 Q: I have a patient with late-presenting dendriform after his primary-care physician diagnosed shingles, but hes experienced little to no pain. And, hes gotten worse since Ive increased his topical steroidthe whole cornea is covered with dendriform. What should I do?
Q: I have a patient with late-presenting dendriform after his primary-care physician diagnosed shingles, but hes experienced little to no pain. And, hes gotten worse since Ive increased his topical steroidthe whole cornea is covered with dendriform. What should I do?
A: Ensure the accuracy of the diagnosis. Pain isnt as significant a factor as presentation. More than half of patients affected by herpes zoster ophthalmicus (HZO) experience pain prior to the development of skin vesicles, but the diagnosis should not be based on the presence or absence of pain, which can vary from person to person, says Diane Calderon, O.D., of Nova Southeastern University College of Optometry.1,2 The rash that respects the vertical midline and follows one or more branches of the ophthalmic division of the trigeminal nerve is usually enough to diagnose HZO.
Examine the dendriform lesion closely, says J. James Thimons, O.D., of Ophthalmic Consultants of Long Island and
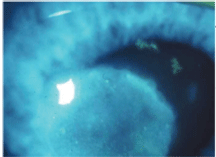
Stromal herpes zoster keratitis presents here with two small pseudodendrites. Courtesy: J. James Thimons, O.D.
Zoster lesions have raised centers, he says. Pseudodendrites are actually areas of inflammatory cells. Theres a mounding of cells in the middle. With dye, theres no staining in the middle; it sheds to the sides.
A dendrite necroses the central tissue while viral replication takes place, says Dr. Thimons. In the middle, the tissues dead and the cells have sloughed off. Upon staining, youll see an intense accumulation of dye around the lesion. The middle will be less intense.
But, this patients lesions appear secondary to the zoster, says Dr. Calderon. He appears to have developed an anterior stromal keratitis, characterized by multiple fine infiltrates found directly beneath the corneal surface in the anterior stroma, she says. These lesions tend to develop one to two weeks after the onset of the skin rash and are often formed beneath pre-existing epithelial dendriform keratitis. It may progress to a deep stromal keratitis, often occurring from one month to many years later.
Initial treatment should include an oral antiviral (acyclovir, famciclovir or valacyclovir), she says. This helps reduce the development of further ocular complications. Topical corticosteroid therapy often helps to decrease inflammation associated with HZO stromal keratitis, but can make cases where the corneal epithelium is involved worse. Another precaution: patients with renal insufficiency must be managed carefully while on oral antivirals, she adds.
If the epithelium is not involved, expect a response to treatment in about one week, says Dr. Thimons. But, mistakenly prescribing a topical steroid in a case of epithelial keratitis only allows the virus to flourish.3
In immunocompromised patients, a chronic zoster infection is possible. Says Dr. Calderon: The course of healing will vary depending on the strength of the patients immune system. It can become chronic and relapsing. Serious visual sequelae can be expected in patients who are severely immunocompromised. Such cases typically respond to longer courses of topical and oral antivirals.
If the patient is younger than age 50, find the cause of his immunosuppression, Dr. Thimons says. The immune system should be able to ward off the disease. Ensure that the presentation doesnt signify an underlying systemic condition.
Treatment will not be short and simple. Active virus has been found within the cornea for up to 30 days, says Dr. Calderon.4
Educate the patient about the progress of treatment, Dr. Thimons says. This tends to motivate compliance, and its much easier [for a patient] to be compliant in an acute episode such as this.
1. Shaikh S, Ta CN. Evaluation and management of herpes zoster ophthalmicus. Am Fam Physician 2002 Nov 1;66(9):1723-30.
2. Cobo M, Foulk GN, Liesegang T, et al. Observations on the natural history of herpes zoster ophthalmicus. Curr Eye Res 1987 Jan;6(1):195-9.
3. Calderon D, Schinas Z. Vanquish the Virus. Rev Optom 2005 May 15;142(5):98-107.
4. Moon CH, Silverberg MA. Herpes Zoster Ophthalmicus. www.emedicine.com/emerg/topic249.htm (Accessed December 2007).

