 A 15-year-old Hispanic male presented following a referral from his pediatrician. Recently, the patient noted difficulty with his distance vision. At the time of the examination, he was undergoing genetic testing for a potential diagnosis of Marfan syndrome.
A 15-year-old Hispanic male presented following a referral from his pediatrician. Recently, the patient noted difficulty with his distance vision. At the time of the examination, he was undergoing genetic testing for a potential diagnosis of Marfan syndrome.
His entering visual acuity measured 20/40 OU. With a small myopic correction, his vision improved to 20/20 OU. Confrontation visual fields were full to careful finger counting OU. His pupils were equally round and reactive, without evidence of afferent defect.
Extraocular motility testing was normal. The slit-lamp examination was unremarkable. His intraocular pressure measured 13mm Hg OU. Dilated fundus examination of the right eye revealed obvious changes (figure 1).
Take the Retina Quiz
1. How would you describe the remarkable blood vessel pattern observed in figure 1?
a. Venous tortuosity and engorgement.
b. Arteriovenous (AV) malformation.
c. Dilated afferent and efferent vessel.
d. Blood vessel sheathing.
2. What does this finding represent?
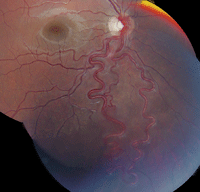
1. Fundus photograph of the right eye shows a very interesting vessel pattern exiting the optic nerve. What is the correct diagnosis?
a. Hemangioma.
b. Retinal angioma.
c. Neovascularization.
d. Genetic disorder.
3. What is the correct diagnosis?
a. Combined hamartoma of the retinal pigment epithelium.
b. Capillary hemangioma of the retina.
c. Racemose hemangioma of the retina.
d. Von Hippel-Lindau disease.
4. What further testing is warranted?
a. Neuroimaging.
b. Blood pressure measurement.
c. Ultrasonography.
d. Chest X-ray.
5. What significant ocular finding would you expect to see if the patient had Marfan syndrome?
a. Choroidal hemangioma.
b. Optic nerve glioma.
c. Port wine staining.
d. Lens subluxation.
For answers, scroll down.
Discussion
The prominent dilated retinal artery and vein seen exiting the optic nerve of the patient’s right eye represents an abnormal congenital AV malformation. This particular finding is termed Racemose hemangioma of the retina (also referred to as Wyburn-Mason syndrome). This condition is one of the phakomatoses––a collection of disorders characterized by systemic hamartomas of the eye, brain, skin, and sometimes the viscera and bones.1 Even though Racemose is classified as a “hemangioma,” there is no distinct tumor present.
Interestingly, 30% of patients with this condition also have similar vascular malformations located elsewhere in the body––most commonly in the midbrain.1 In some cases, retinal lesions may be an extension of an intracranial vessel abnormality that has extended anteriorly along both the visual pathway and the optic nerve toward the retina.
The ocular/retinal manifestations of Racemose hemangioma include one or more dilated, tortuous arteries that emerge from the optic disc and extend into the retina. The arteries typically form a distinct AV communication with a similarly dilated vein, as was seen in our patient. The AV anastomoses exhibit variable alterations in capillary and arteriolar networks, and visual symptoms are related to the size, extent and location of the abnormal vascular process. The AV malformations can vary dramatically, presenting as only subtle alterations located within the capillary system to more profound anatomical changes (as seen in this case).
In some patients, the AV anastomoses can involve the entire fundus. Such massive presentations have been described as resembling a “bag of worms,” and are often associated with more severe vision loss. More advanced retinal lesions also have a higher incidence of central nervous system involvement.
Racemose hemangiomas usually are non-progressive. Orbital AV malformations may be associated with mild proptosis, conjunctival vascular dilatation or a bruit.
Except for fluorescein angiography (FA), ancillary testing contributes little information to the diagnosis. The FA exhibits early, rapid arteriole filling as the eye passes through the AV communication back toward the optic disc with a short transit time. In stark contrast to capillary hemangioma, no leakage is observed from the retinal vessels during its late phases.
Neurologic symptoms may be present, depending on lesion size, location and configuration. Patients can exhibit mental changes, headaches, seizures, visual field abnormalities and cranial nerve palsies. Other systemic complications include subarachnoid hemorrhage, hydrocephalus, cognitive deficiencies and gingival hemorrhages secondary to AV malformations in the maxilla/mandible.
In most cases of Racemose hemangioma, the retinal vascular lesions remain stable and are not treated. A neurologic evaluation is recommended, including an MRI or CT scan to rule out central nervous system (CNS) involvement.
Our patient’s MRI showed no CNS involvement. Also, the genetic testing for Marfan syndrome was normal. So, exempting annual eye examinations, our patient will not require any additional follow-up care going forward.
1. Shields CL, Shields JA. Phakomatoses. In: Ryan SJ, Schachat AP, Murphy RP (eds). Retina, Vol. III: Section 1, Chapter 132. Tumors of the Retina. 5th ed. St. Louis: Mosby; 2013:2170-83.
Answers
1. b
2. a
3. c
4. a
5. d

