 |
|
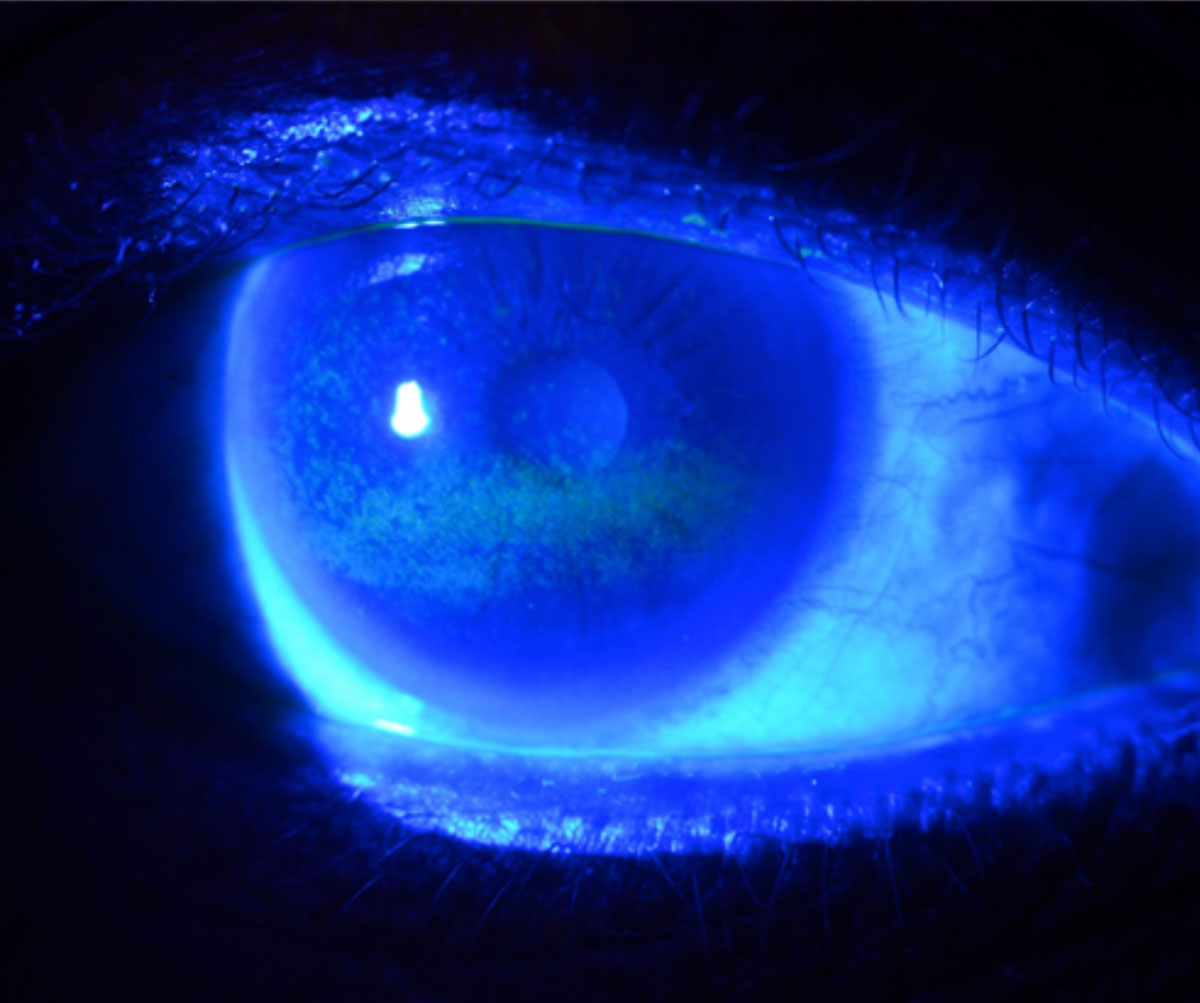
Variability in testing can make it more challenging for clinicians to accurately diagnose and interpret changes in dry eye signs and symptoms. Photo: W.R. Buie, OD. Click image to enlarge. |
Clinicians have several tools at their disposal for diagnosing and monitoring patients’ dry eye disease, but experts note that there’s no single gold standard test for this multifactorial condition. With so many options for dry eye disease diagnosis and monitoring, which tests should clinicians turn to first? Also worrisome is the variable repeatability of many such tests: Will repeating a given test on a different day yield the same result? If not, that introduces concerns about unreliability and the risk of false positives or negatives.
In a poster presentation at ARVO this Tuesday, DREAM Study researchers reported retrospective findings on dry eye test repeatability, an indication of a test’s reliability as a diagnostic tool. They focused on eyes with moderate to severe disease, noting that previous studies have evaluated test repeatability in mild to moderate dry eye. In the moderate to severe patient population, they found only moderate test repeatability.
The randomized DREAM study included a screening visit and a baseline visit about two weeks apart. At both visits, dry eye disease was assessed by the same physician in the same order: tear break-up time (TBUT), corneal fluorescein staining, meibomian gland dysfunction (MGD), conjunctival lissamine staining and Schirmer test. “Theoretically, if the tests were perfectly repeatable, there should be little variation between visits,” the authors explained in their abstract.
The researchers of the present study calculated the agreement of dry eye signs for 1,046 eyes (523 patients) between the two visits. They reported variable measurement agreement between visits. Corneal staining score had the least variability, followed by conjunctival staining score. These were followed by Schirmer test, MGD and TBUT, respectively.
The researchers noted that “a substantial percent of eyes showed clinically significant absolute differences between visits.” with two or more points in conjunctival staining score in 17.8% of eyes, three or more points in corneal staining score in 9.9% of eyes, three or more seconds TBUT in 6.2% of eyes, 5mm/5 min or greater in 22.7% of eyes for Schirmer test and greater than two points in 13.7% of eyes for MGD.
“These findings suggest the need to consider test-retest variability of dry eye disease measurements when designing dry eye clinical trials and monitoring progression of dry eye disease,” the researchers concluded in their ARVO abstract.
Original abstract content @2024 Association for Research in Vision and Ophthalmology.
Chen A, Augello P, Asbell PA, Ying G. The repeatability of tests for dry eye signs in the Dry Eye Assessment and Management (DREAM) study. Poster presented on Tuesday, May 7, at ARVO 2024 in Seattle, WA. |

