 Q: I have an elderly patient with vitreomacular adhesions (VMA). I normally send these patients out for surgery, but she’s reluctant to have an eye operation at her age. Are there any other options?
Q: I have an elderly patient with vitreomacular adhesions (VMA). I normally send these patients out for surgery, but she’s reluctant to have an eye operation at her age. Are there any other options?
A: Until recently, the only two options had been observation and vitrectomy—or, more likely, observation until vitrectomy, says Ajey S. Alurkar, MD, vitreoretinal specialist at Omni Eye Services, in Atlanta.
Bear in mind that the problem resolves on its own in about 10% percent of these patients, he says. “So, if you had a patient with vitreomacular traction (VMT), vitreomacular adhesions or early-stage macular holes, you’d watch and wait, but eventually book the patient for surgery,” Dr. Alurkar says.
Vitrectomy is not exactly a cakewalk for the patient, he says. “Once you do vitrectomy surgery, you’re automatically committing the patient to a second surgery, because that lens is going to mature into a cataract within six months to five years.” Not to mention, the patient will be facing the risks of retina surgery as well as spending at least a few days post-op facing the floor.
The good news is there’s now a new option for symptomatic patients: Jetrea (ocriplasmin, ThromboGenics) is a one-time intravitreal injection that basically dissolves the vitreous attachments to the retina. It was approved by the FDA in October 2012 and became available in January 2013.
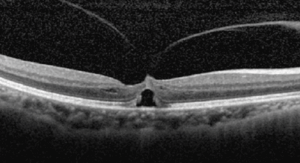
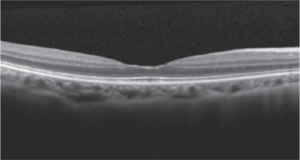
OCT of the macula shows vitreomacular traction (left). Less than a month after Jetrea injection, the problem has resolved (right).
“Now, when a patient comes in with an early stage macular hole, I say, ‘I’m going to schedule you for surgery, but I’m going to inject this into your eye first. There’s a 40% chance it will fix the hole within 28 days. And if it doesn’t fix it, then we’re going to take you into surgery as planned,’” Dr. Alurkar says. He adds that the success rate for VMA or VMT is around 30%.
A second injection of Jetrea is not recommended. “If it doesn’t work the first time, it’s likely not going to work at all,” he says. Also, be aware that a single shot costs the patient $4,000. “But, if it works, it saves a lot of time and trouble for both the surgeon and the patient, and it also saves the patient’s lens.”
Optical coherence tomography is essential for diagnosing VMA, VMT or macular holes, Dr. Alurkar says. So, if you don’t have one of these instruments, and you have a patient with flashes, floaters or visual distortion that you just can’t diagnose, be sure to send the patient for an OCT scan or to a retinal specialist, he says.
If you do have an OCT, and the patient lives far from the surgeon, you could offer to do the scan at day 28 to see if the injection worked.
Patients with multiple vitreomacular attachments, as seen on OCT, are probably not good candidates for Jetrea, Dr. Alurkar advises. Likewise, patients should not be given this treatment if they have high myopia (greater than 8.00D), a history of prior retinal detachment, a macular hole greater than 400μm in diameter, or have other ischemic retinal diseases that affect their vision.

