Provocative comparisons among glaucoma medications drew much attention at ARVO 2012. Visitors to this milestone forum designed to encourage and assist research, training, publication and dissemination of knowledge in vision and ophthalmology also benefited from an updated look at exercise and prevention.
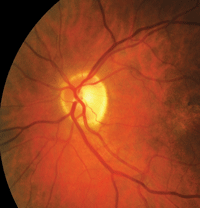
Researchers at this year’s meeting investigated whether generic glaucoma medications are truly a suitable substitute for their brand name counterparts.
Researchers tackled structure and function from several vantage points, including diagnostic technologies and nerve perfusion. In addition, fresh perspectives were presented on monitoring and disease process, as well as overall diagnostics.
New Insights on Topical Therapy
With the increased use of generic glaucoma drops, one study helped explain the inconsistencies in these agents that we see clinically. Researchers in New Delhi compared the physical properties of three commercially available generic brands of latanoprost with Xalatan (Pfizer).5096/A237 The aim of the study was to compare the eye drop volume dispensed, total number of drops dispensed per vial and physical properties (pH, density and relative viscosity) of 2.5ml vials of the medications. On the basis of pH estimation and relative viscosity, the researchers estimated absolute drug concentration per drop.
Significant differences were found among the drop size, number of drops per bottle and physical properties of the generic brands compared to Xalatan. The researchers said the study underscored the unmet need for better quality control in the production of generic prostaglandin analogues. The findings also raised implications for the IOP lowering efficacy, adverse effect profile and cost of glaucoma therapy associated with generics.
In Thessaloniki, Greece, and Brescia, Italy, the 24-hour efficacy of preservative-free tafluprost (Zioptan, Merck) and preservative-containing latanoprost (Xalatan) were compared in patients with primary open-angle glaucoma (POAG) or ocular hypertension (OHT).5104/A245 The 24-hour IOP control was obtained when both agents were administered as first-choice therapy. The study, a prospective, observer-masked, crossover comparison, included consecutive, newly-diagnosed patients with POAG or OHT who had baseline IOP between 24mm Hg and 33mm Hg. Thirty-eight patients were randomized to either latanoprost or tafluprost administered in the evening for three months. Patients were then switched to the opposite therapy for another three months.
Tafluprost, when employed as first-choice therapy, achieved statistically similar 24-hour IOP reduction when compared to latanoprost. The study highlighted the importance of complete assessment of efficacy over 24 hours.
Researchers in Milan and Rome evaluated the effects of bimatoprost 0.1% (Lumigan, Allergan) and timolol 0.5% on circadian IOP and blood pressure based on an interim analysis of 20 patients.5105/A246
Both treatments were associated with statistically significant reductions in IOP compared to baseline (-3.8mm Hg, with timolol 0.5%; -4.8mm Hg, with bimatoprost 0.1%). IOP was also statistically significantly lower after treatment with bimatoprost 0.1%. Bimatoprost 0.1% once at night was found to be more effective than timolol 0.5% twice daily in reducing the IOP at all time points of the 24-hour curve. Night-time IOP under timolol 0.5% seemed not to be different than IOP after washout. Heart rate and blood pressure were significantly reduced by timolol 0.5%.
Studying Adherence and Ocular Surface Health
Investigators from the University of Colorado and Aristotle University of Thessaloniki, Greece used electronic monitoring to assess patients’ adherence to glaucoma therapy regimens and ocular surface health. They compared the effects of latanoprost/timolol fixed vs. latanoprost/timolol unfixed therapy in glaucoma.5097/A238
The prospective six-month, parallel, observational study involved 142 consecutive well-controlled patients with open-angle glaucoma (OAG) or OHT who received either unfixed therapy (latanoprost) once in the evening and timolol twice daily or latanoprost/timolol fixed combination (Xalacom, Pfizer) therapy once in the evening.
Patients in the unfixed group demonstrated worse vertical cup-to-disc ratio (0.65 vs. 0.58) and worse mean visual field defect (5,9 dB vs. 3,8 dB) at baseline. The unfixed group also demonstrated higher mean IOP at six months (16.6mm Hg vs. 15.0mm Hg).
The adherence rate was significantly better in the fixed combination group at three months (75.6% vs. 61.2%) and six months (73.0% vs. 57.3%) of follow up. Signs of ocular surface disease were significantly worse in the unfixed group at baseline. The trial demonstrated a significantly superior rate of adherence and ocular surface health in the fixed combination treatment group, verifying superior benefits for the first time in a trial. Hopefully, this fixed combination will soon be available to us here in the United States.
Exercise and Prevention
Can aerobic exercise be a prescription for prevention of glaucoma? Canadian researchers sought an answer to this long-debated question in a meta-analysis to compare the effect of exercise parameters on IOP levels.5070/A211 They analyzed 10 studies, focusing on sedentary or normally-active participants with normal baseline IOP (10mm Hg to 21mm Hg) who had completed a single bout of mild aerobic exercise (producing a 40% heart rate) to moderate aerobic exercise (50% to 70% heart rate) ranging from two to 60 minutes in duration.
Their findings? IOP reduction from exercise was within the range that is most useful to those at risk of POAG. Prescription of even a mild daily aerobic exercise regime could be an effective method to keep slightly elevated IOP levels within a normal range.

Can aerobic exercise protect against glaucoma?
Considering Structure and Function
Seeking to identify the best functional and structural indicators of glaucoma progression, investigators at the University of Pittsburgh and the New England Eye Center evaluated the visual field (VF) and optic nerve head (ONH) parameters of 110 eyes of 60 subjects (including 24 healthy, 48 glaucoma suspects and 38 glaucomatous eyes). The patients had undergone comprehensive ocular examination and four or more visits involving VF testing (Carl Zeiss Meditec), spectral-domain optical coherence tomography (SD-OCT) (RTVue-100, Optovue) and scanning laser ophthalmoscopy (SLO) (HRT III, Heidelberg Engineering).219/A460
For VF, the Visual Field Index (VFI) showed statistically significantly better correlation with the common latent progression than both mean deviation and pattern standard deviation. For SD-OCT, the parameters with the highest correlation with latent progression were cup area and rim area and statistically significantly better than other measured parameters. SLO also showed cup area and rim area to be the parameters most correlated with latent progression.
Cup and rim area were found to be the most useful structural measurements of progression, while VFI was the most useful functional parameter. Even though SD-OCT and HRT quantified ONH structure, there was a poor correlation between the devices in detecting progression.
Blood Flow and Glaucoma
Changes in retrobulbar blood flow may correlate to changes in the optic disc in patients with glaucoma, according to clinicians who coordinated a research effort in Indiana and Kaunas, Lithuania.247/A488 Ninety-eight patients with OAG were examined at baseline and after two years of follow-up for retrobulbar blood flow and optic nerve structure, as measured by color Doppler imaging and OCT, respectively.
Decreased perfusion in the retina and optic nerve were associated with increased optic cup area in this cohort of patients. Decreasing retinal blood flow may increase optic nerve damage, as defined by optic cup area, in patients with OAG, a researcher noted. We are still waiting for a reliable, affordable device for the private office.
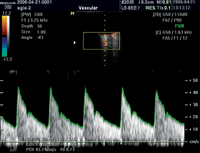
Doppler imaging was used to determine whether changes in blood flow correlate with changes in the optic disc.
In the state of New York, the efficacy of the Amsler grid was evaluated for detecting glaucomatous central visual field defects.177/A418 Ninety-six eyes of glaucoma patients who had either a normal or abnormal 10-2 VF finding for both eyes within the previous four months were included in the study. The results of the Amsler grid tests were found to approximate the 10-2 VF results. Therefore, the Amsler grid was determined to be a possible useful supplement to 10-2 VF testing for evaluating and monitoring central VF loss in glaucoma.
Monitoring and Understanding Disease Process
The utility of a new diagnostic indicator, age-adjusted concurrent pressure to cornea index (CPCI), was tested as a means for discriminating between glaucoma and non-glaucoma.4176 Researchers in Singapore, China, and Australia defined CPCI as the age-adjusted ratio between untreated intraocular pressure and central corneal thickness (CCT) in mm, measured within two hours of each other. In a population-based, cross-sectional study, the distribution of CPCI in 294 normal controls with normal visual fields, 124 with normal-tension glaucoma, 11 with OHT with normal visual fields, and 14 with POAG was determined.
The CPCI was determined to have better discriminatory ability for glaucoma than IOP and CCT alone. CPCI may be a useful summary indicator of glaucoma risk. Longitudinal studies are needed to prove its prognostic value.
Assessing Nerve Rim
Rim assessment lacks a solid anatomical basis. Clinical disc margin does not provide a reliable outer border of rim tissue because of clinically and photographically invisible extensions of Bruch’s membrane (BM) inside the disc margin.1745 As a result, rim tissue orientation in ONH also cannot be determined.
To address this issue, investigators in Halifax, Nova Scotia, Canada and Portland, Ore., introduced a BM opening-minimum rim width (BMO-MRW) measurement that quantified the rim from its true anatomical outer border and accounted for its variable trajectory in the measurement plane. Glaucoma patients (n = 107) and normal controls (n = 48) underwent Spectralis SD-OCT (Heidelberg Engineering) imaging (24 B-scans centered on the optic nerve head).
Greater than three-fold higher sensitivity at 95% specificity in early glaucoma of BMO-MRW was found, compared to results found with current methods. This was clinically significant, indicating the possiblity of a new structural marker for the detection and risk-profiling of glaucoma.
Estimating Morning IOP Peak
An alternative way of estimating morning IOP peak in glaucoma patients––the water-drinking test–– was the focus of a cross-sectional study in Porto Alegre, Brazil.5050/A191 Forty-five adult glaucoma patients (90 eyes) had their IOP checked by hand-held applanation tonometry between 6 a.m. and 7 a.m. at home, immediately after awaking and while still lying in bed. Patients were advised to fast for one hour and to arrive at the clinic 15 minutes before additional IOP testing, avoiding activities that could lead to accommodation.
They then drank 500ml of room-temperature water in five minutes and had their IOP measured in the sitting position. Afterward, they laid down under dim light for 15 minutes in a quiet place before IOP was measured again. Reproducible results showed that IOP verified at wake-up time in bed had excellent agreement with IOP in the clinic under these conditions, raising the possibility of an easy, fast and reliable method of appraising morning IOP peak in glaucoma patients.
Exploring Diagnostic Technologies
Researchers from the Wilmer Eye Institute in Baltimore, Md., assessed the ability of pupillography to discriminate glaucoma patients from persons without glaucoma.5621 Three approaches were evaluated:
1. Detecting a relative afferent pupillary defect (RAPD) between the two eyes.
2. Comparing pupil responses to stimuli aimed at different parts of the retina within the same eye.
3. Comparing overall pupillary responses of eyes with glaucoma to responses of normal eyes.
The RAPiD (Konan Medical), a binocular pupillographic device, recorded latency and amplitude of pupil responses. Thirty controls and 104 glaucoma patients from a single clinic were enrolled. Patients with glaucoma had a significantly larger RAPiD result compared to controls. Researchers identified five parameters, suggesting that a prototype pupillography device may be able to discriminate glaucoma from normal eyes with relatively high specificity and sensitivity. This device may prove ideal for screening.
In an observational cohort study that looked at 134 eyes from 88 patients, researchers in La Jolla, Calif., compared the diagnostic accuracy of the Spectralis and the HRT for detection of glaucoma in patients suspected of having glaucoma.5620 Patients were recruited from the Diagnostic Innovations in Glaucoma Study (DIGS). Forty-eight eyes with progressive glaucomatous optic nerve change and 86 eyes without any evidence of progressive damage to the optic nerve were included.
All eyes underwent retinal nerve fiber layer imaging with the Spectralis and topographic imaging with HRT within six months. The researchers concluded that RNFL assessment with the Spectralis performed better than optic disc topographic parameters obtained by the HRT when diagnosing glaucoma in glaucoma suspects.
Finally, researchers in St. Louis, MO, determined that IOP and perimetric mean deviation were higher in winter than during summer, although there was no evidence of a causative relation.1751 The findings could shed light on the disease process, as well as help reduce clinical test-retest variability.
IOP measurements and visual fields were evaluated from 33,873 visits over 12.5 years (median) by 1,636 participants in the Ocular Hypertension Treatment Study (OHTS). The 22 clinics participating in the OHTS were classified into six regions with similar climates (Atlantic, Central, North, Pacific Northwest, Southeast, and West), based on the magnitude and timing of seasonal variations in precipitation, temperature and sunlight hours.

