 |
Anterior uveitis is a complicated and challenging disease. Anterior chamber inflammation may range from very rare cells in a trabeculitis to plasmoid aqueous with hypopyon. Some patients who have chronic iridocyclitis may be minimally symptomatic, while those with acute anterior uveitis may be in agony. We have seen IOP range from 3mm Hg to more than 85mm Hgso high that we could not measure it with conventional applanation tonometry.
Some anterior uveitis patients end up with an excellent visual outcome, while others lose vision and perhaps even develop blindness.1,2
Most of the anterior uveitis patients that we see clinically fall within this broad spectrum. However, any clinician who has managed patients who have anterior uveitis can relate a case involving an extreme situation.
Due to the vast clinical presentations of anterior uveitis, knowledge, skill and experience are needed to manage patients who have this disease. This month, we share our experience and philosophies on treating this disorder so that you can develop a flare for uveitis.
Signs and Symptoms
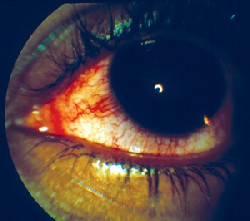
The typical presentation of anterior uveitis is pain, photophobia and hyperlacrimation. Patients report a deep, dull aching of the involved eye and surrounding orbit. Associated sensitivity to light may be severe. Visual acuity is variable, ranging from mild blur to significant vision loss if synechiae or a cyclitic membrane are present. A deep, perilimbal injection of the conjunctiva and episclera is typical. The hallmark sign of anterior uveitis: cells and flare in the anterior chamber.
 |
|
A deep, perilimbal injection of the conjunctiva and episclera is typical in anterior uveitis. |
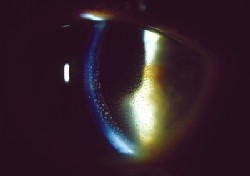 |
| In this case, keratic precipitates are seen. |
Treatment
Rapid control of inflammation is mandatory when managing acute anterior uveitis. If the attack is not broken early, a longer duration of therapy becomes necessary. To control inflammation, you must use the proper steroid and cycloplegic agent in the appropriate doses.
Clinically, the most potent topical steroid available is Pred Forte (prednisolone acetate 1%, Allergan). We typically insist on using this drug (and this drug alone), as we have had less success both with the generic versions and with other steroids when treating anterior uve-itis. A typical dosing at presentation is every 15 minutes for six hours, followed by hourly dosing while awake until follow-up examination (typically the next day but always within 72 hours). We dont prescribe steroid ointments for bedtime; rather we recommend that the patient instill one drop every minute for five minutes before retiring.
Through our clinical experience, we have found that diagnostic agents such as tropicamide or Cyclogel (cyclopentolate), do not provide adequate cycloplegia. Instead, we have found scopolmine 0.25% t.i.d. or atropine 1% b.i.d. to be more appropriate agents. Occasionally, homatropine 5% t.i.d. suffices in mild cases.
With appropriate therapy, each acute episode should last a maximum of six to eight weeks. Longer duration generally indicates that the initial therapy was insufficient.
|
Anterior Uveitis Treatment |
Even a cycloplegic agent as strong as atropine, however, may be insufficient to break posterior synechiae. Remember: A cycloplegic agent only paralyzes the iris sphincter muscle, and mydriasis occurs from unopposed action of the iris radial muscle. When fibrotic membranes form posterior synechiae, the action of the radial muscle may be insufficient to break the adhesion. In this case, a sympathomimetic drug, such as phenylephrine 10%, should be administered topically in your office at follow-up. This combination of steroid, cycloplegic and sympathomimetic typically breaks most cases of posterior synechiae.
We look for any degree of clinical improvement at the first follow-up visit. When the patient shows a response to the therapy, we reduce the steroid dosage to a therapeutic level of q2h while awake. Please note that we are not tapering the medication but changing to a new therapeutic dosage. We do not taper steroids until there are zero cells visible in the anterior chamber.
One frequent problem that we have seen in anterior uveitis management is premature tapering of steroids. Some doctors are uncomfortable treating patients with topical steroids for weeks. Even so, an uncomplicated case of acute anterior uveitis usually takes six to eight weeks to resolve, while other cases may take many months. We frequently see doctors note a reduction in the cell and flare response and thus begin a tapering dose. This invariably leads to a rebound increase in inflammation and necessitates starting treatment all over again. Only taper when there are no cells in the anterior chamber. If several episodes of recurrence occur with attempted steroid taper, employ NSAIDs (oral) with a slower steroid taper.
The goal of anterior uveitis management is threefold: No cells, no steroids (ie. ultimately being able to cease steroid treatment) and no complications. Allowing patients to limp along with 1+ cell and flare reaction eventually leads to vision loss. Chronic inflammation from under-treatment likely has a poor outcome. You must be aggressive early to give the patient the best chance of a good outcome.
Realize that some patients will never be cell free, and others may have unmanageable disease. Some patients may not respond to topical treatment and will progress through oral steroids and non-steroidal agents, injectable steroids, systemic immunosuppressants and even chemotherapy with an oncologist. However, early, aggressive therapy gives anterior uveitis patients the best chance of a good visual outcome.
1. Potter AR. Causes of blindness and visual handicap in the Central African Republic. Br J Ophthalmol 1991 Jun;75(6):326-8.
2. Zak M, Fledelius H, Pedersen FK. Ocular complications and visual outcome in juvenile chronic arthritis: a 25-year follow-up study. Acta Ophthalmol Scand 2003 Jun;81(3):211-5.

