Vitrectomy with membrane peel is the most common vitreoretinal surgery billed to the Centers of Medicare and Medicaid Services. The procedure is typically performed to intervene in the event of epiretinal membrane (ERM) formation or vitreomacular traction syndrome that presents with visually significant symptoms.


An ERM is a semitranslucent, avascular, fibrocellular membrane located along the inner surface of the retina’s internal limiting membrane (ILM). In most instances, ERM formation is seen over or around the macula. Clinically, you may document a loss of foveal reflex, parafoveal light reflection (which looks similar to cellophane), wrinkling of the retinal surface, localized intraretinal hemorrhages or alteration of the parafoveal vasculature (increased tortuosity). Macular edema and/or pseudoholes may also be associated with ERM development.
Some ERM patients are asymptomatic; however, most affected individuals report distorted vision or scotomas that are repeatable on Amsler grid testing. Because some ERMs slowly worsen over time, patients typically experience a gradual reduction in visual acuity.
The first clinical sign of ERM formation tends to be an unnatural macular appearance. Although fluorescein angiography can be used to help diagnose ERM, OCT has become the gold standard; its high-resolution imaging of the vitreoretinal interface detects even the subtlest membrane.
Not all membranes require treatment. The risk of surgical intervention for mild ERMs that have little to no visual impact isn’t justified. Typically, the patient’s symptomatic course will dictate the timing of surgical intervention. In many cases, mild membranes are simply monitored over time for progression. But once the patient’s perception of visual distortion begins to impact his or her quality of life, you should recommend surgical consultation.
Multimedia
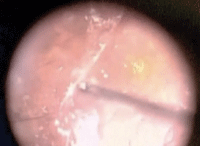
Click
here to view a narrated video of an epiretinal membrane peeling procedure.
Photo and video courtesy of Alan Franklin, MD, PhD
Historically, the only viable treatment for ERM was vitrectomy surgery. Although relatively successful, recurrence rates were as high as 16%.
Recently, surgeons have begun to also peel the ILM from the retina after vitrectomy, to decrease the risk of recurrence. This additional measure, in essence, reduces the recurrence rate to 0%.
To preserve the anatomic integrity of the retina, ILM removal must be executed with extreme caution. Surgeons may use various imaging devices and intraoperative dyes to help visualize the ILM, and then subsequently peel it off the retina.
In vitrectomy with membrane peel procedures, the instruments are usually inserted 4mm behind the limbus. The surgery is performed under local anesthesia with very small incision ports that do not require suturing. Visual recovery varies from patient to patient, but can be dramatic the very next day.
The most common surgical complications include infection (roughly one in 1,000 procedures), retinal detachment (roughly one in 100 procedures), cataract progression in phakic eyes, bleeding and diplopia. Although such complications are relatively rare, open discussion of the possible risks often helps to gauge the patient’s desire for surgical intervention.

