For years, you’ve been deluged with information and factoids about “creating a dry eye practice.” Likely, you listened and have started to manage, or are better managing, your dry eye patients.
The increase in quality education surrounding dry eye is one of the best outcomes of recent industry R&D and marketing outreach. In reviewing the program schedule of education offerings at recent and upcoming optometry meetings, the emphasis on ocular surface disease is very apparent.
And more recently, you may have noticed the “dry eye pendulum” has begun to move, with a movement away from education specific to dry eye management alone and more towards the management of “the ocular surface” including the assessment and treatment of lid disease.
Blepharitis vs. Dry Eye
First, let’s consider traditional definitions. Blepharitis is an inflammatory condition of the eyelid and is considered a common eye disorder that is usually associated with bacterial or skin conditions (such as dandruff on the scalp, or acne rosacea). Although it can be an annoyance for patients, the disease rarely causes any permanent visual impairment.1
What confounds the diagnosis and treatment is the likelihood of a patient presenting with other ocular surface issues. Clinicians typically concentrate treatment strategies on the patient’s ocular surface issues rather than the eyelids.2-4
Common symptoms of blepharitis include irritation, redness, itching, edema, tearing, foreign body sensation, crusting, photophobia and fatigue.5 Clinical findings (collarettes, eyelid margin hyperemia, etc.) are relegated to the eyelid, but can involve the skin around the lid margin as well. Long-term, unmanaged blepharitis can lead to conjunctivitis, lid margin changes, keratitis, or more severe findings, such as corneal neovascularization and cicatricial lid changes.
Blepharitis is traditionally defined by its geographic location on the eyelid. Anterior blepharitis is found on the outer edges of the lids and is typically associated with gram-positive bacteria (Staphylococcus aureus, S. epidermidis and Corynebacterium spp.).
Anterior blepharitis is commonly treated with antibiotic ointments (including bacitracin and erythromycin) and/or antibiotic steroid drops (e.g. tobramycin/dexamethazone), or ointments, lid hygiene and warm compresses, and/or commercial lid scrubs.1 Posterior blepharitis—sometimes referred to as meibomian gland dysfunction (MGD)—occurs at the inner edges of the eyelids and involves the meibomian glands.6
There is significant debate whether expression of the meibomian glands (expressibility and quality of the secretions) can be graded and monitored over time or with treatment. In many cases, the entire lid margin can be involved, often called mixed blepharitis (figure 1).
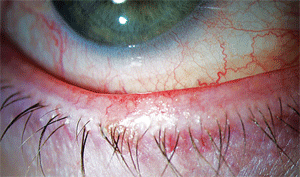
1. Posterior lid margin redness, or
redness posterior to grey line, is often seen in patients with MGD.
Also note the crusting on the anterior lashes—an indication this may be
a “mixed” case of blepharitis.
Blepharitis is fairly common, but we know very little about its prevalence. This isn’t surprising—as clinicians, we look at the lids in every routine examination and likely have a broad tolerance of how “clear” lids/lashes should appear. Most of the available prevalence data has been extrapolated from relatively small clinical samples rather than population-based studies. Notable exceptions include a recent cold-call telephone survey of 5,000 adult Americans and several samples of clinical patients. In the latter, one study found that the prevalence of MGD was associated with an increased age; another study found it to be the most common diagnosis in a large sample of patients complaining about ocular discomfort and irritation (dry eye disease followed closely behind).7-9 MGD has also been linked to rosacea.7
MGD symptoms may result from the release of the inflammatory mediators and products of lipolysis into the tears, or the effect of qualitative and quantitative tear film lipid deficiencies on water loss from the ocular surface.4 Studies have shown that in cases of chronic blepharitis (including both anterior and posterior), symptoms may occur due to MGD and its associated lipid anomalies, or by way of a direct effect of bacterial toxins in the aqueous layer and on the ocular surface and eyelid skin margin.10-12
Key Symptoms
The exact mechanisms that cause symptoms are still unclear, but ocular burning/stinging, red, puffy lids, and morning symptoms are more commonly associated with blepharitis––both anterior and posterior. There is a significant overlap with “dry eye” symptoms, which is likely due to the high frequency of meibomian gland involvement in evaporative dry eye.
Consider “triaging” your symptom questions: First, ask when symptoms are worse, morning or evening. If the answer is morning, look carefully at the lids for lid disease including blepharitis. Don’t forget to rule out lagophthalmos.
If the patient responds that evening symptoms are worse, consider dry eye and possibly aqueous deficiency—but be wary, there is overlap. The most frequently reported symptom in dry eye is dryness/irritation.13 Not surprisingly, the same symptom is most frequent in blepharitis.7
Ocular Surface and Lid Health
The goal of treatment in MGD is to improve the patency of the meibomian glands and to restore them to a normal functional status. Traditionally, clinicians have accomplished this with warm compresses and lid massage, antibiotic ointments and oral tetracyclines. Chronic blepharitis (anterior or posterior) may be exacerbated by environmental irritants and can have periods of remission coupled with a high rate of recurrence.14
Although there have not been studies of long-term progression of blepharitis, it is clinically accepted that, in untreated disease, symptoms and lid findings become increasingly worse, leading to hyperemic, edematous, notched or ulcerated eyelids, chronic cicatricial changes to the lids, and possibly recurring chalazia. Eventually, the recurrent inflammation destroys the meibomian gland architecture. This can be demonstrated using infrared meibography (figures 2 and 3). There remains no cure for blepharitis in most cases, and there is insufficient evidence to scientifically proclaim a gold standard of treatment.
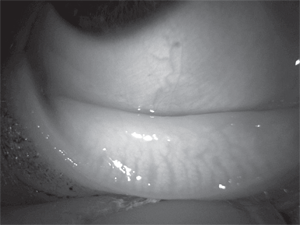
2. Normal meibomian gland structure via infrared meibography.
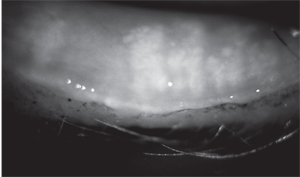
3. Significant meibomian gland structural loss in a patient with moderate to severe meibomian gland dysfunction.
The Dry Eye Link
Every time I lecture on dry eye or MGD, I ask the audience what percentage of all dry eye patients they see is evaporative vs. aqueous deficient. The response is almost always the same—most believe that up to 80% of the dry eye patients seen in optometric practice are evaporative. Evaporative dry eye may occur due to changes in the lipid layer and/or the aqueous mucin gel, where meibomian glands play an important role. An often overlooked component of evaporative dry eye is related to the intrinsic factors of the lid/ blink system, including incomplete blinking related to age or possibly to the use of computers.15
As we age, normal meibomian gland secretions likely change or decrease. In healthy eyes, this occurs without any increased viscosity or opacity of the expressed liquid. The secretory decline may be a marker for gland dysfunction. The challenge for researchers will be to determine what level is “normal” at a given age.
Further, the meibomian gland is regulated in part by androgen, a hormone found in both men and women that decreases with age, and has been associated with an increased risk of dry eye.16 Androgens may suppress inflammatory changes in the meibomian glands as well. In women with complete androgen insensitivity syndrome, androgen receptor dysfunction is associated with meibomian gland changes and a significant increase in the signs and symptoms of dry eye.17
The meibomian glands may also have estrogen receptors and are therefore subject to hormonal changes. This may explain the increased prevalence of dry eye in women, especially after menopause. Hormone replacement therapy has been suggested as a risk factor for dry eye, which may be evaporative dry eye related to local meibomian gland hormonal regulation.18
While research has yet to demonstrate whether hormone modification, either orally or topically would be beneficial for postmenopausal women, it can be expected that future dry eye management could include therapies involving hormones. As mentioned previously, patient symptoms and complaints about blepharitis are often consistent with a diagnosis of dry eye disease, and many hypothesize that the majority of dry eye patients have underlying meibomian gland dysfunction.19 Because blepharitis overlaps with the signs and symptoms of evaporative dry eye, it is often underdiagnosed and misdiagnosed.14
A recent survey suggested that optometrists see blepharitis in clinical practice in 47% of their patients (ophthalmologists responding to the same survey reported 37% of their patients have blepharitis).7 This is consistent with a study performed in which 38.9% of randomly-selected, apparently normal patients presenting for routine vision examinations had absent or cloudy meibomian gland secretion upon expression.8
In my opinion, the remarkable congruence of these prevalence values in studies close to 20 years apart indicates the need for close inspection of the lids and meibomian gland expression in patients with dry eye symptoms.
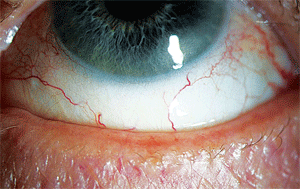
Dry eye disease alone affects approximately three million women and two million men over the age of 50 in the U.S. Depending on which study is cited, dry eye affects anywhere from 14% to 33% of the worldwide population.13,20 In order to derive these prevalence values, surveys were validated against a clinical examination. Unfortunately, at the time this occurred, traditional dry eye “tests” (including assessment of symptoms, tear film break-up time, Schirmer tear wetting, and fluorescein corneal staining) were used. Careful assessment of the lid rarely was included, so it is possible some of these “dry eye patients” are patients with blepharitis (figure 4).
|
| 4. This 65-year-old woman presented with frequent dryness and irritation, and she reported a previous “dry eye diagnosis” by another doctor. Does she have MGD or evaporative dry eye? |
The two diseases are notoriously intertwined. Hyperkeratinization of the lid margin and meibomian gland orifices may cause changes to the tear film, initiate inflammation, and decrease proper lacrimal gland function, which can lead to more serious dry eye symptoms.6 The overlap in symptoms underscores the need for optometrists to be able to better identify and treat these two diseases as early in their development as possible in order to provide the best outcomes for patients. The need for multiple treatment approaches is also warranted, and treating one condition may improve the outcomes of the other. For example, patients with mild cases of aqueous deficiency noted an improvement in their symptoms when concurrent cases of MGD were controlled.21
MGD, Dry Eye and CLs
Up to half of all contact lens wearers report dry eye symptoms, and chronic blepharitis is another cause for contact lens intolerance.3,22,23 Contact lens wearers are substantially more likely to have dry eye than people who wear spectacles or those who do not need refractive correction. The reasons behind this are fairly well established, including the ability of contact lenses to destablize the tear film and increase evaporative loss as well as incomplete blinking, exposure keratopathy, lid wiper epitheliopathy, and refractive surgery.24
A preliminary study that looked at the incidence of MGD in established daily contact lens wearers found that 30% demonstrated some degree of MGD after six months (compared to 20% of non-lens wearers); gender was not a significant factor, with 33% of male and 28% of female lens wearers affected.25
A newer study has also shown contact lens wear adversely affects meibomian gland structure and may be proportional to the duration of wear.22
Anecdotally, meibomian gland dropout and secretion viscosity change is notably higher in contact lens wearers as well.
Practice Prevention and Limit Progression
I’m often asked about treatment of the “asymptomatic patient.” Let’s say, for example, that a patient comes in for a routine eye examination and, when questioned, has minimal to no complaints of dryness. On slit lamp exam, you note debris on the lid margin, mild redness and telangiectasia of lid margin vessels, and grade 2 conjunctival redness (figure 5). In fact, this patient looks similar to most patients her age.

5. The clinical appearance of the ocular surface and lid. Note that the meibography image in figure 3 is of the same eye.
Let me point out one critical difference—the gland loss pictured in figure 3 via meibography is taken of the same eye pictured in figure 5. This patient has instantaneous tear break-up, inferior corneal staining, and rarely drives or reads at night due to eye irritation and fluctuating vision. Essentially, you are unable to express lipid, and the patient likely has minimal to no lipid on her tear film. When further questioned, the patient says this has been ongoing for years, and she has become “used to it.”
Would earlier diagnosis and management have prevented gland drop-out? We don’t know for sure, but I’m willing to take a proactive treatment approach rather than wait to find out.
There are several clinically accepted treatment routines that can address dry eye and blepharitis disease states, including palliative treatments, such as preserved and non-preserved artificial tears, or tear supplements that contain oil. Systemic tetracyclines (oral doxycycline and minocycline) have been traditionally used to reduce lid inflammation, especially in the presence of acne rosacea. Lid scrubs may also indirectly improve lid inflammation by removing potentially irritating lid debris. While mechanisms of action are unclear, essential fatty acid supplementation is very common in dry eye disease, and recent research has demonstrated dietary consumption or omega-3 supplementation may improve signs and symptoms of evaporative dry eye.26
The key to avoiding recurrent flare-ups of anterior blepharitis: Advise patients to keep their lids clean and free of crusts, which is easier said than done.27 Because the aqueous tear deficiency component of dry eye is often found in patients with blepharitis, artificial tears and cyclosporine A (Restasis, Allergan) may be successful adjuncts to lid hygiene and medication.14,28
|
Ask the Right Questions Marguerite McDonald, M.D., recently described her 15-second symptom assessment for blepharitis to me. (Her informative interviews on blepharitis can be seen at www.icareinamerica.com.) After a patient expresses displeasure with his/her vision, ocular comfort or both, ask the following questions: 1. “What time of day do your eyes look and feel their worst?” If morning, think blepharitis. 2. “Next, would you ever say that your eyes burn—would you use that word?” Burning is found almost exclusively in blepharitis patients, caused by the free fatty acids and soaps released after bacterial lipases break down the meibomian gland secretions. Just the Right Expression To perform meibomian gland expression, follow these steps: 1. Device: clean index finger or Q-tip (horizontal placement).
|
Treatment Strategies
A primary goal of blepharitis and dry eye treatment is to prevent progression to irreversible lid and ocular surface damage. At present, there is no definitive, FDA-approved treatment therapy for either anterior or posterior blepharitis, and only one FDA-approved drug (i.e., Restasis) for dry eye thought to be related to inflammation associated with keratoconjunctivitis sicca.29 Thus, many palliative, over-the-counter, or off-indication approaches are utilized.
The likely first course of treatment for the most common presentation of evaporative dry eye/MGD may be lubrication, lid hygiene and warm compresses, and often omega-3 fatty acid supplementation (2g/day), as was done for the patient described above.
Patients who do not benefit from lubrication and lid hygiene may start therapy with topical antibiotic ointments or oral tetracyclines; however, a slow onset of effect and known side effects may limit usefulness in true chronic cases.14,30
Classic therapy regimens are often discontinued by the patient who are non-compliant with compresses/lid therapy, or who have gastrointestinal side effects from tetracycline use. For these patients, low dose 20mg doxycycline may reduce side effects.
A need remains for better treatments that can address both the blepharitis component and its dry eye counterpart. Topical cyclosporine 0.05% has anti-inflammatory properties that have made it well-suited for the treatment of dry eye and MGD, but symptomatic relief is not necessarily a given in cases of MGD.31
Artificial tears, gels and ointments, and 2% topical metronidazole address some of the goals of a treatment regimen, but not all.29 Likewise, as discussed above, essential fatty acids have been shown to provide some relief, but are not consistently efficacious, nor is their method of action fully understood.
Several studies are under way or have recently completed that evaluate the efficacy of topical azithromycin 1% ophthalmic solution (AzaSite, Inspire Pharmaceuticals) in the treatment of blepharitis. Azithromycin has unique pharmacokinetic properties that allow for high bioavailability in ocular tissue, as well as anti-inflammatory properties independent of its anti-infective activity.32,33 In its ophthalmic delivery vehicle and once-daily dosing, the drug has recently been shown to improve lipid properties of meibomian gland secretions in patients non-responsive to warm compress therapy.34,35 While several studies are underway, longer-term studies of these therapeutic approaches are needed in order to better guide clinical care with this chronic condition.
For my patient, lubrication, omega-3 supplementation, lid hygiene, and ultimately topical azithromycin q.d. have been used in her management plan. At her upcoming visit we will assess her ocular status to determine whether cyclosporine drops should be re-initiated (she reported a previous trial from the doctor originally diagnosing dry eye). In their mildest forms, both dry eye and blepharitis are treatable, although not curable. Left untreated, however, the two diseases may progress. Clinicians should continue to evaluate patients with a renewed goal of reducing the signs and symptoms of both diseases. Ideally, this would include a careful lid evaluation, including meibomian gland expression (see ”Just the Right Expression,” above), as well as an effective, affordable treatment regimen with which patients will remain compliant and without negative side effects.
Dr. Nichols is an associate professor at the Ohio State University College of Optometry, in Columbus, Ohio. She lectures and writes on ocular surface disease, and currently chairs the International Meibomian Gland Workshop sponsored by the Tear Film and Ocular Surface Society. She is a paid consultant to Allergan, Alcon, Inspire, Occulogix (TearLab) and Pfizer, and has NIH funding to study dry eye in postmenopausal women.
1. AOA. Blepharitis. Available at: www.AOA.org/Blepharitis.xml (Accessed March 17, 2010).
2. Jackson WB. Blepharitis: current strategies for diagnosis and management. Can J Ophthalmol. 2008;43:170-79.
3. AOA. Optometric Clinical Practice Guideline: Care of the patient with ocular surface disorders. Available at: www.aoa.org/documents/CPG-10.pdf (Accessed June 19, 2009).
4. Foulks GN, Bron AJ. Meibomian gland dysfunction: a clinical scheme for description,diagnosis, classification, and grading. Ocul Surf. 2003;1:107-26.
5. John T, Shah AA. Use of azithromycin ophthalmic solution in the treatment of chronic mixed anterior blepharitis. Ann Ophthalmol. 2008;40:68-74.
6. Mathers WD. Meibomian gland disease. In: Pflugfelder SC, Beuerman RW, Stern ME. Dry eye and ocular surface disorders. Marcel Dekker Inc. 2004; New York, NY: 253, 260.
7. Lemp MA, Nichols KK. Blepharitis in the United States 2009: a survey-based perspective on prevalence and treatment. Ocul Surf. 2009;7(suppl 2):S1-S14).
8. Hom MM, Martinson JR, Knapp LL , Paugh JR. Prevalence of meibomian gland dysfunction. Optom Vis Sci. 1990 Sep;67(9):710-2.
9. Venturino G, Bricola G, Bagnis A, Traverso CE . Chronic Blepharitis; Treatment Patterns and Prevalence. Invest Ophthalmol Vis Sci. 2003;44: E-Abstract 774.
10. McCulley JP, Shine WE. Eyelid disorders: the meibomian gland, blepharitis, and contact lenses. Eye Contact Lens. 2003;29(suppl 1):S93-S95; discussion S115-18, S192-94.
11. McCulley JP, Shine WE. The lipid layer of tears: dependent on meibomian gland function. Exp Eye Res. 2004;3:361-65.
12. Raskin EM, Speaker MG, Laibson PR. Blepharitis. Infect Dis Clin North Am. 1992;6:777-87.
13. The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007 Apr;5(2):93-107.
14. American Academy of Ophthalmology, Cornea/External Disease Panel. Blepharitis Preferred Practice Pattern Guidelines. Available at: www.aao.org/ppp (Accessed June 19, 2010.)
15. Wensi S, Baker R, et al. Age-related changes in human blinks: passive and active changes in eyelid kinematics. Invest Ophthalmol Vis Sci. 1997 Jan;38(1)92-9.
16. Schaumberg DA, Dana R, Buring JE, Sullivan DA. Prevalence of dry eye disease among US men: Estimates from the Physicians’ Health Studies. Arch Ophthalmol. 2009;127(6):763-68.
17. Sullivan DA, Sullivan BD, Evans JE, et al. Androgen deficiency, meibomian gland dysfunction, and evaporative dry eye. Ann NY Acad Sci. 2002 Jun;966:211-22.
18. Schaumberg DA, Buring JE, Sullivan DA, Dana MR. Hormone replacement therapy and dry eye syndrome. JAMA. 2001 Nov 7;286(17):2114-9.
19. Driver PJ, Lemp MA. Meibomian gland dysfunction. Surv Ophthalmol.1996;40:343-67.
20. Behrens A, Doyle JJ, Stern L, et al. Dysfunctional tear syndrome: a Delphi approach to treatment recommendations. Cornea. 2006;25:900-7.
21. Foulks GN. The evolving treatment of dry eye. Ophthalmol Clin N Am. 2003;16:29-35.
22. Arita R, Itoh K, Inoue K, et al. Contact lens wear is associated with decrease of meibomian glands. Ophthalmology. 2009;116:379-84.
23. Nichols JJ, Sinnott LT. Tear film, contact lens, and patient-related factors associated with contact lens-related dry eye. Invest Ophthalmol Vis Sci. 2006; 47:1319-28.
24. McMonnies CW. Incomplete blinking: exposure keratopathy, lid wiper epitheliopathy, dry eye, refractive surgery, and dry contact lenses. Cont Lens Anterior Eye. 2007 Mar;30(1):37-51.
25. Ong BL, Larke JR. Meibomian gland dysfunction: some clinical, biochemical and physical observations. Ophthalmic Physiol Opt. 1990;2:144-8.
26. Rosenberg ES, Asbell PA. Essential Fatty acids in the treatment of dry eye. Ocul Surf. 2010 Jan;8(1):18-28.
27. National Eye Institute. Blepharitis. Available at: www.nei.nih.gov/health/blepharitis (Accessed March 17, 2010).
28. Rubin M, Rao SM. Efficacy of topical cyclosporine in the treatment of posterior blepharitis. J Ocul Pharmacol Ther. 2006 Feb; 22:47-53.
29. Jackson WB. Blepharitis: current strategies for diagnosis and management. Can J Ophthalmol. 2008;43(2):170-9.
30. Smith K, Leyden JJ. Safety of doxycycline and minocycline: a systematic review. Clin Ther. 2005; 27:1329-42.
31. Perry HD, Doshi-Carnevale S, Donnenfeld ED, et al. Efficacy of commercially available topical cyclosporine A 0.05% in the treatment of meibomian gland dysfunction. Cornea. 2006;25:171-5.
32. Amar T, Caillaud T, Elena PP. Ocular pharmacokinetic study following single and multiple azithromycin administrations in pigmented rabbits. Curr Eye Res. 2008;33:149-58.
33. Ianaro A, Ialenti A, Maffia P, et al. Anti-inflammatory activity of macrolide antibiotics. J Pharmacol Exp Ther. 2000;292:156-63.
34. Foulks GN, Borchman D, Yappert M, et al. Topical azithromycin therapy for meibomian gland dysfunction: clinical response and lipid alterations. Cornea. 2010 Jul;29(7):781-8.
35. Luchs J. Efficacy of topical azithromycin ophthalmic solution 1% in the treatment of posterior blepharitis. Adv Ther. 2008;25:858-70.

