 Q: I have a contact lens patient who has a corneal/conjunctival lesion that is quite raised and has a white appearance. How can I differentiate between pterygia, vascularized limbal keratitis (VLK) and conjunctival intraepithelial neoplasia (CIN)?
Q: I have a contact lens patient who has a corneal/conjunctival lesion that is quite raised and has a white appearance. How can I differentiate between pterygia, vascularized limbal keratitis (VLK) and conjunctival intraepithelial neoplasia (CIN)?
A: “The big issue is the nature of the lesion,” says J. James Thimons, OD, center director for Ophthalmic Consultants of Connecticut. “All three of these are best differentiated by the anatomy of the appearance and the location.” Let’s take a look at some of the defining features of each.
• Pterygia. Of the three conditions, this is by far the most common. “I tell my patients that a pterygium is effectively a callus on the eye, secondary to chronic exposure to sun, dust or wind,” Dr. Thimons says. It is almost always bilateral and not gelatinous. The vascular bed runs parallel with the wedge of the lesion, apexes toward the cornea, and weaves itself into the corneal epithelium and Bowman’s membrane.
In the case of a medium to large pterygium, you should perform topography to rule out induced distortion, according to Henry D. Perry, MD, a founding partner of Ophthalmic Consultants of Long Island. Histopathology shows a thickened epithelium, amorphous eosinophilic staining, hyalinized material and numerous vessels identified in the substansia propia. Stromal fibrocyte proliferation can also be seen.
“Several papers have reported as many as 10% of pterygia having foci of CIN—interestingly, none of these 10% were clinically recognized preoperatively,” Dr. Perry says. “Therefore, clinical photos are helpful, and performing a conjunctival scraping with a Kimura spatula and putting the material on a glass slide may be diagnostic.” Put the slide in a Coplin jar with methanol and send to a cytologist for evaluation.
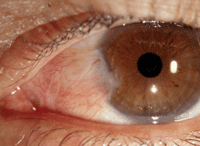
Pterygium, such as the one seen in this photo, is a common diagnosis. Photo: J. James Thimons, OD
• VLK. This condition is usually associated with hard contact lens wear and in patients with dryness or desiccation of the cornea secondary to lens fit dynamics. “It’s basically like a scab on the cornea—it’s thought to be a hyperplastic response of the cornea to try to heal itself,” Dr. Thimons says. It’s typically located between the limbus and the edge of the lens where it rides into the temporal cornea.
Usually smaller in size than a CIN, VLK does not have a whitish or gelatinous appearance. “This is clearly a corneal lesion with some limbal involvement,” Dr. Thimons says.
• CIN. Less common than pterygia or VLK, CIN tends to be more gelatinous with a bumpy texture and some gray-white pigment in the body of the lesion. “Any white lesion on the conjunctiva that looks suspicious for a neoplasm should be at least evaluated by serial photography and perhaps conjunctival scrapings,” Dr. Perry says. “Pinguecula that become elevated and/or develop a whitish, foamy appearance may actually represent CIN. Pterygia may also degenerate into CIN.”
Whereas most pterygia are nasal, CINs are typically temporal but can occur superiorly. Usually unilateral, CIN crops up more often in men, elderly patients and those with a history of chronic sun exposure or tobacco use. “Quite frankly, a CIN looks bad because it usually is,” Dr. Thimons says. “It’s one of those lesions that lives up to its reputation. Clinicians become concerned by the atypical aspect of the presentation and, as a result, either monitor regularly in the early phase or refer for biopsy and treatment if changes occur.”
“I would be uncomfortable with just a visual diagnosis; you would definitely want to biopsy,” he says. CIN is a pre-malignancy and can certainly progress to squamous cell CA when it breaks through the conjunctival basement membrane. If a CIN continues to grow, it can cause significant tissue damage and can invade adjacent structures, such as the sclera, lids and orbit. CIN can be aggressive, but very rarely metastasizes when it progressses to squamous cell CA.

