 History
History
A 68-year-old white female presented for an urgent visit with a chief complaint of severe ocular pain and reduced visual acuity in her left eye. She reported that her symptoms manifested fairly suddenly and persisted for one day. She denied any history of recent ocular trauma.
Her ocular history was significant for progressive bilateral cataracts; however, we documented no acute abnormalities at her previous routine ocular health examination eight months earlier. She did not use any ocular medications.
Her systemic history was significant for hypertension, which was controlled with oral beta blockers. She reported no allergies.
Diagnostic Data
Her best-corrected visual acuity measured 20/25 OD and 20/400 OS at distance through habitual +1.25D sphere/+2.50D bifocal spectacles. Refraction revealed no changes to her spectacle prescription.
External examination was unremarkable, with no evidence of afferent pupillary defect.
Her intraocular pressure measured 16mm Hg OD and 51mm Hg OS. Undilated 90D funduscopic examination revealed quiet grounds and normal posterior poles, with a cup-to-disc ratio of 0.40 x 0.40 OU.
Your Diagnosis
How would you approach this case? Does the patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
Any time that you document an abnormally elevated IOP measurement, you must perform gonioscopy to view the angle structures. In cases that exhibit an acute pressure increase, use a small gonio lens (e.g., Posner or Sussman 4-mirror) to facilitate the execution of Forbes’ compression gonioscopy. The Forbes’ compression technique (or indentation gonioscopy, as it is sometimes called) allows you to distinguish between a zippered or syneched angle closure and an appositional or anatomic angle closure. (In cases of a zippered closure, Forbes’ compression typically fails to reveal the angle structures, while the rocking/pushing pressure of the technique depresses the iris diaphram, revealing structures in angles that are not synechially closed.)
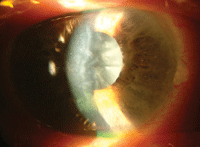
The left eye of our 68-year-old patient who complained of severe pain and reduced visual acuity.
The diagnosis in this case is phacomorphic angle closure. In our patient, a hypermature cataract caused the crystalline lens to thicken to a point where mechanical contact with the iris interrupted aqueous outflow. This problem is fairly uncommon and can be remedied with prompt pharmaceutical intervention and cataract extraction.1-4
Some hypermature lenses break down (phacoanaphylaxis). In these instances, their proteins can induce blockage of the trabecular meshwork (TM) or induce an iritis, where the cells and flare of the inflammation create TM obstruction.4
Alternatively, a YAG laser peripheral iridotomy could be attempted to create a communication channel between the anterior and posterior chambers.
Finally, atropinization could be attempted; however, cycloplegic agents generally are ineffective in cases of phakic iridolenticular touch. Ultimately, the ideal solution is lensectomy with intraocular lens implantation.1-4
In our patient, we initiated immediate therapy with topical timolol 0.5% BID, apraclonidine BID and prednisolone acetate 1.0% Q2H as well as 500mg acetozolomide BID to lower her intraocular pressure and reduce inflammation. The patient was prescribed timolol BID, apracloniodine, BID OS and given one additional 500mg acetazolamide capsule for the morning. An ophthalmology consult was arranged for 24 hours to rule out the need for prompt surgical intervention. The ophthalmologist concurred with our diagnosis and treatment of the acute event, and recommended emergent cataract extraction to reverse the process.
The topical and systemic therapy reduced the acute intraocular pressure in her left eye to 30mm Hg within 90 minutes. The IOP, measured at the ophthalmologist’s office, was 18mm Hg the next day. Subsequent cataract extraction yielded an excellent final outcome, with resolution of the pressure issue.
Thanks to Marc D. Myers, OD, of Coatesville, Pa., for contributing this case.
1. Tham CC, Lai JS, Poon AS, et al. Immediate argon laser peripheral iridoplasty (ALPI) as initial treatment for acute phacomorphic angle-closure (phacomorphic glaucoma) before cataract extraction: a preliminary study. Eye. 2005;19(7):778-83.
2. Rao SK, Padmanabhan P. Capsulorhexis in eyes with phacomorphic glaucoma. J Cataract Refract Surg. 1998;24(7):882-4.
3. Lee JW, Lai JS, Lam RF, et al. Retrospective analysis of the risk factors for developing phacomorphic glaucoma. Indian J Ophthalmol. 2011; 59(6):471-4.
4. Papaconstantinou D, Georgalas I, Kourtis N, et al. Lens-induced glaucoma in the elderly. Clin Interv Aging. 2009; 4(8):331-6.

