|
|
A 77-year-old white female with symptoms of increasing floaters in her left eye for the past five months was referred to my office. She also noted a painless, progressive decline in her vision in both eyes during the past year.
She had not been to an eye doctor in more than four years. She denied any history of trauma or past surgeries. Her medical history was unremarkable.
On examination, best-corrected visual acuity was 20/20 O.D. and 20/30 O.S. Confrontation fields were full to careful finger counting O.U. Pupils were equally round and reactive with no afferent pupillary defect. Motility testing was normal. The anterior segment exam was significant for early nuclear sclerosis and cortical cataract in both eyes.
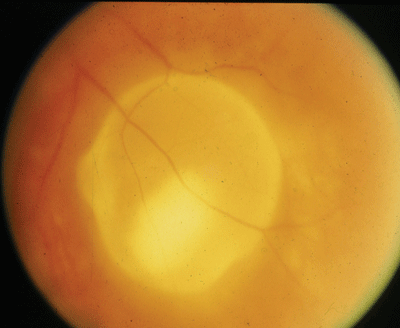 |
|
This patient presented with symptoms of increasing floaters for five months and this unusual lesion in the inferotemporal portion of the left eye. |
Take the Retina Quiz
1. What additional testing would help confirm the diagnosis?
a. Fluorescein angiography.
b. Optical coherence tomography.
c. Electroretinogram.
d. Standardized ultrasound.
2. What does the lesion in the left eye represent?
a. Choroidal neovascular membrane.
b. Subclinical retinal detachment.
c. Macular dystrophy.
d. Invasion from a nematode.
3. What is the correct diagnosis for this patient?
a. Retinal pigment epithelial detachment (RPED).
b. Eccentric disciform lesion secondary to AMD.
c. Adult vitelliform maculopathy-pattern dystrophy.
d. Ocular cysticercosis.
4. What is the most common cause of vision loss in this setting?
a. Subretinal hemorrhage and scarring.
b. Retinal detachment.
c. Cystoid macular edema.
d. Optic neuropathy.
5. What is the cause of the floaters?
a. Posterior vitreous detachment.
b. Vitreous hemorrhage.
c. Vitreous cells.
d. Normal vitreous syneresis.
6. What is the most appropriate management for this patient?
a. Observation.
b. Laser photocoagulation.
c. Vitrectomy and scleral buckle procedure.
d. Surgical removal.
(For answers, see below.)
Discussion
The lesion in our patient represents a localized serous retinal detachment due to invasion of the nematode Cysticercus cellulosae. This results from human ingestion of the eggs of the pork tapeworm (Taenia solium). Cysticercosis is more common in developing countries, with approximately 50 million cases of Taenia solium infestations worldwide.1
The pig becomes infected from ingesting the eggs of the tapeworm. Once in the intestines of the pig, the tapeworm invades the intestinal wall and migrates into the striated muscle, where it forms a cyst.
Humans become infected by ingesting raw or undercooked infected meat. The eggs disintegrate in the gastrointestinal tract, where the embryos invade the intestinal wall and travel throughout the body in the bloodstream.
They enter the eye via the central retinal artery or the short posterior ciliary arteries. Once in the eye, they can be found in the vitreous cavity or anterior chamber, or within the subretinal space, as with our patient.2
Within several months, the larvae can grow into large cystic structures. A white head, or scolex, often can be recognized moving within the cystic cavity. This is usually helpful in confirming the diagnosis. Standardized ultrasound can also be used to identify the cystic lesion.
Over time, vitreous inflammation often develops, leading to cystoid macular edema. The inflammation becomes much worse once the organism dies. Because of this, surgical removal via a transscleral approach is recommended.2
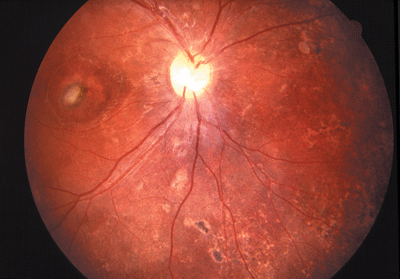 |
| Diffuse unilateral subacute neuroretinitis (DUSN), part of your differential diagnosis, is caused by two nematodes. In this 7-year-old patient, dilated exam of the right eye showed pallor of the optic nerve, diffuse mottling of the RPE and a lesion in the macula. |
DUSN is caused by at least two identified nematodes. The first is a smaller worm that is from either Toxocara canis or Ancylostoma caninum, which are more common in dogs. This intestinal nematode is more prevalent in the southern United States. Human transmission usually occurs through the ingestion of food contaminated with Toxocara eggs, or contact with infected puppies.3
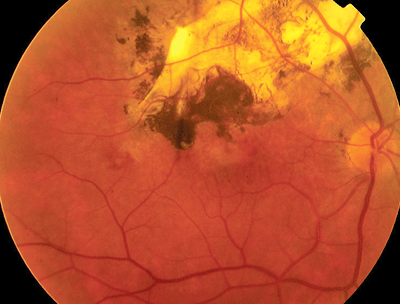 |
|
Ocular toxoplasmosis, perhaps the most common parasite to invade the eye, should also be part of your differential diagnosis. This large pigmented lesion seen in another patient is an old chorioretinal scar, probably from an episode of active toxoplasmosis. |
Of course, ocular toxoplasmosis is perhaps the most common parasite to invade the eye. It is caused by the intracellular protozoan parasite Toxoplasma gondi. The characteristic lesion is a focal white area of active retinochoroiditis, which results from direct invasion of the trophozoite.
We referred our patient to J. Donald M. Gass, M.D., who made the diagnosis. He initially managed the patient with laser photocoagulation to wall off the organism, then performed posterior sclerotomy and a choroidotomy to remove the organism.
The patients visual acuity improved to 20/20 following the surgery.
(Answers: 1) d; 2) d; 3)d; 4) c; 5) c; 6) d.)
1. Vaxa Homeopathic Medicinals. Taenia Solium, The pork tapeworm. Available at: www.vaxa.com/human-tapeworms-taenia-solium.cfm. (Accessed May 24, 2006)
2. Gass JDM. Stereoscopic Atlas of Macular Disease: Diagnosis and Treatment. 4th ed. St. Louis: Mosby-Year Book, 1997:156-8.
3. Sabrosa NA, de Souza EC. Nematode infections of the eye: toxocariasis and diffuse unilateral subacute neuroretinitis. Curr Opin Ophthalmol 2001 Dec;12(6):450-4.


