 |
Q:
A patient called me Sunday evening after being on the losing end of a bar brawl Friday night. When seen in the ER on Saturday, a CT scan revealed an orbital floor fracture. He was told to see an eye doctor. How do you examine this swollen eye and how do you know when surgery is in order?
A:
“First of all, don’t panic,” says James Milite, MD, an oculoplastic surgeon from Omni Eye Services in Iselin, NJ. In many cases, the impact of the injury will make the eye look worse than it is. “Take a step back and take your time doing a thorough exam,” he says.
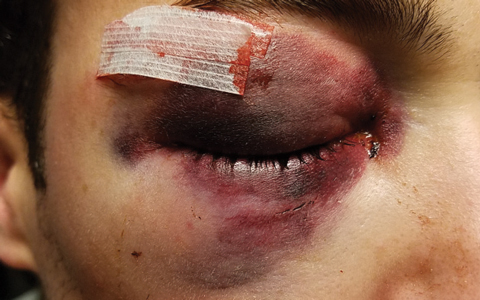 |
| A 25-year-old male with orbital floor fracture raises questions about the need for reconstructive surgery. |
A comprehensive history is your next step. You’ll want to know how the injury happened and what struck the eye. “Ask if there was any loss of consciousness at the scene of the incident; also find out if there have been any flashes, floaters or double vision. Check their lateral gaze and downgaze, ability to open and close the mouth, and look for evidence of decreased sensitivity in the distribution of the maxillary division of the trigeminal nerve,” says Dr. Milite.
After ruling out head trauma and foreign bodies, conduct your typical eye exam—acuities, confrontation fields, pupils and a careful anterior and posterior segment exam. “Make sure the retinal periphery is OK, and look out for corneal abrasions, hyphema, iridodialysis, uveitis, cataract, vitreous hemorrhage and retinal detachment,” adds Dr. Milite. Also, examine the orbit. “This can be the trickiest part due to the eye swelling,” he says. “Observe if the globe is sunken or displaced downward away from the midline. This might indicate a fracture of the cheek bone or cheek complex,” he says. Left untreated, it could permanently pull the lower lid down or flatten the malar region.
To Refer or Not to Refer?
After examination, you should have a sense of whether or not you have a surgical candidate on your hands, says Dr. Milite. “You’re looking for either or both of the following: entrapment causing restriction of extraocular muscles (EOMs) and diplopia in functional fields, and enophthalmos greater than 2mm.” However, the degree of periorbital edema often makes assessment of globe position and motility difficult.
“It’s also important to look out for signs of proptosis of the eye,” adds Dr. Milite. “This is an indicator of a retrobulbar hemorrhage.” Though uncommon, it necessitates an urgent referral to an oculoplastic specialist. All these patients require CT imaging if not already obtained prior to your exam.
Typically, if the primary injury is an orbital floor fracture, you won’t need to send for emergency surgery. However, there are a few extenuating circumstances. Young kids, for example, can more easily present with entrapment and require immediate surgery. “I usually see this in kids under age 13,” adds Dr. Milite, “as their bones are pliable and don’t crack—they bend and snap back, causing tight EOM entrapments.” This can lead to nausea, vomiting and a decrease in blood pressure.
Since the fracture snaps closed almost like a trap door, it might not seem significant on the scan, but these signs represent a potentially urgent case and require a rapid referral to an oculoplastic surgeon. Failure to refer could result in irreparable damage to the tightly entrapped muscle.
When choosing to treat these cases with antibiotics or steroids, a few simple rules will suffice. “Antibiotics are given due to theoretical risk of infection, so a five-day course of prophylactic antibiotic can’t hurt,” says Dr. Milite. “If you have a patient with a moderate-size fracture and excessive swelling, an oral steroid will cut the window down for edema resolution to unmask the development of enopthalmos and help determine the need for repair.”
Consult a specialist if in doubt. In this case, referral resulted in surgery later that week. “Describe the fracture, explain motility issues and record everything,” Dr. Milite says. “If it’s a surgical candidate, ask what you can do to prepare the patient before sending them along.”

