 |
|
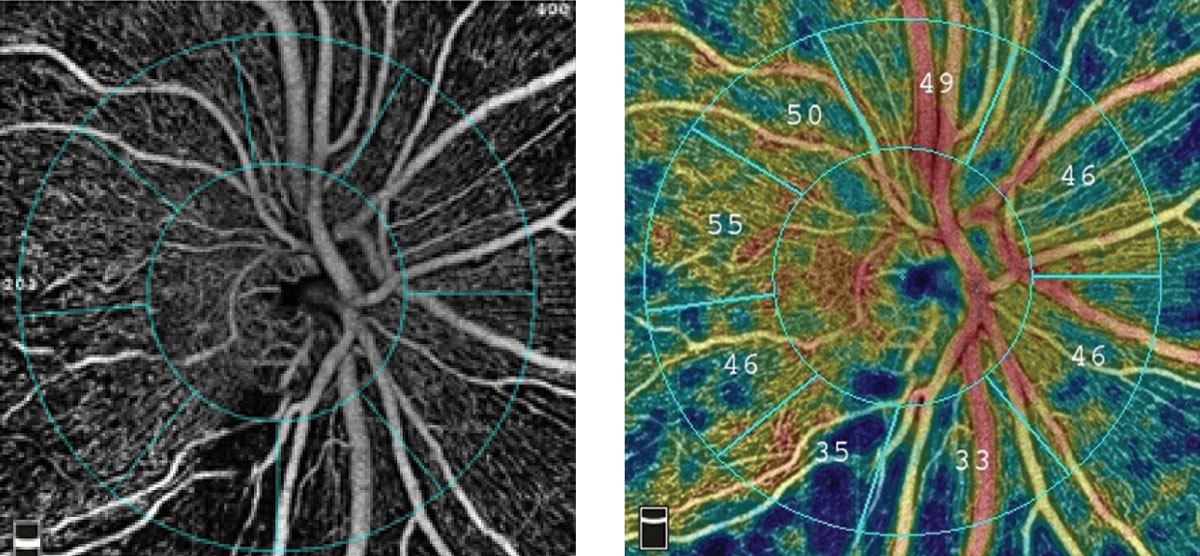
OCT angiography is more resilient in advanced glaucoma, one reason the technology improves clinical assessment of the disease. Photo: Optovue. Click image to enlarge. |
While structural OCT metrics like retinal nerve fiber layer (RNFL) thickness have become an indispensable tool when diagnosing and following glaucoma, the technology’s angiographic capabilities (OCTA) have not as routinely been incorporated into clinical practice. One new study demonstrates the power OCTA has as an emerging technology, especially when used in tandem with structural OCT to predict the severity of paracentral visual field loss for patients with primary open-angle glaucoma (POAG).
The prospective study included 44 patients with POAG and 42 control subjects, all of whom underwent both OCTA and OCT imaging. OCTA parameters of the circumpapillary microvasculature—specifically vessel density and vessel flow (cpFlow)—were recorded. Structural OCT measured RNFL thickness as well as Bruch’s membrane opening-minimum rim width (BMO-MRW). This model with all four parameters was measured against one that only included structural OCT findings.
Results indicated that POAG patients had findings lower across the board than controls in the affected hemisphere. Paracentral total deviation was better predicted in the model that included RNFLT, BMO-MRW and OCTA parameters.
The reason the combined model works better, the researchers explained in their paper, is because of what OCTA adds to the appreciation of pathophysiology in glaucoma. Compromised blood flow is seen in glaucoma, especially in systemic vascular abnormalities like hypotension or migraine, both conditions associated with paracentral visual field loss. Anatomically, the superficial vascular plexus is what supplies the circumpapillary and parafoveal areas. Thus, since the study measured superficial vasculature of the circumpapillary region, it may have been measuring the area most affected in paracentral visual field loss.
An additional advantage to OCTA is its sustained accuracy even in advanced glaucoma. While structural OCT metrics like RNFL thickness can be susceptible to a “floor effect” once neuronal loss is substantial enough to prevent detection of additional changes, OCTA provides information about the microvasculature that can still be captured in late-stage disease.
The study authors acknowledge that “OCTA is not yet routinely incorporated in glaucoma clinical care, in part due to imaging challenges such as the presence of artifacts, difficulty in segmentation of the optic nerve and reproducibility given the variety of OCTA devices available.” Nevertheless, they believe that “because microvascular pathology likely plays an important role in the pathophysiology of paracentral VF loss, adding OCTA may lead to better diagnosis and disease monitoring for patients with this type of VF loss.”
Xu C, Saini C, Wang M, et al. Combined model of OCT angiography and structural OCT parameters to predict paracentral visual field loss in primary open-angle glaucoma. Ophthalmol Glauc. 2022. [Epub ahead of print]. |

