 |
Q:
A patient presents to me with a significantly swollen left upper lid. What are the next steps?
A:
While there are plenty of possible causes of swollen eyelids, the first that comes to mind is preseptal cellulitis. “While this is the most probable, we must always keep the differential with the highest chance of morbidity or mortality in mind,” says Mark Miriello, OD, of The Eye Institute in Philadelphia. “With swollen eyelids, that is orbital cellulitis.”
Other differentials to consider involve severe anterior segment inflammation such as viral conjunctivitis, corneal abrasion and even uveitis. Taking a careful symptom inventory and thorough slit lamp examination can help rule these differentials out.
 |
|
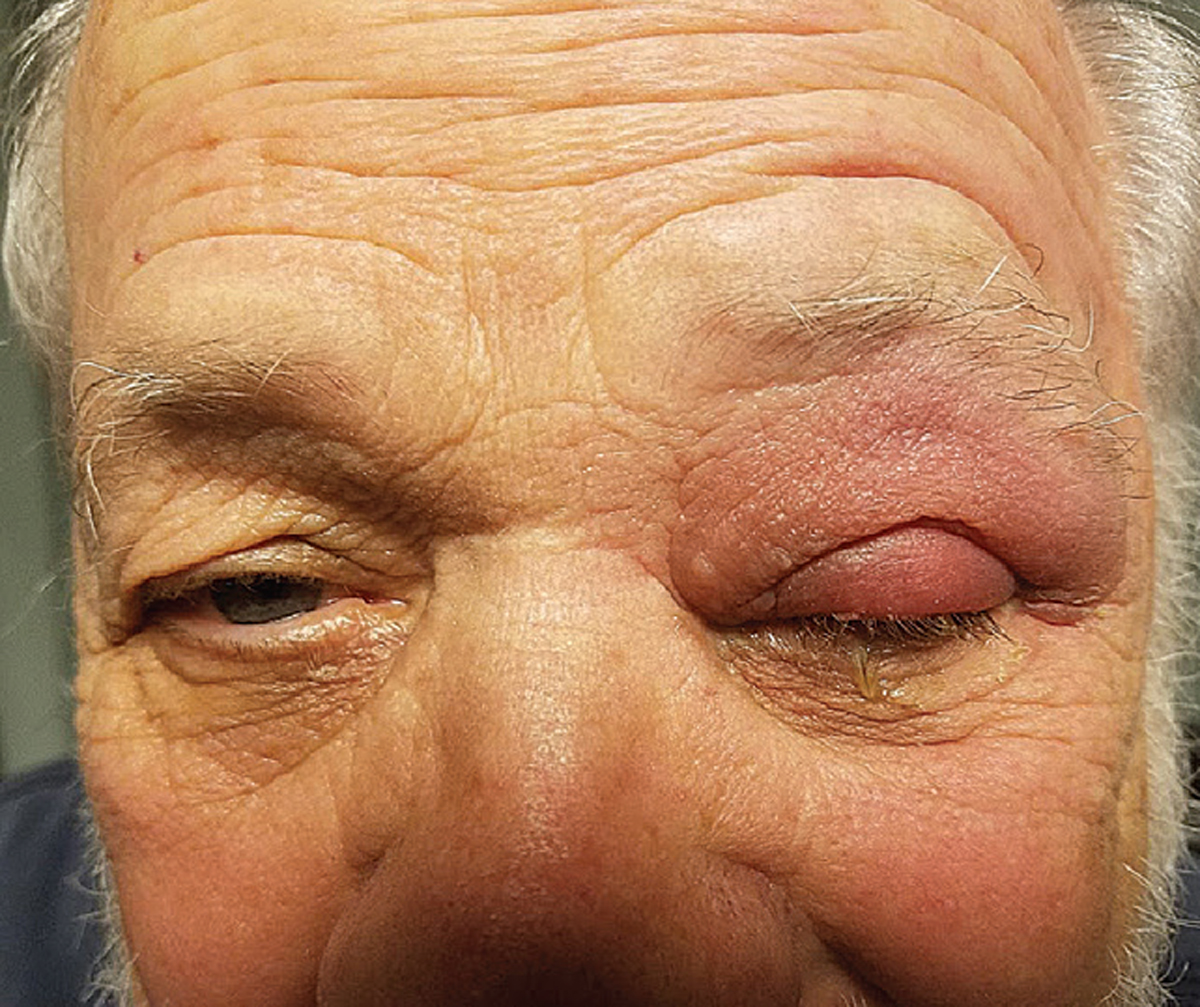
A patient with preseptal cellulitis who responded well to oral antibiotics. Click image to enlarge. |
Trace the Source
The orbital septum is a shield of fibrous tissue that acts as a barrier between the eyelids and the orbit itself. Preseptal cellulitis, then, is a bacterial infection of the skin—effectively isolated to the eyelids.1,2
Patients present with swollen, red lids that may be tender to the touch and febrile. Since the inflammation is confined to the eyelid, they present with unaffected vision, ocular motility and pupils and without proptosis.1-3
The source of the infection is often a result of other infectious eyelid lesions. Sinusitis, particularly of the ethmoid sinus, is a common culprit. Other routes of infection include superficial facial traumas and surgeries, foreign bodies and insect bites.1
When taking history, determine if the patient is at risk for any of these etiologies. “Ask about precipitating styes, traumas and sinus infections,” Dr. Miriello says. “If the patient can localize the part of the lids where their symptoms first presented, pay special attention there during slit lamp examination.”
Preseptal cellulitis treatment involves oral antimicrobial therapy. With gram-positive cocci, such as Staphylococcus and Streptococcus species, being the most common causative organisms, select antibiotics accordingly.1 Keflex (cephalexin, Advancis Pharmaceutical) is a great choice and is commonly dosed 500mg PO BID for adults.3 This dosage is well tolerated and can be safely taken up to QID.4
Dr. Miriello prefers the more frequent dosing so he never has to wonder if a persistent case would have responded better. The treatment course can range from seven to 10 days, depending on the severity of the initial presentation.1
Check Motility
Orbital cellulitis occurs when these infections gain access to the orbit itself. While these patients may look preseptal, there are several symptoms and signs that readily set this more serious orbital infection apart. Look for some degree of ophthalmoplegia and pain with eye movement due to inflammatory infiltration of the extraocular muscles, Dr. Miriello says. Exophthalmometry is also recommended, since ipsilateral proptosis signals likely orbital involvement.1,3,5
As the disease progresses and the retrobulbar optic nerve becomes involved, visual acuity, color vision and pupillary reactions can become affected. Untreated orbital cellulitis may also result in orbital abscesses, cavernous sinus thrombosis or even intracranial extension of the infection, which can be deadly.1,3,5
Orbital cases may stem from preseptal ones if timely treatment is not initiated. Sinusitis is overwhelmingly the most common cause. Others include the spread of dental and middle ear infections, infected adnexal injection sites and traumas or surgeries that allow access to the orbit.1,5
“These patients require intravenous antibiotics and hospitalization, so prompt referral is crucial when you suspect orbital involvement,” Dr. Miriello says. Multidisciplinary management can greatly improve outcomes.1,3,5
Dr. Ajamian is the center director of Omni Eye Services of Atlanta. He currently serves as general chairman of the education committee for SECO International and is vice president of the Georgia State Board of Optometry. He has no financial interests to disclose.
1. Lee S, Yen MT. Management of preseptal and orbital cellulitis. Saudi J Ophthalmol. 2011;25(1):21-9. 2. Rimon A, Hoffer V, Prais D, et al. Periorbital cellulitis in the era of Haemophilus influenzae type B vaccine: predisposing factors and etiologic agents in hospitalized children. J Pediatr Ophthlamol Strabismus. 2008; 45(5):300-4. 3. Lim LT, Miller D, Ah-Kee EY, Ferguson A. Preseptal cellulitis or orbital cellulitis? West Indian Med J. 2015; 65(2):304-7. 4. Rodríguez-Uña I, Bañeros-Rojas P, Jiménez C, Díaz-Valle D, Gegundez-Fernandez J, Benítez-del-Castillo J. Systemic antibiotics with ophthalmic clinical usefulness. In: Benítez-del-Castillo J, Díaz-Valle D, Gegundez-Fernandez J, eds. Ocular Pharmacotherapy. Jaypee Brothers Medical Publishers; 2017:93-110. 5. Danishyar A, Sergent SR. Orbital Cellulitis. StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2021. |

