
Acute primary angle closure is an ocular emergency where hours can make the difference in a patient’s final visual outcome. If left untreated, primary angle closure glaucoma—a major cause of blindness worldwide—can occur and prompt intervention will be needed to preserve vision.1-3 Primary angle closure most commonly occurs when aqueous flow from the posterior to anterior chamber is blocked at the pupil by contact between the iris and the lens, leading to an increased intraocular pressure (IOP) in the posterior chamber and a forward bowing of the peripheral iris (known as iris bombé). As the peripheral iris bows forward, it makes contact with the trabecular meshwork and blocks the outflow of aqueous from the eye, leading to an elevated IOP. As the iris continues to touch the trabecular meshwork, it can form peripheral anterior synechiae. This can occur acutely, causing an angle closure attack, or proper aqueous flow may be restored spontaneously, resulting in a subacute/intermittent or chronic disease course.
Primary angle closure can occur by non-pupil block mechanisms as well, such as angle crowding from a thickened peripheral iris stroma, or plateau iris syndrome.1,2
The Patient Experience
Primary angle closure is more common in people of Asian or Inuit decent and usually occurs in female patients with hyperopia, shorter axial length and a thickened crystalline lens.1 Prolonged exposure to dim illumination or topical medications, such as tropicamide 1.0% or vasoconstrictors such as tetrahydrozoline 0.05% (found in Visine eye drops) may cause at-risk patients to develop an acute angle closure attack.
Patients with an acute angle closure attack will experience blurry vision with halos around lights, nausea, vomiting, headaches and severe eye pain. Slit lamp exam findings include conjunctival hyperemia, microcystic and stromal corneal edema, a shallow anterior chamber with cells and flare, iris bombé and a classic mid-dilated pupil.
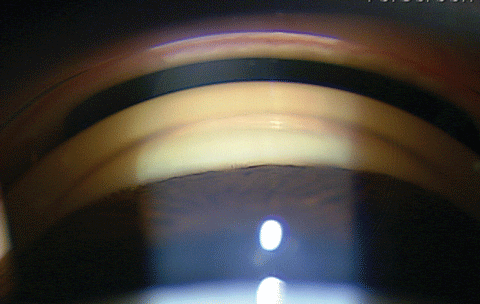 |
| This semi-narrow angle patient is a candidate for the laser peripheral iridotomy. Click image to enlarge. |
The mid-dilated pupil occurs in acute angle closure for two reasons. First, the greatest amount of iris/lens contact occurs when the pupil is mid-dilated—this is why angle closure attacks commonly occur hours after patients are dilated as the drops start to wear off and the pupil begins to return to normal size. As the IOP increases to above 40mm Hg, the iris sphincter muscle becomes ischemic and can no longer constrict the pupil. Iris pigment cells may be liberated into the anterior chamber and coat the endothelium and anterior lens capsule. Residual iris atrophy is common after acute angle closure attacks. Glaucomflecken, whitish opacities on the anterior lens capsule, may also be present. Glaucomflecken is a result of lens epithelial cell necrosis from the elevated IOP. If the IOP remains elevated long enough, glaucomatous optic neuropathy may occur, resulting in primary angle closure glaucoma.
Diagnosis
Compression gonioscopy is key to properly diagnosing an acute angle closure. On slit lamp examination, the anterior chamber will be shallow and only anterior trabecular meshwork or Schwalbe’s line will be visible on gonioscopy. The corneal wedge technique, using an optic section to find the end of Descemet’s membrane, can be helpful in determining your location within the angle. On compression of the cornea with a flange-less gonioscopy lens, the iris should indent, exposing at least the posterior trabecular meshwork, implying appositional angle closure. This may help to break the angle closure attack. However, if no deeper structures are seen, then peripheral anterior synechiae are present and the angle is closed. In this scenario, a laser peripheral iridotomy is contraindicated and filtration surgery or goniosynechialysis should be considered. Other possible causes of secondary angle closure should also be explored, such as neovascular or inflammatory glaucoma. Anterior segment optical coherence tomography (AS-OCT) can also be useful in identifying angle structures and showing angle closure, especially if the cornea is cloudy from edema. The cornea can be cleared using glycerin, a topical hyperosmotic, to perform gonioscopy or a laser peripheiral ididotomy.
Medications
Therapeutic agents used for acute angle attacks include topical beta blockers, alpha-2 agonists, carbonic anhydrase inhibitors and prostaglandin analogs—even though their onset of action may be delayed. Topical drops are given every five minutes for 30 minutes and the pressure is rechecked in one hour. Additionally, oral carbonic anhydride inhibitors, such as 1,000mg oral acetazolamide, are given as long as the patient does not have kidney disease or a sulfa allergy. Oral acetazolamide should be given as the immediate release tabs and not the extended release version. If the pressure is still not down at the one-hour check, apply more drops and check the pressure in another hour.
Paracentesis
At this point, if the pressure is not responding and is at a sight-threatening level, it’s time to consider an emergent paracentesis. This can be performed easily at the slit lamp with a lid speculum, sterile 30g needle and Betadine. First, the eye is numbed with a topical anesthetic eye drop and the lid speculum is placed. Topical Betadine drops are applied, and the patient is positioned in the slit lamp. A 30g-needle attached to a 1ml tuberculin syringe with the plunger removed is inserted tangentially into the cornea, parallel to the iris, as close to the limbus as possible. Extreme care must be taken to not hit the iris or lens during this procedure, which can be difficult due to the shallow anterior chamber. If the needle cannot be safely inserted, a paracentesis should not be performed. Once a few drops of aqueous are removed from the anterior chamber, remove the 30g-needle and apply pressure to the needle track using a sterile cotton tip applicator. Apply Betadine again after the procedure and check for a Seidel sign. If present, apply additional pressure to the needle track until the wound is sealed. A bandage contact lens may also help seal the cornea.
Iridotomy
Topical antibiotics should be started for at least three days following paracentesis. If paracentesis cannot be performed and the IOP is still at sight-threatening levels, send the patient to the emergency room for intravenous 20% mannitol 1g/kg.
Once the IOP is less than 40mm Hg, topical pilocarpine 2% can be given and a laser peripheral iridotomy should be performed as soon as possible. Giving pilocarpine when the IOP is above 40mm Hg is usually not effective as the iris sphincter is ischemic and topical pilocarpine may also exacerbate the angle closure attack by rotating the iris-lens diaphragm anteriorly.
Laser peripheral iridotomy is performed with a Nd:YAG laser (neodymium-doped yttrium aluminium garnet). The eye is numbed with topical proparacaine and an iridotomy lens is placed on the eye. The laser is set to a 0µm offset with a starting power of 3mJ to 5mJ and a single shot burst. Ideally, a crypt at 11 o’clock or 1 o’clock, hidden under the upper lid, is found and the iridotomy is placed at that location, avoiding iris blood vessels. Care should be taken to find a location with adequate space between the corneal endothelium and the iris to avoid potential damage to the cornea. The patient will feel a small snap, hear a click and see a flash of light. The laser should be applied until a patent iridotomy is made in the iris and a plume of fluid is seen rushing from the posterior chamber to the anterior chamber. This plume indicates that the pressure between the posterior and anterior chamber has equalized and the iris should fall flat. If iris debris or blood blocks the iridotomy site and no laser response is seen, it is best to pause and have the patient wait for 10 to 15 minutes, until the debris settles and additional laser shots can be applied to create a patent iridotomy. The iridotomy should be approximately 1mm x 1mm in size. Following the procedure, the patient is given a topical alpha-2 agonist and advised to continue all topical and oral IOP medication. Additionally a topical steroid QID for one week is started following the procedure to control inflammation. The IOP should be checked in an hour and again 24 hours following the LPI procedure.
Iridoplasty
On follow-up examination, the peripheral iridotomy should be checked to confirm that it is patent and repeat goniopscopy to ensure the angle has deepened. Transillumination of the peripheral iridotomy is not sufficient to confirm its patency. Topical and oral IOP medications are stopped as needed. The fellow eye is also scheduled for a laser peripheral iridotomy as soon as possible as 50% of patients will develop an angle closure attack in the other eye within five years.1 A dilated fundus exam, visual fields and OCT imaging should be performed following the LPI to evaluate the optic nerve for glaucomatous optic neuropathy, Cataract extraction may also be considered at this time.
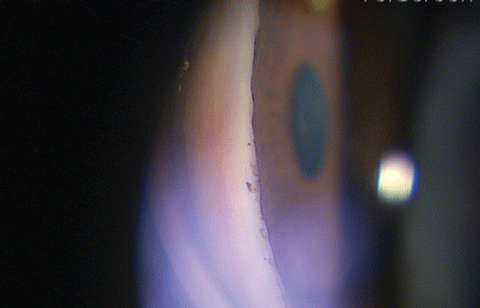 |
| A semi-narrow angle seen from the side. Click image to enlarge. |
If, on follow up, the angle is still narrow on gonioscopy, even in the presence of a patent PI, and the IOP is still elevated, additional angle closure mechanisms may be involved, such as plateau iris syndrome which results when the iris inserts into the ciliary body too far anteriorly, or the ciliary body is rotated anteriorly, putting the angle in appositional closure. This is usually diagnosed only after LPI is performed. Chronic topical miotics may be needed to treat this; however, research shows LPI may reduce IOP in these patients by 32%.4 Laser peripheral iridoplasty physically pulls the angle open and reduces appositional iris closure.4
To perform the laser peripheral iridoplasty, an argon laser or frequency-doubled Q-switched Nd:YAG laser is used. The patient is given topical pilocarpine 2% to constrict the iris and numbed with topical proparacaine. An iridotomy lens is then placed on the eye and the laser is set to 300mW with a 0.5 second duration. A 400µm spot size is used to contract the iris and the laser spots should be placed as far peripheral on the iris as possible, with six laser spots every 90 degrees. The lasers power can be titrated until iris constriction occurs and the angle opens. Care should be taken to avoid large iris blood vessels. Following the procedure, a topical alpha-2 agonist is given and the IOP checked in one hour. Additionally, a topical steroid should be started four times a day for one week.
Prognosis for acute angle closure is good as long as it is treated promptly and appropriately. Following an acute angle closure attack, 62% of patients do not have residual visual field loss; however, if treatment is delayed and the IOP is elevated for a prolonged period of time, vision loss can develop.5
Dr. McWherter is a consultative optometrist with Bennett & Bloom Eye Centers in Louisville, KY.
|
1 . See J, Aquino M, Chew P. Angle-closure glaucoma. In: Yanoff MD M, Duker MD JS, eds. Ophthalmology. 4th ed: 1160-1165. Elsevier, Inc.; 2014 2. Quigley HA. Angle-closure glaucoma-simpler answers to complex mechanisms: LXVI Edward Jackson Memorial Lecture. Am J Ophthalmol. 2009 Nov;148(5):657-669.e1. 3. Kaiser, Peter K. The Massachusetts Eye and Ear Infirmary Illustrated Manual of Ophthalmology. 4th ed: 233-235. Philadelphia:Saunders, 2014.. 4. Ramakrishnan R, Mitra A, Abdul Kader M, Das S. To study the efficacy of laser peripheral iridoplasty in the treatment of eyes with primary angle closure and plateau iris syndrome, unresponsive to laser peripheral iridotomy, using anterior segment OCT as a tool. J Glaucoma. 2016 May;25(5):440-6. 5.Aung T, Looi AL, Chew PT. The visual field following acute primary angle closure. Acta Ophthalmol Scand. 2001 Jun;79(3):298-300. |

