 History
History
A 20-year-old black female presented for follow-up care after sustaining a blunt trauma injury to her right eye. The insult occurred approximately one month earlier.
A local hospital’s emergency room staff and ophthalmology department managed the initial acute trauma associated with the injury. However, she switched practitioners because our office was closer to her house.
The patient explained that she had exhausted her supply of eye drops––one with a “red cap” and one with a “white cap”––and that her right eye felt achy.
Except for the traumatic injury, she had no documented ocular history and reported no allergies.
Diagnostic Data
Her best-corrected visual acuity was 20/30 O.D. and 20/20 O.S. at both distance and near. Her extraocular muscle motilities were normal, with no evidence of diplopia. However, she reported mild photophobia and pain upon right eye movement.
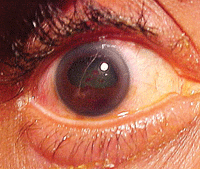
The right eye of our 20-year-old patient who suffered blunt trauma. What do you notice?
Confrontational fields were normal. There was no evidence of afferent pupillary defect; however, her right pupil had a pronounced “D shape.” Refraction improved her visual acuity to 20/25 O.D. and revealed the presence of mild myopia.
Biomicroscopic examination of the right eye uncovered grade 1 cell and flare with evidence of either old inflammatory synechia or impact pigmentation (Vossius’ ring) on the anterior lens capsule.
Intraocular pressure measured 19mm Hg O.U. The dilated fundus findings were normal O.U. The pertinent external/anterior segment findings O.D. are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? What’s the most likely prognosis?
Discussion
Additional tests/procedures included close inspection of the corneal endothelium to rule out the presence of significant, potentially visually debilitating keratic precipitate and residual corneal blood staining secondary to any hyphema caused by the original injury. Also, we performed gonioscopy with a Zeiss 4-mirror lens to record the angle’s status and rule out angle recession.
The diagnosis in this case is a smoldering traumatic iritis O.D. in the setting of a resultant traumatic iridodialysis.
Iridodialysis is defined as a rupture of the iris at its thinnest area––the root.1 Patients with iridodialysis present with a history of jarring, blunt-force trauma, such as being struck with a projectile or participation in a collision injury (e.g., the impact of an air bag or contact with the ground upon falling).2
Pain, photophobia and lacrimation associated with post-traumatic uveal inflammation (iritis or iridocyclitis), variable facial swelling secondary to fluid accumulation, pain upon eye movement and diplopia secondary to incidental correctopia are all common.3 In any suspected case of iridodialysis, the classic “D-shaped” pupil with the flat pupillary margin observed at the papillary margin located opposite the point of iris release is the telltale sign. Other associated collateral injuries may include subconjunctival hemorrhage, ruptured globe, corneal abrasion, conjunctival laceration, hyphema, angle recession, increased intraocular pressure (IOP), lenticular subluxation, orbital bone fracture, blow-out fracture, retinal detachment, vitreous hemorrhage, choroidal rupture and optic nerve evulsion.4-6
Upon direct contact with an object or secondary to a sudden acceleration or deceleration, energy is perpetuated inside the eye by a hydraulic shock wave.7,8 This wave travels through the ocular media, transferring sufficient forces to the “contrecoup region” (area located 180° or directly opposite the site of impact) to detach the iris at its thinnest and most vulnerable location. This peripheral anchor, which connects the iris to the ciliary body/muscle, is known as the iris root.8 As the tissue becomes freed, it creates an alternate, oval pupil that is confined by its points of attachment. The iris body located adjacent to the separation becomes flaccid, which creates a flat, tensionless border. These processes yields the classic, “D-shaped” pupil. Because the trabecular meshwork also is susceptible to the hydraulic effects of the shock wave, it too may incur damage, altering aqueous egress either acutely or on a delayed timeline.9,10 Cases of iridodialysis involving more than 180° pose a greater statistical risk for the late glaucomatous development.11
Because iridodialysis involves the traumatic (injurious or surgical) dissection of well-vascularized and innervated iris tissue, an accompanying inflammatory response (secondary iridocyclitis) and bleeding (hyphema) should be expected.12 Topical cycloplegics, such as atropine 1% dosed q.d. to t.i.d., can provide pain relief by mitigating the spasmodic response of both the iris and ciliary body as well as their effect on the sensory nerves that travel in the uveal tunic. Further, the aggressive use of topical steroidal and nonsteroidal anti-inflammatory preparations can be employed to reduce the incited immune response. If the patient experiences an acute IOP increase secondary to trabecular meshwork obstruction by blood or inflammatory debris (cells and flare), topical apraclonidine can be instilled in the office to initiate a rapid reduction in aqueous production. The serial use of topical brimonidine, a topical beta blocker or topical carbonic anhydrase medication may be used individually or in combination to lower IOP as the underlying injury heals.
Because the consequence of angle recession and late or post-traumatic glaucoma exists in all patients who sustain ocular blunt trauma, the entire angle in both eyes (for comparison) should be inspected with gonioscopy following the repair of and recovery from all acute sequellae.12 (Take note that gonioscopy always should be performed, irrespective of visible iris damage.) Further, in the absence of a treatable, acute, secondary open-angle glaucoma, patients with a history of ocular blunt-force trauma should be assessed periodically for rising IOP to exclude a delayed traumatic effect on aqueous drainage.9-12 Baseline fields and photographs also may be included in the database, and repeated as necessary. In the event that late or post-traumatic glaucoma becomes evident, it can be treated using the same algorithm as primary open-angle glaucoma.
Resolved iridodialyses that neither require surgical repair nor produce ill-cosmetic effects require no additional ophthalmic management. Patients who are upset by the shape of their pupils or the appearance of their irises, or are suffering from any secondary effects from an additional iris opening, may be fit with large-diameter, painted/opaque contact lenses.
Patients who require surgical remediation have two primary options:
- Microsurgical repair. A 22.0mm, plastic handled, 27-gauge straight needle through a 1.0mm distal hole can serve as a passage for 9-0mm or 10-0mm polypropylene or nylon sutures.13
- A “sutureless” technique. This includes use of a limbal peritomy, multiple sclerostomies to gain access to the iris base at multiple clock hours of the iridodialysis (with a microvitreoretinal blade), and placement/incarceration of the peripheral iris through these ports using a vitreoretinal forceps with conjunctival closure via absorbable sutures.13
The sutureless technique is suitable for use in simple iridodialysis repair in conjunction with other intraocular procedures.14 Surgical repair of this injury is not emergent and often is accomplished following the resolution of all resultant complications (e.g., conjunctival injury, iritis, hyphema, increased IOP).
We counseled our patient on the options for cosmetic intervention. We provided her with in-office cycloplegia only, instilling one drop of 5% homoatropine O.D. Further, she was placed on topical prednisolone acetate q.i.d. O.D. Because there was no evidence of hyphema or active ocular bleeding, we advised her to use 600mg ibuprofen t.i.d. after meals to help arrest the inflammation and achieve adequate analgesia.
She returned for her scheduled seven-day follow-up, and exhibited complete resolution. We discontinued the oral therapy and taped the topical treatment accordingly. We then scheduled the patient for a four-month follow-up to evaluate her IOP.
1. Oyster CW. The iris and pupil. In: Oyster CW. The human eye structure and function. Sunderland, Mass.: Sinauer Ass Inc.; 1999:411-46.
2. Lehto KS, Sulander PO, Tervo TM. Do motor vehicle airbags increase risk of ocular injuries in adults? Ophthalmology. 2003 Jun;110(6):1082-8.
3. García-Medina JJ, García-Medina M, Pinazo-Durán MD. Severe orbitopalpebral emphysema after nose blowing requiring emergency decompression. Eur J Ophthalmol. 2006 Mar-Apr;16(2):339-42.
4. Morris DS. Ocular blunt trauma: loss of sight from an ice hockey injury. Br J Sports Med. 2006 Mar;40(3):e5.
5. Vize CJ, Gauba V, Atkinson PL. Eye injury as a result of coat toggle trauma. Eye (Lond). 2007 Jan;21(1):94-5.
6. Wong MH, Yang M, Yeo KT. Elastic cord-related ocular injury. Singapore Med J. 2008 Apr;49(4):e90-2.
7. Oyster CW. The limbus and the anterior chamber. In: Oyster CW. The human eye structure and function. Sunderland, Mass.: Sinauer Ass Inc.; 1999:379-410.
8. Ahmad F, Kirkpatrick NA, Lyne J, et al. Buckling and hydraulic mechanisms in orbital blowout fractures: fact or fiction? J Craniofac Surg. 2006 May;17(3):438-41.
9. Ellong A, Ebana Mvogo C, Nyouma Moune E, et al. Post-traumatic glaucoma with irido-corneal angle injuries in Cameroon. Bull Soc Belge Ophtalmol. 2005;(298):21-8.
10. Manners T, Salmon JF, Barron A, et al. Trabeculectomy with mitomycin C in the treatment of post-traumatic angle recession glaucoma. Br J Ophthalmol. 2001 Feb;85(2):159-63.
11. Sihota R, Kumar S, Gupta V, et al. Early predictors of traumatic glaucoma after closed globe injury: trabecular pigmentation, widened angle recess, and higher baseline intraocular pressure. Arch Ophthalmol. 2008 Jul;126(7):921-6.
12. Walker NJ, Foster A, Apel AJ. Traumatic expulsive iridodialysis after small-incision sutureless cataract surgery. J Cataract Refract Surg. 2004 Oct;30(10):2223-4.
13. Bardak Y, Ozerturk Y, Durmus M, et al. Closed chamber iridodialysis repair using a needle with a distal hole. J Cataract Refract Surg. 2000 Feb;26(2):173-6.
14. Richards JC, Kennedy CJ. Sutureless technique for repair of traumatic iridodialysis. Ophthalmic Surg Lasers Imaging. 2006 Nov-Dec;37(6):508-10.

