A 63-year-old Caucasian male presented for consultation with complaints of a chronically red and watering right eye. He said the condition had persisted for at least six months, intermittently improving, but gradually worsening overall. He claimed that his eye really was not terribly uncomfortable, but that the tearing was problematic and interfering with his ability to drive and read. His medical history was positive for controlled hypertension (nebivolol 5mg once daily). A dermatologist diagnosed him with rosacea, but he was not currently treating it.
Upon examination, his right eye showed moderate conjunctival injection and epiphora. The upper and lower lids were grossly normal, but inspection of the inferior nasal region showed distinct swelling with punctal occlusion. When pressure was applied, a small amount of pus regurgitated through the punctum, along with two small yellowish concretions. The nasolacrimal sac area did not appear hyperemic, and was not tender to the touch. The remainder of the ocular surface and anterior segment structures appeared normal. Based upon the history, symptoms and examination, the patient was diagnosed with chronic canaliculitis.
A Red, Red Eye
Canaliculitis is an uncommon infection of the lacrimal system, yet it remains grossly underdiagnosed in clinical practice. The hallmark symptoms include a chronic, recalcitrant red eye with focal swelling and variable tenderness of the medial canthus. Epiphora, or excessive lacrimation to the point of overflow, is also characteristic. Ocular discharge may range from simple tearing to full-blown mucopurulence. In many cases, the patient will report previous therapy with topical antibiotics, but to no avail.
Low-grade infections can sometimes persist for a long time because the clinician simply fails to observe the subtle signs. Studies suggest that the average duration before a correct diagnosis is made may be up to 36 months.1,2
The classic biomicroscopic sign of canaliculitis is said to be a “pouting punctum.”1-10 This term describes the red, swollen and outwardly turned punctal orifice, which tends to resemble a pair of pouting lips. In actuality, however, the most common (and most important) sign is the presence of discharge and concretions upon canalicular compression.11 These dacryoliths, a term which literally translates as “tear stones,” are another hallmark of this disease. According to a recent study, 90% of patients will have dacryoliths that are observable with expression.4 Other important signs include erythema and swelling of the lid and adnexal tissue, and a conjunctivitis that is more pronounced inferiorly and nasally.8 Canaliculitis is typically encountered in older adults, with a mean age of 59 years.2 Women are affected up to five times more often than men.4,6 Most cases are unilateral, though bilateral phenomena have been documented.12,13
Discussion
Canaliculitis is essentially an infection (and subsequent inflammation) of the lacrimal outflow system, at the level of the canaliculus.4 While a great many pathogens have been associated with this condition, the most widely reported organism is a gram-positive, anaerobic bacterium called Actinomyces israelii.4,9 In canaliculitis, infection by Actinomyces (or similar pathogens) helps to produce the aforementioned dacryoliths, which harbor the microbes and create small intervening “pockets” in the canaliculus. This physical blockade by the dacryoliths allows the pathogens to flourish undisturbed, invulnerable to the natural antimicrobial properties of the tear film or even to topically administered antibiotics.4
Canaliculitis can also occur secondarily as a complication of lacrimal occlusion, either from migrated punctal or intracanalicular plugs.4,5 These plugs can function as artificial dacryoliths, harboring potentially pathogenic bacteria and providing an environment in which they can thrive. In some cases, concretions can form around or adjacent to retained plugs.14 Secondary canaliculitis has seen its greatest incidence with use of the SmartPlug (Medennium) device, a thermoacrylic polymer designed for lacrimal occlusion therapy in patients with dry eye.12-16
Treatment Options
Conservative measures such as warm compresses, digital massage, topical antibiotics and even oral antibiotics are generally insufficient to overcome canaliculitis infections, although they may provide temporary improvement and symptomatic relief.4,11,17 Much greater overall success can be achieved by first removing the obstructing dacryoliths. Simply expressing the canaliculus firmly on either side with cotton-tipped applicators should help to “roll” these stones out through the punctum, affording greater access to medications that can help overcome the infection. A study employing this technique, followed by canalicular irrigation with fortified cefazolin (50mg/ml) and the use of topical antibiotics for several weeks resulted in a success rate of 100%, although most subjects required multiple irrigations.17
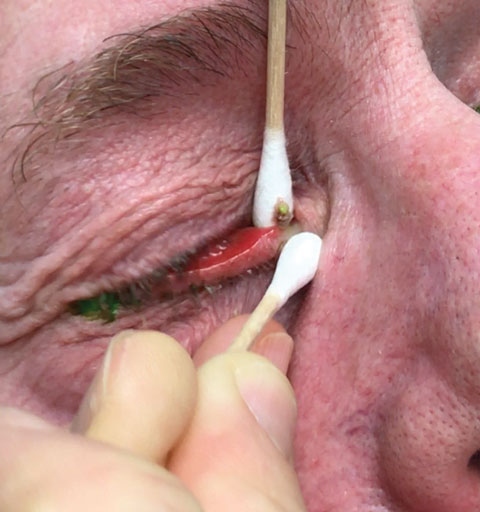 |
| Expressing the canaliculus firmly on either side with cotton-tipped applicators should help “roll” these dacryoliths stones through the punctum, affording medications greater access. Photo and video: Laura M. Periman, MD. |
Should these less invasive efforts for canaliculitis fail to achieve resolution, surgical intervention may be required. Classically, canaliculotomy (surgical excavation of the canaliculus) with canalicular curettage (surgical removal of the dacryoliths and other obstructions of the canaliculus) is considered the treatment of choice.3-7,17 This technique is performed under local anesthesia and involves a horizontal incision through the conjunctiva into the canaliculus, dissecting the nasal lid from the punctal orifice down to the level of the common canaliculus (approximately 10mm). Next, a small chalazion curette is used to remove the dacryoliths and other debris, and canalicular irrigation with antibiotic solution (aqueous penicillin G) or povidone-iodine may be subsequently performed. Performing smears, cultures, or both, of the retrieved material may be helpful in determining the correct pharmacologic course, as postoperative antimicrobial therapy is generally indicated.1
Medical Intervention
In cases of Actinomyces canaliculitis, oral penicillin or ampicillin is commonly prescribed for several weeks following surgical recovery.1,4 The use of topical, broad-spectrum antibiotics (e.g., ciprofloxacin 0.3% solution QID or bacitracin zinc/polymyxin B ointment BID) may be employed as an adjunct to systemic therapy.6
The prognosis for recovery is dependent upon how quickly the correct diagnosis is made, as well as the level of therapeutic invasiveness. With prolonged infections or in cases that require radical surgical intervention, the nasolacrimal system may become scarred and permanently occluded. In such instances, dacryocystorhinostomy may be required to successfully reestablish lacrimal outflow. This surgical technique essentially creates a new channel to bypass the canaliculus and drain tears from the punctum directly into the superior nasal cavity.
Remember, canaliculitis does not come around often, but when it does we need to recognize its calling card: a chronic red eye with persistent tearing in an older patient, who often has not responded to conventional therapy with topical antibiotics. Inspect the punctum and, if it appears swollen or occluded, always check to see if any material can be expressed. Take note of any little stones that come rolling your way, and you’ll know exactly how to proceed.
|
1. Briscoe D, Edelstein E, Zacharopoulos I, et al. Actinomyces canaliculitis: diagnosis of a masquerading disease. Graefes Arch Clin Exp Ophthalmol. 2004;242(8):682-6. 2. Lin SC, Kao SC, Tsai CC, et al. Clinical characteristics and factors associated the outcome of lacrimal canaliculitis. Acta Ophthalmol. 2011;89(8):759-63. 3. Yılmaz M, Sen E, Euron E, et al. Canaliculitis awareness. Turk J Ophthalmol. 2016;46(1):25-29. 4. Freedman JR, Markert MS, Cohen AJ. Primary and secondary lacrimal canaliculitis: a review of literature. Surv Ophthalmol. 2011;56(4):336-47. 5. Zaveri J, Cohen AJ. Lacrimal canaliculitis. Saudi J Ophthalmol. 2014;28(1):3-5. 6. Kim UR, Wadwekar B, Prajna L. Primary canaliculitis: The incidence, clinical features, outcome and long-term epiphora after snip-punctoplasty and curettage. Saudi J Ophthalmol. 2015;29(4):274-7. 7. Anand S, Hollingworth K, Kumar V, et al. Canaliculitis: the incidence of long-term epiphora following canaliculotomy. Orbit. 2004;23:19-26. 8. Liyanage SE, Wearne M. Lacrimal canaliculitis as a cause of recurrent conjunctivitis. Optometry. 2009;80(9):479-80. 9. Vagarali MA, Karadesai SG, Dandur MS. Lacrimal canaliculitis due to actinomyces: a rare entity. Indian J Pathol Microbiol. 2011;54(3):661-3. 10. Xu J, Liu Z, Mashaghi A, et al. Novel therapy for primary canaliculitis: a pilot study of intracanalicular ophthalmic corticosteroid/antibiotic combination ointment infiltration. Medicine (Baltimore). 2015;94(39):e1611. 11. Xiang S, Lin B, Pan Q, et al. Clinical features and surgical outcomes of primary canaliculitis with concretions. Medicine (Baltimore). 2017;96(9):e6188. 12. Scheepers M, Pearson A, Michaelides M. Bilateral canaliculitis following SmartPLUG insertion for dry eye syndrome post LASIK surgery. Graefes Arch Clin Exp Ophthalmol. 2007;245(6):895-7. 13. Klein-Theyer A, Boldin I, Rabensteiner DF, et al. Prevalence of canaliculitis after Smartplug insertion during long-term follow-up. Br J Ophthalmol. 2015;99(8):1134-6. 14. Hill RH 3rd, Norton SW, Bersani TA. Prevalence of canaliculitis requiring removal of SmartPlugs. Ophthal Plast Reconstr Surg. 2009;25(6):437-9. 15. SmartPlug Study Group. Management of complications after insertion of the SmartPlug punctal plug: a study of 28 patients. Ophthalmology. 2006;113(10):1859.e1-6. 16. Fowler AM, Dutton JJ, Fowler WC, et al. Mycobacterium chelonae canaliculitis associated with SmartPlug use. Ophthal Plast Reconstr Surg. 2008;24(3):241-3. 17. Mohan ER, Kabra S, Udhay P, Madhavan HN. Intracanalicular antibiotics may obviate the need for surgical management of chronic suppurative canaliculitis. Indian J Ophthalmol. 2008;56(4):338-40. |

