A recent survey of eye care practitioners revealed that nearly 50% of all patients seen by optometrists are diagnosed with blepharitis.1 Without question, it is one of the most common conditions encountered in any primary eye care practice. Despite its prevalence, however, there are several major shortcomings in the diagnosis and management of blepharitis.
Barriers to Effective Management

The symptoms associated with blepharitis—burning, itching, grittiness, soreness, intermittently blurred vision—are all quite nonspecific, and can overlap with those of a variety of related ocular surface disorders. These symptoms are commonly misattributed to other conditions, including dry eye, allergic eye disease and bacterial conjunctivitis to name a few.
And because today’s clinicians are frequently rushed, hasty decisions may be made without the benefit of a thorough ocular evaluation.
In short, some practitioners diagnose by the history and symptoms alone, without taking the time to look closely at the ocular structures (see, “Appropriate Management Requires Careful Categorization”). This is particularly true in the case of meibomian gland dysfunction (MGD); clinicians often admit their failure to regularly inspect and express the meibomian glands during the course of an examination, even when the symptoms dictate doing so.
The second major deterrent to effectively managing blepharitis is the fact that, even when the condition is properly diagnosed, clinicians may fail to prescribe appropriate, definitive therapy. All too often, doctors rely on their pre-printed “lid hygiene sheets” to address this group of disorders, the majority of which are woefully outdated or incomplete. Moreover, relying on patients to initiate and maintain behavioral changes, such as daily lid cleansing and massage, without explanation or reinforcement simply invites noncompliance.
Management Strategies
Proper therapy for blepharitis needs to consist of:
• Education, including the etiology, course, and prognosis of the condition.
• Aggressive short-term therapy, which often requires the use of topical therapeutic agents.
• Long-term maintenance therapy, to prevent recurrences.
• Behavior modification, such as lid hygiene techniques, to ensure a continually healthy and stable ocular environment.
In addition, blepharitis therapy must be “case-specific” for each patient, because the treatment options for an individual with mild seborrheic blepharitis are obviously not the same for a patient with advanced MGD.
Management strategies for any form of blepharitis need to be multifaceted; rarely will one simple technique or agent serve to completely address the signs and symptoms of these chronic disorders. A variety of modalities, including lubrication therapy, lid hygiene, topical medications and even oral medications, may be utilized.
Historically, optometrists tended to take a “least-invasive” to “most-invasive” approach, relying on over-the-counter options initially and reserving pharmaceutical agents for only the most extreme cases. Recent thinking and experience, however, suggest that this may not be the most effective way of managing the majority of patients.
Case Report
• History. A 50-year-old Hispanic male presented with complaints of irritated red eyes, which he had experienced for the past few months. He reported having crusty eyelids upon awaking every morning. He further claimed that he had been advised to use lid scrubs and artificial tears in the past, but this failed to alleviate his symptoms. His past ocular history as well as his medical history was unremarkable.
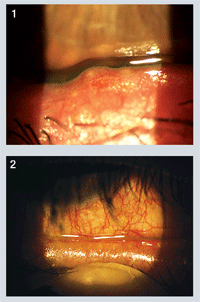
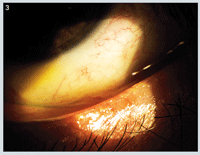
• Diagnostic Data. Upon examination, best-corrected visual acuity was 20/20 O.U. Biomicroscopic evaluation revealed bilateral conjunctival hyperemia with evidence of “frothy” tear debris both inferiorly and medially in both eyes. Tear film break-up time (TFBUT) was approximately three seconds in each eye. There was no evidence of corneal infiltration, although mild punctate epitheliopathy was present in both eyes. Lid evaluation revealed moderate crusting of the lashes at the base, as well as tylosis ciliaris (figure 1) and meibomian plugs with turbid secretions upon manual expression (figure 2).
• Discussion. Based upon the presentation and history, we diagnosed the patient with mixed blepharitis and associated ocular surface disease in both eyes. Therapy was initiated as follows: AzaSite (azithromycin 1% ophthalmic solution; Inspire Pharmaceuticals) b.i.d. for two days, followed by once daily for the next two weeks. We recommended Soothe XP lubricant eye drops (Baush + Lomb) for additional irritation, as needed. We further educated the patient regarding appropriate lid hygiene, including the daily use of warm compresses.
The patient returned two weeks later and reported great improvement of both signs and symptoms. He displayed marked improvement of the blepharitis as well as decreased conjunctival injection and normalization of the lid margin (figure 3).
Appropriate Management Requires Careful Categorization
Typically,
we recognize two broad categories of blepharitis: anterior and
posterior. Anterior blepharitis denotes those manifestations primarily
affecting the lashes and their associated pilosebaceous glands; this
category may be further divided into bacterial and seborrheic
categories. Posterior blepharitis deals with disorders of the meibomian
glands, modified sebaceous glands designed to produce the complex lipid
tear component. Subsequently, posterior blepharitis is often referred to
as meibomitis, or, more commonly, meibomian gland dysfunction (MGD).
Bacterial-associated
anterior blepharitis results from bacterial overgrowth—most commonly
Staphylococcus epidermidis and Staph. Aureus—along the eyelid margins
and lashes. Toxic bacterial products released into the tear film
stimulate the production and release of pro-inflammatory cytokines and
leads to recruitment of inflammatory cells, triggering host-induced as
well as organism-induced inflammation.2 Bacterial blepharitis may be
recognized by its inflamed, erythematous lid margins and dry, crusty
debris in the lashes, especially collarettes.
Seborrheic blepharitis
results from a dysfunction of the pilosebaceous glands, and may be
related to Malassezia furfur (previously referred to as Pityrosporum
ovale), a pathogenic yeast fungus that resides on or near hair
follicles.3 In seborrhea, the glands produce excessive sebum, resulting
in the accumulation of large, greasy scales along the hair shaft and
surrounding skin. Common sites include the eyebrows, glabella and
anterior scalp; in seborrheic blepharitis, these “dandruff-like” flakes
are evident along the lashes and lid margins. Lid erythema is usually
mild, except in extreme cases.
MGD is a condition marked by chronic
obstruction and inflammation of the meibomian glands. Clinical and
histopathic observations of subjects with MGD have revealed an abundance
of ductal occlusion due to hyperkeratinization of the ductal
epithelium, as well as a potential loss of glands in advanced
disease.4,5 Likewise, the meibomian lipid secretions in these
individuals are more saturated and contain less-branched chain
hydrocarbons and more protein.6 This change results in more ordered,
more viscous lipid secretions, which retard the flow and impede the
delivery of meibum to the lid margin. Stagnated meibum means that less
lipid is available to form the tear film, resulting in increased tear
evaporation and tear osmolarity.7,8
But, in addition to reduced tear
lipid production, MGD is also exacerbated by the presence of bacterial
lid flora, such as Propionibacterium acnes and Staph. epidermidis, which
seem to thrive in this environment.2 These bacteria secrete lipases,
which act directly on the meibum, initiate conversion of the lipids into
free fatty acids and soaps. These unwanted elements, in turn, cause
ocular surface irritation and further disrupt the tear film.8
The
glandular and meibum alterations that are evident in MGD typically occur
with increasing age, but may also be associated with several
dermatological conditions, particularly rosacea.9 Clinical
manifestations of MGD include poor stability of the tear film, which can
be marked by a rapid tear break up time and/or the presence of “foamy”
or “frothy” tears (representing saponification of the lipids). Punctate
keratopathy may also be noted, especially along the inferior one-third
of the cornea.
Inspection of the lid margin reveals inspissated gland
orifices at the gray line and cloudy, viscous or sometimes
toothpaste-like meibum upon digital expression of the glands. Long-term
complications of MGD can include recurrent hordeola, chalazia, and
ultimately, meibomian gland dropout.
Treatment Options
Let’s review the various treatment options and explore their clinical utility.
• Tear supplementation. One of the few universal treatments for ocular surface disease is the use of lubrication therapy, or as we more commonly refer to these products, “artificial tears.” Whether the condition results from aqueous deficiency or lid dysfunction, the end result is a compromised tear film and frictional damage to the ocular surface. Hence, it is critical to replenish that lost moisture and restore the barrier and lubrication effect to the tears. While some dismiss this therapy as merely transient, palliative relief, tear supplementation is, in fact, a crucial element to alleviating symptoms and restoring ocular surface integrity.
• Lid hygiene. Lid hygiene is considered by many practitioners to be the mainstay of blepharitis management, and indeed, it can be a crucial element in restoring and maintaining lid margin health. In most cases, lid hygiene consists of two elements: lid hyperthermia (a.k.a. warm compresses) and lid scrubs, which involve direct cleansing of the lid margins with a mild detergent.
Lid hyperthermia can be helpful in both anterior and posterior blepharitis. The direct application of heat (approximately 105°F to 110°F) to the lid margins helps to improve circulation in the lids and lower the viscosity of meibomian secretions, allowing them to flow more freely.10,11 In addition, heat helps to control bacterial overgrowth and dissolve crusty lid debris, making it easier to remove.
Lid scrubs are beneficial for patients with anterior blepharitis, because they remove the excess sebum and debris while further reducing excess bacterial colonization of the lid margins.
However, lid cleansing with baby shampoo or another detergent-based product can actually be counterproductive in MGD patients. These agents function in a similar fashion as bacterial lipases, breaking down residual, healthy meibum into free fatty acids and soaps, further compromising the lipid tear elements and increasing symptoms.11
Lid hygiene, either with or without lid scrubs, is usually recommended twice daily for the first two days, and then once daily in the evening for an additional 28 days thereafter.11
• Topical medications. Historically, the use of topical antibiotics in anterior blepharitis was reserved for only the most chronic and severe cases. Medications like bacitracin and erythromycin ointment were the drugs of choice, and it was not unusual for patients to use these medications three or four times daily.12 While these agents may have helped to address the bacterial component in blepharitis, they unfortunately offered little in the way of anti-inflammatory efficacy. Hence, many doctors turned to corticosteroid-antibiotic combinations for these severe cases, finding that the use of a concurrent steroid resulted in faster and greater degrees of improvement in the signs and symptoms of blepharitis.13,14
Unfortunately, the long-term effects of corticosteroids must always be weighed against the benefit of any chronic disease. Today, most experts recommend corticosteroids for short-term use only—usually two weeks or less—in an effort to “jump start” therapy for moderate-to-severe anterior blepharitis or blepharoconjunctivitis.
One of the more recent additions to the management of blepharitis is topical azithromycin (AzaSite, Inspire Pharmaceuticals). Despite that it is not specifically FDA-approved for the treatment of lid margin disease, AzaSite has rapidly become one of the most widely embraced topical medications for blepharitis therapy, particularly in optometry. While much of the support for this therapy comes from anecdotal tales of clinical success (see the case report on page 64), there are now several published studies that also show a distinct improvement in both signs and symptoms of blepharitis when treated with AzaSite.15-17
In addition to providing antimicrobial efficacy against the most common bacterial pathogens, azithromycin has been shown to effectively address inflammation by inhibiting the production of pro-inflammatory cytokines and matrix metalloproteinases (MMPs), in part by suppressing nuclear transcription factor kappa B (NF-KB).18,19 An in vitro study presented at ARVO in 2008 found topical azithromycin to be as effective as doxycycline in suppressing MMPs in human and bovine corneal tissue.20
Clinically, Gary Foulks, M.D., and associates demonstrated that the use of AzaSite for four weeks in patients with recalcitrant MGD resulted not only in improved signs and symptoms, but also in more ordered meibomian lipids and a subsequent alteration of phase transition temperature—in other words, a thinner, less viscous oil component with a lower melting point.17 Additional studies are ongoing, and Inspire is currently seeking an FDA-approved indication for AzaSite in the management of blepharitis.
• Oral medications and supplements. More chronic or severe cases of blepharitis, especially MGD, may warrant the use of essential fatty acid (EFA) supplements. EFAs, especially the omega-3 variety, tend to be deficient in the typical Western diet; however, these agents purportedly have the capacity to improve meibomian secretions by stimulating tear-specific anti-inflammatory prostaglandins.21 Typical dosing consists of 2g to 4g daily, although there are many varieties of these dietary supplements and patients should be advised to read all packaging directions and precautions. EFA supplements must be used with caution in those patients taking systemic anticoagulant or anti-platelet therapy (i.e., “blood thinners” such as aspirin, Coumadin [warfarin, Bristol-Myers Squibb] Plavix [clopidogrel bisulfate, Sanofi Aventis/Bristol-Myers Squibb] or Ticlid [ticlopidine, Roche]) because of a potential dose-related effect on bleeding time.22,23 Also, advise patients that increased urinary and/or bowel frequency can occur with these supplements, particularly at high doses or when first initiating therapy.
Oral tetracycline derivatives (e.g., doxycycline and minocycline) have also proven beneficial in cases of advanced MGD. It is believed that these drugs hinder the production of bacterial lipases, which serve to alter the consistency of the meibomian oils.24 Additionally, tetracyclines are recognized to be potent anti-inflammatory agents, inhibiting the expression of matrix metalloproteinases and other cytokines in a fashion similar to azithromycin.25,26 Therapeutic effects may be seen with as little as 40mg of doxycycline hyclate daily, although there is typically a delayed response––often taking up to six weeks––for patients to appreciate symptomatic improvement.27
They say that “familiarity breeds contempt,” and so it is true in clinical practice as well. Often, it is the most common conditions that end up getting the least of our attention. Blepharitis affects nearly half of our patients, yet it remains an underappreciated and undermanaged ocular disorder by many eye care providers. As such, it represents a tremendous area of opportunity and growth. Emerging research and unique new therapies have spurred a renewed interest in the various forms of blepharitis among ocular surface disease specialists. Hopefully, this raised awareness will ultimately result in better detection, management and control of this rampant problem.
Dr. Kabat is a contributing editor to Review of Optometry. He is a consultant for Alcon Laboratories and Inspire Pharmaceuticals. He has no direct financial interest in any of the products mentioned in this article. Dr. Shechtman is a contributing editor to Review of Optometry. She has no direct financial interest in any of the products mentioned in this article.
1. Lemp M, Nichols K. Blepharitis in the United States 2009: A survey-based perspective on prevalence and treatment. Ocul Surf. 2009 Apr;7(2 suppl):S1-14.
2. O’Brien TP. The role of bacteria in blepharitis. Ocul Surf. 2009 Apr;7(2 Suppl):S21-2.
3. Gupta AK, Bluhm R, Cooper EA, et al. Seborrheic dermatitis. Dermatol Clin. 2003 Jul;21(3):401-12.
4. Obata H. Anatomy and histopathology of human meibomian gland. Cornea. 2002 Oct;21(7 Suppl):S70-4.
5. Gutgesell VJ, Stern GA, Hood CI. Histopathology of meibomian gland dysfunction. Am J Ophthalmol. 1982 Sep;94(3):383-7.
6. Oshima Y, Sato H, Zaghloul A, et al. Characterization of human meibum lipid using Raman spectroscopy. Curr Eye Res. 2009;34:824–835.
7. Mathers WD, Shields WJ, Sachdev MS, et al. Meibomian gland dysfunction in chronic blepharitis. Cornea. 1991 Jul;10(4):277-85.
8. McCulley JP, Shine WE. Meibomian gland function and the tear lipid layer. Ocul Surf. 2003 Jul;1(3):97-106.
9. Foulks GN, Borchman D. Meibomian gland dysfunction: the past, present, and future. Eye Contact Lens. 2010 Sep;36(5):249-53.
10. Blackie CA, Solomon JD, Greiner JV, et al. Inner eyelid surface temperature as a function of warm compress methodology. Optom Vis Sci. 2008 Aug;85(8):675-83.
11. Donnenfeld ED, Mah FS, McDonald MB, et al. New considerations in the treatment of anterior and posterior blepharitis. Refractive Eyecare. 2008 Apr;12 Suppl:3-14.
12. Smolin G, Okumoto M. Staphylococcal blepharitis. Arch Ophthalmol. 1977 May;95(5):812-6.
13. Donshik P, Kulvin SM, Mckinley P, Skowron R. Treatment of chronic staphylococcal blepharoconjunctivitis with a new topical steroid anti-infective ophthalmic solution. Ann Ophthalmol. 1983 Feb;15(2):162-7.
14. Shulman DG, Sargent JB, Stewart RH, Mester U. Comparative evaluation of the short-term bactericidal potential of a steroid-antibiotic combination versus steroid in the treatment of chronic bacterial blepharitis and conjunctivitis. Eur J Ophthalmol. 1996 Oct-Dec;6(4):361-7.
15. Luchs J. Efficacy of topical azithromycin ophthalmic solution 1% in the treatment of posterior blepharitis. Adv Ther. 2008 Sep;25(9):858-70.
16. Haque RM, Torkildsen GL, Brubaker K, et al. Multicenter open-label study evaluating the efficacy of azithromycin ophthalmic solution 1% on the signs and symptoms of subjects with blepharitis. Cornea. 2010 Aug;29(8):871-7.
17. Foulks GN, Borchman D, Yappert M, et al. Topical azithromycin therapy for meibomian gland dysfunction: clinical response and lipid alterations. Cornea. 2010 Jul;29(7):781-8.
18. Abelson M, Protzko E, Shapiro A, et al. A randomized trial assessing the clinical efficacy and microbial eradication of 1% azithromycin ophthalmic solution vs tobramycin in adult and pediatric subjects with bacterial conjunctivitis. Clin Ophthalmol. 2007 Jun;1(2):177-82.
19. Ianaro A, Ialenti A, Maffia P, et al. Anti-inflammatory activity of macrolide antibiotics. J Pharmacol Exper Ther. 2000 Jan;292(1):156–163.
20. Jacot JL, Jacot TA, Sheppard JD, et al. Evaluation of MMP 2/9 modulation by AzaSite and DuraSite in human corneal epithelial cells and bovine corneal endothelial cells in vitro. Ft. Lauderdale, FL: Association for Research in Vision and Ophthalmology; 2008 Apr 28.
21. Pinna A, Piccinini P, Carta F. Effect of oral linoleic and gamma-linolenic acid on meibomian gland dysfunction. Cornea. 2007 Apr;26(3):260-4.
22. Covington MB. Omega-3 fatty acids. Am Fam Physician. 2004 Jul 1;70(1):133-40.
23. Jalili M, Dehpour AR. Extremely prolonged INR associated with warfarin in combination with both trazodone and omega-3 fatty acids. Arch Med Res. 2007 Nov;38(8):901-4.
24. Dougherty JM, McCulley JP, Silvany RE, Meyer DR. The role of tetracycline in chronic blepharitis. Inhibition of lipase production in staphylococci. Invest Ophthalmol Vis Sci. 1991 Oct;32(11):2970-5.
25. Ralph RA. Tetracyclines and the treatment of corneal stromal ulceration: a review. Cornea. 2000 May;19(3):274-7.
26. Stone DU, Chodosh J. Oral tetracyclines for ocular rosacea: An evidence based review of the literature. Cornea. 2004 Jan;23(1):106-9.
27. Yoo SE, Lee DC, Chang MH. The effect of low-dose doxycycline therapy in chronic meibomian gland dysfunction. Korean J Ophthalmol. 2005 Dec;19(4):258-63.

