 |
Q:
A 70-year-old woman was walking her dog and tripped, landing on the left side of her face. What are some things I should think about before sending her to an orbital specialist?A:
Orbital trauma can be overwhelming on initial presentation; however, breaking down your evaluation by ocular structure can help to focus your management,” says Paige Thompson, OD, of SouthEast Eye Specialists in Chattanooga, TN. Initially, doctors should obtain a visual acuity measurement, assess pupillary function and evaluate the patient’s extraocular motilities.
If visual acuity is reduced or an afferent pupillary defect is noted, investigate the underlying cause. Assess extraocular motilities to rule out any restriction or pain on eye movement, which may occur secondary to periorbital edema or orbital fracture.
Next, evaluate the orbits and adnexa for edema and ecchymosis. With palpation of the orbital rim, rule out focal tenderness and hypoesthesia, which may be associated with orbital fracture. Manage lid edema and bruising with cool compresses and head elevation. Rule out any conjunctival lacerations, corneal abrasions, or penetrating injuries.
“If a patient is found to have a ruptured globe, stop your exam, avoid applying any pressure to the eye and cover the patient’s eye with a protective shield,” Dr. Thompson says. Refer these patients immediately to a level one trauma center for appropriate management. Evaluate and treat the anterior chamber for traumatic hyphema, iritis or any combination.
“Evaluate the lens to rule out phacodonesis or lens subluxation,” says Dr. Thompson. “If the patient is found to have a subluxated lens, refer to a skilled cataract surgeon for evaluation and management.”
 |
| Evaluate a patient who experienced ocular trauma by using a stepwise approach. Click image to enlarge. |
Lastly, perform a dilated fundus examination to rule out commotio retinae, a common finding of whitening of the retinal tissue which typically resolves on its own within two weeks. Other potential posterior segment findings include retinal detachment, vitreous hemorrhage and traumatic optic neuropathy.
Orbital Fractures
Ultimately, an optometrist can appropriately manage many sequelae of ocular trauma. The main indication to refer to an orbital specialist would be with concern for orbital fracture, according to Dr. Thompson. An orbital fracture is most likely to occur in the orbital floor, followed by the medial orbital wall and commonly causes restricted upgaze, secondary to entrapment of the inferior rectus in the orbital floor.
If an orbital fracture is suspected, send the patient for neuroimaging to confirm the diagnosis with a CT scan, the preferred modality in traumatic cases. Specifically, axial views are preferred for evaluation of the orbital rim, and coronal views are ideal for detecting orbital floor fractures and muscle entrapment.
“Educate these patients to avoid nose blowing and valsalva maneuvers to prevent potential cellulitis,” says Dr. Thompson. Most orbital fracture repairs are not emergency situations. The surgeon will typically wait for resolution of periorbital edema prior to surgical intervention. Treat orbital fractures emergently only in the case of muscle entrapment to prevent ischemia and persistent diplopia.
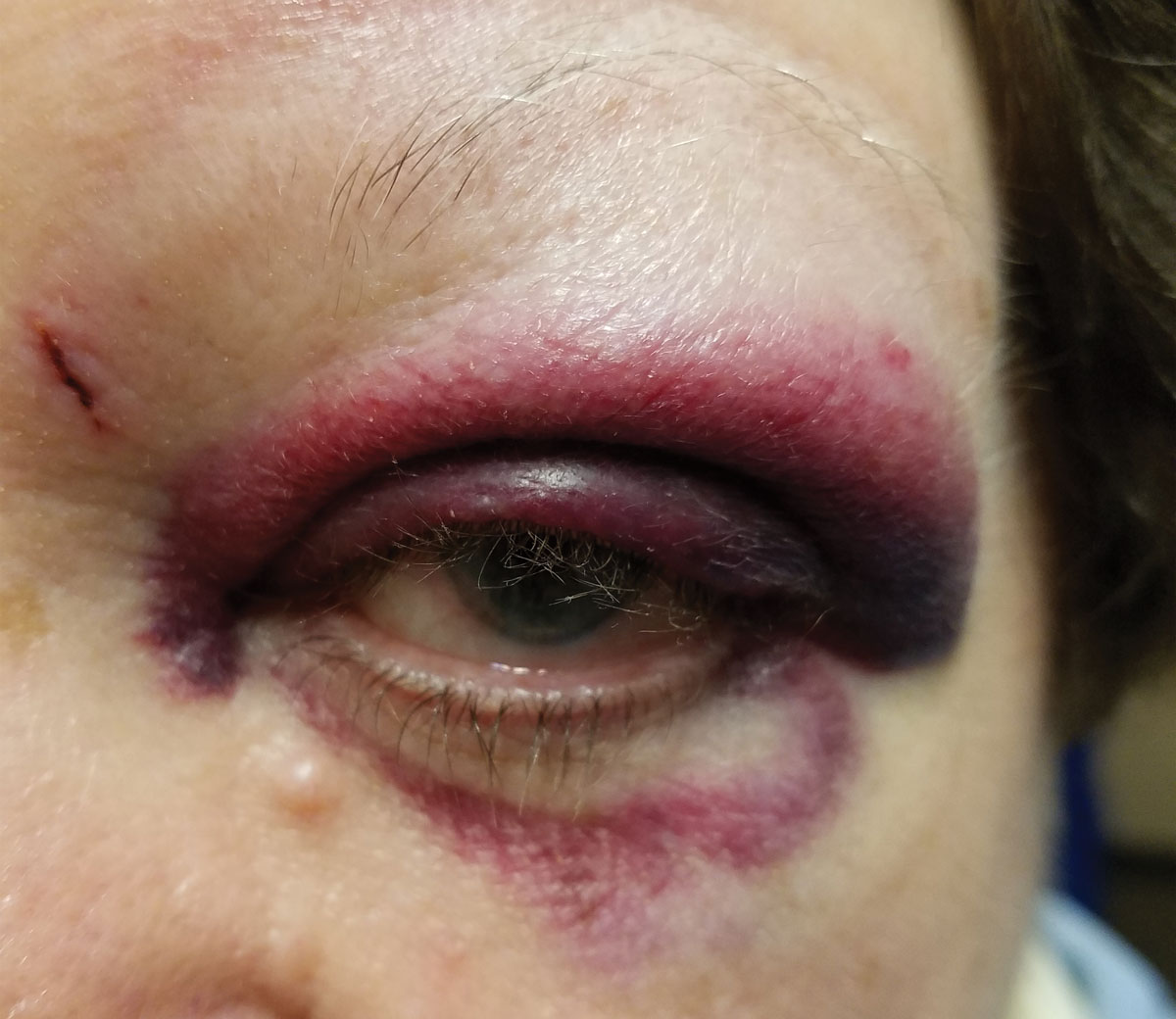
“We evaluated and diagnosed our patient with periorbital edema and ecchymosis,” Dr. Thompson says. All other exam findings were unremarkable. She and her team conservatively managed the patient with cool compresses, and the patient’s contusions and edema resolved over several weeks without any further sequelae. “Next time you evaluate a patient with blunt trauma, relax and examine the patient with a stepwise approach to determine if a referral is truly necessary,” Dr. Thompson adds.

