 A 55-year-old white man presents complaining of chronically red, irritated eyes. The problem has waxed and wanedbut it has never completely disappearedover the past several years. He has used many topical therapies, including artificial tears, steroids, antibiotics, steroid/antibiotic combinations and lid hygiene regimens. All seem to offer some benefit. Once, when the problem was at its most severe level, he was prescribed oral doxycycline, which he used over the course of three months with moderate success.
A 55-year-old white man presents complaining of chronically red, irritated eyes. The problem has waxed and wanedbut it has never completely disappearedover the past several years. He has used many topical therapies, including artificial tears, steroids, antibiotics, steroid/antibiotic combinations and lid hygiene regimens. All seem to offer some benefit. Once, when the problem was at its most severe level, he was prescribed oral doxycycline, which he used over the course of three months with moderate success.
At examination, his visual acuity is unaffected. He manifests mild conjunctival injection in each eye. The eyelid margins demonstrate telangiectasis and an irregular surface. There are multiple capped glands, and a cheesy sebum can be manually expressed from them. There is also a mild punctate corneal epitheliopathy inferiorly O.U. Also notable are telangiectasias on the nose and cheeks, as well as a mild degree of rhinophyma.
The patient clearly has meibomian gland dysfunction (MGD)and likely ocular rosacea as well. This meibomian gland abnormality can be very difficult to manage, as evidenced by the patients use of multiple therapies with marginal success.
Perhaps, it is time to try something different. A new topical formulation of azithromycinFDA- approved for the treatment of bacterial conjunctivitismay benefit such patients. This month, we look at the science behind a new medication for off-label management of MGD and rosacea.
Conditions
Blepharitis is a generic term for inflammation of the eyelids that is often precipitated by local bacterial colonization. It generally involves the eyelashes and eyelid margin, including the sebaceous glands deep within the tarsus. Patients chronic disease may be linked to poor hygiene, or there may be an underlying dermatological condition (such as rosacea) contributing to the problem.
MGD is associated with chronic obstruction and inflammation of the meibomian glands, which results in accumulation of meibomian secretions, or meibum, within the glands. Colonizing bacteria target the meibum, altering normal secretion composition and consistency, making it thicker and less soluble.1-4 This can result in tear film instability secondary to abnormal lipid secretion, with resultant evaporative dry eye and associated symptoms of grittiness and irritation. Chronic meibomian duct obstruction may result in hordeola and/or chalazia.
Recalcitrant forms of MGD may be associated with rosacea, a generalized dermatologic condition that affects the sebaceous glands of the faceparticularly the nose, cheeks, forehead and periorbital regions.2,3 Though bacterial infection is not a major cause of MGD, tetracycline and its derivatives (e.g., doxycycline or minocycline) have been shown to inhibit bacterial lipase production and reduce free fatty acids, and have been effective in controlling severe or recalcitrant MGD.5
Specific signs of rosacea include periodic skin flushing, visible telangiectasis of the affected skin, inflammatory papules or pustules and rhinophyma. Patients often report a burning sensation that coincides with instances of flushing. Ocular signs associated with rosacea may include a recalcitrant posterior blepharitis with inspissation of the meibomian glands.6 The condition may be initiated when the glands become colonized by bacteria (typically Staph. aureus or Propionibacterium acnes) that release enzymes and upset the lipid components proper composition.7 Ocular rosacea can produce a chronically dry eye secondary to evaporative processes, which spawns a perpetual cycle of local inflammation and degenerative changes in the skin (ulcerative blepharitis), resulting in meibomianitis, hordeola, chalazia, and in severe cases, scarring of the tissues of the eyelid and globe. Traditional therapy for ocular rosacea consists of oral tetracycline or macrolide therapy. (For more on this, see Soothe the Burn of Ocular Rosacea, June 2008.)
A Topical Alternative?
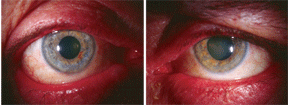
This patient presented with blepharitis and rosacea (O.D. left, O.S. right). Used off-label, the topical formulation of azithromycin may be of some benefit.
Azithromycin is a macrolide antibiotic that exerts its action by binding to the 50S ribosomal subunit of susceptible bacteria, interfering with microbial protein synthesis. It is commonly prescribed in oral form for sinusitis, upper respiratory infections and chlamydia. AzaSite (Inspire Pharmaceuticals) is a 1% topical formulation of azithromycin contained in a novel vehicle, DuraSite. It is FDA-approved for the management of bacterial conjunctivitis caused by susceptible organisms.8
Recently, a two-week preliminary clinical trial evaluated the safety and efficacy of topical 1% azithromycin solution in combination with mechanical therapy vs. mechanical therapy alone in subjects with MGD (posterior blepharitis).9
In this study, 21 patients with moderate to severe MGD were recruited and studied to assess the efficacy of topical 1% azithromycin solution in conjunction with hot compresses vs. hot compresses alone in alleviating the signs and symptoms of MGD. Subjects in the study had signs and symptoms of MGD, including redness or swelling of the eyelid margin, eyelid debris and plugging of the meibomian glands.The dosing schedule of topical 1% azithromycin solution was one drop in each eye b.i.d. for two days, then one drop in each eye q.d. for 12 days. The hot compress regimen involved a 10-minute application twice daily for the duration of the study. The study identified several distinct benefits regarding the use of topical azithromycin combined with hot compresses vs. hot compresses alone. When examining the degree of meibomian gland plugging, there was a 70% improvement from baseline in the topical azithromycin group compared to hot compresses alone; 44% of the topical azithromycin patients demonstrated no meibomian gland obstruction in at least one eye, whereas no patient in the hot compress group was relieved of meibomian gland obstruction.9
Assessment of meibomian gland secretion ranged from completely clear to completely blocked, or with a paste-like secretion in those individuals whose glands were not completely blocked. In terms of secretion quality, there appeared to be some benefit to the use of topical azithromycin solution, with a 68% improvement from baseline in the treatment group compared to an 11% improvement in the hot compress group.9
After two weeks of treatment, 22% of patients treated with topical azithromycin and hot compresses experienced a normalization of meibomian gland secretions. No patient in the hot compress group achieved meibomian gland secretion normalization.9
Patients who used the topical azithromycin also experienced lessening of eyelid margin rednessoverall, by 69%, as compared to an improvement of 10% in the group using hot compresses alone.9
Additionally, a greater proportion of patients treated with the topical azithromycin solution reported symptomatic improvement compared to those who used hot compresses alone. Topical azithromycin was seen to be safe and well tolerated throughout the study, with only one patient reporting intermittent stinging and blurring.
Clinical Application
It appears that the use of topical 1% azithromycin solution may be a clinical option in the management of patients with MGD, and perhaps even ocular rosacea, a more severe form of MGD. A significant advantage may be the easy once-daily maintenance dosing, which could be an improvement over the long-term use of oral doxycycline in these patients.
Indeed, these results suggest that there may be a benefit in the off-label use of AzaSite for patients with MGD. However, we want to caution readers against accepting this information as conclusive clinical data at this time. Keep in mind that, in the preliminary clinical trial, there was only a small number of subjects and the trial itself was short. This information is merely preliminary; these results must yet undergo the scrutiny of the peer review process. Still, such research is encouraging, and it is these types of studies that ultimately help to shape the future of clinical care. For now, AzaSite appears to be a safe, easy-to-use topical therapy that may benefit patients with MGD.
The authors have no direct financial interest in any product or company, nor have they received financial support from any company mentioned in this article.
1. Smith RE, Flowers CW Jr. Chronic blepharitis: a review. CLAO J 1995 Jul;21(3):200-7.
2. Driver PJ, Lemp MA. Meibomian gland dysfunction. Surv Ophthalmol 1996 Mar-Apr;40(5):343-67.
3. Quarterman MJ, Johnson DW,
4. McCulley JP, Shine WE. Changing concepts in the diagnosis and management of blepharitis. Cornea 2000 Sep;19(5):650-8.
5. Dougherty JM, McCulley JP, Silvany RE, Meyer DR. The role of tetracycline in chronic blepharitis. Inhibition of lipase production in staphylococci. Invest Ophthalmol Vis Sci 1991 Oct;32(11):2970-5.
6. Mackley CL, Thiboutot DM. Diagnosing and managing the patient with rosacea. Cutis 2005 Apr;5(4 Suppl):25-9.
7. McCulley JP, Shine WE. The lipid layer of tears: dependent on meibomian gland function. Exp Eye Res 2004 Mar;78(3):361-5.
8. Inspire Pharmaceuticals Inc. AzaSite package insert, May 2007.
9. A single-center, open-label, randomized pilot study of the safety and efficacy of AzaSite ophthalmic solution, 1% in combination with mechanical therapy versus mechanical therapy alone for two weeks in subjects with posterior blepharitis. Available at: http://clinicaltrials.gov/show/NCT00629590. Study ID Number: 041-106. (Accessed September 2008).

