Capsaicin—an oily extract from chili pepper plants—is the active ingredient in pepper spray. Commonly used by police officers, security guards and civilians for protection against assailants, the spray’s recommended target is the eye. Capsaicin has been added to these self-defending sprays because it has an immediate onset of action—inducing pain, tearing, blurred vision and blepharospasm.1
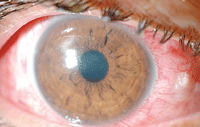
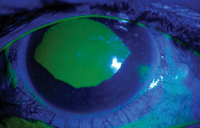
1, 2. Anterior segment photography (top) and fluorescein staining (bottom) of our patient’s right eye at the initial visit.
Previous studies have shown that capsaicin can cause mild and transient ocular surface injury, but is relatively harmless to the cornea and conjunctiva after a single exposure.2 Capsaicin is considered safer than early-generation tear gas, such as chloroacetophenone, which frequently lead to broad keratopathy that required long-term medical management.3 These advantages have made pepper spray the preferred legal, non-lethal form of self-protection used by both civilians and law enforcement agencies.
Law enforcement officers must go through drills and simulations with live pepper spray exposures to appreciate its effects and management.4 Although acute exposure to pepper spray is relatively safe with appropriate and prompt first aid, serious and long-lasting damage to the ocular surface—including the cornea—can arise when medical attention is delayed or omitted.
Here, we present the case report of a patient who got pepper sprayed in his right eye, which resulted in severe conjunctival hyperemia, chemosis and a large central corneal abrasion. We will briefly review the literature on capsaicin and discuss its clinical management and use.
History
A 27-year-old Hispanic male presented with a complaint of general ocular pain, pain on eye movements, severe redness, tearing and blurry vision in his right eye. He explained that a security guard at a nightclub had subdued him with pepper spray on a Saturday night four days prior. The exposure was mainly in his right eye and minimal in his left eye. Immediately after the incident, he washed his eyes with soda.
On Sunday, he woke up with severe pain in his right eye, but decided to wait, hoping it would improve. He had a similar experience three years ago with minimal symptoms. He was healthy and not taking any medications.
Diagnostic Data
The patient’s right eye had moderate lid swelling, conjunctival hyperemia and a large, central corneal abrasion, which was alarming at initial presentation. We instilled a drop of topical anesthetic to relieve the blepharospasm. Before measuring visual acuity, we performed a thorough saline lavage and confirmed (with litmus strips) that his ocular pH was neutral. His best-uncorrected entering visual acuity was 20/60-1, pinhole 20/50+2 OD in the affected right eye and 20/25-1 OS. Confrontational fields were normal and there was no afferent defect. Refraction was deferred.
Biomicroscopy of the anterior segment showed 360° grade 3 conjunctival injection (figure 1) and, upon fluorescein staining, a large (1DD) central corneal abrasion OD with significant swelling, but no Seidel’s sign (figure 2), symblephara or foreign debris. The lids were everted. Anterior segment examination of the left eye showed mild conjunctival injection without corneal defect.
Intraocular pressure by applanation measured 18mm Hg OU. Direct funduscopy showed no gross defects.
Management
We instilled one drop of atropine sulfate 1% for in-office cycloplegia as well as TobraDex (tobramycin/dexamethasone, Alcon) for antibiotic/inflammatory coverage OU.
We prescribed a bandage contact lens (AirOptix Night & Day, Ciba Vision), along with TobraDex QID OD, and scheduled the patient to return to the clinic in two days. We educated the patient about bandage contact lenses, medical treatment and the importance of follow-up visits. We also advised him to take over-the-counter acetaminophen or ibuprofen as needed, along with cold compresses and artificial tears. The left eye required only passive lubrication therapy.
Follow-up Visit 1
The patient returned two days later for a follow-up. He reported feeling better with less pain. After removal of the bandage contact lens, uncorrected visual acuity was 20/70, pinhole 20/60- OD and 20/20- OS.
Biomicroscopy of the anterior segment showed 360° grade 2 conjunctival injection (figure 3) and a resolving corneal abrasion OD via fluorescein staining (figure 4). Anterior segment examination of the left eye was normal. IOP was 16mm Hg OD and 14mm Hg OS.
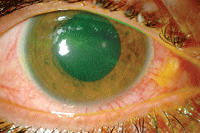
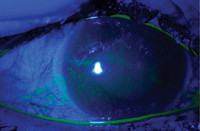
3, 4. Anterior segment photography (left) and fluorescein staining (right) of our patient’s right eye at the two-day follow-up visit.
Dilated fundus examination showed normal ocular health with cup-to-disc ratios of 0.15H x 0.15V OU. We instructed the patient to continue with TobraDex QID OD and return in five days, or sooner if necessary. We did not replace the bandage lens.
Follow-up Visit 2
One week later, the patient’s visual acuities had improved significantly and measured 20/25- OD and 20/20- OS. Biomicroscopy of the anterior segment OD showed trace conjunctival injection (figure 5) and an intact cornea via fluorescein staining (figure 6). Anterior segment examination of the left eye was normal. IOP by applanation was 16mm Hg OD and 15mm Hg OS.
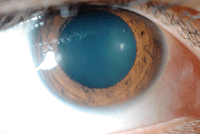

5, 6. Anterior segment photography (left) and fluorescein staining (right) of our patient’s right eye at the one-week follow-up visit.
We informed the patient that the surface injuries to both the conjunctiva and cornea were now 95% resolved. We instructed him to taper the TobraDex to BID for two days OD, then QD for two days and then discontinue.
We explained the possibility of recurrent corneal erosion in the future and advised him to continue using the topical artificial tears to prevent it. We also educated him on first aid for chemical exposure (emergency eye wash techniques) in case of future exposures, and asked him to return in four months, or earlier if needed.
Discussion
Pepper spray products are sold in various formulations and packages containing a large variety of ingredients and different concentrations of capsaicin. For example, one version used in a police drill study (Cap-Stun, Zarc) was a mixture containing 5.5% oleoresin capsicum, 30.5% isobutane as a propellant and 64% isopropyl alcohol as a carrier.2 In addition, caustic chemicals—such as alcohols and organic solvents—are standard components of both the spray and propellant, and each of these components has the potential to induce serious conjunctival and corneal injury.
Central corneal abrasion secondary to pepper spray insult is not common, but can occur secondary to the chemical’s effects or rubbing of the eyes following the exposure. Ocular injury associated with pepper spray is common. Fortunately, most cases of capsaicin exposure cause only minor and ephemeral ocular injury with prompt irrigation and medical care. However, serious and long-lasting ocular damage can result with delayed management.
Our patient’s large corneal epithelial damage could very well have been caused by violent rubbing and/or isopropyl alcohol, and other organic solvents that were part of the pepper spray mixture, rather than by capsaicin.
Previous studies on the acute effects of capsaicin on corneal nerve in animals suggested that it activates the vanilloid receptor (VR1, an ion channel) in polymodal nociceptive neurons, leading to massive neuronal calcium entry and a transient excitation of the nerves producing intense pain followed by neuronal damage and desensitization of most fibers to all subsequent stimuli.5-8 In other words, capsaicin usually causes acute neurogenic inflammation, pain, erythema, tearing, blepharospasm and blurred vision.
Most recently, researchers in Switzerland reported a rare case of conjunctival proliferation in a toddler after a mild exposure to pepper spray.9 Emergency medical doctors reported the case of a 21-year-old military police officer candidate who developed a corneal ulcer after pepper spray exposure following military training.10 Serious systemic effects due to pepper spray exposure have been also reported, including bradycardia, hypotension and even death.11
Pepper spray has been approved for use as self-defense weapon since the 1970s.2 There have been various anecdotal treatments published but little research into their efficacy—including vegetable oil, baking soda paste, vinegar, milk, alcohol, lidocaine gel, antacids and corticosteroids.
A 2008 trial studied the amount of pain relief over time provided by antacid Maalox (magnesium hydroxide-aluminum hydroxide, Novartis), whole milk, 2% lidocaine gel and baby shampoo, as compared with tap water, in adult volunteers who were exposed to Cap-Stun.13 Results showed there was no significant difference between treatment groups, and time was the most important factor in the resolution of pain from pepper spray exposure. The authors concluded that a copious water wash remains the preferred method of decontamination after exposure to pepper spray, and oral analgesics may be used for pain relief as needed.
Interestingly, low-concentration topical capsaicin has been used effectively as treatment of post-herpetic neuralgia (PHN) for decades and, more recently, Qutenza (capsaicin, NeurogesX Inc.), a higher concentration (8%) capsaicin patch, has been approved for PHN.14,15
The patch is applied to the affected area with a topical anesthetic to reduce application site pain. A single, one-hour application can provide three months of relief from PHN or pain after shingles.16
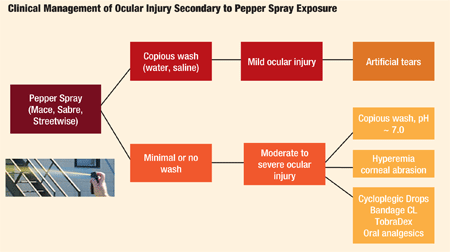
Although acute exposure to pepper spray is relatively safe with appropriate and prompt first aid, serious and long-lasting damage to the ocular surface—including the cornea—can arise without prompt irrigation and medical attention. Exposure to pepper spray is similar to other chemical exposure; thus, ocular injury must be managed initially by copious irrigation with water or saline and followed by medical therapy.
Dr. Hua is assistant professor of optometry at the Pacific University College of Optometry in Forest Grove, Ore. Mr. Hughes is a third-year optometric intern at the same university.
1. Zollman TM, Bragg RM, Harrison DA. Clinical effects of oleoresin capsicum (pepper spray) on the human cornea and conjunctiva. Ophthalmology. 2000 Dec;107(12):2186-9.
2. Vesaluoma M, Muller L, Gallar J, et al. Effects of oleoresin capsicum pepper spray on human corneal morphology and sensitivity. Invest Ophthalmol Vis Sci. 2000 Jul;41(8):2138-47.
3. Hoffmann DH. Eye burns caused by tear gas. Br J Ophthalmol. 1967 Apr;51(4):265-8.
4. Lee RJ, Yolton TL, Yolton DP, et al. Personal defense sprays: effects and management of exposure. J Am Optom Assoc. 1996 Sep;67(9):548-60.
5. Caterina MJ, Schumacher MA, Tominaga M, et al. The capsaicin receptor: a heat-activated ion channel in the pain pathway. Nature. 1997 Oct 23;389(6653):816-24.
6. Tominaga M, Caterina MJ, Malmberg AB, et al. The cloned capsaicin receptor integrates multiple pain-producing stimuli. Neuron. 1998 Sep;21(3):531-43.
7. Belmonte C, Gallar J, Pozo MA, Rebollo I. Excitation by irritant chemical substances of sensory afferent units in the cat’s cornea. J Physiol. 1991 Jun;437:709-25.
8. Chen X, Belmonte C, Rang HP. Capsaicin and carbon dioxide act by distinct mechanisms on sensory nerve terminals in the cat cornea. Pain. 1997 Mar;70(1):23-9.
9. Gerber S, Frueh BE, Tappeiner C. Conjunctival proliferation after a mild pepper spray injury in a young child. Cornea. 2011 Sep;30(9):1042-4.
10. Shimada M, Young C, Tanen DA. Corneal ulcer associated with pepper spray exposure during military training. J Emerg Med. 2012 Aug;43(2):e149.
11. Steffee CH, Lantz PE, Flannagan LM, et al. Oleoresin capsicum (pepper) spray and “in-custody-deaths.” Am J Forensic Med Pathol. 1995 Sep;16(3):185-92.
12. Watson WA, Stremel KR, Westdorp EJ. Oleoresin capsicum (Cap-Stun) toxicity from aerosol exposure. Ann Pharmacother. 1996 Jul-Aug;30(7-8):733-5.
13. Barry JD, Hennessy R, McManus JG Jr. A randomized controlled trial comparing treatment regimens for acute pain for topical oleoresin capsaicin (pepper spray) exposure in adult volunteers. Prehosp Emerg Care. 2008 Oct-Dec;12(4):432-7.
14. Watson CP, Tyler KL, Bickers DR, et al. A randomized vehicle-controlled trial of topical capsaicin in the treatment of postherpetic neuralgia. Clin Ther. 1993 May-Jun;15(3):510-26.
15. Irving GA, Backonja MM, Dunteman E, et al. A multicenter, randomized, double-blind, controlled study of NGX-4010, a high-concentration capsaicin patch, for the treatment of postherpetic neuralgia. Pain Med. 2011 Jan;12(1):99-109.
16. Jones VM, Moore KA, Peterson DM. Capsaicin 8% topical patch (Qutenza)--a review of the evidence. J Pain Palliat Care Pharmacother. 2011;25(1):32-41.

