 |
Q:
A patient came in as an emergency due to severe pain in both eyes after a recent blepharoplasty at a plastic surgery center. I asked her to close her eyes, and she couldn’t. Her corneas revealed exposure keratitis as expected. What is the predicted course of her post-op recovery?
A:
“Manage and optimize risk factors such as dry eye and ocular surface disease pre-op,” James P. Milite, MD, an oculoplastic surgeon of Omni Eye Services in Iselin, NJ, says. “A conservative approach is mandated intraoperatively, with careful skin resection and attention to eyelid closure.”
When a patient asks you about lid surgery, take into consideration complaints of visual obstruction and brow fatigue. Cosmetic concerns, such as hooding or dermatochalasis, might be accentuated by physical discomfort that abrasion of the upper lid fold creates as it overrides the cilia. “Brow ptosis can cause a false appearance of upper eyelid hooding, leading to possible unexpected skin over-resection,” says Dr. Milite.
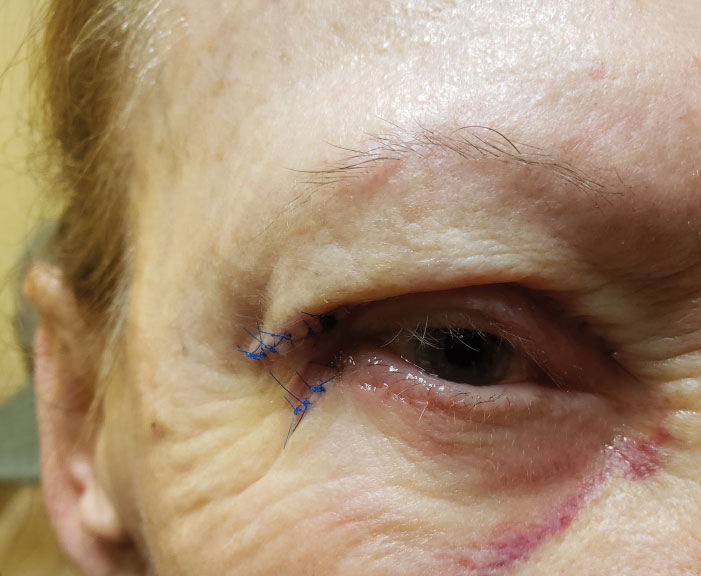 |
| Post-op overcorrection of ptosis could cause upper eyelid retraction and exposure keratitis. Click image to enlarge. |
Surgical Considerations
Margin reflex distance distinguishes true ptosis with low position of the upper eyelid margin from hooding. Have the patient focus on a focal light source with both eyes and measure the distance from the pupillary light reflex to the upper and lower eyelid margins. Cases with good levator function (greater than 10mm) can employ levator advancement. Poor levator function—more commonly seen in ptosis of congenital, muscular dystrophic or neurologic etiology—requires frontalis suspension.
To prevent post-op upper eyelid retraction and exposure keratitis, Dr. Milite emphasizes that careful preoperative incision marking can help avoid excessive skin excision. He believes a conservative approach is always appropriate. “Residual skin excess can always be secondarily resected, but excess skin removal cannot be easily corrected,” Dr. Milite says.
In cases where true ptosis exists and the levator position has advanced onto the tarsus, the surgeon will check eyelid position by asking the patient to open and close their eyes intraoperatively. They will assess symmetry as well as check for over- or under-correction. If the main source of visual obstruction is excessive skin fold overhang, patients should still open and close their eyes intraoperatively. An intraoperative
levator dehiscence induced by resecting skin could be missed and lead to an under-correction.
Post-op Checks
Dr. Milite advises to check for eyelid symmetry and ensure that eyelid closure is complete. “Symmetry is usually not exact at initial follow-up due to edema, so schedule a three- or four-week post-op visit when the edema has resolved,” he says. The patient should expect two to three weeks of post-op swelling and bruising.
If exposure keratitis persists, there are many possible causes. Primarily, there might be over-advancement of the levator muscle or there is a skin shortage from excessive skin resection or both. If it’s the levator muscle, a re-operation and levator position adjustment usually corrects it.
If the skin has been excessively removed, Dr. Milite says that is much more difficult to manage. He recommends maximizing topical lubrication, nocturnally applying ointment, placing punctual plugs, using moisture chamber goggles and massaging the upper eyelid skin downward once incisions have healed. If the patient’s problems persist, refer them back to the surgeon.
Maintaining ocular health takes priority over patient expectations of cosmetic and visual outcomes overall, so temper their expectations when counseling them before surgery, Dr. Milite adds. In the end, adequate eyelid closure and maintenance of a healthy ocular surface always trumps cosmesis.

