To See in 3D
We all have a tendency to slip into bad habits, especially as we aim for greater efficiency in our clinical exams. One test that some practitioners may overlook or omit in order to decrease chair time is stereopsis. Many practitioners perform stereo testing on new, younger patients but not established or adult patients in the belief that stereopsis does not change over time or that it is only needed in childhood. As we have observed, however, not only can stereo change, but regular assessment of stereo can provide insight into patients’ overall comfort and binocular stability. Here, we offer you a review of four commonly used stereo tests and discuss their clinical usefulness.
Soft Toric Lenses: Harness This Valuable Practice Opportunity
Experts demystify common misconceptions and offer fitting pearls.Big Things in Small Packages
Q: I have an advanced glaucoma patient who won’t comply with drops, has had SLT and yet continues to progress. What are my options?
Custom vs. Standard Soft Lenses for the Irregular Cornea: How to Choose
Learn which approach works best in this case-based article.The News Feed
Nutraceutical for Dry Eye Coming This Fall
Vision-related QoL Unchanged After Trabeculectomy
Smoking Reduces ONH Vessel Density in Glaucoma
AREDS Report Updates Simplified Severity Scale
Study Finds Prophylactic LPI Cost-Effective for PACS
Red Light Therapy Less Effective in Pre-myopia Phase
MEWDS Characterized by Unique Photoreceptor Damage Patterns
Lamina Cribrosa Pores May Help Identify Severe Glaucoma
Optic Nerve Head Structure Affected by Birth Status
Patient Survey Describes Dry Eye Management Habits, Burdens
Study: Epi-off Accelerated CXL Yields Good Results
Heavy Smoking, High BMI Associated With Earlier Onset nAMD
Access to Pediatric Eye Care Severely Lacking Across the US
Statins Decrease Graves’ Ophthalmopathy Risk
Glaucoma Rate 3x Higher in Poor and Minority Populations
Dry Eye Patients Have Worse Sleep Quality
New Punctal Plug Features Tapered End for Easier Insertion
Glaucoma-related Blindness Decreased Between 2000 and 2020
Structural Complications Not Specific to High Myopia
Look Inside The Current Issue
Features
Advances in Endothelial Surgery: An Update for ODs
Corneal Cases: Which are Right For You?
Building a Top-Flight Staff
Corneal Pain Presentations: Causes and Interventions
Sizing Up Keratoconus: The Roles of Topography and Tomography
Departments
Attack of the Clones
Big Things in Small Packages
Corneal and Allergy Conundrums
Enough Data to Track Glaucoma Patients?
Flashes? Think Beyond the Retina
Hot Topic
The Enemy Within
Twin Tumor Therapies
Upcoming Events
Continuing Education
Corneal Pain Presentations: Causes and Interventions
OCT Beyond the Basics: Unlocking the Power of This Essential Tool
Demystifying the Complement System
The Physical Manifestations of Glaucoma and What They Signify
Additional Publications
-
The Value of Real Tears
Francis Mah, MD, and Jessica Steen, OD, FAAO, discuss the importance of a stable tear film, how real tears help maintain the health of the ocular surface and the effect that various dry eye interventions can have on tear film homeostasis.
Sponsored by Viatris A Wider View Of The Retina Advances Care
It’s Time to Talk to Your Patients about Digital Eye Strain
New Developments in Glaucoma
Ophthalmic Product Guide - February 2024
Preservatives in Eye Care: Intrepid Eye Society Consensus Discussion
Review of Cornea & Contact Lenses
-
Custom vs. Standard Soft Lenses for the Irregular Cornea: How to Choose
Learn which approach works best in this case-based article. -
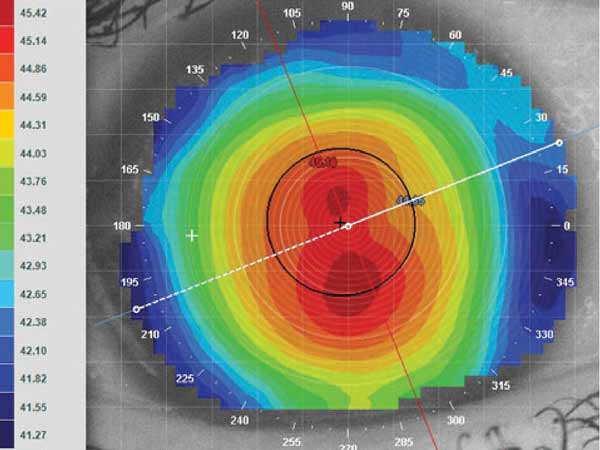
Corneal Topography: Get to New Heights
See how elevation data reveals the greatest truths about corneo-scleral shape. -
Soft Toric Lenses: Harness This Valuable Practice Opportunity
Experts demystify common misconceptions and offer fitting pearls. -
Wave Hello to Wavefront-Guided Sclerals
These lenses are a great option for those with residual higher-order aberrations but also can be used to create excellent multifocals. -
GP Multifocal Contact Lenses: The 2024 Lineup
Recent design advancements give clinicians even more options to help meet patients’ vision demands. -
Empirical Fitting of GP Lenses
Advanced technology has paved the way for a quite easy and successful approach.

Women In Optometry continues to be published online, with regular updates on practice design, practice success, news, trends and perspectives. Visit womeninoptometry.com.