 |
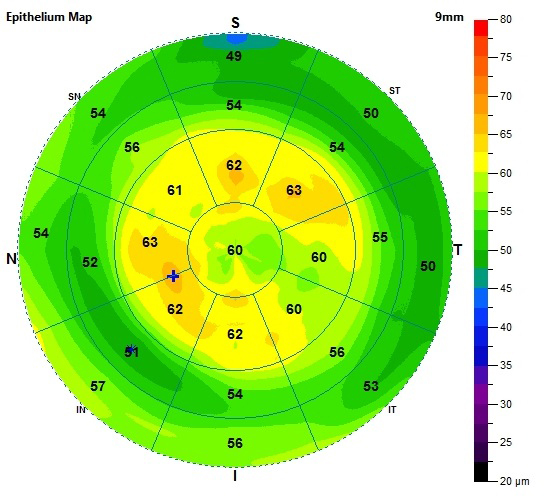
If a patient’s eye has both superior corneal epithelial thickness <45µm and Schirmer’s test result <10mm, they are five-times more likely to have antibody-positive bloodwork and associated visual compromise. Photo: Justin Cole, OD, and Jarett Mazzarella, OD. Click image to enlarge. |
Previous studies have shown that patients with dry eye disease (DED) display thinner superior corneal epithelium compared with normal controls. Researchers at the University of Illinois Chicago recently tested their hypothesis that presence of autoantibodies has been associated with superior epithelial thinning. They also assessed the link between corneal epithelial thickness and clinical findings and assessed the utility of including corneal epithelial thickness as a diagnostic tool for patients with DED. Their results will be presented this morning at ARVO 2023 in New Orleans.
This study included 208 patients who visited the DED clinic at University of Illinois Chicago and had blood work results in their medical records for autoantibodies associated with DED-related autoimmune diseases. If available, superior corneal epithelial thickness, Schirmer’s 1 test and corneal higher order aberrations (HOAs) were obtained from the patient's medical records. Superior corneal epithelial thickness was determined with the RTVue XR OCT Avanti (Visionix) system, and corneal HOAs were determined using the iTrace (Tracey Technologies) system. A decision tree was used to determine feature variables and cutoffs necessary to accurately classify antibody positive and negative groups.
The researchers found that patients with antibody-positive blood work had a significantly thinner superior corneal epithelial thickness (47.41µm vs 49.73µm) compared with patients with antibody negative blood work (n=181 eyes).
The top two most useful clinical indicators that a patient will have antibody-positive blood work are a Schirmer’s <15mm and an epithelial thickness <45µm. Eyes with epithelial thickness <45µm and Schirmer’s <10mm (n=69 eyes) have significantly greater corneal HOAs (1.85 vs. 0.1) compared with eyes with thickness ≥45µm and/or Schirmer’s ≥10mm (n=164 eyes). If a patient’s eye had both superior corneal epithelial thickness <45µm and Schirmer’s test results <10mm, the probability that they have autoantibody-positive bloodwork was 81.2%.
“Presence of autoimmune disease must be considered in patients who have superior epithelial thinning and reduced tear production because these patients are five-times more likely to have antibody-positive bloodwork and associated visual compromise, as demonstrated by high corneal HOAs,” the researchers concluded in their abstract.
Original abstract content © Association for Research in Vision and Ophthalmology 2023.
Bernal A, Yang Y, Surenkhuu B, et al. Corneal epithelial thickness in dry eye disease (DED) patients: association with autoimmunity. ARVO 2023 annual meeting. |

