An estimated 20.5 million (17.2%) Americans past age 40 have cataract in either eye, and the total number of persons who have cataract is estimated to rise to 30.1 million by 2020, according to a 2004 report from the Eye Diseases Prevalence Research Group. Further, the number of Americans affected by cataract and undergoing cataract surgery will dramatically increase over the next 20 years as the
Also, refractive errors affect approximately one-third of persons 40 years or older in the
However, there probably isnt as exciting a time as now to be involved in comanaging cataract and refractive surgery patients. Patients have much more variety than in the past, meaning that O.D.s must stay abreast to help ensure the most successful visual outcome.
Research from this years Association for Research in Vision and Ophthalmology (ARVO) meeting yielded findings on visual quality and intraocular lenses (IOLs), implantable contact lenses, complications of cataract surgery and even options that may improve the vision of patients who have keratoconus.
CME and Endophthalmitis
Cystoid macular edema (CME) is the second most common complication of modern cataract surgery. It also is the most common cause of visual decline during the immediate postoperative period after uncomplicated cataract surgery. Other than anecdotal risk factors, however, we still have no idea why this occurs.
But, researchers from
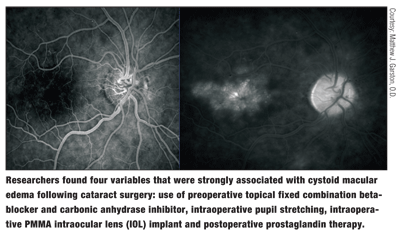
Four variables were strongly associated with clinical CME, the researchers found. These were use of preoperative topical fixed combination beta-blocker and carbonic anhydrase inhibitor, intraoperative pupil stretching, intraoperative PMMA intraocular lens implant and postoperative prostaglandin therapy.
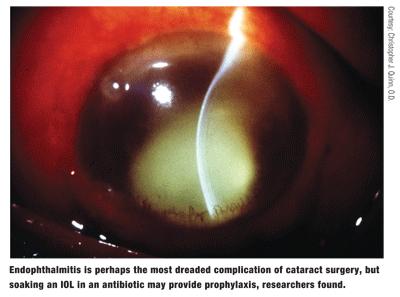
Perhaps the most dreaded complication from cataract surgery, however, is endophthalmitis. This complication may present one to four days following surgery or have a delayed onset of weeks or even years. The consequences may be devastating.
Researchers from Illinois, however, may have found a viable option to prevent this from occurring.2673 They immersed Staar Surgical Collamer IOLs in Vigamox (moxifloxacin, Alcon), Quixin (levofloxacin, Vistakon Pharmaceuticals) and Zymar (gatifloxacin, Allergan) for 10 minutes or 15 minutes before placing them in a mock anterior chamber (MAC). The MAC consisted of an enclosed chamber (0.3ml in volume), attached to a micro pump and a normal saline reservoir. They also inserted these presoaked IOLs in the capsular bag of 20 rabbits (40 eyes).
While in the MAC, lenses soaked in moxifloxacin for 15 minutes developed a maximum antibiotic concentration of 95g/ml at 120 minutes and sustained concentrations greater than 4g for up to 10 hours. Those soaked in moxifloxacin for 10 minutes achieved maximum concentration of 57.5g/ml and concentrations greater than 4g for up to seven hours. Those lenses soaked in gatifloxacin and levofloxacin achieved similar concentrations. Implantation of the IOL in the rabbit model produced antibiosis for up to six hours. Immersion of the IOL in an antibiotic prior to cataract surgery may one day be a viable option for preventing endophthalmitis, the researchers say.
IOLs and Visual Quality
Theres a debate among practitioners about whether to implant an aspheric or spherical IOL when a cataract patient receives a monovision procedure. The concern: Aspheric IOLs may provide higher-quality vision than spherical IOLs, but aspheric IOLs cause the patient to lose depth of focus. Current thinking is that the traditional spherical IOLs might be better for monovision because there is greater depth of field for near vision tasks.
 A new study, however, calls that argument into question. Researchers from
A new study, however, calls that argument into question. Researchers from
Wavefront analysis revealed fewer spherical aberrations and less higher-order aberrations in those patients who received the aspheric lens. There were no statistically significant differences in defocus, coma, astigmatism, trefoil and tetrafoil. The researchers also found that the aspheric IOL did not compromise depth of focus.
Patients achieved better results in contrast sensitivity under mesopic and mesopic-with-glare conditions; but, there was no difference in contrast sensitivity between the lenses under photopic conditions. Perhaps the improved quality of vision and the neutral aspheric optics allow for greater depth of field, allowing one to have optimal vision correction and maintain an equivalent depth of focus.
Correcting High Myopia
Patients with large amounts of myopia have always presented special concerns. Among them: LASIK will not be adequate, and phakic IOLs will not be as accurate in the higher prescriptions.
Not so, say researchers from the
At six months, 89% of eyes had uncorrected visual acuity (UCVA) of 20/40, and 49% of eyes had uncorrected visual acuity of 20/20 or better. All eyes now had best-corrected visual acuity (BCVA) of 20/25 or better, and 95% of the eyes now had BCVA of 20/20 or better. At six months, 89% of eyes were within 1.00D of the target correction, and 75% of LASIK eyes were within 0.50D of the target correction.
At one month, three out of five eyes that received the phakic ICL had UCVA of 20/20 or better, and one patient measured 20/25. One hundred percent of the eyes that received the phakic ICL were within +/-0.50D spherical equivalent of target correction, showing extremely good accuracy even in the higher myopes.
Both procedures achieved favorable results, but additional experience and longer follow-up evaluation are warranted for the ICL group, the researchers say.
Deep Anterior Lamellar Keratoplasty
Outside of LASIK, femtosecond technology may have applications for 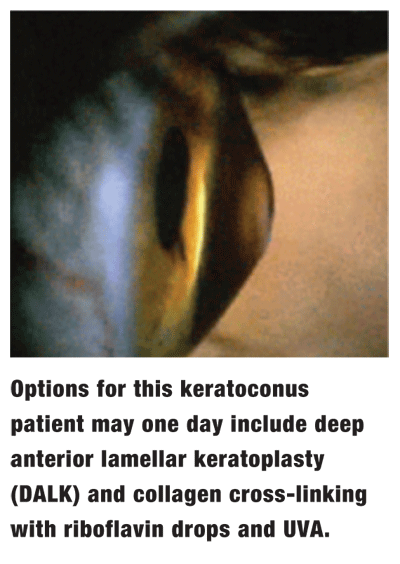 keratoconus patients vs. using a trephine.
keratoconus patients vs. using a trephine.
Many keratoconus patients eventually require a corneal transplant. However, because keratoconus spreads far into the periphery, the surgeon must remove a large button. The transplant also involves removal of Descemets membrane and the endothelium, even though those layers remain healthy. This is especially true in younger patients.
Deep anterior lamellar keratoplasty (DALK) presents an alternative for these patients. In DALK, the surgeon only removes damaged portions of the cornea. This preserves healthy endothelial tissue, requires fewer sutures than a full-thickness graft and allows the cornea to remain stronger.
Researchers from
Although one patient had a perforation that required penetrating keratoplasty, there were no intraoperative complications in the other four cases. The graft was clear at the end of the first week post-op. Three months after surgery, mean uncorrected visual acuity was 0.30D, and mean best spectacle corrected visual acuity was 0.60D.
The researchers believe that this technique for performing DALK is safe and effective, but add that greater follow-up is needed.
Stabilizing Keratoconus
In keratoconus patients, the bands of collagen tissue in the cornea do not hold together. So, collagen cross-linking induced by riboflavin drops and exposure to ultraviolet-A radiation (UVA) followed by excimer laser treatment may be a treatment option for keratoconus. One day, it might also make keratoconus patients whose eyes are pretreated with riboflavin eligible for refractive surgery.
In this case, researchers pretreated 36 eyes with riboflavin drops and exposed patients to UVA (370nm) for 30 minutes.5324 The UV light strengthens the drops. At the same time, the riboflavin protects against retinal burns from the UV light.
Collagen cross-linking held the bands of collagen together, and treatment appeared to stabilize the progression of keratoconus. Also, keratometry improved from 55.00D to 47.50D. Pachymetry decreased from 420m to 390m.
Afterward, patients underwent topography-guided surface ablation. UCVA and best spectacle-corrected visual acuity improved from 20/400 to 20/50 and from 20/100 to 20/30, respectively.
The downside to this treatment: Recovery is painful for the first 24 to 48 hours even with cycloplegia, pain medications and bandage contact lenses. Oral analgesics may be warranted.
Of note: Another study presented at this years meeting found that the UVA and riboflavin combination has both antibacterial and antifungal properties and may one day become a treatment for infectious keratitis.2676 Further in vivo experiments are under way to test the efficacy of this approach.
Dr. Karpecki is Review of Optometrys education advisor and author of the Research Review column. He recently accepted a position in cornea and ocular surface disease at the Cincinnati Eye Institute.
2673. Nijm ALM, Ulanski LJ II, Tu EY, et al. Using the STAAR Collamer intraocular lens as a drug delivery system for the prevention of endophthalmitis.
2676. Behrens A, Castro-Combs J, Noguera G, Martins S. UV-A and riboflavin: potential application as a new broad-spectrum treatment for infectious keratitis.
3135. Bottos KM, Rocha KM, Bottos JM, et al. Wavefront analysis, contrast sensitivity and depth of focus in eyes implanted with aberration free IOL (Softport AO) and spheric IOL (Soflex SE): a multicentric randomized prospective study.
4678. Mosca L, Fasciani R, Mosca L, et al. Deep anterior lamellar keratoplasty performed with Intralase femtosecond laser for keratoconus: personal surgical technique.
5324. Lai EC, Kanellopoulos AJ. Keratoconus management: riboflavin/ultraviolet A-induced collagen cross-linking followed by excimer surface ablation.
5359. Parker JW, Sugar A, Soong HK, et al. Outcomes of LASIK and Visian phakic implantable contact lens in the treatment of high myopia.
5462. Yuen D, Mao A, Quinn J, Tingey D. Clinically significant cystoid macular edema after cataract surgery: a retrospective analysis to identify predictors.

