
Fifty million Americans are affected by allergy each year, and 30 million of these individuals suffer from seasonal allergies.1 Meanwhile, ocular surface disease (OSD) affects approximately 20.7 million people in the U.S. every year.2 Of these, nearly 4.25 million individuals have chronic ocular surface disease.3 While many clinicians still ascribe to the general notion that "allergy affects the young and dry eye affects the old," international epidemiology data suggests that allergic disease is on the rise across all age groups.4 The prevalence of allergic rhinitis (AR) has increased during the last three decades and is now estimated to affect 20% of the adult population in the U.S.4 AR is actually considered the most common chronic condition in both adults and children.6 And, 75% of those diagnosed with AR actually have allergic rhinoconjunctivitis.5
It can be challenging to differentiate ocular surface disease from allergic
conjunctivitis, as seen in this patient.
It can be a challenge to distinguish allergic symptoms from dry eye symptoms. Treating a patient who presents with concurrent allergy and dry eye symptoms, however, can be an even greater challenge. Whether you are considering a true type I IgE-mediated allergic reaction or a type IV delayed cell-mediated reaction, the likelihood of allergy colliding with ocular surface disease in patients of advanced age is significant.
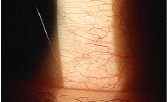
Courtesy: Jason R. Miller, O.D.
In the following case, the patient presents with concurrent allergy and OSD. What risk factors does she face? How should she best be treated? And, what general management tips and strategies can you recommend to her?
A Case of Concurrent Allergy and Ocular Surface Disease
History. A 49-year-old postoperative LASIK patient presented to our
At first, the patient was miserable because she did not want to rub her eyes and disturb her corneal flap. She reported some relief after taking Claritin (loratadine, Schering Corporation) and using Refresh Liquigel (Allergan) q.i.d. O.U., but noted that her eyes still bothered her noticeably.
Her medical history was unremarkable. Her ocular history was positive for preoperative spectacle correction and wavefront-guided LASIK for compound myopic astigmatism (spherical equivalent of -7.25D O.U.). Interestingly, she reported no history of allergies on her pre-LASIK questionnaire.
Diagnostic data. Her best-uncorrected visual acuity measured 20/20 O.U. A slit lamp examination confirmed conjunctival papillae and palpebral conjunctival injection, with mild bulbar conjunctival chemosis O.U. Also, there was mild thickening and hyperemia of the lid margins. There was adequate lid and punctal apposition O.U., and her silicone punctal plugs were in place. Despite intermittent reflex tearing, her tear prism was poor, and there was mild lissamine green staining involving both the nasal and temporal conjunctiva O.U.
Upon further questioning, the patient indicated that she had suffered from seasonal allergies in the past, but that they had not bothered her since she moved to
Discussion. Our patient demonstrates several risk factors for seasonal allergic conjunctivitis (SAC):
1. Springtime in the southeastern
2. History of SAC. Our patient has a personal history of SAC, and her recent move from
3. Morning symptoms. Our patient's allergic symptoms are worse during the morning hours when pollen counts are highest (usually between 5:00 a.m. and 10:00 a.m.).
Additionally, our patient demonstrates several risk factors for ocular surface disease:
1. Post-menopausal female. According to the Women's Health Study, 3.2 million women age 50 or older suffer from clinically significant dry eye.9 In this demographic, ocular surface disease tends to affect females at a rate of 3:1 vs. males.9 Additionally, the risk of dry eye increases both during and after menopause. Advancing age and varying hormonal changes are also associated with ocular surface disease.10
2. History of refractive surgery. The creation of a corneal flap disrupts normal corneal innervation and results in hypoesthesia that may persist for six months or longer.11 Hypoesthesia, or decreased corneal sensitivity, contributes to the disruption of the normal neuronal-feedback loop, causing decreased tear production, tear film instability, decreased tear clearance, increased tear osmolarity and epitheliopathy.12
Superior hinge flaps decrease innervation to an even greater degree; the main branches of the long posterior corneal nerves enter the eye at both a 3 o'clock and 9 o'clock position. When a nasal hinge flap is created, the nasal arm is preserved.13 Femtosecond flap technology (e.g., IntraLase, Abbott Medical Optics) provides more flexibility with respect to flap size, hinge location and flap thickness--all of which can be adjusted to improve post-LASIK dry eye symptoms and recovery time.14 Some clinicians have also proposed that the greater the refractive error (thus, the greater ablation depth in laser vision correction), the greater the decrease in corneal sensitivity and the longer the recovery time.8,15
3. Oral antihistamine use. According to a 2008 survey conducted by Pharmacy Times,
Also, oral histamine H1-receptor antagonists are the most frequently prescribed class of agents used for allergic rhinitis management.17 Unlike first-generation antihistamines, second-generation agents are highly selective peripheral histamine blockers that demonstrate little or no side effects upon the central or autonomic nervous systems.18 While second-generation agents are actually "minimally-sedating," they still exhibit a tendency to reduce tear volume and may exacerbate symptoms of ocular irritation, itching and dryness.19
After considering these factors extensively, I suggested that our patient modify a few of her lifestyle activities, including jogging in the evening instead of the morning. Also, I started her on a regimen of Elestat (epinastine HCL 0.05%, Allergan) b.i.d. O.U. and Refresh Plus (Allergan) q2h; I instructed her to refrigerate both products. Finally, if our patient's ocular symptoms improve but her nasal congestion persists, I will remove her silicone punctal plugs.
Drug
1. Claritin (loratadine, Schering Corporation)
2. Zyrtec (cetirizine, Pfizer)
3. Benadryl (diphenhydramine,
Warner Lambert)
4. Chlor-Trimeton (chlorpheniramine
maleate, Schering Plough)
5. Alavert (loratadine, Wyeth)
Top Five Most-Frequently Prescribed Oral OTC Antihistamines16
Prescription Frequency
Classification
48.5%
(Second-generation, non-sedating)
15.0%
(Second-generation, non-sedating)
7.5%
(First-generation, sedating)
6.8%
First-generation, sedating)
4.1%
(Second-generation,
non-sedating)
Five Tips for Allergy Sufferers
1. Avoid the avoidable. Allergy testing is a critical first step in determining precisely what is causing your patient's allergic reaction. Narrowing the list of potentially offending allergens through skin-prick or blood testing allows for more targeted avoidance techniques and treatments, including immunization therapy.
Also, patients with seasonal allergies should pay attention to local weather and pollen counts on a daily basis to avoid acute allergic reactions. Instruct your patients to remain indoors in the air conditioning as much as possible when pollen counts are high. When spring arrives, most people have a natural tendency to want to open all of the windows and let fresh air in. Despite this natural impulse, seasonal allergy sufferers need to remember that this could incite or worsen allergy symptoms.
Remind patients to avoid prolonged rubbing of itchy eyes. Intense itching is the classic sign of an IgE-dependent hypersensitivity response. In susceptible individuals, initial exposure of an allergen to the ocular surface stimulates the production of specific immunologic antibodies, which bind to and degranulate mast cells that contain several preformed mediators, including histamine. Histamine, once released, binds to H1 and H2 receptors located on the conjunctiva, resulting in vaso-endothelial dilation and secondary chemosis, redness, tearing, lid swelling and intense itching. Unfortunately, this intense itching and reflex tearing can lead to a vicious cycle of eye rubbing, which subsequently degranulates more mast cells and furthers the response.
Instruct your patients with allergic conjunctivitis to remain indoors when local pollen counts are elevated.
Courtesy: Jason R. Miller, O.D.
Instead of rubbing, instruct your patients to apply cool compresses and instill refrigerated eye drops. While icepacks work well, gel-filled facemasks work better and are readily available at most drug stores. The chilled drops soothe the eye, decrease vascular permeability of the conjunctiva vessels and reduce chemosis.
Finally, tell your patients to shower at night before they go to bed. Pollen and spores may get deposited on the skin or in hair after prolonged outdoor activity. Washing away these allergens before bedtime ensures they do not get transferred to sheets and pillowcases, which could make symptoms more chronic.
2. Lower viscosity preservative-free artificial tears. Just like our postoperative LASIK patient, it is not uncommon for someone with moderate ocular surface disease to be on a more viscous artificial tear, such as Refresh Liquigel, Refresh Celluvisc (Allergan) or Bion Tears (Alcon). When allergy strikes, however, a less viscous tear, such as Preservative Free Optive (Allergan) or Systane Ultra (Alcon), used more frequently would be better at washing out environmental allergens and inflammatory mediators from the ocular surface.
3. Limit punctal plug use. When confronted with a type I IgE mediated allergic reaction, the goal is usually to flush inflammatory mediators from the ocular surface. Punctal plugs are counter-productive for this goal. Also, intense itching promotes eye rubbing, which could put the patient at risk for several punctal plug associated complications, such as extrusion or canalicular migration with secondary nasolacrimal obstruction, canaliculitis or dacryocystitis.
If your patient has moderate ocular surface disease, and closure of the lacrimal punctum is warranted despite a history of seasonal allergic conjunctivitis, you might decide upon occlusion with extended-duration plugs. Extended-duration punctal plugs, which typically demonstrate a partial occlusive effect at four months post-insertion, are ideal for dry eye patients during the allergy "off-season."
For patients who present with seasonal allergic rhinoconjunctivitis and have already undergone punctal cautery, dual therapy of topical antihistamine/mast-cell stabilizers and nasal corticosteroids should adequately reduce symptoms and histamine-related flare-ups.
4. Avoid oral antihistamines. As noted above, all oral antihistamines
including newer-generation antihistamines, such as Claritin, Zyrtec (cetirizine, Pfizer) and Allegra (fexofenadine, Aventis Pharmaceuticals)
dry the eye. This can worsen ocular allergies in two ways. First, less tear production means less tear flow and inadequate flushing of environmental allergens from the ocular surface. Second, decreased tear volume results in an increased concentration of inflammatory mediators on the ocular surface.
Instead, consider treating topical allergy topically. The third-generation topical antihistamines/mast-cell stabilizers, such as Pataday (olapatadine hydrochloride 0.2%, Alcon), Patanol (olapatadine hydrochloride 0.1%, Alcon) and Elestat have shown to be fast-acting and quite effective in quelling the allergic cascade, while reducing allergic ocular symptoms without the secondary effects of surface drying.19,20 As an added benefit, olapatadine 0.2% has shown potential in reducing allergic rhinitis symptoms in patients with a patent nasolacrimal duct system.21 For patients without prescription drug coverage, Zaditor (ketotifen 0.025%, Novartis Pharmaceuticals) is now available over the counter.
For exaggerated, late-phase allergic responses (i.e., conjunctival inflammation, including chemosis and lid edema), the safer topical ester-based steroids, including Alrex (loteprednol etabonate ophthalmic suspension 0.2%, Bausch & Lomb) and Lotemax (loteprednol etabonate ophthalmic suspension 0.5%, Bausch & Lomb), are ideal. Pulse therapy in conjunction with a fast-acting medicine, such as Patanol or Elestat, can minimize congestion and abort ocular symptoms.
For persistent symptoms of AR, intranasal glucocorticosteroids--delivered topically as a spray to the nasal mucosa--are generally considered very safe and effective. Contraindicated in patients with a history of nasal polyps or surgery, steroid nasal sprays, such as flunisolide, were found to be more effective at improving symptoms of AR when compared with intranasal antihistamines, such as azelastine HCl.22 In addition to flunisolide, this group of medications includes fluticasone propionate, mometasone, budesonide, triamcinolone, beclomethasone and fluticasone furoate.
For patients with contraindications or aversions to nasal sprays, oral leukotriene inhibitors such as Singulair (montelukast sodium, Merck) may be the answer. The FDA has approved montelukast for the treatment of AR. Additionally, Singulair has the added benefit of being non-drying.23 And, several studies show that montelukast was more beneficial than placebo and was equally as effective as loratadine for the treatment of seasonal AR.24,25
5. Remember Restasis. Restasis (topical cyclosporine A 0.05%, Allergan), a T-cell immunomodulating agent, was approved by the FDA in 2002 for the primary indication of treating immune-mediated dry eye.
However, since that time, Restasis has shown tremendous off-label benefits in the management of other ocular disease entities, such as allergic keratoconjunctivitis, posterior blepharitis and keratomycosis.26
Additional data show that Restasis also inhibits activation of mast cells and eosinophils.26 One of its most beneficial off-label uses is against vernal and atopic keratoconjunctivitis.26,27 Because Restasis is a very effective anti-inflammatory agent with a superb safety profile (no deleterious effect on intraocular pressure, premature cataract formation or phagocytosis), it has allowed physicians to decrease or limit the long-term use of topical steroids in managing many sight-threatening conditions.
That said, can Restasis play a role in the management of SAC? As a primary or first-line agent, probably not. However, in a patient with
chronic OSD, Restasis may lesson the severity of future seasonal allergic attacks.
With adequate inquiry into a patients personal and family history of allergy, followed by education on lifestyle modification and treatment strategies for SAC, your dry eye patients will be better prepared for the onslaught of allergy season.
Dr. Mangan is chair of the refractive surgery and research committees for the Eye Center Group, a multi-specialty comanagement center in central
1.
2. Harmon D. Market Scope, LLC. 2008 Comprehensive Report on the Global Dry Eye Market. Available at:
http://dev.market-scope.com/market_reports/2008/07/2008-comprehensive-report-on-t.html (Accessed July 7, 2009).
3. Schaumberg DA, Gardiner M, Schein OD. Epidemiology of major cornea and external diseases. In: Foster CS, Azar DT, Dohlman CH (eds). The Cornea: Scientific Foundations and Clinical Practice, 4th ed.
4. Fineman S. The burden of allergic rhinitis: beyond dollars and sense. Ann Allergy Asthma Immunol. 2002 Apr;88(4 Suppl 1):2-7.
5. Nathan RA, Meltzer EO, Derebery J, et al.
The prevalence of nasal symptoms attributed to allergies in the
6. Berger WE. Overview of allergic rhinitis. Ann Allergy Asthma Immunol. 2003 Jun;90(6 Suppl 3):7-12.
7. The Asthma and Allergy Foundation of
8. Nassaralla BA,
9. Schaumberg DA, Sullivan DA, Buring JE, Dana MR. Prevalence of dry eye syndrome among US women. Am J Ophthalmol. 2003 Aug;136(2):318-26.
10. Mathers WD, Stovall D, Lane JA. Menopause and tear function: the influence of prolactin and sex hormones on human tear production. Cornea. 1998 Jul;17(4):353-8.
11. Albietz JM, Lenton LM, McLennan SG. Dry Eye after LASIK: Comparison of outcomes for Asian and Caucasian Eyes. Clin Exp Optom. 2005 Mar;88(2):89-96.
12. Benitez-del-Castillo JM,
13. Vroman DT, Sandoval HP, Fernndez de Castro LE, et al. Effect of hinge location on corneal sensation and dry eye after laser in situ keratomileusis for myopia. J Cataract Refract Surg. 2005 Oct;31(10):1881-7.
14. Barequet I, Hirsh A, Levinger S. Effect of thin femtosecond LASIK flaps on corneal sensitivity and tear function. J Refract Surg. 2008 Nov;24(9):897-902.
15. Kim WS, Kim JS. Change in corneal sensitivity following laser in situ keratomileusis. J Cataract Refract Surg. 1999 Mar;25(3):368-73.
16. Terrie YC, Bowling EL. Update on the OTC treatment of allergies: focus on allergic conjunctivitis. Pharmacy Times. ACPE program number: 290-999-09-005-H01-P. Available at:
https://secure.pharmacytimes.com/lessons/200903-02.asp (Accessed June 16, 2009).
17. Hansen J, Klimek L, Hormann K. Pharmacological management of allergic rhinitis in the elderly: safety issues with oral antihistamines. Drugs Aging. 2005;22(4):289-96.
18. May JR. Allergic Rhinitis. In DiPiro JT, Talbert RL, Yee Gc (eds) Pharmacotherapy: A Pathophysiologic Approach, 5th Ed. New York: McGraw-Hill, 2002:1679-87.
19. Ousler GW 3rd, Workman DA, Torkildsen GL. An open-label, investigator-masked, crossover study of the ocular drying effects of two antihistamines, topical epinastine and systemic loratadine, in adult volunteers with seasonal allergic conjunctivitis. Clin Ther. 2007 Apr;29(4):611-6.
20. Mah FS, OBrien T, Kim T. Evaluation of olopatadine
hydrochloride 0.2% in an allergic conjunctivitis patient population with dry eye. Summary of paper presented at Western Society of Allergy, Asthma and Immunology scientific session. Maui, Hawaii: January 15-19, 2007.
21. Abelson MB, Gomes PJ, Vogelson CT, et al. Clinical efficacy of olopatadine hydrochloride ophthalmic solution 0.2% compared with placebo in patients with allergic conjunctivitis or rhinoconjunctivitis: a randomized double-masked environmental study. Clin Ther. 2004 Aug;26(8):1237-48.
22. Berlin JM, Golden SJ, Teets S, et al. Efficacy of a steroid nasal spray compared with an antihistamine nasal spray in the treatment of perennial allergic rhinitis. J Am Osteopath Assoc. 2000 Jul;100(7 Suppl):S8-13.
23. Sheppard JD, Pflugfelder SC. Eye World. Allergy: Stepping up to treat unique and challenging cases of ocular allergy with co-morbid disease. Available at:
www.eyeworld.org/article.php?sid=3665&strict=&morphologic=&query=sheppard%20pflugfelder (Accessed July 7, 2009).
24. Meltzer EO, Malmstrom K, Lu S, et al. Concomitant montelukast and loratadine as treatment for seasonal allergic rhinitis: a randomized, placebo-controlled clinical trial. J Allergy Clin Immunol. 2000 May;105(5):917-22.
25. Pullerits T, Praks L, Ristioja V, Lotvall J. Comparison of a nasal glucocorticoid, antileukotriene, and a combination of antileukotriene and antihistamine in the treatment of seasonal allergic rhinitis. J Allergy Clin Immunol. 2002 Jun;109(6):949-55.
26. Akpek EK, Dart JK, Watson S, et al. A randomized trial of topical cyclosporin 0.05% in topical steroid-resistant atopic keratoconjunctivitis. Ophthalmology. 2004 Mar;111(3):476-82.
27. Cetinkaya A, Akova YA, Dursun D, Pelit A. Topical cyclosporine in the management of shield ulcers. Cornea. 2004 Mar;23(2):194-200.

