 For most of us, when we hear the term dry eye, we picture a
“65-plus” postmenopausal female patient. Even though dry eye is most prevalent
in this population, there are other populations to consider, too.
For most of us, when we hear the term dry eye, we picture a
“65-plus” postmenopausal female patient. Even though dry eye is most prevalent
in this population, there are other populations to consider, too.
In the pediatric population, dry eye appears much less frequently in general practice. But, it should be taken seriously when it comes to the implications of the patient’s ocular signs and symptoms. Little data is available on the prevalence of dry eye in the population under age 18, but dry eye is known to occur in children due to a variety of causes.
 |
| Frequent blinking, eye rubbing, tendency to shy away from light, or general ocular redness, grittiness or foreign body sensation can all suggest dry eye in kids. |
Underlying Causes of Dryness
Systemic conditions associated with dry eye include inflammatory, congenital, nutritional and endocrinologic origins.
• Inflammatory causes. Dry eye in children with diminished tear production can be caused by inflammatory conditions including Sjögren’s syndrome, graft-versus-host disease (GVHD) and juvenile rheumatoid arthritis. In a retrospective study of 14 patients under 18 years of age with dry eye, two cases involved patients whose dry eye manifested due to primary Sjögren’s, and two cases involved patients who were diagnosed with GVHD after bone marrow transplantation.1 Although Sjögren’s is most common among women in the fifth decade of life, reports suggest that disease onset can occur as early as five years of age and that it may be underdiagnosed in pediatric populations.2,3 Sjögren’s syndrome is characterized by lymphocytic infiltration of exocrine glands, so xerostomia (dry mouth) generally accompanies dry eye in patients with the disease, as well as potential association with other connective tissue diseases (in secondary Sjögren’s).2 Dry eye can also be associated with juvenile rheumatoid arthritis (JRA). In one study of 64 children diagnosed with JRA between the ages of 8 and 12, 1.5% were found to have probable diagnoses of dry eye, and 10.9% and were determined to have definite diagnoses.4 Additionally, among children with JRA, both males and those participants with a longer duration of disease were determined to be more likely to have decreased basal tear secretion and tear film stability than others.
• Congenital disorders. Congenital disorders can also cause dry eye in children. Familial dysautonomia, a condition that occurs almost exclusively among people of Ashkenazi Jewish descent (roughly one in 3,600 people in this population have the disease), affects the autonomic nervous system.5 Patients with familial dysautonomia (also known as Riley-Day syndrome) exhibit alacrima (deficiency or absence of tear production) and corneal hypoesthesthia—conditions that typically involve decreased blinking frequency and decreased sensitivity to corneal trauma, which can lead to epithelial erosions. Particularly in this disease, ocular signs and symptoms tend to manifest prior to systemic effects (e.g., progressive impairment of motor, sensory and peripheral functions), so be certain to question parents about any family history of the disease.1,5 Patients can also present with signs and symptoms of dry eye if they have alacrima alone, Allgrove syndrome (or “triple-A,” a rare autosomal disease exhibiting alacrima, achalasia—a disorder of esophageal function that leads to difficulty swallowing—and adrenal deficiency), cystic fibrosis (which affects all secretory epithelia) or ectodermal dysplasia syndromes.6
• Poor nutrition. The lack of proper nutrition can also influence dry eye. Undernutrition, a significant problem especially in developing parts of the world, can lead to vitamin A deficiency, which can also be caused by diets low in animal sources providing vitamin A, diets low in iron, cystic fibrosis, and other causes of malabsorption syndrome. Children with vitamin A deficiency can also exhibit clinical signs and symptoms of dry eye disease. Approximately 250,000 to 500,000 vitamin A-deficient children worldwide become blind each year (and half of them die within 12 months of blindness), so efficient diagnosis of the deficiency is crucial.7
• Diabetes. Demonstrated to be a significant risk factor in the overall dry eye population, diabetes is yet another possible cause of dry eye in children. One in every 400 to 600 people under the age of 20 years is estimated to have type 1 diabetes.8 Although type 2 diabetes is clinically rare in children, clinical reports and regional studies suggest that it is being diagnosed more frequently in youth. One study of 104 children with type 1 diabetes found that 15.4% reported dry eye symptoms compared with 1.9% of 104 age- and sex-matched controls.9 Clinical signs of dry eye were observed in 7.7% of children with type 1 diabetes vs. less than 1% of children in the control group.
Other causes of dry eye in children include systemic medications, environmental factors, and ocular causes. Systemic antihistamines can decrease tear production due to their antimuscarinic activity.10 Retinoids for acne vulgaris are theorized to cause adverse effects of ocular dryness by decreasing lipid production.11 Environmental factors—including exposure to low humidity, exposure to urban pollutants, and significant time spent performing visual tasks—can adversely impact tear film stability.6,12,13 Blink rate during video game usage has been observed to decrease to nearly one-quarter of normal resting blink rate.14 The average American child (age 17 and younger) is estimated to spend seven hours playing video games every week, which could suggest diminished ocular surface protection. Borderline dry eyes may become symptomatic with contact lens wear, and approximately 50% of people begin to wear contacts under age 18—another potential cause of dryness in children and adolescents.15
|
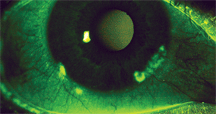
| Ocular surface staining with liquid fluorescein or lissamine green administered via a pipette (as opposed to a strip) makes dry eye assessment easier for young patients. |
Diagnosis of dry eye in any patient can be challenging due to the multifarious causes and manifestations of the disease. Diagnosing dry eye in children can be especially challenging due to their potential difficulty articulating their symptoms. Well-tuned and efficient diagnosis in these cases is very important, considering the possibility that this is the first medical notice of what could be a systemic disease.
In order to carefully examine the potential underlying root of the case, it is first important to capture a thorough medical history. Family history of diseases known to contribute to dry eye, systemic medication usage, and discussion of ocular and systemic symptoms can lend significant insight. The patient could complain about itchy, red eyes, for example, which might suggest ocular allergy. Patient or parent accounts of frequent blinking, the child rubbing his or her eyes often, tendency to shy away from light, or general ocular redness, grittiness or foreign body sensation can all suggest dry eye. Systemic symptoms can give the practitioner a glimpse into what, if any, systemic involvement is present. Patient complaints of dry mouth in addition to dry eye, for example, should trigger investigation into Sjögren’s syndrome. This can be confirmed using anti-Ro and anti-La serum testing. When the medical history suggests dry eye, the clinician should perform an array of tests for clinical signs of the disease.
Typical dry eye assessments include ocular surface staining, tear film break-up time (TFBUT) assessment, blink rate assessment, and calculation of the Ocular Protection Index (OPI). The OPI, which translates to average ocular surface protection, is easily calculated by dividing TFBUT by inter-blink interval (an OPI less than 1.0 exhibits insufficient protection and an OPI of 1.0 or more demonstrates sufficient levels of protection).16
Diagnostic approaches—such as tear meniscus height assessed through the slit lamp, phenol red threads (or Schirmer’s test with anesthetic) to assess tear production, and ocular surface staining observation using liquid fluorescein or lissamine green administered via a pipette (as opposed to the commonly-used strip)—can all make dry eye assessment easier for the young patient. If a systemic cause is suspected at the end of testing, referral to a specialist may be warranted. If the patient experiences mild symptomatology and displays lesser severity in clinical signs, then consider asking about the frequency of video display use (e.g., gaming or computer use), extended close work (e.g., reading, studying, etc), and exposure to adverse environmental conditions.
Replenishing the Moisture
If a systemic cause has been determined, ideally it should first be treated systemically. For instance, if the use of oral antihistamines causes the dryness, the patient could potentially benefit from switching to the use of a topical ocular antihistamine. For treatment of ocular manifestations of systemic diseases, refer the patient to the appropriate specialist and then to follow up in order to treat any residual ocular dryness. If over-activity of computer use or gaming seems to be the problem, behavior adjustment may be necessary, along with patient and family education about the importance of awareness of blinking frequency, which could improve the patient’s situation tremendously.
Often, the patient can be treated with artificial tears to lubricate the ocular surface in conjunction with systemic treatment of the underlying cause, or as primary treatment for external causes. These tears are often chosen from the large variety available, including formulations incorporating lubricants, osmo-protectors, mucomimetics and lipid replacements. Several of these formulations are scientifically designed to have improved interaction with the tear film. The use of lubricant eye drops as prophylaxis for extended periods of visual tasking could be a good recommendation for those patients who experience ocular dryness symptoms frequently while performing these tasks, or for patients with already-compromised ocular surfaces who anticipate video display terminal use. Research recently demonstrated enhanced visual function ability 90 minutes post-instillation of an ocular lubricant.17
Ophthalmic preservatives can also be an important factor in deciding the appropriate formulation. Cytotoxicity can be a concern with repeated dosing of preserved solutions, as might be the case in severe forms of dry eye (e.g., due to Riley-Day syndrome).18 So, non-preserved artificial tears can be beneficial for those patients requiring frequent or prolonged dosing.
Precautions and Prevention
Dry eye in youths may require treatments used in adult dry eye cases, but take care to consider potential for side effects when choosing specific medications in this age population. Topical corticosteroid use in young patients, for example, has demonstrated cases of glaucoma and subcapsular cataracts.19 Avoid systemic tetracyclines in patients younger than age 9 due to reports of interrupted tooth and bone development.6
When treating with tetracyclines, advise patients and/or their parents of the risk of sunburn and potential interaction with concomitant medications (e.g., oral contraceptives). Additional consideration, especially in young children, should also address compliance issues, including frequency of dosing and the potential necessity of school-day dosing. The school nurse can be an invaluable asset for situations involving school-age children. By sending an order and reviewing it with the nurse, or by writing separate prescriptions for the school nurse, you can better ensure proper administration during the school day.
As patients reach their teenage years, it’s great to empower them to take charge of their own treatment by emphasizing habitual dosing around everyday occurrences (e.g., breakfast, lunch, dinner and bedtime). This timing strategy can also work well for home care in younger patients. Additionally, patients and their families should be educated on environmental hazards to the ocular condition and ways to avoid further ocular surface damage external to their underlying cause (e.g., use of polycarbonate eyeglasses or sunglasses as protection against wind and sun).
In short, don’t neglect to diagnose this uncommon but troublesome condition in children. If you can be proactive in efforts to identify these signs and symptoms, you’ll provide preventative measures to tomorrow’s dry eye population.
Dr. Pietrantonio is director of eye services at East Boston Neighborhood Health Center and adjunct clinical faculty at the New England College of Optometry.
1. Mac Cord Medina F, Silvestre de Castro R, Leite SC, et al. Management of dry eye related to systemic diseases in childhood and longterm follow-up. Acta Ophthalmol Scand. 2007 Nov;85(7):739-44.
2. Chudwin DS, Daniels TE, Wara DW, et al. Spectrum of Sjögren syndrome in children. J Pediatr. 1981 Feb;98(2):213-7.
3. Stiller M, Golder W, Döring E, Biedermann T. Primary and secondary Sjögren’s syndrome in children—a comparative study. Clin Oral Investig. 2000 Sep;4(3):176-82.
4. Akinci A, Cakar N, Uncu N, et al. Keratoconjunctivitis sicca in juvenile rheumatoid arthritis. Cornea. 2007 Sep;26(8):941-4.
5. Barankin B, Metelitsa AI, Schloss EH, Wasel NR. Skin disorders in Ashkenazi Jews: a review. Int J Dermatol. 2005 Aug;44(8):630-5.
6. Alves M, Dias AC, Rocha EM. Dry eye in childhood: epidemiological and clinical aspects. Ocul Surf. 2008 Jan;6(1):44-51.
7. World Health Organization. Micronutrient deficiencies. Available at: www.who.int/nutrition/topics/vad/en (accessed November 13, 2008).
8. American Diabetes Association. Total prevalence of diabetes & pre-diabetes. Available at: www.diabetes.org/diabetes-statistics/prevalence.jsp (accessed November 13, 2008).
9. Akinci A, Cetinkaya E, Aycan Z. Dry eye syndrome in diabetic children. Eur J Ophthalmol. 2007 Nov-Dec;17(6):873-8.
10. Welch D, Ousler GW, Nally L, et al. Ocular drying associated with oral antihistamines (loratadine) in the normal population—an evaluation of exaggerated dose effect. In: Sullivan DA, Stern ME, Tsubota K, et al (eds). Lacrimal Gland, Tear Film, and Dry Eye Syndromes 3. New York: Kluwer Academic/Plenum Publishers; 2002:1051-5.
11. Lebowitz MA, Berson DS. Ocular effects of oral retinoids. J Am Acad Dermatol. 1988 Jul;19(1 Pt 2):209-11.
12. Ousler GW, Gomes PJ, Crampton HJ, Abelson MB. The effects of a lubricant eye drop on the signs and symptoms of computer vision syndrome (CVS) exacerbated in a controlled adverse environment. Invest Ophthalmol Vis Sci. 1999 Mar;40(4-ARVO Suppl):B722.
13. Abelson MB, Leung S, Maffei C. Breaking the barrier: allergy, dry eye and contact lenses. Rev Cornea Contact Lenses. 2008 Mar;144(2):15-18.
14. Tsubota K, Miyake M, Matsumoto Y, Shintani M. Visual protective sheet can increase blink rate while playing a hand-held video game. Am J Ophthalmol. 2002 May;133(5):704-5.
15. Iribarren R, Cerrella MR, Armesto A, et al. Age of lens use onset in a myopic sample of office-workers. Curr Eye Res. 2004 Mar;28(3):175-80.
16. Ousler GW III, Hagberg KW, Schindelar M, et al. The Ocular Protection Index. Cornea. 2008 Jun;27(5):509-13.
17. Torkildsen G, Christensen A, Martin AE, et al. Evaluation of functional visual performance using the IVAD method with currently marketed artificial tear products. Invest Ophthalmol Vis Sci. 2009;50:E-abstract 4649.
18. Ayaki M, Yaguchi S, Iwasawa A, Koide R. Cytotoxicity of ophthalmic solutions with and without preservatives to human corneal endothelial cells, epithelial cells and conjunctival epithelial cells. Clin Exp Ophthalmol. 2008 Aug;36(6):553-9.
19. Thadani SM, Foster CS. Treatment of ocular inflammation in children. Paediatr Drugs. 2004;6(5):289-301.

