 |
On a recent Saturday night, the answering service called and relayed a message from a patient complaining of flashes and floaters. The patient, a 50-year-old high myope who had an onset of flashes and floaters 10 days earlier, was seen by an optometrist that day and was diagnosed with an uncomplicated posterior vitreous detachment (PVD). At that visit, she was educated on the warning signs of retinal detachment and instructed to call the office immediately should there be any
worsening or change in her symptoms. When she noticed an increase in floaters and felt that the lower segment of her vision had become affected, she called. Based on her symptoms, we asked her to meet us in the office that night. Surprisingly, she asked if this could wait until tomorrow. Because she lives by herself, in a rural town approximately 45 minutes away, and it was snowing, she was not comfortable driving herself. When I explained that she may have a retinal detachment at risk of involving her central vision, she said she would try and find a ride and would get back to me.
This column will review the risks of waiting eight to 12 hours to make this diagnosis and determine whether it is reasonable for the patient to simply prepare for possible surgery in the morning.
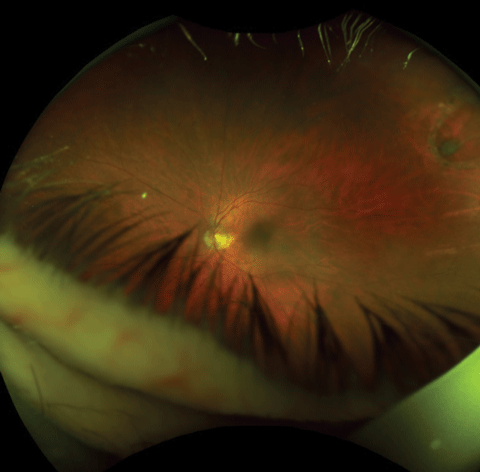 |
| Fig. 1. An 82-year-old asymptomatic male with an old self-sealing horseshoe retinal tear. Click image to enlarge. |
Full-Thickness Tear Risk
PVD is largely regarded as a degenerative process of the vitreous resulting in the separation of the vitreous gel from the internal limiting membrane of the retina. In most cases, the posterior hyaloid separation occurs without complication, resulting in a complete or incomplete Weiss ring “floater” that casts a vacillating shadow of varying darkness, depending on its proximity to the retina. However, in a minority of cases, tractional forces can lead to a full-thickness tear that, if not addressed in a timely fashion, can lead to rhegmatogenous retinal detachment (RRD).
PVD is largely an age-related event.1 Patients in their 50s have an expected prevalence of only 25%, while almost 90% of patients in their 80s will have already had a PVD.1 With that said, investigators report PVD occurs a full decade earlier in highly myopic patients (>6.00D). In fact, the higher the myopia, the earlier the onset.1
Tear or Detachment Risk
An evidence-based review and meta-analysis sought to find the percentage of patients with symptoms of flashes or floaters, or both, who are likely to present with a retinal tear or detachment.2 It found that, in all PVD cases, when patients reported the acute onset of flashes or floaters, or both, the prevalence of a retinal break or tear was 14%.2 Interestingly, the incidence was almost identical in cases of just flashes without floaters (13.7%) to those reporting just floaters without flashes (13.5%).2 The study also found that, in patients with additional subjective complaints of vision reduction, the risk of complicated PVD increased to 45%.2
Not all retinal tears lead to detachment. Studies show approximately one-third to nearly half of retinal tears actually result in retinal detachment (Figure 1).3,4
The mechanism of RRD or extension is largely dependent on such factors as size and location of the retinal break, residual vitreous traction and the degree of vitreal syneresis (liquefied vitreous).5,6 Superior breaks in the retina present a greater risk for detachment, especially if there is persistent vitreoretinal traction. The vitreous has a higher specific gravity than aqueous. When the adhesion between the vitreous and retina is strong, a small break can turn into a large retinal tear in short order. The longer the break goes undiagnosed, the greater the risk of RRD secondary to fluid migration into the subretinal space. Conversely, gravitational forces of the vitreous can provide some tamponade effect on inferior retinal breaks.7,8
Clinical Findings of Concern
In the same meta-analysis, investigators reviewed 12 studies looking at predictive factors for retinal tear based on direct clinical examination. They found two significant findings that should raise concern of a possible retinal tear:2
1. Vitreous hemorrhage (62% chance of retinal tear or detachment).
2. Pigment dusting of the vitreous (88% probability of the same).
Retinal detachment occurs with an estimated incidence of 12 per 100,000 persons per year and with a prevalence of 0.3%.9,10 Risk factors for retinal detachment include, among others, age, aphakia, myopia, pseudophakia, recent eye surgery and trauma. While retinal detachments involving the macula are considered less urgent, “macula-on” detachments are usually considered an ocular urgency.10
What the Studies Say
The timing of surgical repair for macula or foveal-sparing RRDs has been a source of debate recently among retinal specialists. While most surgeons attempt to evaluate and repair macula-on detachments in a timely fashion, sometimes there are medical (i.e., comprehensive medical clearance for comorbid conditions) or logistical barriers (i.e., operating room, anesthesia, and caregiver availability) preclude timely surgery. A number of studies have reviewed the importance of timing for surgery in this subset of patients, and their conclusions might surprise you.
One retrospective analysis studied 199 patients who underwent scleral buckling surgery for macula-on detachments. While the majority of patients had the surgery within the first 24 hours (52%), 27% were addressed within one to three days, 10% between three to seven days and the rest longer than one week. The authors did not find a relationship between the timing of surgery and postoperative acuity at any time interval.11
| Fig. 2. This widefield image displays a patient’s superiorly located retinal break with a secondary macula-on RRD, which we discovered using indirect ophthalmoscopy. |
Because this and other studies suggest that the rate of RRD progression is likely slower than intuitively expected, in some cases, it may be beneficial to delay surgery 24 to 48 hours.
Recognize an Emergency
While the data suggests we can be flexible concerning the timing of surgical repair for macula-on detachments, those involving giant retinal tears that are superiorly located and encroaching on the macula should be treated as an ocular emergency. When barriers exist to timely surgery, however, limited activity and bed rest should be considered. Some advocate occluding both eyes to limit saccadic eye movements, which can increase fluid dynamics and migration into the subretinal space.
Our patient called back within 20 minutes indicating she had founda ride. I instructed her to pack a bag of clothes and not to eat anything before her visit. Upon examining her, it was determined that she had preserved central vision (BCVA 20/20- each eye), but had reduced confrontation fields inferiorly in her left eye and slight asymmetry in her intraocular pressures (16mm Hg OD, 12mm Hg OS). Prior to and after dilation, slit-lamp exam of the vitreous increases revealed mild pigmentary “dusting” of the anterior vitreous. Indirect ophthalmoscopy revealed a large, superiorly located retinal break with a secondary “macula-on” rhegmatogenous retinal detachment (Figure 2). In six hours she was undergoing surgical intervention.
|
1. Hikichi T, Hirokawa H, Kado M, et al. Comparison of the prevalence of posterior vitreous detachment in whites and Japanese. Ophthalmic Surg. 1995;26(1):39-43. 2. Hollands H, Johnson D, Brox A, et al. Acute-onset floaters and flashes: is this patient at risk for retinal detachment? JAMA. 2009 Nov 25;302(20):2243-9. 3. Davis M. Natural history of retinal breaks without detachment. Arch Ophthalmol. 1974;92(3):183-94. 4. Shea M, Davis MD, Kamel I. Retinal breaks without detachment, treated and untreated. Mod Probl Ophthalmol. 1974;12(0):97-102. 5. Lincoff H, Gieser R. Finding the retinal hole. Arch Ophthalmol. 1971;85(5):565–9. 6. Machemer R. The importance of fluid absorption, traction, intraocular currents, and chorioretinal scars in the therapy of rhegmatogenous retinal detachments. XLI Edward Jackson Memorial Lecture. Am J Ophthalmol 1984;98(6):681–93. 7. Pederson J, MacLellan H. Experimental retinal detachment. I. Effect of subretinal fluid composition on reabsorption rate and intraocular pressure. Arch Ophthalmol. 1982;100(7):1150–4. 8. Wilkinson C, Rice T. Michels retinal detachment. 2nd ed. St. Louis: Mosby;1997:471–81. 9. Sodhi A, Leung LS, Do DV, et al. Recent trends in the management of rhegmatogenous retinal detachment. Surv Ophthalmol. 2008;53:50-67. 10. Haimann MH, Burton TC, Brown CK. Epidemiology of retinal detachment. Arch Ophthalmol. 1982;100(2):289-92. 11. Wykoff C, Smiddy W, Mathen T, et al. Fovea-sparing retinal detachments: time to surgery and visual outcomes. Am J Ophthalmol. 2010;150:205-10. |

