In recent times, we have seen the emergence of serious ocular infections and resultant contact lens solution recalls. These recalls have had a tremendous impact on our solution paradigms. Products once considered a “safe” recommendation are now carefully studied and reviewed before making it to store shelves or doctors’ offices. The process behind solutions’ approval and how they meet safety standards is complex, although necessary to understand to have a true grasp on what is best for the patient. Mere recommendations aren’t enough anymore.
As optometrists, we need to comprehend solution efficacy, what to prescribe for contact lens care and why. Let’s take a closer look at what components make up contact lens solutions, what to consider when pairing them with lens materials, and why it’s important to prescribe solutions vs. making a recommendation.
Science Behind the Solution
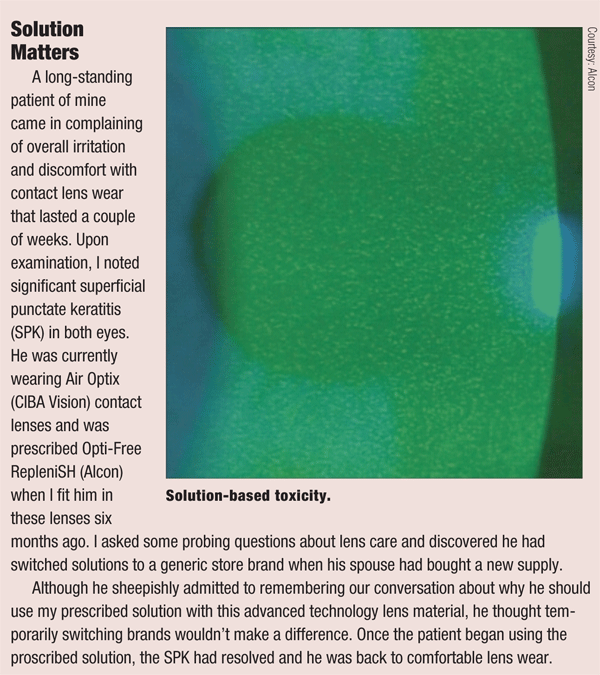
Today’s multipurpose contact lens solutions (MPS) are comprised of cleaners/surfactants that maintain a clean, wettable surface, as well as antibiotic preservatives and buffers.1 Lubricants or wetting agents are also needed in these solutions to decrease the wetting angle and make the lens more comfortable for patients to wear.
It’s been inferred that the preservatives were the culprits in some solution recalls because they have varying molecular weights. These changes in weight have caused interactions with newer lens materials, and possibly decreased disinfection efficacy. Wetting agents have been suspected to harbor opportunistic microbes in non-compliant patient conditions as well.
These mainstays of contact lens care systems have met—with mixed results—the challenge of cleaning and disinfecting the newest contact lens material: silicone hydrogel. Several studies have reported increased incidence of corneal staining associated with various care systems in combination with silicone hydrogel materials.2-5 What this staining means clinically has been somewhat unclear, however, and continues to be under investigation.
Several MPS systems have been reformulated in an attempt to improve their compatibility with these newest lens materials and to decrease the potential of staining and infectious complications. Wetting of these lenses has proved to be the biggest challenge, and reformulated solutions were aiming to create a moisturized lens for the patient. But, adverse events with Fusarium and Acanthamoeba keratitis have resulted in a couple of these solutions being pulled from the market.6
In contrast, hydrogen peroxide systems have resulted in low amounts of corneal staining compared to some MPS systems. Although potentially not as convenient or economical to use as MPS systems, the proportion of market share has risen in recent times and this form of disinfection has shown to be a viable option for patient lens care.7
Hydrogen peroxide solution systems work by penetrating the matrix and oxidizing microbes. Their chemistry enables further breakdown of protein and lipid bonds.1 Another advantage is their ability to penetrate microbial biofilms, which most MPS systems have difficulty accomplishing. Hydrogen peroxide systems are also preservative-free, although the solution needs to be neutralized before placing lenses on the eyes.
The Solution Evolution
The solution issues of the recent past involved many variables, the biggest and most unpredictable of which was the patient. Convenience was a large factor in marketing within the last 10 years, and the no-rub indication was a significant part of that push. One cannot deny the testing, which showed that the no-rub regimen did actually work but only if followed precisely.2 Unfortunately, many patients seemed unable to adhere to the copious amounts of solution needed to not have to rub the lenses, in order to keep them disinfected and clean.
The convenience of no-rub has certainly come back to haunt us, even if not directly. Patients’ cavalier attitude toward contact lens care was certainly at the root of our solution recalls. Bausch + Lomb recognized this when ReNu with Moisture Loc was fully studied status post recall.8 The company acknowledged that polymers in this particular lens solution formulation easily formed microbial films under certain conditions that resulted from poor patient compliance. These included topping off the solution, not replacing the lens case regularly and not closing the bottle top between uses.8
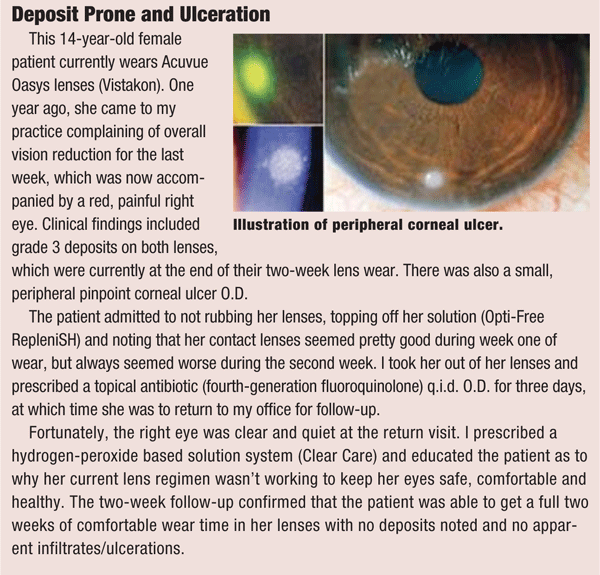
When patients were surveyed about such habits, many doctors were surprised at how few are honestly compliant with hygiene instruction.8 Many patients admitted to not rubbing contact lenses when cleaning them—even if directed—and/or topping off old solution with new solution when storing lenses. Shortcuts and ways to “save” solution or extend contact lens wear are common, even among our best patients.
Contact lenses are medical devices, and patients need to be consistently reminded of that. Many patients with poor care habits are fortunate to never deal with ocular morbidities. This is due, in large part, to the extensive FDA approval process for any solution on the market today.
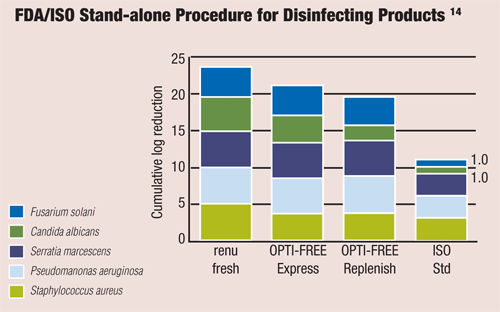
The FDA and International Organization for Standardization (ISO) have developed performance criteria by which contact lens solutions are measured.9 The ability to reduce the numbers of standard “challenge” organisms is evaluated. The decrease is measured by log reductions; one-log reduction means 90% of the organism is reduced, which is the standard for fungi. Bacteria, such as Staph, must be reduced by a 3-log reduction, or 99.9%.10,11 Acanthamoeba reduction by a contact lens solution does not currently have any FDA performance standards, which is interesting in light of current solution issues. At this time, hydrogen peroxide solution systems seem to have the best disinfection capability in this arena.12
What many clinicians do not often realize is that these tests are conducted in vitro. What happens once you introduce a contact lens? The answer to that question lies not only in looking to our past mistakes, but also continuing to demand safe and effective solutions for our patients now and in the future.
Today’s Contact Lens Technology
With the rise of silicone hydrogel technology, it is clear that solution performance is compatible with contact lens materials, and not the other way around. So, which pairings work best for our patients?
As mentioned previously, wettability is the biggest obstacle to successful contact lens wear in newer-technology materials. Researchers in one recent study set out to explore surface wettability of silicone hydrogel materials.13 What they found was that various silicone hydrogel materials had large differences in wetting properties when taken directly from the lens pack. Surface modifications of these lenses have helped improve wettability, but at what cost to solution disinfection capabilities?
A study that compared the performance of traditional MPS systems vs. hydrogen peroxide systems in cleaning and disinfecting silicone hydrogel materials found that both options are viable.6 In this study, Opti-Free RepleniSH (Alcon) and Clear Care (CIBA Vision) were compared using the silicone hydrogel materials. Researchers gathered both clinical and subjective data from patients, and the results imply that Clear Care could provide longer wear times than the other MPS system. However, another investigation shows that it really might depend on lens type, and that Opti-Free can improve wettability in several silicone hydrogel/Opti-Free combinations.13 The solid conclusion is that further research is needed to determine what solution is best for particular silicone hydrogel contact lenses.
The world of contact lens technology and the accompanying care systems is dynamic and ever changing. Fortunately, that usually means patients and practitioners benefit alike in terms of performance and overall satisfaction. However, with new technology come new precautions, and it may take time to work out the particulars of the reasons behind the necessary care steps. It is our job as primary eye care providers to stay abreast of recent findings and tests, so we can make clinically sound, evidence-based decisions and recommendations to each and every patient in the exam room chair.
Dr. Wesley practices in Medina, Minn., where she focuses on primary eye care optometry with an emphasis on contact lenses. She is a fellow of the American Academy of Optometry and was recently awarded the 2011 Minnesota Young Optometrist of the Year award. Dr. Wesley is a consulting lecturer and research investigator for Alcon.
1. Gromacki S. Hydrogel and Silicone Hydrogel Lens Care. Available at:
www.visioncareeducation.com/no-feece/course1.asp. (Accessed March 2011).
2. Garofalo RJ, Dassanayake N, Carey C, et al. Corneal staining and subjective symptoms with multipurpose solutions as a function of time. Eye Contact Lens. 2005 Jul;31(4):166-74.
3. Jones L, MacDougall N, Sorbara LG. Asymptomatic corneal staining associated with the use of balafilcon silicone hydrogel contact lenses disinfected with a polyaminopropyl biguanide preserved care regimen. Optom Vis Sci. 2002 Dec;79(12):753-61.
4. Carnt N, Jalbert I, Stretton S, Naduvilath T, Papas E. Solution toxicity in soft contact lens daily wear associated with corneal inflammation. Optom Vis Sci. 2007 Apr;84(4):309-15.
5. Andrasko G, Ryen K. Corneal staining and comfort observed with traditional and silicone hydrogel lenses and multipurpose solution combinations. Optometry. 2008 Aug;79(8):444-54.
6. Keir N, Woods CA, Dumbleton K, Jones L. Clinical performance of different care systems with silicone hydrogel contact lenses. Cont Lens Anterior Eye. 2010 Aug;33(4):189-95.
7. Efron N. Morgan PB. Soft contact lens care regimens in the UK. Cont Lens Anterior Eye. 2008 Dec;31(6):283-4.
8. Bausch & Lomb Recalls Contact Lens Solution. June 2006. Available at:
www.aoa.org/x5080.xml. (Accessed March 2010).
9. Karpecki P, Schechtman D. Microbial Threats in CL Wear. Rev Optom. 2010 December;12(147):14-5.
10. FDA/CDRH website. Premarket Notaification FDA (510{k}). Guidance Document for Contact Lens Care Products. Available at:
www.fda.gov/downloads/MedicalDevices/DeviceRegulationandGuidance/GuidanceDocuments/UCM080218.pdf (Accessed February 2011).
11. International Standards Organization ISO 14729. Ophthalmic Optics – Contact Lens Care Products. Microbiological requirements and test methods for products and regimens for hygienic management of contact lenses, 2001.
12. Johnston SP, Sriram R, Qvarnstrom Y, et al. Resistance of Acanthamoeba cysts to disinfection in multiple contact lens solutions. J Clin Microbiol. 2009 Jul;47(7):2040-5.
13. Ketelson H, Meadows D, McQueen N, Stone R. Wettability of silicone hydrogel lenses in the presence of tear components. RCCL. April 2005;3(142):24-8.
14. Testing MPS Lens Care Solutions Against Staphylococcus aureus. Available at:
www.clspectrum.com/article.aspx?article=13228. (Accessed February 2011).

