 Q: What should be in my differential diagnosis of recently induced astigmatism?
Q: What should be in my differential diagnosis of recently induced astigmatism?
A: Consider this case for comparison: A 49-year-old white female came in for a routine eye examination at the office of Joseph Rappon, O.D., in
Four years later, she presented to the office again, but now she had an unexplained reduction in visual acuity in one eye of 20/20-1. Dr. Rappon took keratometry readings and noted distorted mires in her left eye.
A few times a year, an optometrist will see a patient who has reduced visual acuity but no apparent corresponding pathology or symptoms that would cause this reduction, Dr. Rappon says. This is very disturbing to practitioners because one of the most basic doctrines in eye care is to always explain a reduction in visual acuity.
Reduced visual acuity of this sort can be caused by one of several conditions, such as corneal distortion, tumor, optic nerve disease or occult retinal pathology, he says. Such patients are often sent for unnecessary MRIs or retinal consultations, when it turns out they simply have corneal distortion. Yet, this can be easily confirmed with corneal topography or a gas permeable contact lens-aided refraction.
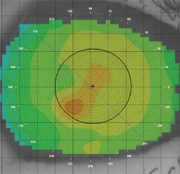
This patient presented with unexplained acuity loss in her left eye. Topgraphy revealed corneal astigmatism.
In this patients case, topography detected almost 3.00D of irregular corneal astigmatism O.S. Topography of the right eye was normal.
While not every O.D. has a topographer, every O.D. can use a rigid contact lens for this purpose, Dr. Rappon says. You eliminate the distortion by putting a rigid contact lens on a distorted cornea, which allows you to re-refract the patient to normal acuity. Of course, if the patient had a brain tumor, optic nerve disease or occult retinal pathology, the patients visual acuity would still be reduced with the rigid contact lens on eye.
So, what caused the corneal distortion in this patients case? Anything that puts pressure on the cornea can cause it to distort, Dr. Rappon says. This can be a chalazion, an orthokeratology lens, a subtle corneal dystrophy (such as map-dot-fingerprint), keratoconus or another corneal degeneration, eyelid surgery, or even prolonged reading in downgaze.1,2
In this case, Dr. Rappon learned that after the patients initial eye exam in 2003, she was prescribed sulindac, a sulfa-based non-steroidal anti-inflammatory drug, for psoriatic arthritis. After two weeks of treatment, she developed some flu-like symptoms, which turned out to be the initial presentation of toxic epidermal necrolysis, a more severe version of Stevens-Johnson syndrome, Dr. Rappon says. Sulindac has been linked to similar cases, and at least one fatality.3,4
After being admitted to the hospital, she was put into a medically induced coma for five weeks, he says. Taping a coma patients eyes shut is standard procedure to avoid exposure keratopathy. But, of course, it didnt come to mind when I initially considered this patients case. After questioning her extensively, we eventually pieced together that this had caused her corneal distortion.
The patient is once again able to wear contact lenses and she continues to wear spectacles with astigmatic correction O.S.
So, before sending a patient with unexplained reduced acuity on a wild goose chase, try topography or a GP contact lens first.
1. Zinkernagel MS, Ebneter A, Ammann-Rauch D. Effect of upper eyelid surgery on corneal topography. Arch Ophthalmol 2007 Dec;125(12):1610-2.
2. Golnik KC, Eggenberger E. Symptomatic corneal topographic change induced by reading in downgaze. J Neuroophthalmol 2001 Sep;21(3):199-204.
3. Small RE, Garnett WR. Sulindac-induced toxic epidermal necrolysis. Clin Pharm 1988 Oct;7(10):766-71.
4. Ikeda N, Umetsu K, Suzuki T. A fatal case of sulindac-induced Lyell syndrome (toxic epidermal necrolysis). Z Rechtsmed 1987;98(2):141-6.

