History
 A 58-year-old white male presented for a comprehensive eye examination, with a chief complaint of blurred near vision in both eyes. He explained that his spectacles were old and that he simply required a new pair.
A 58-year-old white male presented for a comprehensive eye examination, with a chief complaint of blurred near vision in both eyes. He explained that his spectacles were old and that he simply required a new pair.
His systemic history was remarkable for both type 2 diabetes mellitus and hypertension, which were well controlled with metformin and lisinopril. Additional questioning uncovered a long history of substance abuse. His ocular history was non-contributory. He reported no known allergies of any kind.
Diagnostic Data
Best-corrected visual acuity measured 20/20 OU at distance and 20/40 OU at near. External examination was normal, with no evidence of afferent pupillary defect. Refraction revealed mild hyperopia with presbyopia that was correctable to 20/20 at distance and near.
Biomicroscopy showed normal anterior segment structures, with no rubeosis. IOP measured 16mm Hg OU. His cup-to-disc ratio measured 0.40 x 0.50 OU.
|
|
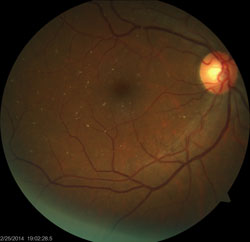
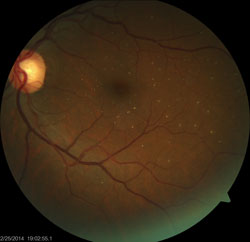
The pertinent dilated fundus findings are illustrated in the photographs.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What's the likely prognosis?
Discussion
In addition to fundus photography, we performed an optical coherence tomography scan and visual fields test to determine if the patient had any structural or functional losses secondary to glaucoma.
The diagnosis in this case was talc retinopathy––a build-up of irregularly shaped, white or yellow crystalline emboli in the retinal vasculature. In this case, the process was also occurring in the systemic circulation. 1-3 These intravascular particles range from 6µm to 8µm in diameter and are typically seen bilaterally in the inner retina.3,4 This condition is a consequence of long-term intravenous drug use.1-4
Talc is an innate mineral used as filler in certain recreational drugs, such as methylphenidate hydrochloride, heroin and cocaine. Talc cannot dissolve in blood, so the mineral becomes embolic.2,3
As long as the talc deposits do not lodge in vessels and completely obstruct flow, they do not pose a significant threat to contaminated organs. Over time, and with continued drug abuse, however, the particles can become larger. In the eye, this can induce ocular complications, such as retinal artery occlusion and optic nerve ischemia, which can lead to severe progressive vision loss.3 Secondary to ischemia, neovascularization of the retina and optic disc may occur, potentially yielding vitreous hemorrhage and arteriovenous anastomosis.1,2
If detected, peripheral retinal neovascularization should be treated with panretinal photocoagulation.1,2 Static talc emboli do not require treatment. Cessation of drug use and counselling are the best therapy.
This patient sought therapy and enrolled in a 10-step program. Currently, he is drug free. His eyes have not developed any treatable sequellae.
Additionally, we provided an updated near vision spectacle prescription to improve his visual blur while reading.
Thanks to David Lai, BSc, of Philadelphia for contributing to this case.
1. Abbasi O, Tewari A. Common medications that may be toxic to the retina. Available at:
www.reviewofophthalmology.com/content/d/retina/c/22893/ . Accessed November 5, 2014.
2. Schoenberger SD, Agarwal A. Talc Retinopathy. N Engl J Med.
2013;368(9):852.
3. Tran KH, Ilsen PF. Peripheral retinal neovascularization in talc retinopathy. Optometry.
2007;78(8):409-14.
4. Zoumalan CI, Marmor MF. Revisiting talc retinopathy. Arch Ophthalmol. 2007;125(7):988.