A 23-year-old white female who wears contact lenses presented for a routine eye exam. The patient reported a decrease in her distance vision but had no other complaints.
She reported no health or ocular history problems. Her only medication was birth control pills. She reported no known drug allergies.
Diagnostic Data
Entering corrected visual acuity was 20/25 O.D. and 20/30 O.S. Pinhole improved her acuity to 20/20 O.U. Pupils were equal, round and reactive to light and accommodation with no afferent pupillary defect. Extraocular muscle motilities were full, and confrontation visual fields were full to finger counting. Manifest refraction revealed a myopic shift to -9.00D O.U. and best-corrected visual acuity of 20/20 O.U. Biomicroscopy was unremarkable. IOP measured 12mm Hg O.D. and 13mm Hg O.S.
Dilated fundus exam was unremarkable. It revealed a 0.3/0.3 cup-to-disc ratio, distinct optic disc margins, flat macula, healthy vasculature and flat periphery in both eyes.
I diagnosed the patient with myopia and dispensed disposable contact lenses. I told her to return in two years.
The patient returned two months later, complaining of decreased vision in her right eye. She reported a persistent slight gray cloudiness in her right eye that had gradually worsened over the previous eight to 10 days. She also reported stationary gray spots that she could not see through and a few sparkles in her vision. She had no significant overall pain, but she did experience mild, nonspecific periocular pressure. She reported no significant pain with eye movements or any other changes in her health.
At this visit, her best-corrected vision was finger counting at 20 feet O.D. and 20/20 O.S. The patient was not wearing her contact lenses because she feared they were causing her vision loss. Pinhole evaluation brought acuity to 20/80+ O.D. Pupils were equal, round and reactive to light and accommodation with no afferent pupillary defect. IOP measured 14mm Hg O.D. and 12mm Hg O.S. Anterior segment examination was completely normal in both eyes.
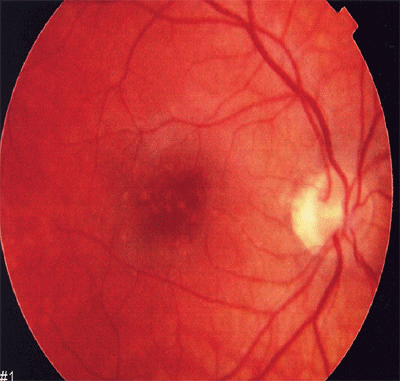
Dilated fundus exam of the right eye revealed similar findings to the previous exam except for the macular region. There were several very small, discrete hypopigmented lesions with hyperpigmented tiny central spots in the central macula (figure 1). There was no subretinal fluid or hemorrhage, and there were no lesions outside the central macula. The vitreous was devoid of cells. The fundus exam of the left eye was unremarkable, with no lesions noted in the macula.
 |
|
1. The right eye revealed several very small, discrete hypopigmented lesions with hyperpigmented tiny central spots. |
Diagnosis
I diagnosed the patient with acute retinal pigment epitheliitis in her right eye.
Treatment and Follow-up
I informed the patient that this is a self-limiting condition that should resolve spontaneously within several weeks. I told her to continue wearing her contact lenses and to return for an evaluation in six weeks, or immediately if her vision worsened.
The patient presented three months later for an evaluation. She said the vision in her right eye had returned to normal and she was too busy to return any earlier. She had no concerns. Her general health and medications had not changed.
Her entering visual acuity was 20/20 O.U. Pupils and all anterior segment structures were normal. Dilated fundus exam showed that the retinal lesions in the right eye completely resolved. There was slight mottling of the retinal pigment epithelium (RPE) that I attributed to the acute pigment epitheliitis.
I informed the patient that her condition resolved with no permanent damage to her potential visual acuity. I informed her that the condition was unlikely to reoccur and instructed her to return in one year.
Discussion
Acute retinal pigment epitheliitis is a rare, self-limiting and usually unilateral disorder that affects healthy young adults.1 It was originally described by Krill and Deutman in 1972 as a disturbance of the RPE in the posterior pole.2-4
Acute retinal pigment epitheliitis presents as an acute or subacute decrease in central vision associated with ophthalmoscopically visible spots in the RPE.2-4 The condition appears to be a benign inflammation of the deeper retinal layers without associated systemic findings, although some patients have reported a preceding flu-like illness.5
The macular lesions are typically deep, dark spots surrounded by yellow-white, halo-like zones, and they often appear in clusters.6 These lesions are usually 0.25DD in size.4 Vitreous cells are rarely observed.3
On fluorescein angiography, the halo-like zones and central dark spots show hyperfluorescence, even in the later phase of the fluorescein.6 The fluorescein angiography does not reveal subretinal leakage.3
The cause of acute retinal pigment epitheliitis is unknown.1,4 It is a localized condition that likely has a viral etiology.3 However, it would seem natural to occasionally find other evidence of ocular inflammation, such as vitritis. The responsible causative agents must find their way to the RPE via the choroidal circulation, so this entity likely represents choriocapillartis in the macular area with secondary pigment epithelium disturbance.3
There is no known treatment for acute retinal pigment epitheliitis.2 Some clinicians have prescribed systemic corticosteroids, but because the disease is self-limiting, it is difficult to determine whether these agents are beneficial.3
Acute retinal pigment epitheliitis has an acute onset of blurring that is typically unilateral and self-limiting (note that the patient perceived the onset as gradual, but it was likely acute). The loss of visual function is out of proportion to the changes in the macula.4 The subnormal visual acuity usually resolves in six to 12 weeks.4,6 Patients may also notice a sudden onset of a unilateral central scotoma but do not report metamorphopsia or altered color vision.2
Results of an electroretinogram are normal, but results of an electro-oculogram are subnormal in the affected eye of patients who have acute retinal pigment epitheliitis. This suggests that the RPE is the primary site of involvement.2
After this condition resolves, the pigment dots become less distinct over time, leaving a subtle area of pigment mottling in the fovea.2,7 Residual window defects in the RPE may also remain.3 The patients vision will return to normal, and no long-standing scotomas are attributed to the disease.
The halo-like lesions that are the hallmark of acute pigment epitheliitis may be present in patients who have other conditionssuch as central serous chorioretinopathy, drusen, adult-onset vitelliform foveomacular (pattern) dystrophy and occult choroidal neovascularizationand in patients who are asymptomatic.4 Two other acute inflammatory disorders that predominantly affect the RPE and bordering neuroepithelium include acute macular neuroretinopathy and acute posterior multifocal placoid pigment epitheliopathy.
The diagnosis of acute retinal pigment epitheliitis typically depends on observation of a subacute, subfoveal pigmentary disturbance.1 All patients regain 20/20 visual acuity and have no further complaints.2 Accurate diagnosis is important to inform patients of the excellent prognosis for visual recovery.2
Dr. Riley is the resident and clinical director of optometry at the Spokane VA Medical Center in Spokane, Wash.
1. Luttrull JK. Acute retinal pigment epitheliitis. Am J Ophthalmol 1997 Jan;123(1):127-9.
2. Chittum ME, Kalina RE. Acute retinal pigment epitheliitis. Ophthalmology 1987 Sep;94(9):1114-9.
3. Jamison RR. Acute retinal pigment epitheliitis with macular edema. Ann Ophthalmol 1979 Mar;11(3):359-61.
4. Gass JD. Inflammatory diseases of the retina and choroid. In: Stereoscopic Atlas of Macular Diseases Diagnosis and Treatment. 4th ed. St. Louis: Mosby, 1997:676-8.
5. Schwartz PL, Rosen DA, Lerner DS, Lichtenfeld PJ. Acute retinal pigment epitheliopathies. Ann Ophthalmol 1981 Oct;13(10):1139-41.
6. Suzuki R, Suga Y, Teranishi H, et al. Diffuse midperipheral acute retinal epitheliopathy. Ann Ophthalmol 1988 Jan;20(1):17-9,22.
7. Prost M. Long-term observations of patients with acute retinal pigment epitheliitis. Ophthalmologica 1989;199(2-3):84-9.

