 |
Q:
A 69-year-old recently presented with a bruised eyelid after taking a spill on the sidewalk. I normally just use a cold compress to treat discomfort and send them on their way. Is there anything else I should be doing?
A:
“While this looks like a straightforward case of ecchymosis, you can’t be dismissive,” says Joseph Sowka, OD, a professor of optometry at Nova Southeastern University College of Optometry. He says it’s crucial to thoroughly check the patient for rare instances when the situation is more complicated than it seems at first glance. “You need to do a full evaluation from the front to the back when recent trauma is involved. Though problems here are unlikely, check to ensure that the globe is intact, the anterior chamber is formed, and that there is neither cell nor flare present.”
Heed the following four-point plan in all cases of bruising, Dr. Sowka advises.
1. Listen for Crepitus
Dr. Sowka says that palpating the eyelid and periorbital region can help you identify whether the patient has experienced trauma significant enough to break bones. “As you palpate the eyelids, you are looking and listening for the telltale crackling of crepitus, which is air that has invaded the lid tissue. This indicates that an orbital wall has fractured.” Another tip:
“Test the skin sensation of the lower eyelid. Loss of sensation also indicates an orbital fracture and neuronal compromise,” says Dr. Sowka. And, if you suspect a break, X-ray or computed tomography (CT) is helpful to confirm the diagnosis.
2. Check the Retina
Dr. Sowka says that, in any case of blunt trauma to the eye and periorbital region, dilate and perform binocular indirect ophthalmoscopy to check for retinal tears and detachments. “It’s important to be sure that neither a tear nor a detachment has occurred, because the force from the injury may have disturbed the vitreous enough to make these complications possible.” Ultra-widefield imaging has its place, but this isn’t one of them. Commotio, peripheral breaks and retinal elevation have to be evaluated in stereo with the trained eye of the optometric clinician.
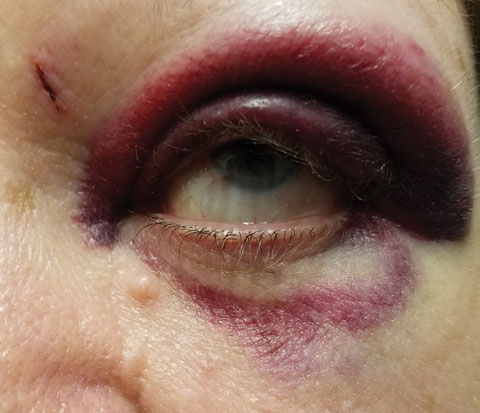 |
| As swollen and dramatic as this looked at onset, the problem resolved within a week after we ruled out damage to the eye itself. |
3. Watch for Symptoms of Emergent Cases
If altered mentation exists, or if the patient presents with a severe headache or somnolence, Dr. Sowka says it’s necessary to refer for an urgent CT. Further, he says to be aware of severe bruising. “If a patient received trauma to the eye substantial enough to cause severe ecchymosis, then they received enough trauma to induce a subarachnoid or other type of intracranial hemorrhage,” notes Dr. Sowka. “While we hate to send people to the ER unless absolutely necessary, it is difficult to get patients in to see an orbital specialist or neurologist at a moment’s notice. The ER can be the best entry point into the system, but be sure to send a detailed note along with the patient so that the physician knows why they are being sent in.”

