 A 35-year-old Hispanic male presented for a LASIK screening to determine if he was a suitable candidate. He said that he had worn glasses since childhood and wanted to learn if LASIK could provide him with freedom from corrective lenses. His medical history was unremarkable. He reported using no medications.
A 35-year-old Hispanic male presented for a LASIK screening to determine if he was a suitable candidate. He said that he had worn glasses since childhood and wanted to learn if LASIK could provide him with freedom from corrective lenses. His medical history was unremarkable. He reported using no medications.
On examination, his best-corrected visual acuity measured 20/20 O.U. Confrontation fields were full to careful finger counting O.U. Extraocular motility testing was unremarkable. His pupils were equally round and reactive, with no afferent pupillary defect. The anterior segment examination was unremarkable.
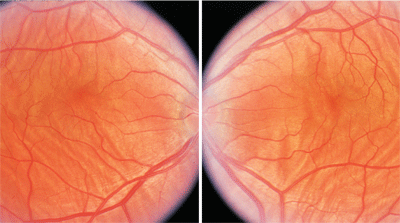
Dilated fundus examination showed small cups, with good rim coloration and perfusion in both eyes. The vessels were of normal caliber and the periphery was unremarkable. However, we documented significant changes seen throughout the posterior poles of both eyes (figures 1 and 2).
3. In some cases, fluorescein angiography (FA) might provide a more detailed illustration of choroidal folds, as seen here.
Take the Retina Quiz
1. What are the obvious changes seen throughout the posterior poles of both eyes?
a. Subretinal fluid.
b. Subretinal tracks.
c. Choroidal folds.
d. Retinal striae.
2. What is the etiology of this finding?
a. Inflammation.
b. Hypotony.
c. Orbital tumor.
d. Idiopathic.
3. What form of refractive error does this patient likely have?
a. Cannot be determined.
b. Moderate to high myopia.
c. Moderate to high hyperopia.
d. Emmotropia.
4. What additional test would be helpful to confirm the diagnosis?
a. Fluorescein angiography.
b. Magnetic resonance imaging (MRI).
c. Optical coherence tomorgraphy (OCT).
d. Standardized ultrasound.
5. How should this patient be managed?
a. Observation.
b. Referral for an MRI.
c. Referral to a retinal specialist for evaluation of hypotony.
d. Referral for LASIK.
For answers, see below.
Discussion
The striking fundus changes seen in our patient are choroidal folds. Choroidal folds represent folds or wrinkles in the inner portion of the choroid, retinal pigment epithelium (RPE) and neurosensory retina. Choroidal folds often appear as alternating light and dark horizontal bands located posterior to the equator, usually in the posterior pole. In our patient, this presentation is very prominent and can be seen throughout the entire posterior pole.
Choroidal folds develop as a result of scleral shrinkage or thickening that results from a variety of causes, such as orbital inflammatory disease (posterior scleritis or inflammatory pseudotumor), hypotony following intraocular surgery, choroidal neovascularization, and orbital tumors.1,2 Any of these conditions can cause a reduction of the sclera’s inner surface. Because the choroid and RPE are immune to this process, the tissues become redundant, yielding choroidal folds.
Choroidal folds are quite common in moderate to high hyperopes, because these patients have shorter axial lengths and thicker scleras (as measured by standardized ultrasound) than normal patients. Interestingly, the refractive error in out patient was approximately +7.50D. We did not obtain an ultrasound, but on clinical examination, his globe and other anatomic structures appeared small. In fact, gonioscopy is strongly recommended for most patients with small structures and narrow angles because of an increased risk for angle-closure glaucoma. We performed gonioscopy on our patient, and his angle was wide open to the ciliary body
Typically, choroidal folds are idiopathic and are discovered as an incidental finding during a routine eye exam. The folds may involve most of the posterior pole, or may be confined to an area either above or below the macular and optic disc. Their distribution is usually bilateral and symmetric, and may be associated with small amounts of hyperopia. In most instances, visual acuity remains unaffected. Choroidal folds can occur in patients of any age, but are more commonly seen in middle-aged adults. Also, they can be unilateral, but are more commonly bilateral.
A diagnosis of choroidal folds is generally based on the clinical appearance; however, in some cases, fluorescein angiography (FA) might provide a more detailed illustration (figure 3). FA will demonstrate hyperfluorescence at the crest of the fold as well as relative hypofluorescence at the trough due to the thickened and folded RPE. We did not perform FA on our patient because the folds were obvious, and we believed that it would not provide any additional information.
Ultrasound is perhaps the most important diagnostic test because it helps rule out any underlying causes of choroidal folds. In most cases, a B-scan shows flattening of the posterior pole and thickening of the choroid and sclera. This is likely the result of scleral and/or retrobulbar inflammation, which, in turn, leads to subsequent scleral shrinkage.1 We did not perform an ultrasound on our patient due to the high amount of hyperopia and the bilateral nature of the presentation.
We discussed the findings with our patient and informed him that he was not a good candidate for a LASIK procedure.
1. Gass JD. Stereoscopic atlas of macular diseases, diagnosis and treatment. St. Louis: C.V. Mosby Company, 1987:222-34.
2. Cohen SM, Gass JD. Bilateral radial chorioretinal folds. Int Ophthalmol. 1994-1995;18(4):243-5.
Retina Quiz Answers: 1) c; 2) d; 3) c; 4) d; 5) a.

