Optometric practices are facing increased demands as the US population ages. Approximately 4% of the US population has vision impairment that is not correctable with surgery or corrective lenses, and 80% of these people are over the age of 65.1-2 Currently, four million Americans live with vision impairment, and this number is expected to increase by 350,000 people each year.1-2 The cost associated with vision impairment and eye diseases is expected to reach 770 billion dollars by the year 2050.3
Despite the rising need, vision rehabilitation remains an underused service. One report estimates that less than 10% of those who could benefit from vision rehabilitation services used them.4 If optometrists can increase the availability of low vision services, they can improve the quality of life for their patients and reduce the overall burden on the health care system in the process.5-6 In addition, providing low vision services can be an area for practice growth, as it often includes the prescription of multiple pairs of glasses, device sales and improved relationships with referral sources such as occupational therapists and ophthalmologists.
We all receive low vision training during our optometric education, yet only a small percentage actually incorporate low vision into our practice. In Massachusetts, where we have an abundance of eye care providers, our estimates show that we are meeting the needs of only about 16% of those people living in the state with vision impairment. This article outlines what you can do to incorporate low vision services into your practice to help meet the needs of all of your patients.
 |
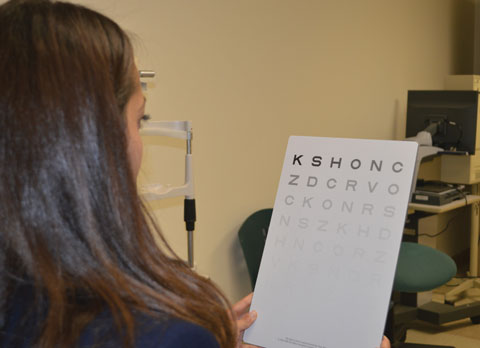
| The high contrast and backlighting of an ETDRS chart is ideal for low vision patients. |
Barriers to Care
A number of issues have been cited as barriers to providing low vision care in optometric practices. For some optometrists the primary barrier is chair time. Low vision exams traditionally take more time than a comprehensive eye health and vision exam. In addition, optometrists may not feel they are up to date on their skillset or on the technology used to care for patients with low vision. Finally, optometrists often express concerns about reimbursement rates for low vision services and device sales.
From the patient’s standpoint, barriers include lack of knowledge of low vision services and the benefits these services may provide.4,7 Even if they are aware, some patients with vision impairment may lack transportation and are unable to access services. Finally, there are not enough low vision doctors to provide care to all of those who need it.
One of the challenges we face is how to define low vision. According to Medicare, low vision is defined as visual acuity worse than 20/70, visually significant scotomas, visual field loss or any combination of these three. However, most low vision practitioners define low vision as any level of vision impairment that impacts a patient’s function. Many patients are not aware that their functional complaint can be addressed and do not volunteer information about difficulties they are having with a particular task. Thus, we must ask direct questions to elicit these functional complaints from a patient and begin the conversation about low vision services.
Recommended Equipment
The first two questions doctors ask when considering adding low vision to their practices is what kind of equipment they need, and how much it will cost them.
There is a difference between the ideal setup—found at comprehensive low vision centers such as those affiliated with the major hospitals and academic institutions in ophthalmology and optometry—and what a private practitioner requires to provide low vision care. Here are some essentials to get any clinician started with low vision services in their office:
ETDRS chart. This is the ideal acuity chart for low vision patients because of the high contrast and the backlighting. It can be moved to various distances from 4m to 2m and then to 1m, depending on the patient’s acuity.
a. There are an equal number of letters per line, allowing the 20/400 patient to have five letters to localize with their eccentric view (EV) rather than the one found on a traditional chart.
b. The ETDRS chart is also logarithmic in its progression from the largest line to the smallest line, as well as with the letter spacing.
c. If an ETDRS chart is not available, a digital acuity chart and a Feinbloom chart are alternatives to a standard projector to measure acuities at greater levels.
Contrast sensitivity chart. Contrast sensitivity can give a better sense of a patient’s functional vision than acuity alone. Reduced contrast sensitivity is an independent risk factor for reduced function in all of the visual domains except mobility.6 There are multiple options for testing contrast sensitivity, including: Mars, Pelli-Robson and iPad apps (with calibrated screen settings).
 |
| A Mars contrast sensitivity chart provides a better sense of this patient’s functional vision than acuity alone. |
Continuous text reading card. A continuous text card, such as MNRead or Lighthouse Continuous text card, will help determine a patient’s critical print size (i.e., the print at which fluent reading slows). This is different than assessing a threshold print size or a letter acuity, as the critical print is truer to the real-world reading needs of the low vision patient.
Near vision materials. Have magazines, pill bottles, food packages and checkbooks (standard and large print) on hand to test patients’ spot reading abilities.
To properly evaluate patients, clinicians must also invest in visual assistive equipment such as:
High plus spectacles/prism half-eyes. Powers from +4D with 6 BI to +8D with 10 BI will cover a good range of visual needs.
Hand magnifiers. A range of powers from about 8D to 20D will meet the needs of many low vision patients; LED hand magnifiers tend to be the most well received, but non-illuminated hand magnifiers can be useful for their portability.
Stand magnifiers. Consider starting with a dome/bar magnifier and one to two LED stand magnifiers. Don’t forget to think about the add power presbyopes require to use a stand magnifier.
Telescopes. Monoculars ranging from 2x to 6x are good starting points. Patients requiring more power will likely need more advanced low vision services. Also invest in a 2x to 3x binocular system for television viewing.
Video/digital magnification. Demonstrating a portable or desktop CCTV can help patients understand the full range of low vision aids available to them. Although you do not need to obtain all of the brands and styles, familiarize yourself with the various features of the different devices so you can discuss them with the patient.
Filters. Keep a range of filters in your optical or low vision supply, especially yellow, plum, amber and gray. Patients with all levels of visual impairment experience symptoms of both indoor and outdoor glare. Having several options available in office will help you determine the most appropriate filter for the patient’s comfort and visual function.
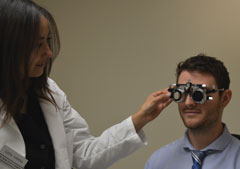 |
| Trial frames are a must for low vision exams, as they help patients eccentrically view with greater ease. |
Non-opticals. Large print checkbooks, bold-lined paper, bold pens and typoscopes are all useful tools to demonstrate to patients.
Clinicians may also choose to keep some visual assistive equipment in stock so that the devices can be readily dispensed to the patient.
The Low Vision Exam
The low vision functional history is one of the most important components in a low vision exam. We can break the history down into five functional domains: reading, visual information/seeing, mobility, activities of daily living and driving (Table 1).
Reading. Most patients who present to low vision clinics come with a chief complaint of difficulty reading.8 Determining the patient’s preferred type of reading will help guide the low vision exam and the strategies used for rehabilitation. Inquire as to whether the patient has primarily spot reading goals (labels, mail, bills) or if they also have continuous text goals (newspaper, books, magazines). Knowing whether the patient is reading electronically (computer, tablet, cell phone) or if the patient reads only standard print materials will impact your treatment approach as well.
Visual information/seeing. This encompasses the patient’s ability to see faces at a distance, to see a television and also how the patient functions in different lighting conditions. Patients may express difficulty adapting to changing lighting conditions or with their ability to tolerate indoor or outdoor glare.
Mobility. A decrease of just one or two lines of acuity (from 20/20 or 20/30) increases the risk of falls significantly.9 Patients may not always understand the interaction between their vision and their mobility, and we can play a very important role in educating the patient and helping prevent future falls. It is essential to ask all low vision patients about their history of falls, fear of falling and what, if any, mobility aids they are using. Referring a patient to an orientation and mobility specialist or recommending they seek an evaluation with a physical therapist may make a substantial improvement to that patient’s ability to continue to live safely and independently.
Activities of daily living. Asking patients specific, directed questions about their daily living activities—cooking, cleaning, bathing, dressing and medication management, for example—can help you create the best rehabilitation plan. For patients who have significant reported difficulty in this particular domain, a referral to low vision occupational therapy can be beneficial.
Table 1. Addressing Five Functional Domains During the Exam | |
| Functional Domain | Suggested Questions in Case History |
| Reading | - Are you an avid reader? |
| Visual Information | - Do you have trouble recognizing faces? From what distance? - Do you have difficulty adapting to variable lighting conditions? |
| Mobility | - Have you had any falls in the last two years? - Are you afraid of falling? |
| Activities of Daily Living | - Have you had any accidental cuts or burns while cooking? - Do you have difficulty with medication management? |
| Driving | - When was the last time you drove? - Are you limiting your driving? - Have you had any accidents or near misses? |
Driving. Whether a patient has vision impairment or not, we are frequently called upon to sign off on driver’s licenses. As low vision specialists, we must be familiar with state laws and understand the intricacies of the medical review board process to best advise patients. In addition, identifying certified driving rehabilitation instructors in the community can help you make more informed decisions about a patient’s safety on the road.
The intricacies of a low vision exam go beyond the scope of this article, but keeping these functional domains at the forefront can provide a general guideline for conducting a low vision history and identifying patient goals. Moving through the exam based on the patient’s goals will minimize chair time without sacrificing your ability to provide low vision care.
After the patient history, the fundamentals of a low vision exam are similar to the basics of a standard ocular health evaluation.
All low vision exams begin with a measurement of visual acuity at both distance and near. Supplemental testing may include contrast sensitivity and Amsler grid/mapping of central scotomas. These tests are useful in determining the appropriate magnification requirements for patients. They are also helpful when educating patients and their families about the visual condition and visual function. Visual field testing such as facial fields, confrontation fields, Goldmann visual fields or standard perimetry may also be necessary. Understanding the extent of a patient’s peripheral field loss will guide the rehabilitation plan and provide valuable information to the members of the rehabilitation team, including the occupational therapist and orientation and mobility specialist.
Low vision refractions are best performed through a trial frame, allowing the patient to eccentrically view with greater ease. Trial frames also facilitate the larger lens changes needed to use the principle of just noticeable differences (JND). Patient education about how much or how little change there is to the glasses Rx will aid in success during the remainder of the low vision exam. Patients are often optimistic that there will be significant changes in their vision after refraction. If there is a minimal change, it is important that the patient understand so that they can be open-minded to the rehabilitative strategies that you will explore.
 |
| Continuous reading charts help simulate the real-world reading needs of patients with low vision. |
Rehabilitation/Team Management
Integrating low vision into your practice requires more than just your expertise—a team approach is key for patients with low vision. To be successful in providing low vision care, become familiar with the available resources in your community. Each state has resources for those who are legally blind, and, often, these services extend to those with vision impairment as well. Either the department of education or the department of disability usually runs these services.
You must also be prepared to refer patients for low vision occupational therapy as needed. In order to see a patient, an occupational therapist requires a written referral from you. Many occupational therapists have forms that include the covered diagnosis codes as well as any other information essential to their evaluation. You will also sign off on the plan of care as well as the progress notes as the patient continues through their rehabilitation. Whether the occupational therapist works with the patient in the home or in the clinic, they can address activities of daily living the patient struggles with most. Occupational therapists may work in conjunction with speech and language pathologists and physical therapists to provide comprehensive care to the patient with low vision. Occupational therapists can assist with developing strategies to reinforce new learning, home modifications and problem solving. These skills help patients remain independent, even as their visual condition changes. This team approach to care ensures your patient’s needs are being met on all fronts.
Billing and Coding
Billing for low vision exams is less complicated than you think. Because all low vision patients enter with a medical diagnosis, you will most likely use the patient’s medical insurance and will bill with an E/M code for the visit. The low vision visit is typically not billed on medical complexity but instead is based on the face-to-face time spent with the patient.10 Medicare provides guidelines for visits during which you spend extended time on education and counseling. To be compliant with this type of billing, document the amount of time spent with the patient and what percentage of the time was spent on education, counseling and coordination of care. These codes are used most frequently when the face-to-face time component is greater than 50% of the exam. It is also important to educate the patient that the refraction is not a covered service in a medical visit, even though it’s part of the low vision exam. Low vision refraction fees vary by practice but are often more than the standard refraction given the extra time and complexity. Do not include the refraction in the face-to-face time, since you will bill that portion of the exam separately.
Some insurances are beginning to provide coverage for low vision aids, particularly when patients have vision plans. It is important to discuss this possibility with patients and help them understand, for insurance purposes, the difference between standard spectacles and visual assistive equipment.
Staff Training
Having a well-trained staff is the key to any successful practice, and a low vision practice is no different. Staff responsibilities will shift, and everyone has to be prepared to answer a whole new battery of questions. Here are some tips to ensure your staff is ready to take on the challenges associated with low vision patients:
Technician training:
Ask patients about their functional vision.
Ask how patients are coping with a diagnosis.
Assist with setting patient expectations regarding the low vision exam.
Front desk training:
Schedule low vision when the patient is referred to retina/glaucoma/cornea specialist for a chronic ocular disease.
Educate the patient on the phone that the doctor will be spending extra time looking at functional vision.
Educate the patient that the doctor is going to do a very different exam than the standard eye exam, which is why the appointment needs to be on a specific day/time.
Optical training:
Be prepared to answer questions about replacing magnifier batteries.
Have a full selection of tints available and schedule time to work through these options with the patient.
Become familiar with Fresnel lenses and working distances of high adds.
Prepare for the possibility that some patients may not be 20/20 when they pick up their new glasses.
Although all optometrists have the training to provide low vision care, not everyone decides to become a low vision specialist. Integrating some components of low vision into your practice can help with patient satisfaction and will allow for an easier transition to more advanced low vision care as the patient’s disease progresses. Patients are very appreciative when you take the time to provide the detailed trial frame refraction, can provide information about apps/assistive technology and can refer the patient for home safety assessments. Take advantage of the resources in your community, get to know local low vision specialists for the more complex patients and increase patient satisfaction.
Dr. Malkin is an assistant professor of optometry at the New England College of Optometry (NECO). She is a graduate of Emory University and completed her optometry training at NECO, where she graduated salutatorian. She completed her residency at the Northport VA Hospital with a focus in primary care optometry, low vision rehabilitation and vision therapy. Dr. Malkin completed the Lions Vision Rehabilitation Fellowship at Johns Hopkins in 2010. She is particularly interested in clinical research, including outcome measures and improved access to low vision care. She has published numerous peer-reviewed manuscripts in low vision rehabilitation and clinical outcomes and has lectured throughout the United States and internationally on a variety of topics including patient outcomes and technology in low vision.
|
1. Congdon N, O’Colmain B, Klaver CC, et al. Causes and prevalence of visual impairment among adults in the United States. Arch Ophthalmol. 2004;122(4):477-85. 2. Massof RW. A model of the prevalence and incidence of low vision and blindness among adults in the U.S. Optom Vis Sci. 2002;79:31-38. 3. Prevent Blindness. Future of Vision report. The Focus on Eye Health National Summit. 2014. Available at http://forecasting.preventblindness.org. 4. Leonard R, Gordon AR. Statistics on Vision Impairment: A Resource Manual. Research Institute of Lighthouse International. 2002. 5. Stelmack JA, Tang C, Reda DJ, et al. Outcomes of the Veterans Affairs Low Vision Intervention Trial (LOVIT). Arch Ophthalmol. 2008;126:608-17. 6. Goldstein JE, Massof RW, Deremeik JT, et al. Baseline traits of low vision patients served by private outpatient centers in the United States. Arch Ophthalmol. 2012;130:1028-37. 7. Casten RJ, Maloney EK, Rovner BW. Knowledge and use of low vision services among persons with age-related macular degeneration. Journal of Visual Impairment & Blindness. 2005;99(11):720-4. 8. Brown JC, Goldstein JE, Chan TL, et al.; the Low Vision Research Network Study Group. Characterizing functional complaints in patients seeking outpatient low vision services in the United States. Ophthalmology. 2014;121:1655-62. 9. Abdelhafiz AH, Austin CA. Visual factors should be assessed in older people presenting with falls or hip fracture. Age and Ageing. 2003;32:26-30. 10. Verhovshek JG. Go beyond the basics of time-based E/M coding. AACP. Available at www.aapc.com/blog/4615-go-beyond-the-basics-of-time-based-em-coding. Accessed September 27, 2016. |

