Epiphora is a common sign and symptom that’s often a nuisance for our patients. It is usually caused by a blockage located somewhere along the lacrimal excretory system, and leads to an abnormal flow of tears down the cheek. Affected individuals generally complain of constant tearing, while others report intermittent symptoms. Also, epiphora patients typically experience unilateral and/or asymmetric symptoms.

|

|
There are several differentials for epiphora, including dry eye disease, conjunctivochalasis, lid abnormalities and/or nasolacrimal obstructions. Patient history, lid evaluation, lacrimal sac palpitation, slit lamp examination, schirmer testing, dye disappearance and Jones I test, lacrimal dilation and irrigation, lower lid taping, nasal speculum exam and radiography will help you most effectively determine the underlying cause.
Try Rolling the Dye
The dye disappearance test followed by lacrimal dilation and irrigation is essential in determining the correct diagnosis. This test will help you evaluate tear lake malposition, tear pump function and punctal stenosis or blockage of the canaliculus, lacrimal sac or the nasolacrimal duct.
To perform the dye disappearance test, instill 1gtt Fluress (fluorescein sodium 0.25% and benoxinate 0.4%, Akorn) into the lower lid cul-de-sac. The dye should drain properly through the lacrimal excretory system after approximately five minutes, indicating a negative (i.e., normal) result. A positive result, however, is confirmed by an increased tear meniscus or frank epiphora, which suggest a blockage somewhere within the drainage system.
 |
|
| Click here for a narrated video of dilation and irrigation. |
Test the Flow
Lacrimal dilation and irrigation should follow any positive dye disappearance result. Indications for the procedure include canalicular obstruction, intracanalicular plug removal and canaliculitis. Instruments frequently used for dilation and irrigation include a sterile disposable syringe, lacrimal cannula and saline.
Prior to the procedure, topical anesthetic is instilled into the eye. Some ODs may apply additional anesthesia by holding a soaked cotton-tipped applicator against the puncta for several minutes.
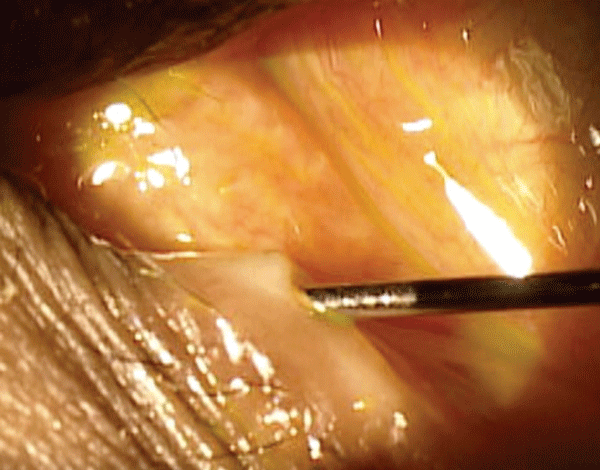
Next, use the index finger of your non-dominant had to gently pull the lid and expose the punctum. The thin-tapered dilator is inserted perpendicularly into the inferior punctum (2mm deep) while the dilator is rolled to expand the puncta. If needed, the punctum can be further stretched by switching to the medium-tapered dilator or by inserting the dilator further into the horizontal canaliculus.
Once the punctum is adequately dilated, the lacrimal cannula is inserted perpendicular to the lid both vertically (2mm deep) and then horizontally (3mm to 4mm deep). Next, apply gentle pressure to the plunger to eject saline into the lacrimal secretory system, which will help remove any obstructions.
A normal result is confirmed when the saline flows freely through the system and the patient feels/tastes the solution in their nose or throat.
If the saline flows out of the inferior puncta and discharges from the superior punctum, a blockage is located at either the common canaliculus or the lacrimal sac. In these cases, further evaluation includes repeating the procedure while occluding the superior punctum with a dilating instrument.
If you observe saline egress from the same punctum you are testing, there is likely a blockage located along the inferior canaliculus. In such instances, a surgical consult may be indicated.

