7.

