In our December 2010 column (“Could Less Be More?”), we discussed the issue of pharmaceutical companies decreasing the concentrations of select medications while maintaining similar clinical efficacy.
To continue with the “less is more” theme, we want to discuss how occasionally the best therapeutic intervention is minimal therapeutic intervention. That is, sometimes we should simply stop at basic first aid.
Something ‘Screwy’
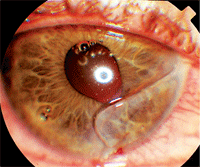
Here, you can see our 21-year-old patient’s full-thickness laceration with corectopia and several air bubbles in the anterior chamber.
One patient exemplifies this concept. He was a 21-year-old plumber who called us and reported that he had a “mishap” while working. He said that he was trying to hammer something with a screwdriver and accidentally hit himself in the left eye with the screwdriver’s blunt end.
He reported that he initially had major pain, but had taken some Tylenol (acetaminophen, McNeil) and the pain subsided significantly over the course of an hour. He also reported that he felt a lot of fluid running down his cheek. Additionally, he reported that it felt like he had cut his eye and was unsuccessfully trying to remove a loose flap of “skin”.
We instructed the patient to stop manipulating his injured tissue and come in immediately.
His corrected entering acuity was 20/20 O.D. and 20/100 O.S. Biomicroscopically, his external eye was injected and inflamed. Inspection revealed a full-thickness corneal laceration and a completely flat anterior chamber. There was corectopia, but no uveal extrusion through the wound. Seidel’s test was not performed because air bubbles in the otherwise flat anterior chamber removed any doubt that this was a full-thickness laceration.
In a trauma triage such as this, there is the temptation to do what we know best: apply antibiotics to reduce infection risk, use NSAIDs to alleviate corneal pain, apply a bandage to protect the globe, evert the eyelids to inspect for further damage, use topical steroids to reduce inflammation and perform a dilated fundus exam to assess for additional ocular compromise.
However, in this case, all of the above would likely just worsen the existing condition and perhaps cause irreparable damage. When dealing with a corneal laceration, always remember that less is more.
What is a Corneal Laceration?
Typically, the injury comes from a metallic instrument, such as a hand tool or similar object. However, there are myriad possible traumas that could potentially result in a corneal laceration, with some insults seeming rather mild.1-9 While not common, even a human fingernail can lacerate a cornea.
The initial presenting symptom is intense pain. This pain often diminishes when corneal desensitization sets in secondary to nerve damage. In this man’s case, the injury lacerated his corneal nerves. The corneal hypoaesthesia coincided with his Tylenol use.
A full-thickness laceration is termed a penetrating injury. In full-thickness non-sealing lacerations, there will be a flat chamber. Seidel’s sign will be present––as fluorescein is added, aqueous diffuses out from the wound amid the fluorescein. Damage to the iris may result in an irregularly shaped, unreactive pupil or even extrusion of uveal tissue.
Management: Less is More
The diagnosis of corneal laceration must be made as quickly as possible with as little intervention as possible. Additionally, a partial-thickness laceration must be differentiated from a full-thickness laceration with the use of Seidel’s test (unless the case is as obvious as the case presented here).
Avoid measuring the patient’s intraocular pressue when you suspect a full-thickness laceration because pressure applied to the globe may cause uveal tissue to extrude through the wound. Any other examination technique that involves pressure to the globe—such as gonioscopy, ocular ultrasonography or eyelid manipulation—should also be avoided.
Visual acuity should be measured, or at least attempted, if possible. Judicious use of a topical anesthetic (from a previously unopened bottle) will alleviate patient discomfort and allow you to make an appropriate diagnosis.
An eye with a full-thickness laceration should not be manipulated unnecessarily. Pressure patching of the eye is contraindicated. Soft contact lenses have been used successfully as bandages for patients with small corneal perforations.10,11 However, attempting to insert a lens in a blepharospastic patient may cause further damage, making this an option that should be exercised judiciously, if at all. An eye shield should be used for additional protection. (A simple Styrofoam cup can be taped over the eye if a shield is unavailable.)
Arrange for the corneal laceration to be surgically repaired by a specialist immediately. Instruct the patient to neither eat nor drink prior to the surgical consultation.
Patients with poor initial acuity, significant hyphema, uveal prolapse, lens damage, vitreous hemorrhage and larger size tend to have the poorest prognosis, often resulting in enucleation. Those without these factors may fare rather well following surgery.8
There are several surgical options for patients with corneal lacerations, including a number of suturing techniques that are capable of reapposing the corneal edges with a watertight bond.1-4,12 Viable alternatives to conventional sutures are various tissue adhesives and glues, along with amniotic membrane transplantation, which also can form a watertight bond while the cornea heals.13-19
In the plumber’s case, after instilling proparacaine (from a freshly opened bottle), we assessed the extent of his injury and did little else. We taped a Fox shield in place to protect the globe without adding any pressure to the eye. We arranged for the patient to be transported immediately to an anterior segment surgeon. He was told to neither eat nor drink until after the surgical consultation.
By the end of the evening, the laceration had been sutured, because it was too large to be glued. His final visual outcome was 20/30 O.S. in that eye.
1. Muller L, Kohnen T. Scleral and corneal laceration with iris prolapse caused by an eagle claw. Graefes Arch Clin Exp Ophthalmol. 2005 Apr;243(4):377-9.
2. Hamill MB. Corneal and scleral trauma. Ophthalmol Clin North Am. 2002 Jun;15(2):185-94.
3. Cosar CB, Rapuano CJ, Cohen EJ. Corneal laceration and intraocular foreign body in a post-LASIK eye. Cornea. 2002 Mar;21(2):234-6.
4. Jeng BH, Steinemann TL, Henry P, et al. Severe penetrating ocular injury from ninja stars in two children. Ophthalmic Surg Lasers. 2001 Jul-Aug;32(4):336-7.
5. Young AL, Cheng LL, Rao SK, et al. Corneal laceration with total but isolated aniridia caused by a pecking injury. J Cataract Refract Surg. 2000 Sep;26(9):1419-21.
6. Tsuda Y, Wakiyama H, Ameniya T. Ocular injury caused by an air bag for a driver wearing eyeglasses. Jpn J Ophthalmol. 1999 May-Jun;43(3):239-40.
7. Taneja S. Arora R, Yadava U. Fingernail trauma causing corneal laceration and intraocular cilia. Arch Ophthalmol. 1998 Apr;116(4):530-1.
8. Barr CC. Prognostic factors in corneoscleral lacerations. Arch Ophthalmol. 1983 Jun;101(6):919-24.
9. Alfaro DV 3rd, Jablon EP, Rodriguez Fontal M, et al. Fishing-related ocular trauma. Am J Ophthalmol. 2005 Mar;139(3):488-92.
10. Kanpolat A, Ucakhan OO. Therapeutic use of Focus Night & Day contact lenses. Cornea. 2003 Nov;22(8):726-34.
11. Lim L, Tan DT, Chan WK. Therapeutic use of Bausch & Lomb PureVision contact lenses. CLAO J. 2001 Oct;27(4):179-85.
12. Akkin C, Kayikcioglu O, Erakgun T. A novel suture technique in stellate corneal lacerations. Ophthalmic Surg Lasers. 2001 Sep-Oct;32(5):436-7.
13. Velazquez AJ, Carnahan MA, Kristinsson J, et al. New dendritic adhesives for sutureless ophthalmic surgical procedures: in vitro studies of corneal laceration repair. Arch Ophthalmol. 2004 Jun;122(6):867-70.
14. Skorpik C, Gnad HD, Paroussis P. Cyanoacrylate tissue gluing in corneal perforations. Wien Klin Wochenschr. 1986 May 2;98(9):276-9.
15. Chan SM, Boisjoly H. Advances in the use of adhesives in ophthalmology. Curr Opin Ophthalmol. 2004 Aug;15(4):305-10.
16. Alio JL, Mulet ME, Cotlear D, et al. Evaluation of a new bioadhesive copolymer (ADAL) to seal corneal incisions. Cornea. 2004 Mar;23(2):180-9.
17. Sharma A, Kaur R, Kumar S, et al. Fibrin glue versus N-butyl-2-cyanoacrylate in corneal perforations. Ophthalmology. 2003 Feb;110(2):291-8.
18. Duchesne B, Tahi H, Galand A. Use of human fibrin glue and amniotic membrane transplant in corneal perforation. Cornea. 2001 Mar;20(2):230-2.
19. Datta H, Sarkar K, Chatterjee PR. Amniotic membrane transplantation in ocular surface disorders. J Indian Med Assoc. 2004 Dec;102(12):726-9.

