Although many clinicians consider cataract surgery to be an economical procedure, cost containment is always a concern in an unstable economy. Cataract is one of the leading causes of reversible vision loss in the world, and ranks as the most common age-related eye disease in America.1-3 With nearly three million cataract surgeries performed in the United States each year, it is estimated that the total annual cost of cataract management exceeds six billion dollars.3,4
If researchers were able to successfully develop even moderate avenues of prevention, the cost savings could amount to tens of millions of dollars. So, the search is on for methods to delay the onset of clinically significant cataract formation. Currently, considerable research is being conducted to evaluate such modalities.
In this article, we will look at risk factors for age-related cataracts (ARCs), its pathophysiology and some noteworthy research regarding new and potential treatments.
Risk Factors and Pathophysiology
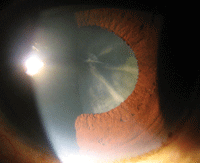
Cortical cataracts—characterized by white, wedge-like opacities that start in the periphery of the lens—form due to the disruption of fiber cell membranes, followed by the disintegration of the damaged fiber cell’s cytoplasmic contents.
So, what causes a cataract? More to the point: Can any of those causes be modified or removed in order to prevent cataract formation?
Intrinsic or non-modifiable risk factors include age, gender, race, family history of cataracts, myopic refractive error and the size of the crystalline lens.5-8 Major environmental risk factors include, but are not limited to, UV exposure, living in warmer ambient temperatures, nutrition and supplement usage, systemic disease and its medical management, increased body mass index, and smoking.5-8 The most common forms of ARCs include nuclear sclerotic, cortical spoke and posterior subcapsular (PSC) lens opacities.1-6
• Nuclear sclerosis is considered the end-product of insoluble lens protein aggregation.8,9 Although the process is not completely understood, these changes in the lens proteins are due to increased protein oxidation as well as modifications of the crystalline proteins.8,9
As protein oxidation increases, insoluble proteins accumulate and aggregation occurs, causing the process of aging of the lens—in which the lens nucleus becomes more rigid, light scattering occurs and lens coloration increases.8,9
• Cortical cataracts form due to the disruption of fiber cell membranes, followed by the disintegration of the damaged fiber cell’s cytoplasmic contents.6-9 Different than nuclear opacification, cortical cataract formation occurs whenever alterations develop in the cortical fibers.
This type of cataract formation is not necessarily a consequence of aging. Unlike nuclear cataracts—which evolve uniformly throughout the center of the lens—cortical lens changes begin in small clusters of cortical fiber cells near the equator of the lens and progress as stressors dictate.6-9
• PSC opacities, perhaps the least understood type of ARC, occur less often than nuclear or cortical opacities.8-10 Postmortem lens examination has revealed that the cellular changes appearing secondary to PSC are streams of cells migrating from the equator to the posterior pole.8-10
These cells are swollen with eosinophilic cytoplasm, suggesting that they have somehow failed to elongate.8-10
The abnormal conglomeration reduces the transparency of the lens close to the anterior convergence point (or nodal point) of the eye, interfering with the convergent light of near objects.
Are Vitamin Supplements the Answer?
Dietary antioxidants, such as vitamin C (ascorbate), vitamin E (tocopherol), beta-carotene and omega-3 fatty acids, have been included in human epidemiologic, animal and laboratory-based studies that investigate ARC formation (see “Significant Studies of Vitamins/Minerals in ARC”).11
Carotenoids, specifically the xanthrophylls xanthin and zeaxanthin that have been found in the crystalline lens, also are being studied to assess their ability to influence cataractogensis.12
Vitamin C
Significant Studies of Vitamins/Minerals in ARC
• The Age-Related Eye Disease Study (AREDS), sponsored by the National Eye Institute, is the most highly publicized study to investigate the use of oral supplements for eye care.36 Researchers used a high-dose formulation of antioxidants and zinc to determine if these oral supplements could alter the clinical course of AMD and/or the progression of lens opacities.36
After five years of supplement usage, the opacity component of the study revealed that the AREDS supplement formulation did not slow the development or progression of age-related lens opacification.36
• AREDS 2 has been designed to determine if modifying the formulation—by adding macular xanthophylls (lutein and zeaxanthin) and/or long-chain omega-3 fatty acids (DHA) and eicosapentaenoic acid (EPA)—would impact the progression to advanced AMD in high-risk patients, or if the supplement could influence the progression of ARC.47 In addition, the AREDS 2 formulation includes reduced zinc and/or no beta-carotene.47 The outcome of AREDS 2 is currently pending.
• The Roche European American Cataract Trial (REACT) was a multicenter, double-masked, placebo-controlled study that monitored cataract progression over a four-year period.48 A total of 297 adult American and English patients were randomized to receive a placebo or an oral multivitamin containing beta-carotene, vitamin C and vitamin E. Cataract severity was documented with serial digital retroillumination imagery of the lens.
Progression was quantified by image analysis assessing increased area of lens opacity. In the American patient population, the combination of micronutrients produced a slight deceleration in the progression of ARC after a three-year period. In the English population, no statistically significant benefit was observed.48
• The Linxian Cataract Study looked at subjects from a rural Chinese population, ages 45 to 74, in a large trial to determine if a multivitamin supplement could affect the risk of ARC.49 Subjects received one of four multivitamin/mineral combinations. The possible combinations included retinol/zinc, riboflavin/niacin, ascorbic acid/molybdenum and selenium/alpha-tocopherol/beta-carotene. Subjects in the control group received a placebo.
In the 65- to 74-year-old patient group, who were randomized to the retinol/zinc preparation, a statistically significant 36% reduction in nuclear cataracts was observed.49 No statistical significance was observed in the other age groups, other combination groups or in the development of cortical spoke or PSC cataracts.49
• The Beaver Dam Eye Study was an investigation of the relationship between multivitamin supplement use and the five-year incidence of nuclear, cortical and posterior subcapsular cataract.41 The subjects reported the type, dosage and duration of supplement used at baseline and logged their supplement usage to the end of the five-year trial period.41 When compared to nonusers, those reporting the use of vitamin C or E showed a 60% lower five-year risk of nuclear or cortical cataract formation.50
The authors concluded that the evidence supported an association between supplement use and benefit, but also acknowledged the limitations of the study’s design, its inability to measure lifestyle differences and the inability of the study to determine the specifics of other daily nutrients consumed.50
Vitamin C is present in high concentrations in the aqueous humor and the human lens.13 It prevents aggregation of crystallin by inhibiting disulphide cross-linking; by acting as a scavenger of reactive oxygen species; and by sequestering unfolded lens proteins.13,14 Mixed conclusions have been reported with respect to the potential benefit of a vitamin C supplement and reduced cataract incidence.15-20
One investigation monitored 24,593 Swedish women who were administered a questionnaire regarding lifestyle factors and supplement use.15 Following eight years of monitoring, researchers concluded that the use of vitamin C supplements may actually be associated with a higher risk of ARC formation.15
In contrast, some studies identified dietary vitamin C as having a protective role that may lower the risk of ARC formation.16,17 In addition, a recent study examined cataract formation revealing a strong association with vitamin C depletion and lens opacification.18 In separate investigations assessing the impact of long-term vitamin and carotenoid use, vitamin C was found to have an association with reduced risk of cortical cataract formation in a cohort of non-diabetic women.19
A later report from the same cohort of U.S. women discovered that subjects with the highest intake of vitamin C had a reduced prevalence of nuclear opacities.20
In the Baltimore Longitudinal Study on Aging, researchers assessed plasma levels of ascorbate in 660 subjects and discovered that recommended plasma levels were not associated with risk of nuclear or cortical lens opacities.21 In phase II of the Physician Health Study, male physicians from the United States were randomized to use vitamin C or placebo—this large study demonstrated that long-term use of vitamin C had no overall effect on cataract occurrence.21 Taking these data as a whole, it appears that vitamin C neither prevents nor provokes cataractogensis.13-22
Vitamin E
Vitamin E, specifically alpha-tocopherol, is a lipid-soluble antioxidant that is concentrated in lens fibers and membranes.23 The coenzyme is believed to inhibit cataract formation by reducing photoperoxidation of lens lipids and by stabilizing lens cell membranes; however, studies have shown vitamin E supplementation does not necessarily reduce the incidence of ARC.23,24
As was the case with vitamin C, phase II of the Physician Health Study found that long-term vitamin E supplementation had no overall effect on cataract occurrence.22 Additional large clinical trials that reported similar results include the Alpha-Tocopherol, Beta-Carotene (ATBC) Cancer Prevention Study; the Vitamin E, Cataract, and Age-Related Macular Degeneration (VECAT) Study; and the Women’s Health Study (WHS).25-27
Similarly, investigators in Melbourne, Australia, determined that a daily dose of 500 international units of vitamin E used over a four-year period did not reduce the incidence of progression of ARC.28 Also, a randomized, double-masked, placebo-controlled trial using 600 international units of vitamin E on an every-other-day dosing schedule vs. a placebo for 9.7 years showed no benefit in daily use of vitamin E in cataract prevention.29
In short, the majority of evidence suggests that vitamin E does not delay the onset of cataracts.
Beta-carotene
Beta-carotene, a fat-soluble compound and member of the carotenoid family, is a naturally occurring component of fruits, grains, oils and vegetables.30 Common foods that contain beta-carotene include green plants, carrots, sweet potatoes, squash, spinach, apricots and green peppers.
In its natural form, beta-carotene is a precursor (inactive form) to vitamin A.30 Beta-carotene produces retinol—a fat-soluble form of vitamin A.
Beta-carotene has been the focus of investigations due to its effect as an antioxidant at low partial pressures. Low partial pressures are known to exist within the crystalline lens, making the substance worthy of investigating as a possible cataract suppressant. The obvious advantage is that this compound is obtainable naturally in fruits and vegetables.30,31
WHS tested the benefits of beta-carotene (50mg on alternate days) on the development of ARC formation in 18,405 eligible patients.31 After more than two years of follow up, researchers concluded that beta-carotene had neither a large benefit nor harmful effect on
cataractogenesis.31
A similarly designed study, which included more than 22,000 American male physicians, concluded after 12 years of beta-carotene supplementation, that no overall benefit or harm on cataract development was identified.32
Omega-3 Fatty Acids
Omega-3 polyunsaturated fatty acids are fats that may be found in marine and plant oils. In humans, during late fetal and early neonatal life, the brain and eye are primarily enriched with the omega-3 fatty acid docosahexaenoic acid (DHA).33 High levels of DHA are present within the outer segments of the retina’s photoreceptor cells.
Recent literature has identified that the dietary intake of omega-3 fatty acids may reduce the risk of early age-related macular degeneration (AMD).34,35 The Age-Related Eye Disease Study is ongoing and is investigating if omega-3 fatty acids, along with other nutritional supplements, may aid in the prevention or decrease the rate of progression of AMD.36
A systematic literature review in 2005 investigated the effect that omega-3 fatty acids have on human eye health.37 It was specifically designed to examine whether omega-3 fatty acids could prevent, slow the rate of progression or decrease the rate of ARC surgery in an aging population. Data revealed no statistically significant association between the intake of foods or oils containing omega-3 fatty acid and a decreased incidence of ARC.37
In our review of the literature that has emerged since that report, we found no peer-reviewed medical or scientific studies that investigated stand-alone, omega-3 fatty acid supplementation and its influence on ARC. We did, however, discover a paucity of information discussing the potential benefits of omega-3 fatty acid intake and cataract formation as we explored commercial products. However, the majority of this information appears in non-peer reviewed medical literature.
Other Proposed Treatments
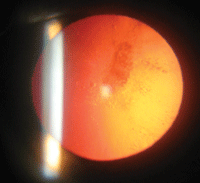
Posterior subcapsular cataracts start as small, opaque areas that usually form near the back of the lens.
Compared to proteins, lipids make up only a small component of the lens structure. Lipid peroxidation (LPO) does, however, lead to the disintegration of lens fiber plasma membrane.38 One proposed treatment strategy to prevent the formation of cataractous opacities is to prevent the activation of LPO end products by administering antioxidants that have a strong affinity to LPO.2,38 Carnosine is a histidine-containing compound that occurs naturally in several human tissues, particularly muscle.
One study reported that carnosine is a potent lipid peroxidase mimetic that possesses powerful antioxidant properties.39
N-acetylcarnosine (NAC) is a pro-drug of carnosine that has been developed for clinical use as an eye drop. Marketed as Can-C (1% N-acetylcarnosine, Innovative Vision Products), the topical solution is supplied as a cellulose-based compound that can be purchased without a physician’s prescription.39-41 In a randomized, double blind, placebo-controlled clinical trial of NAC, Mark Babizhayev, Ph.D., and colleagues reported improvement in best corrected visual acuity, glare sensitivity and increased lens transmissivity.41
Our literature search of peer-reviewed publications relating to NAC found that virtually all information on the subject had been published by Dr. Babizhayev and his colleagues. Interestingly, the publishers are not only the research scientists who discovered and patented the formulation of NAC, but they also have disclosed interests in Innovative Vision Products, the manufacturer of Can-C. With this in mind, one may recognize the potential bias that may exist, leaving the scientific and medical community with an interest in further evidenced-based research investigating the efficacy of NAC.
We located a study from the University of Sydney that investigated the efficacy of NAC with respect to protecting the crystalline lens from oxidation.42 The investigators, using mass spectrometry, concluded that there was no evidence suggesting that NAC had any significant direct effect on reducing the levels of oxidation within lens crystallins.42 Currently, a systematic review is underway in the United Kingdom that will investigate the effectiveness of carnosine as a cataract-reversing and preventive agent.43 This information is pending and may shed more light on NAC as a possible medical therapy for delaying visually significant cataract formation.43
Although research has been limited to animal studies, eye drops containing disulfiram (DSF) are being considered for their anti-cataract effect.44 DSF is a powerful antioxidant that scavenges reactive oxygen species. Due to its poor water solubility, DSF must be combined with methylcellulose to improve solubility, stability and bioavailability. Thus far, animal models have resulted in delaying cataract development in hereditary, as well as steroid-induced cataractogenesis.44-46
Most cataracts are due to natural, slowly progressive changes in lenticular physiology. This fact alone poses a challenge to those who are designing trials to reduce, delay or reverse the effects of ARC.
To date, no human trial has conclusively displayed clinically significant, reliable data that any one treatment or combination of treatments can produce a delay in onset, reduction in progression, or reversal of signs or symptoms of ARC.
For now, the most effective strategies used to prevent cataract formation or delay progression include avoiding dehydration and illness, improving nutrition, staying tobacco-free, and limiting sun exposure.
Dr. Myers is senior staff optometrist at the Coatesville Veterans Affairs Hospital in Pennsylvania. Dr. Gurwood is professor of clinical sciences at The Eye Institute of the Pennsylvania College of Optometry at Salus University in Elkins Park, Pa. He also authors Review’s “Diagnostic Quiz.”
1. Toh T, Morton J, Coxon J, Elder MJ. Medical treatment of cataract. Clin Experiment Ophthalmol. 2007 Sep-Oct;35(7):664-71.
2. Machan CM, Hrynchak PK, Irving EL. Modeling the prevalence of age-related cataract: Waterloo Eye Study. Optom Vis Sci. 2011 Dec 8. [Epub ahead of print]
3. West S. Epidemiology of cataract: accomplishments over 25 years and future directions. Ophthalmic Epidemiol. 2007 Jul-Aug;14(4):173-8.
4. Salm M, Belsky D, Sloan FA. Trends in cost of major eye diseases to Medicare, 1991 to 2000. Am J Ophthalmol. 2006 Dec;142(6):976-82.
5. Beebe DC, Holekamp NM, Shui YB. Oxidative damage and the prevention of age-related cataracts. Ophthalmic Res. 2010;44(3):155-65.
6. Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. Br J Ophthalmol. 2012 May;96(5):614-8.
7. Abraham AG, Condon NG, West Gower E. The new epidemiology of cataract. Ophthalmol Clin North Am. 2006 Dec;19(4):415-25.
8. Congdon N, O’Colmain B, Klaver CC, et al. Causes and prevalence of visual impairment among adults in the United States. Arch Ophthalmol. 2004 Apr;122(4):477-85.
9. Michael R, Barraquer RI, Willekens B, et al. Morphology of age-related cuneiform cortical cataracts: the case for mechanical stress. Vision Res. 2008 Feb;48(4):626-34.
10. Eshagian J. Human posterior subcapsular cataracts. Trans Ophthalmol Soc U K. 1982;102 Pt 3:364-8.
11. Williams DL. Oxidation, antioxidants and cataract formation: a literature review. Vet Ophthalmol. 2006 Sep-Oct;9(5):292-8.
12. Yeum KJ, Taylor A, Tang G, Russell RM. Measurement of carotenoids, retinoids, and tocopherols in human lenses. Invest Ophthalmol Vis Sci. 1995 Dec;36(13):2756-61.
13. Varma SD, Richards RD. Ascorbic acid and the eye lens. Ophthalmic Res. 1988;20(3):164-73.
14. Linklater HA, Dzialoszynski T, McLeod HL, et al. Modelling cortical cataractogenesis. XI. Vitamin C reduces gamma-crystallin leakage from lenses in diabetic rats. Exp Eye Res. 1990 Sep;51(3):241-7.
15. Rautiainen S, Lindblad BE, Morgenstern R, Wolk A. Vitamin C supplements and the risk of age-related cataract: a population-based prospective cohort study in women. Am J Clin Nutr. 2010 Feb;91(2):487-93.
16. Valero MP, Fletcher AE, De Stavola BL, et al. Vitamin C is associated with reduced risk of cataract in a Mediterranean population. J Nutr. 2002 Jun;132(6):1299-306.
17. Yoshida M, Takashima Y, Inoue M, et al. Prospective study showing that dietary vitamin C reduced the risk of age-related cataracts in a middle-aged Japanese population. Eur J Nutr. 2007 Mar;46(2):118-24.
18. Ravindran RD, Vashist P, Gupta SK, et al. Inverse association of vitamin C with cataract in older people in India. Ophthalmology. 2011 Oct;118(10):1958-65.e2.
19. Taylor A, Jacques PF, Chylack LT, et al. Long-term intake of vitamins and carotenoids and odds of early age-related cortical and posterior subcapsular lens opacities. Am J Clin Nutr 2002;75: 40-9.
20. Jacques PF, Chylackk LT, Hankinson SE, et al. Long-term nutrient intake and early age-related nuclear lens opacities. Arch Ophthalmol 2001 July;119(7): 1009-19.
21. Vitale S, West S, Hallfrisch J, et al. Plasma antioxidants and risk of cortical and nuclear cataract. Epidemiology. 1993 May;4(3):195-203.
22. Christen WG, Glynn RJ, Sesso HD, et al. Age-related cataract in a randomized trial of vitamins E and C in men. Arch Ophthalmol. 2010 ;128(11):1397-405.
23. Varma SD, Kovtun S, Hegde KR. Role of ultraviolet irradiation and oxidative stress in cataract formation-medical prevention by nutritional antioxidants and metabolic agonists. Eye Contact Lens. 2011 Jul;37(4):233-45.
24. Ohta Y, Okada H, Majima Y, Ishiguro I. Anticataract action of vitamin E: its estimation using an in vitro steroid cataract model. Ophthalmic Res. 1996;28(Suppl 2):16-25.
25. Teikari JM, Rautalahti M, Haukka J, et al. Incidence of cataract operations in Finnish male smokers unaffected by alpha tocopherol or beta carotene supplements. J Epidemiol Community Health. 1998 Jul;52(7):468-72.
26. Nadalin G, Robman LD, McCarty CA, et al. The role of past intake of vitamin E in early cataract changes. Ophthalmic Epidemiol. 1999 Jun;6(2):105-12.
27. Chasan-Taber L, Willett WC, Seddon JM, et al. A prospective study of vitamin supplement intake and cataract extraction among U.S. women. Epidemiology. 1999 Nov;10(6):679-84.
28. McNeil JJ, Robman L, Tikellis G, et al. Vitamin E supplementation and cataract: randomized controlled trial. Ophthalmology. 2004 Jan;111(1):75-84.
29. Christen WG, Glynn RJ, Chew EY, Buring JE. Vitamin E and age-related cataract in a randomized trial of women. Ophthalmology. 2008 May;115(5):822-29.e1.
30. Burton GW, Ingold KU. Beta-carotene: an unusual type of lipid antioxidant. Science. 1984 May 11;224(4649):569-73.
31. Christen W, Glynn R, Sperduto R, et al. Age-related cataract in a randomized trial of beta-carotene in women. Ophthalmic Epidemiol. 2004 Dec;11(5):401-12.
32. Christen WG, Manson JE, Glynn RJ, et al. A randomized trial of beta carotene and age-related cataract in US physicians. Arch Ophthalomol. 2003 Mar;121(3):372-8.
33. Innis SM. Perinatal biochemistry and physiology of long-chain polyunsaturated fatty acids. J Pediatr. 2003 Oct;143(4 Suppl):S1-8.
34. Ho L, van Leeuwen R, Witteman JC, et al. Reducing the genetic risk of age-related macular degeneration with dietary antioxidants, zinc, and omega-3 fatty acids: The Rotterdam study. Arch Ophthalmol 2011 June; 129(6):758-66.
35. Christen WG, Schaumberg DA, Glynn RJ, et al. Dietary ω-3 fatty acid and fish intake and incident age-related macular degeneration in women. Arch Ophthalmol 2011;129(7):921-9.
36. Age-Related Eye Disease Study Research Group. A randomized, placebo-controlled, clinical trial of high-dose supplementation with vitamins C and E and beta carotene for age-related cataract and vision loss: AREDS report no. 9. Arch Ophthalmol. 2001 Oct;119(10):1439-52.
37. Hodge W, Barnes D, Schachter HM, et al. Effects of omega-3 fatty acids on eye health. Evid Rep Technol Assess (Summ). 2005 Jul;(117):1-6.
38. Babizhayev MA, Deyev AI, Yermakova VN, et al. Lipid peroxidation and cataracts: N-acetylcarnosine as a therapeutic tool to manage age-related cataracts in human and canine eyes. Drugs R D. 2004;5(3):125-39.
39. Babizhayev MA, Yermakova VN, Sakina NL, et al. N alpha-acetylcarnosine is a prodrug of L-carnosine in ophthalmic application as antioxidant. Clin Chim Acta. 1996 Oct 15;254(1):1-21.
40. Babizhayev MA, Deyev AI, Yermakova VN, et al. Efficacy of N-acetylcarnosine in the treatment of cataracts. Drugs R D. 2002;3(2):87-103.
41. Babizhayev MA, Deyev AI, Yermakova VN, et al. Image analysis and glare sensitivity in human age-related cataracts. Clin Exp Optom. 2003 May;86(3):157-72.
42. Ha JW, Schwahn AB, Downard KM. Ability of N-acetylcarnosine to protect lens crystallins from oxidation and oxidative damage by radical probe mass spectrometry (RP-MS). Rapid Commun Mass Spectrom. 2010 Oct 15;24(19):2900-8.
43. Dubois VDJP, Bastawrous A. N-acetylcarnosine (NAC) drops for age-related cataract. Cochrane Database of Systematic Reviews. 2011, Issue 12. Art. No.: CD009493.
44. Nagai N, Ito Y, Takeuchi N. Pharmacokinetic and pharmacodynamic evaluation of the anti-cataract effect of eye drops containing disulfiram and low-substituted methylcellulose using ICR/f rats as a hereditary cataract model. Biol Pharm Bull. 2012;35(2):239-45.
45. Sternberg K, Terwee T, Stachs O, et al. Drug-induced secondary cataract prevention: experimental ex vivo and in vivo results with disulfiram, methotrexate and actinomycin D. Ophthalmic Res. 2010;44(4):225-36.
46. Nabekura T, Koizumi Y, Nakao M, et al. Delay of cataract development in hereditary cataract UPL rats by disulfiram and aminoguanidine. Exp Eye Res. 2003 Feb;76(2):169-74.
47. Meleth AD, Gensler G, Clemons TE, et al, Age-Related Eye Disease Study 2 (AREDS2). Baseline nutritional characteristics of the Age-Related Eye Disease Study 2 (AREDS2) cohort. Annual Meeting, Association for Research in Vision and Ophthalmology (ARVO), Fort Lauderdale, Fl., May 2009. 279-A379.
48. Chylack LT Jr., Brown NP, Bron A, et al. The Roche European American Cataract Trial (REACT): a randomized clinical trial to investigate the efficacy of an oral antioxidant micronutrient mixture to slow progression of age-related cataract. Ophthalmic Epidemiol. 2002 Feb;9(1):49-80.
49. Sperduto RD, Hu TS, Milton RC, et al. The Linxian cataract studies. Two nutrition intervention trials. Arch Ophthalmol. 1993 Sep;111(9):1246-53.
50. Mares-Perlman JA, Lyle BJ, Klein R, et al. Vitamin supplement use and incident cataracts in a population-based study. Arch Ophthalmol. 2000 Nov;118(11):1556-63.

