 |
Q:
A 27-year-old man who was plasma cutting without eye protection woke up in the middle of the night with excruciating pain. An ER visit at 3am resulted in a Polytrim (trimethoprim/polymyxin B sulfate, Allergan) prescription. He presented the next day with mild superficial punctate keratitis (SPK), still in severe pain and with photophobia. What is the best next step?
A:
“What is confusing about these cases is that the patient usually admits that they knowingly broke eye protection safety protocol, resulting in their ocular injury,” Marc Myers, OD, of Coatesville Veterans Affairs Medical Center in Pennsylvania, says. “The patient may notice the welder flash burn only when symptoms begin, usually six to 12 hours after exposure.”
Less experienced welders may not be aware of safety standards, or more experienced welders may attempt to hastily complete a job without eye protection. Proper use of a welder’s hood can virtually eliminate these injuries.
 |
|
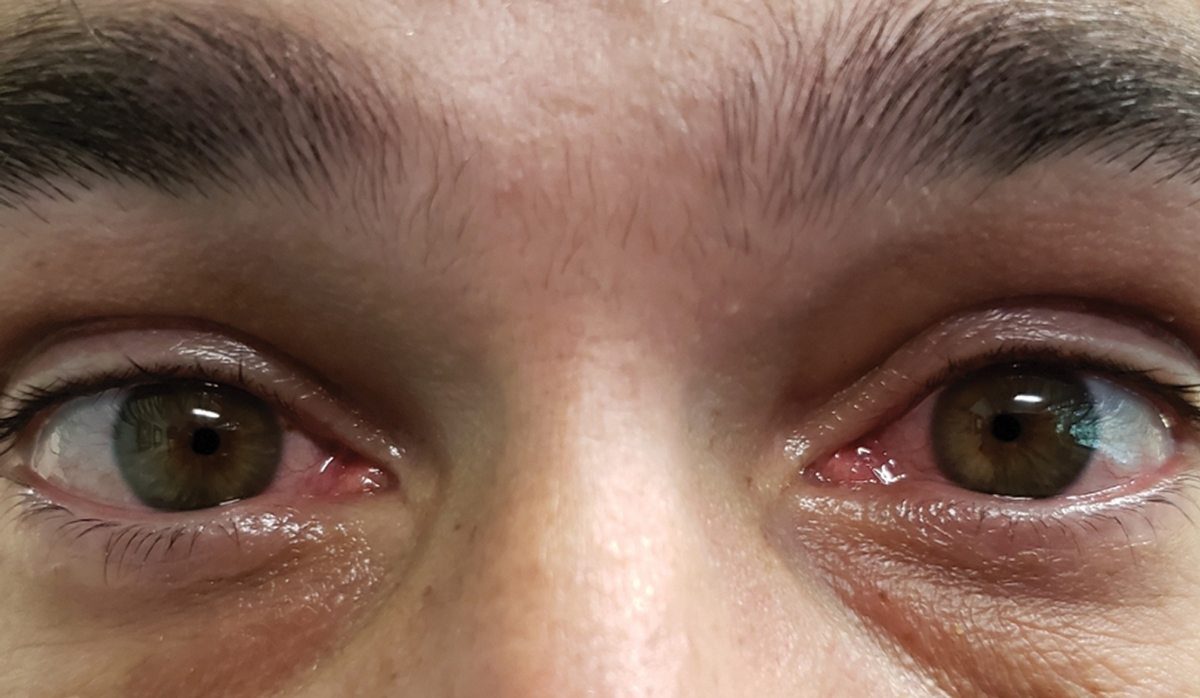
A patient might not notice a welder flash burn until symptoms begin. Click image to enlarge. |
Overexposed
Plasma cutting, or plasma arc cutting, involves a super-heated (40,000°F) column of gas that cuts electrically conductive materials, such as steel, stainless steel and aluminum.1 A plasma arc emits a broad-spectrum of electromagnetic radiation, extending into ultraviolet (UV) range.
Welding is thought to be the primary cause of UV keratitis.2 Other sources of UV energy that may result in keratitis include unprotected exposure to intense sunlight, artificial light from a tanning bed, staring at a solar eclipse and powerful halogen and photography flood lamps.2-4
UV keratitis, or photochemical keratitis, occurs when the cornea is exposed to excessive UV light. The corneal epithelium is chiefly responsible for the greatest quantity of the absorption of UV light. Photochemical toxicity can damage the epithelium, and, in doing so, may result in mitosis inhibition, nuclear fragmentation production and loosening of the epithelial layer, which ultimately leads to SPK.5
Symptoms include a bilateral sandy, scratchy feeling of foreign body sensation (FBS) followed by redness, tearing, pain and reduced visual acuity.5 “By understanding the mechanism behind the injury and predicting the course of recovery, treatment can address symptoms and improve the patient’s comfort,” Dr. Myers says.
Management
According to Dr. Myers, treatment consists of topical preparations to manage FBS and pain and includes viscous lubricants, cycloplegics and nonsteroidal anti-inflammatory drugs, steroids or a combination of these. The patient in question was put on Pred Forte (prednisolone acetate 0.1%, Allergan) QID, which quickly alleviated his symptoms. “I also encourage the use of an over-the-counter oral analgesic if topical therapy does not adequately control pain,” Dr. Myers says.
Customarily, a topical antibiotic is included as prophylaxis against potential infection. Encourage sunglasses to protect against photophobia and sleep during the recovery period. Lastly, Dr. Myers emphasizes appropriate eye protection when engaging in any form of activity that involves excessive UV exposure.
Fortunately, garden-variety cases of UV keratopathy respond well to treatment and significantly improve within 24 to 72 hours. Cases that involve the conjunctiva, UV keratoconjunctivitis, may take slightly longer to completely resolve when employing this same regimen of care. The cumulative effect of UV exposure may go beyond the cornea and result in pterygium and pinguecula as well as cataracts.
An ounce of prevention goes a long way, according to Dr. Myers. “In this case, always use the welder’s hood,” he notes.
1. Glassford E, Burr G, Glassford E, et al. Evaluating optical hazards from plasma arc cutting. J Occup Environ Hyg. 2018;15(1):D1-7. 2. Delic NC, Lyons JG, Di Girolamo N, Halliday GM. Damaging effects of ultraviolet radiation of the cornea. Photochem and Photobiol. 2017;93(4):920-9. 3. Podskochy A. Protective role of corneal epithelium against ultraviolet radiation damage. Acta Ophthalmol Scand. 2004;82(6):714-7. 4. Schein OD. Phototoxicity and the cornea. J Nat Med Assoc. 1992;84(7):579-83. 5. Willmann G. Ultraviolet keratitis: from the pathophysiological basis to prevention and clinical management. High Alt Med Biol. 2015;16(4):277-82. |

